Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista odontológica mexicana
Print version ISSN 1870-199X
Rev. Odont. Mex vol.15 n.2 Ciudad de México Apr./Jun. 2011
Case report
Application of plasma rich in growth factors after extraction of lower third molars. Case report
Víctor Mario Fierro-Serna,* Ricardo Martínez-Rider,§ José Antonio Hidalgo-Hurtado,II José Martín Toranzo-Fernández,¶ Amaury de Jesús Pozos-Guillen**
* 4th year resident, Oral and Maxillofacial Department, Hospital Central "Dr. Ignacio Morones Prieto", San Luis Potosí.
§ Head, Oral and Maxillofacial Department, School of Dentistry, Universidad Autónoma de San Luis Potosí.
II Coordinator, Oral and Maxillofacial Department, Hospital Central "Dr. Ignacio Morones Prieto", San Luis Potosí.
¶ Head, Oral and Maxillofacial Department, Hospital Central "Dr. Ignacio Morones Prieto", San Luis Potosí.
** Professor, Researcher, School of Dentistry, Universidad Autónoma de San Luis Potosí.
ABSTRACT
In recent years, the use of plasma rich in growth factors and platelets has become popular in the fields of oral and maxillofacial surgery. This case report describes a 21 year old female presenting moderate pain in the lower right and left third molar area. Both third molars were surgically removed. 20 cc of the patient's blood were extracted to obtain plasma rich in growth factors. This plasma was applied to the area of the left lower third molar extraction site. The right lower third molar extraction site was irrigated with physiological saline. Three days after the operation, we could clinically observe a lesser degree of extraoral inflammation on the left side, when compared to the right side. On the left side, we observe intraorally less inflammation and erythema in the zone and better epithelization when compared with the right side Five days after the operation suture points are removed from both sides of the mandible On the left side the wound presented better epithelization and lesser degree of erythema. Seven days after the operation, the difference in the soft tissue regeneration is clearly better on the left side when compared to the right one. In every one of her control visits, the patient reported lesser degree of pain in the left side than in the right one. Our experience in this case indicates that the use of plasma rich in growth factors can be beneficial for the postoperative period of patients after surgical extraction of lower third molars.
Key words: Growth factors, plasma, third molars.
INTRODUCTION
In dentistry, extraction of third molars is one of the most common procedures. In general terms, extraction of third molars has a negative impact in the period of four to seven days after surgery, nevertheless it has been observed there is an improvement in the patient quality of life in that period if we can eliminate chronic pain and inflammation (generally due to pericoronitis). This has been itemized in studies describing the improvement found after surgical procedure.1 The most common reasons for the extraction of third molars are: cyst or tumor originating in the dental follicle, repeated pericoronitis episodes, irreversible carious lesions, distal periodontal defects in the second molar, distal carious lesions of the second molar as related to the third molar, and orthodontic reasons.2 The decision of third molar extraction in asymptomatic patients is still a subject for controversy. Extraction is recommended to reduce sequel risks, surgical morbidity, complications affecting neighboring teeth and to achieve better oral hygiene.
It has been reported in patients ranging from ages 20 to 29, a percentile increase from 18 to 40 percent in prophylactic extractions.3,4
Surgical extraction of third molars is associated to a moderate incidence of complications, about 10%.5 Influencing factors could be the surgeon s lack of experience and training to carry out this procedure inflicting minimal traumatism. The most common complications are: bleeding, third molar root factures, which hinder the extraction, occasional displacement of the roots to the submandibular space, lower dental nerve canal or maxillary sinus. Alveolar osteitis, or dry alveoli, appears in 20 to 25% of the cases.6 Post extraction infections after third molar extraction procedures, are less frequent (1.7 to 2.7%) in which cases we recommend antibiotic therapy. In general terms, albeit far less frequently, more extensive surgical procedures are required for the treatment of complications like lesions to nerves, lower jaw fracture, or the displacement of third molar whole body to the infratemporal fosa, maxilary sinus, and floor of the mouth.
The postoperative period to the extraction of third molars frequently presents in the patient swelling, pain, trismus and poor mastication function. The patient negatively rates all these signs and symptoms which are sometimes conductive to a longer convalescing period, which precludes them to carry on with their normal life. Due to these reasons, methods to reduce complications are constantly under research. Postoperative pain settles in when the local anaesthetic wears off or disappears completely and it reaches its maximum intensity in the 12 hour period following the operation. Several analgesics have been proposed to avoid this complication.7 Inflammation is an ever present sequel of third molar extraction procedures, it reaches its peak on the second day after procedure, and abates towards the fifth to seventh day. As treatment to minimize inflammation, parenteral administration of corticosteroids like dexamethasone and betamethasone, has been discussed. One of the factors more frequently related to post-operative pain and inflammation is the type of the surgical wound regeneration. Both primary and secondary wound closures have been evaluated, but controversy is still present concerning these two types of regeneration.8-10
In recent years, the use of platelet rich plasma and plasma rich in growth factors has become popular in maxillofacial and oral surgery procedures. Tayapongsak (1994) incorporates in mandibular reconstruction procedures autologous adhesive fibrin to spongy bone. In his report, he describes components which form the adhesive fibrin: fibrinogen obtained from human plasma and bovine thrombine, calcium chloride, and antifibrinolytic agents. When incorporating autologous adhesive fibrin he observed an improvement in the osteoconduction.11,12 At a later time, Whitman, (1997) proposed the use of platelet rich plasma and he itemized differences between fibrin glue and platelet gel. The platelet gel was obtained from a process of the patients blood extracted moments before the surgical procedure. This gel had a high platelet concentration which triggers the liberation of the growth factors which in turn promote better healing.13 A short time later, Marx (1998) combined platelet rich plasma with autogenous bone to repair mandibular defects. In the radiographic images obtained after this procedure, during the first 6 months after the operation, an accelerated bone formation was observed.14 This same author has described the application of platelet rich plasma in dental procedures such as elevation of maxillary sinus, periodontal defects treatment, increase of the alveolar ridge, placement in alveoli after third molar extractions, regeneration of soft tissue, and craniofacial applications for reconstruction purposes.15 Anitua (1997) has also described the use of plasma rich in growth factors. He reports an excellent epithelization and bone regeneration in zones being primed to receive dental implants.16-18 Properties here described can contribute to the decrease in common complications found after third molar extractions.
In this article we report a case where after the extraction of lower third molars, one side received application of plasma rich in growth factors, the other side did not, and results were compared.
CASE REPORT
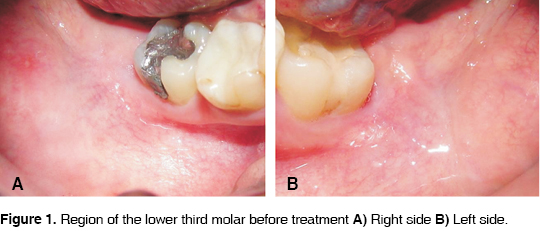
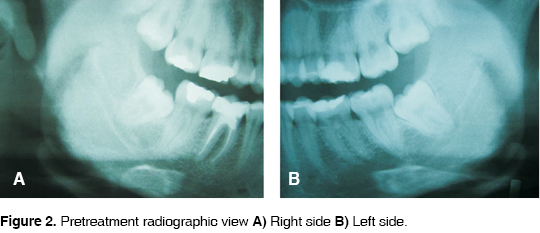
A 21 year old woman was admitted in the Clinica de Cirugía Maxilofacial de la Facultad de Estomatología, Universidad Autónoma de San Luis Potosí (Maxillofacial Surgery Clinic of the Stomatology School of the University of San Luis Potosi) for extraction of lower third molars. The patient informed of moderate pain. Clinically slight erithema of the mucosa in the right and left third molar area is observed (Figures 1A and 1B). Radiographically, both third molars were classified as class I, mesioangled with convergent roots with respect to the second molar, according to classification of Sanchez Torres19 (Figures 2A and 2B). It is decided to surgically remove both third molars under infiltration local anesthesia.
Ten minutes before procedure, approximately 20 cc of the patient's blood were extracted, to obtain plasma rich in growth factors, as described in Anitua s protocol. It was done in the following fashion: The patients blood was placed in sterile tubes with 3.8% sodium citrate (vacutainer) as anticoagulant. Plasma was then centrifuged at 1800 RPM during 8 minutes (Model BTI PRGF system II). Plasma obtained was separated into fractions through careful pipetting so as not to create turbulences in obtained fractions. The first 500 micra 1 were of plasma poor in platelets. The following 500 micra 1 of plasma have a platelet count similar to the one found in peripheral blood. The fraction of plasma richest in platelets and growth factors are the 500 micra 1 immediately above the red series. Once the pipetting was achieved, clot formation was induced by adding 10% calcium chlor after approximately 5 to 8 minutes.20 On both right and left side perioral asepsis and antisepsis was achieved with the help of isodine, anesthetic block of lower dental nerve with articaine and epinephrine (Medicaine 1/100). Approach was initiated through the left side with the design of a triangular flap. Once the flap was raised, osteotomy on the tooth vestibular side was performed, to later carry out odontosection. The tooth was extracted in two section without any trouble. The alveolus was richly irrigated with saline solution. The second fraction of plasma rich in growth factors activated with 10% calcium chloride was used to irrigate the alveolus and it was completely filled with a clot of plasma richer in growth factors. It was tightly sutured with 4-0 silk (Ethicon). The same procedure was applied to the right side with the exception of the plasma placement.
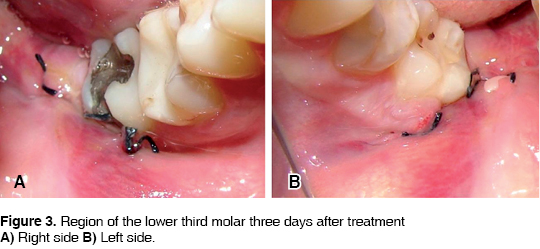
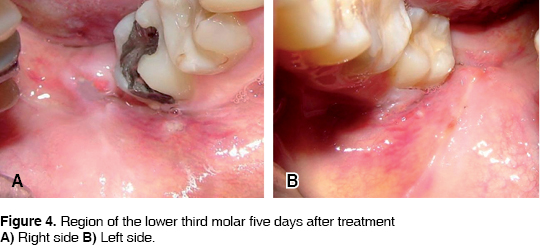
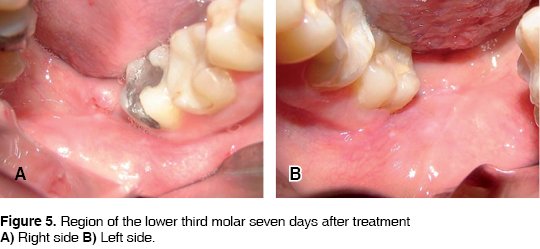
The patient is sent home with the indications specific to this type of procedure: Clindamycin, taken orally, 300 mg every 6 hours and Ketocorolaco, 10 mg every 8 hours. A clinical follow up was observed examining the patient on the third, fifth and seventh day after the operation. On the third postoperative day clinical observation was of lesser extraoral inflammation on the left side, Intraorally, lesser inflammation and erythema in the area was observed, along with improved epithelialization on the left side (Figures 3A and 3B). On the fifth day it is decided to remove suture material from both sides. On the left side, better epithelialization and less erithema of the wound is observed (Figures 4A and 4B). On the seventh postoperative day, there is a blatant difference in soft tissue regeneration in the left side when compared to the right one (Figures 5A and 5B). In all control visits, the patient the patient informed of lesser pain in the left side.
DISCUSSION
After surgery of impacted third molars, the patient feels psychologically affected in cases of slight bleeding, inflammation, pain, and limitations when opening the mouth. The patient feels uneasy about these symptoms. For these reasons, several methods have been suggested to reduce to the maximum these sequels so often present in these cases. The following have been recommended: use of corticosteroids, ice extraoral application in extraction sites to reduce inflammation, several analgesics and their combinations to decrease pain. This case describes the evolution of the patient when plasma rich in growth factors is used as an adjuvant to reduce this type of sequels.
Studies by Babbush21 and Mancuso22 have shown the ability of plasma rich in growth factors to reduce frequency of dry alveolus, and promote bone regeneration in the socket. This plasma also reduces the formation of periodontal pockets or any pathological condition which compromises the distal face of the second molars. This is based on the fact that repair mechanisms of growth factors occur in bone regeneration and repair processes. Soft tissue repair mechanisms occur simultaneously, and these can easier be observed than the changes which take place in the bone. The advantages of applying plasma rich in growth factors in third molar extraction sites, as in the case here described, is that upon intervening on the regeneration of the mucosa in that area, quality can be enhanced, decreasing thus periodontal defects. Healthy flap regeneration depends on a design that must provide good blood supply, and on a periodontium with appropriate osteogenic potential The osteogenic potential of the periostium can be altered by repeated pericoronitis episodes in the area. Therefore we can rate this type of patients as candidates for the use of plasma rich in growth factors after tooth extraction. These events justify the exogenous application of growth factors to improve bone and soft tissue regeneration, as described in this case.
Plasma rich in growth factors provide products which improve bone and soft tissue regeneration, both processes are expedited, the patient experiments less pain and swelling will decrease. No studies were found in which a assessment was made of these two events after extraction of lower third molars, together with application of plasma rich in growth factors. In the present case, the patient reported less pain and swelling on the left side which received plasma rich in growth factors.
Methods to obtain plasma rich in growth factors and plasma rich in platelets vary. There are several systems to obtain plasma rich in platelets. In these systems the amount of blood required varies, from 60cc (SmartPrep, PCCS, Secquire, Acces, GPS, Magellan) up to 450 cc (CATS). The most popular one is perhaps the SmartPRep system. In this system, after obtaining the patients blood it is first submitted to a separation centrifugation, which separates red blood cells from white ones, platelets and plasma. Plasma poor in platelets is separated putting it through a second centrifugation , called concentration centrifugation which separates and compacts platelets, white blood cells and a small portion of red cells. A new separation of plasma is performed, thus plasma rich in platelets sets in the bottom of the container. Once obtained, the plasma rich is platelets is activated with a combination of 10% calcium chloride and bovine thrombine.
Although Marx14 reports good results with plasma rich in platelets, in this case it was decided to use plasma rich in growth factors for the following reasons. The cost of equipment required for its elaboration is much lower. The amount of blood required to obtain plasma rich in growth factors is lower than the amount of blood required in systems to obtain platelet rich plasma. Some systems for obtaining platelet rich plasma, the process takes up to 32 minutes (PCCS). SmartPRep requires the shortest period, 15 minutes. The protocol is similar to the one for obtaining plasma rich in growth factors. Controversy has also arisen concerning the use of bovine thrombine, for some cases have been reported where antithrombine antibodies have been detected with their use. It has been suggested that plasma rich in platelets may cause Kreutzfeldt-Jakob disease. This theory has been disclaimed on the basis that the vector causing the disease is a protein present only in the nervous cells of humans, cats, lambs and other animals, and bovine thrombine is derived exclusively from the blood when submitted to a purification process. Regrettably, this is a difficult and expensive process. In this particular case, a difference was observed in the healing of lower third molar extraction sites when applying plasma rich in growth factors. This quality of plasma rich in growth factors has been exploited in several disciplines. In cosmetic surgery, it has been used to reduce swelling, ecchymosis and to accelerate regeneration of soft tissues.23 In dermatological surgery, it has been applied to obtain faster regeneration with less visible scars after excision of skin lesions.24 The patient informed of lesser pain on the side where plasma had been applied. Clinically better soft tissue regeneration and reduce swelling was found on the same side. All these facts lead us to believe that application of plasma rich in growth factors in third molar extraction sites can be an adjuvant for a better regeneration of bone and soft tissues in shorter periods and at the same time decreasing common sequels in this type of procedures, enabling the patient to return to his daily routines in shorter time.
CONCLUSIONS
Experience gained with this case leads us to suggest that the use of plasma rich in growth factors can benefit the postoperative period of patients after surgical removal of lower third molars.
REFERENCES
 Address correspondence:
Address correspondence:
Amaury de Jesús Pozos Guillén MD
Facultad de Estomatología,
Universidad Autónoma de San Luis Potosí.
Av. Dr. Manuel Nava Num. 2,
Zona Universitaria, 78290;
San Luis Potosí, SLP México.
Phone: 52 (444)8262357 X 106
Fax: 52 (444)8139743.
E-mail: apozos@uaslp.mx
Nota
This article can be read in its full version in the following page: http://www.medigraphic.com/facultadodontologiaunam
1. White RP, Shugars DFA, Shafer DM. Recovery after third molar surgery: clinical and health-related quality of life outcomes. J Oral Maxillofac Surg 1983; 41: 706-710. [ Links ]
2. Liedholm R, Knutsson K, Lysell, Rohlin M. Mandibular third molars: Oral surgeons assessment of the indications for removal. Br J Oral Maxillofac Surg 1999; 37: 443-450. [ Links ]
3. National Institute of Health. Consensus development conference for removal of third molars. J Oral Surg 1980; 38: 235-236. [ Links ]
4. Lysel I, Rohlin M. A study of indications used for removal of third molar. Int J Oral Maxillofac Surg 1988; 17: 161-164. [ Links ]
5. Nordenram A. Postoperative complications in oral surgery. Swed Dent J 1983; 7: 109-114. [ Links ]
6. Nitzan DNW. On the genesis of "dry socket". J Oral Maxillofac Surg 1983; 41: 110-706. [ Links ]
7. Schultze-Mosgau S, Schmelzeisen R, Frolich JC, Schmele H. Use of Ibuprofen and methylprednisolone for prevention of pain and swelling after removal of impacted third molars. J Oral Maxillofac Surg 1995; 53: 2-7. [ Links ]
8. Pasqualini D, Cocero N, Castella A, Mela L, Bracco P. Primary and secondary closure of the surgical wound after removal of impacted mandibular third molars: a comparative study. Int J Oral Maxillofac Surg 2005; 34: 52-57. [ Links ]
9. Korbendau JM, Korbendau X. Clinical success in impacted third molar extraction. Quintessence Books, 2002. [ Links ]
10. Milloro M. Peterson's Principles of Oral and Maxillofacial Surgery . BCDecker Inc., 2004. [ Links ]
11. Tayapongsak P, O'Brien DA, Monteiro CB, Arceo-Diaz LL. Autologous fibrin adhesive in mandibular reconstruction with particulate cancellous bone and marrow. J Oral Maxillofac Surg 1994; 52: 161-166. [ Links ]
12. Matras H. The use of fibrin glue in oral and maxillofacial surgery. J Oral Maxillofac Surg 1982; 40: 617. [ Links ]
13. Whitman DH, Berry RL, Green DM. Platelet gel: An autologous alternative to fibrin glue with applications in oral and maxillofacial surgery. J Oral Maxillofac Surg 1997; 55: 1294-1299. [ Links ]
14. Marx RE, Carlson ER, Eichstaedt RM, Schimmele SR, Strauss JE, Georgeff KR. Platelet-rich plasma growth factor enhancement for bone grafts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998; 85: 638-646. [ Links ]
15. Marx RE, Garg AK. Dental and Craniofacial Applications of Plateket-Rich Plasma. Quintessence Books, 2005. [ Links ]
16. Anitua E. Plasma rich in growth factors: Preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants 1999; 14: 529-535. [ Links ]
17. Anitua E. The use of plasma rich in growth factors (PRGF) in oral surgery. Pract Proced Aesthet Dent 2001; 13: 487-493. [ Links ]
18. Anitua E. La utilización de los factores de crecimiento plasmáticos en cirugía oral, maxilofacial y periodoncia (PRGF). Rev Col Odon 2001; 6: 305-315. [ Links ]
19. Sánchez J, Reyes R. Clasificación de terceros molares inferiores retenidos. Valoración radiográfica. Rev Estomatol 1969; 7: 63-70. [ Links ]
20. Anitua A, Ortiz A. Un nuevo enfoque en la regeneración ósea. Plasma rico en factores de crecimiento . Editorial Puesta al Día Publicaciones, S.L. 2000. [ Links ]
21. Babubush CA. The use of PRP in conjunction with other bone graft material: Allograft, alloplast, senograft. Presented at the 2 nd Symposium on Platelet-Rich Plasma (PRP) & Its Growth Factors, San Francisco , 2003: 23-26. [ Links ]
22. Mancuso J, Bennion JW, Hull MJ, Winterholler BW. Platelet rich Plasma: A preliminary report in routine impacted third molar surgery and the prevention af the alveolar osteitis. J Oral Maxillofacial Surgery 2003; 61 (suppl 1). [ Links ]
23. Powell Dm, Chang E, Farrior EH. Recovery from deep-plane rhytidectomy following unilateral wound treatment with autologous plateket gel: A pilot study. Arch Facial Plat Surg 2001; 3: 245-250. [ Links ]
24. Adler SC, Kent KJ. Enhacing wound healing with growth factors. Facial Plast Surg Clin North Am 2002; 10: 129-146. [ Links ]











 text in
text in 


