Introduction
The number of older patients with cancer is rising with the global aging of the population. As more older people are diagnosed, and a growing number of therapeutic options are made more widely available as well1. Therefore, it is essential to identify and better understand the effects of cancer and treatment on health outcomes for older adults.
Cancer-related emergencies are often used to describe a unique set of malignancy and treatment-related syndromes requiring a prompt evaluation and care2. In older adults, these can manifest as geriatric syndromes. Hence, the importance and beneficial effects of a geriatric approach in the management of older patients with cancer.
In addition, management of older individuals with cancer is complicated. Older adults are at high-risk treatment-related side effects and severe treatment toxicity associated with the management and treatment of their cancers, such as falls, delirium, and acute pain3-5. Unplanned emergency department (ED) visits and hospital admissions occur in older adults under treatment for cancer due to numerous treatment-related side effects6. Helping older adults identify and manage side effects may reduce the number of unplanned admissions and lower the incidence of cancer-related complications reducing resource use and improving quality of life for older patients5,6.
This review article summarizes evidence of common geriatric emergencies in older adults with cancer as well as the importance of a special approach and management in this population.
Epidemiology and characterization of older adults with cancer seeking acute emergency care
Increasing age is one of the strongest risk factors for cancer development. An increasing proportion of people will be living longer, and there will be an increase in cancer prevalence. The proportion of the world’s population aged 60 years or over will increase from 12% in 2013 to 21% in 20507.
According to the National Cancer Institute (NCI), 60% of newly diagnosed malignancies are found in people over the age of 65 years. Projections estimate that the number of new cases in both sexes between 65 and 85 years old will raise from 9.95 million in 2020 to 17.7 million in 20408. Approximately 4% of all adult ED visits in the US are for cancer-related complaints9.
Patients with advanced cancer generate 4 million visits annually to EDs and other oncology urgent care centers. These emergencies represent a wide spectrum of disorders resulting from initial manifestations of malignancy, progression of the disease, recurrence, and adverse effects from therapy10. Due to the normal aging process, the functional capacity of organ systems is reduced, creating a higher risk for the development of chronic diseases, and increasing complications across the disease course of negative outcomes related to their medical history.
Disparities in care of older adults in cancer treatment trials and ED use exist. In fact, Bischoff et al. found that older adults frequently presented for symptom-related diagnoses but received fewer symptomatic interventions in the ED suggesting that important opportunities to improve the care of older adults with cancer exist11.
The aging process is complex and each person ages at a different rate. Modifications targeted at the geriatric patient in inpatient settings have already been shown to successfully reduce adverse events such as delirium, iatrogenic complications, hospital costs, hospital length of stay, and transfer to long-term care facilities12. That is why different needs that often exist in this age group must be considered when making decisions about their treatment and medical care.
General factors associated with unplanned hospitalization and emergency care
Unplanned hospitalizations are more frequent in older adults aged 65 years or more, representing approximately 36-38% of all hospitalizations each year in the USA13. In patients with newly diagnosed cancer, 35% of older adults (> 75 years) present an unplanned hospitalization during the 1st year after diagnosis14.
Patients with cancer are well-known for the numerous complications associated with their disease and/or with the rigorous treatment modalities they receive. This added to the fact that with aging, the physiological reserves, and the ability to compensate toward stressors decrease, older adults are at high risk to present an event that takes them to the ED, or what causes an unplanned hospitalization and should be closely monitored during treatment6. Important risk factors for hospitalizations in older adults include age 75 or older, > 1 hospital admission in the previous 6 months, multiple comorbidities, living alone, poor social support, poor self-rating of health, functional or cognitive impairment, and/or history of depression15.
However, the reasons for hospital admission and the disease spectrum can be very broad. Symptoms of cancer may be more difficult to interpret in older patients due to comorbidity, and sometimes, this leads to delayed diagnosis. These can include the classic manifestations secondary to the neoplasm and its treatment, but sometimes have occult or atypical presentations of disease that can be presented as geriatric syndromes7. In older patients with cancer, geriatric syndromes can complicate cancer treatment and affect the quality of life, overall mortality, and increase the burden of caregivers16. For example, falls and delirium have been shown to be predictive of chemotherapy toxicity and overall survival17. It is important that these symptoms are not interpreted as normal aging.
Most common geriatric emergencies in the older adult with cancer
Falls
Falls are common events that pose a serious health problem for older persons, occurring in 30% of adults over age 65 and 40% over age 80. Falls account for approximately 10% of emergency visits in older adults18. Specifically, the incidence of falls in older people with cancer could be as high as 50% and requires some additional consideration in treatment planning18,19.
Falls are a major geriatric syndrome. Falls may signal underlying issues related to the patient’s ability to tolerate chemotherapy treatment, so fall assessment may add to physicians’ understanding of patient vulnerability when considering cancer treatment19,20.
Fall rates are higher in older adults living with cancer. Findings from Schroder et al. suggested that older patients with cancer receiving chemotherapy or androgen deprivation therapy (ADT) may be more at risk for falling than non-users and advanced stage or palliative patients may be more likely to fall and to sustain injury from the falls21.
Falls are the leading cause of unintentional injury, which ranks as the sixth leading cause of death among older adults20,22. Falls lead to functional decline, hospitalization, mortality, institutionalization, and increased health-care costs22. More importantly, at least one in 20 community-dwelling older patients experiences changes to the treatment regimen because of falls and related injuries. However, falls in community-dwelling older patients with cancer are often under-reported and under-recognized22,23.
Risk factors and assessment in the ED setting
Older adults living with cancer are potentially subject to the interaction between consequences of aging, the local, systemic, and metastatic manifestations of cancer and the problems arising from the effects of cancer treatments24.
A fall should be treated as a symptom, and the physician should evaluate the causes and consequences of fall. Knowledge of an individual’s cancer history and ability to recognize oncologic symptoms is important to the management of oncology patients24,25. Furthermore, it is important to remember that a fall can signal a sentinel event in an older person’s life triggering a downward spiral of complicating events, finally leading to death25.
The most common reasons for injurious fall-related ED visits among older adults are fractures (41.0 %) followed by superficial/contusion injuries (22.6%) and open wounds (21.4 %)26. Serious injuries associated with fall include hip fracture, rib fracture, subdural hematoma, other serious soft-tissue injuries, or head trauma. Furthermore, they are associated with fear of falling, loss of confidence, going out less often, functional decline, and nursing home placement. Moreover, falls may alter the trajectory of the disease progression, care planning, and prognosis24-26.
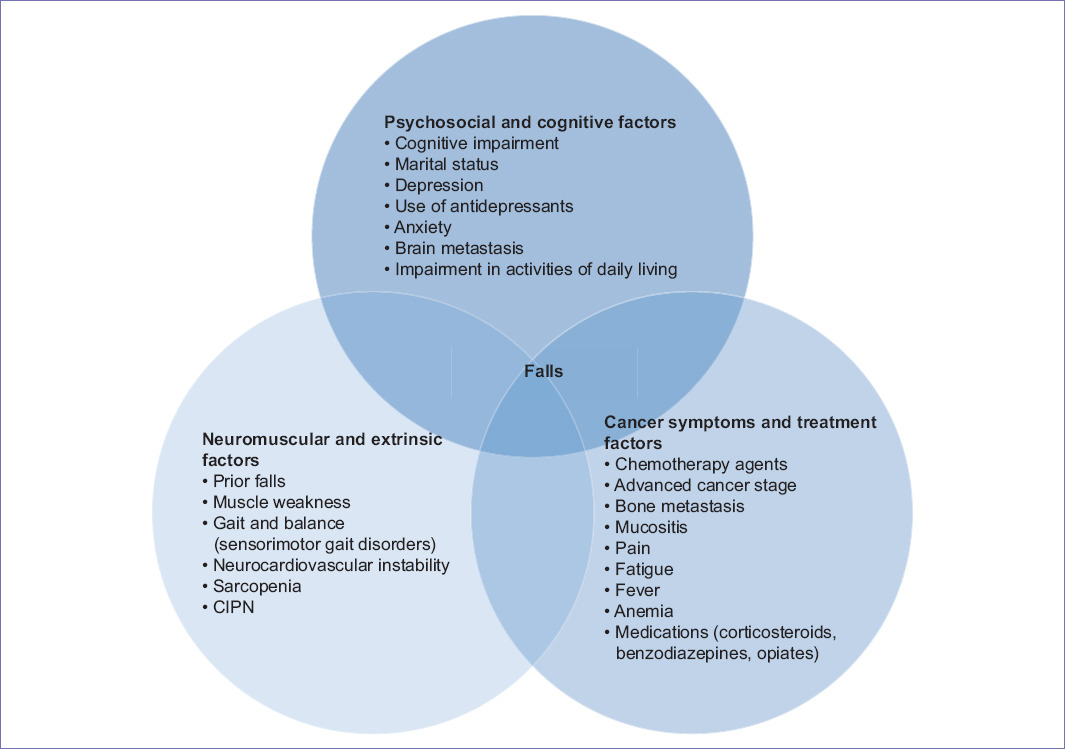
Appropriate assessments can help identify underlying causes and individuals at risk for falls, which, in turn, can help mitigate falls and their associated negative impact on older adults with appropriate interventions. Main identified risk factors for falls in older adults with cancer are shown in figure 1.
Psychosocial and cognitive factors
Psychosocial and cognitive issues including cognitive impairment, marital status, and depression are significantly associated with falls. Cognitive impairment was associated with 12-53% greater odds of falls27. The incidence of falls in community-dwelling subjects with cognitive impairment and dementia is about twice that in cognitively normal counterparts. Specific factors identified in unselected populations relate to gait and balance (sensorimotor gait disorders), central processing, memory, and neurocardiovascular instability (orthostatic hypotension and carotid sinus hypersensitivity)27,28. The availability of social support, evidenced by married marital status, was associated with 60% lower odds of falls (odds ratio [OR] = 0.42 [95% confidence interval (CI) = 0.19-0.93]). The score on the geriatric depression scale was significantly associated with falls, while the use of antidepressants was associated with a 29% increased risk of falls. In addition, anxiety is long established risk factor for falls and their debilitating consequences26,29-31.
Among various risk factors, the presence of brain metastases and impairment in activities of daily living (ADL) is importantly associated with falls in community-dwelling older adults in both general geriatric and oncology settings22,29-33.
Cancer symptoms and treatment factors
There are risk factors for falls that are unique to a population of patients with cancer. These include certain chemotherapeutic agents and advanced cancer stage31. Older patients are especially at risk for falls and fall injuries because of bone loss and disruption of bone cell homeostasis related to bone malignancies or bone metastases, interference in bone blood supply (e.g., pelvic hip region) related to radiation therapy, increased falls and osteoporosis resulting from ADT, and osteoporosis from use of aromatase inhibitors32,33. Mucositis resulting from chemotherapy and radiation therapy, treatment-related sarcopenia, and chemotherapy-induced peripheral neuropathy (CIPN) are also identified risk factors. CIPN is a significant complicating and often dose-limiting side effect of chemotherapy. The cumulative dose of chemotherapy and the use of more than 1 neurotoxic agent may be associated with higher rates of falling and fall-related injuries33-35. In addition, the well-recognized effects of cancer treatment on working memory, attention, processing speed, and executive function are often apparent before treatment and may be as much the result of the cancer itself as they are “chemo brain”35.
Pain and chemotherapy type are significantly related to falls. Patient report of daily pain was associated with 44% greater odds of falls (OR = 1.44 [95% CI = 1.32-1.59]). Increasing numbers of cycles of neurotoxic chemotherapy were associated with greater risk of falls (OR = 1.3/cycle [95% CI = 1.01-1.75])36. Neurological examination of the lower limbs with reference to tactile sensation and proprioception is an essential prerequisite in the consideration of neurotoxic chemotherapy.
Cancer-related fatigue was associated with greater likelihood of falls, diminution in functional capacity, and the lack of motivation associated with mood disturbance has sequential effects on muscle strength, gait, and balance, in turn, exerting a cumulative effect on fall risk. Treatment-related anemia and thrombocytopenia, specifically anemia requiring a blood transfusion, were significantly associated with falls (OR = 2.36 [95% CI = 1.25-4.46]). The presence of fever (OR = 7.19 [95% CI = 2.06-25.11]) and lower blood pressure (OR = 0.96/mmHg [95% CI = 0.93-0.99]) were also significantly associated with inpatient falls. Furthermore, certain medications were noted to be significantly associated with falls, including antipsychotics (adjusted OR = 1.94 [95% CI = 1.06-6.54]), corticosteroids (OR = 2.85 [95% CI = 1.65-4.9]), benzodiazepines (OR = 2.15 [95% CI = 1.09-4.23]), and opiates36.
Neuromuscular and extrinsic factors
Prior falls have been consistently identified as the most common fall risk factor in both inpatient setting and community setting in the general geriatric population, as well as within the geriatric oncology setting. Prior falls are associated with increased risk for chemotherapy toxicity and death21,34-36.
Muscle weakness, gait, and balance abnormalities are among the strongest risk factors for falls in older people. Postural instability and falls erode confidence and result in a negative cycle of diminishing activity levels, further deconditioning, and a higher risk of further falls. Sarcopenia may be present in up to 40% of patients before undertaking any cancer-related treatment and is strongly associated with poor outcomes36,37. Age-related impairments of lower limb neurological function are commonly exacerbated by neurotoxic chemotherapy, resulting in gait and balance deficits.
Importantly, screening for the presence of known risk factors before treatment through simple functional assessments has been advocated as a rapid means of identifying those patients who would probably benefit from a more detailed geriatric assessment to reduce the presence or recurrence of falls.
Comprehensive geriatric assessment (CGA)-led interventions and management
Immediate assessment of the falls is suggested in the ED, and referral to specialist multifactorial interventions is essential18. To date, multiple intervention trials have been conducted including multifactorial targeted risk factor intervention studies, which have resulted in an approximately 30% relative risk reduction in fall rate.
Comprehensive assessment plus individualized multifactorial intervention to address contributing risk factors is the most recommended actions for those who are at heightened risk for falls38-42. Importantly and irrespective of age, exercise has been shown to be safe and beneficial for a wide range of cancer types and positive effects can be realized at all stages, including end of life. Group and home-based exercise training incorporating balance, gait, and strength training and Tai Chi have been found to be effective in preventing falls41,42. Exercise activity/programs should be titrated according to the person’s current functional level and abilities. Moreover, in terms of preventing injurious falls, exercise alone and various combinations of interventions (e.g., visual assessment, environmental assessment and modification, etc.) can help lower risk of injurious falls.
Other commonly recommended interventions include routine fall assessment and gait and balance assessment. Recommendations regarding Vitamin D supplementation are mixed, with the most recent guideline recommending against Vitamin D supplementation as a means of fall prevention. Dietary intervention (including calcium supplementation to optimize bone health and nutritional supplement for those who are malnourished); home safety evaluation and referral to geriatrician or primary care provider for further assessment and intervention for potentially modifiable issues; medication review to identify for potential high-risk medications that have been known to contribute to falls (e.g., psychotropic and antihypertensive medications); assessing for postural hypotension, and providing education to the older adult and their caregiver (as appropriate) in conjunction with other interventions. Patients may also need specific advice concerning environmental or activity modifications, such as extra vigilance while negotiating sidewalk curbs, steps, and stairs, for those at risk for treatment-related peripheral neuropathy. In-home safety evaluations should also be arranged for older patients with neurotoxicities38-44.
Using an individualized approach to exercise prescription, PT can tailor training programs for older adults based on findings from physical assessment instead of “off-the-shelf” exercise programs. Hence, PTs are valuable interdisciplinary members in helping tailor exercises for older patients in the oncology context41. Furthermore, activities including outdoor walking or mall walking are likely the most feasible and accessible ways of exercising that enhance strength, balance, and flexibility, in turn, aiding the reduction of falls44.
Acute pain
Pain is defined by the International Association for the Study of Pain (IASP) as “an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage”45. Cancer pain is a complex symptom and a common cause of ED visits and decreased quality of life and functionality46. In older adults, unresolved cancer pain has been associated with impaired walking, sleep disturbances, malnutrition, depression, fatigue, and social isolation47. Nevertheless, studies had reported inadequate symptom control in the ED and its association with hospitalization and death48.
Risk factors and assessment in the ED setting
The screening and assessment of oncologic pain is an essential part in the care of older patients with cancer, however, older adults with cancer are often undertreated and underrepresented in cancer-related pain clinical trials and have a high prevalence (80%) of non-oncologic chronic pain posing a major challenge to clinicians, especially in the ED47,48.
In the emergency room, assessment should start by ruling out a life-threatening medical emergency revealed by pain, cancer, or non-cancer related, followed by a quick relief of the uncontrolled cancer pain. Assessment of pain includes symptom and patient characterization, classification of etiology of pain, and identification of cancer syndrome48,49.
The characterization of the symptom includes inquiry of the location, duration, intensity, quality, and patterns of pain. Patients with cognitive impairments and/or limited communication skills require the assessment of pain-related behaviors. Several screening tools had been implemented and until now none have been superior to the others. The Checklist of Non-verbal Pain Indicators (CNPIs) and the Pain Assessment in Advanced Dementia Scale (PAINNAD) are some screening tools that can be used in these populations49,50. Patient characterization must include comorbidities, on-going and past treatments, and the impact of pain on functionality, malnutrition, and psychological state. In the ED, short screening tools such as the short brief pain inventory, and the patient health questionnaire-2 (PHQ-2), can aid the clinician to achieve this50.
The second step is to classify the etiology of the pain into nociceptive and/or neuropathic as it will improve the choice of treatment. Nociceptive pain is caused by the injury of a tissue, which activates the somatosensory system. It is subdivided into somatic and visceral pain. Patients may refer to the pain quality as stabbing, throbbing, or pressure. On the other hand, neuropathic pain is the result of a lesion of the somatosensory nervous system. The patient may refer to uncomfortable sensations such as shock-like, burning, or electric. In non-communicating patients, sensitivity to a light touch can signal neuropathic pain (NP).
The third step is to identify the pain cancer syndrome. Cancer pain syndromes are classified into acute (few weeks of duration) or chronic. Acute syndromes are subdivided into pain directly related to cancer and pain associated with antineoplastic treatments, the latter being the most prevalent type of acute cancer pain (Table 1). It is important to differentiate acute cancer pain to breakthrough cancer pain, defined as a transitory flare of moderate or severe pain that occurred on a background of relatively well-controlled baseline pain with a short duration51.
Table 1 Acute cancer pain syndrome
| Acute cancer syndrome | Characteristics |
|---|---|
| Directly related to cancer | |
| Pathologic fracture | Sudden onset of back or limb neuropathic pain. |
| – Multiple myeloma, breast, lung, or prostate cancer | |
| Perforation of hollow viscus | Acute severe intra-abdominal pain |
| – Gastric cancer | |
| Intratumoral hemorrhage | Severe right upper quadrant pain |
| – Hepatocellular carcinoma | |
| Superior vena cava obstruction | Facial and neck swelling, dyspnea, neck pain, dilated neck, and chest wall veins |
| Acute thrombosis | Pain and swelling in the limb |
| Related to antineoplastic treatments | |
| Chemotherapy induced | |
| Oral mucositis | Oral pain and ulceration |
| – Myeloablative chemotherapy, methotrexate, 5-fluorouracil, and doxorubicin | |
| Neuropathy | Paresthesias |
| – Vinca alkaloids, platinum-based agents. Thalidomide and bortezomib | |
| Erythrodysesthesia | Painful rash on palms and soles |
| – Cytarabine, capecitabine, 5-fluorouracil, docetaxel | |
| Headaches | Holocephalic, positional quality (worse upright) |
| – Intrathecal chemotherapy of methotrexate, cytarabine, and trans-retinoic acid | |
| Angina | Coronary vasospasm |
| – 5-fluorouracil and capecitabine | |
| Radiation therapy induced | |
| Plexopathy | Pain, paresthesias and weakness in shoulder, arm, and hand |
| Bone pain | Acute increase in focal bone pain transitory |
| Enteritis | Cramping, nausea, and vomiting |
| Proctitis | Painful tenesmus, diarrhea, mucus discharge, and bleeding |
CGA-led interventions and management
Cancer pain management consists of a multimodal approach that includes pharmacological treatment (following the WHO ladder strategy), primary antitumor treatment, interventional analgesic therapy, and non-invasive therapy. Geriatric-led interventions and modifications in pain management include the following:
Pharmacological treatment
- Dose reduction: Consider age-related changes, comorbidities, and pharmacologic interaction that could alter pharmacokinetics and pharmacodynamics on the patient.
- Route of administration: While the oral route of administration should be the first choice, the subcutaneous route has proven to be a simple and effective form of administration (morphine and hydromorphone), and it should be the first-choice alternative route for patients with contraindication for oral administration.
- Reassessment of pain and side effects: Analgesic titration to the smallest effective dose possible.
- Non-communicative patients: Empiric analgesic trial and titration if procedures or conditions are likely to cause pain or the patient presents behavioral manifestations of pain.
- Patient education and empowerment: Patients should learn the adverse effects of antineoplastic and analgesic treatment, as pain is a possibility at any stage of the disease, and to communicate their symptoms and its intensity to their physician
- Non-pharmacological interventions: Screening of depression, anxiety, and sleep disorders, as it can reduce coping mechanisms, alter perception of pain, and treatment adherence51,52.
Delirium
Delirium is defined by the diagnostic and statistical manual, 5th edition (DSM-V) as a disturbance in attention, reduced awareness of the environment and a change in baseline cognition which tends to fluctuate, cannot be explained by another preexisting neurocognitive disorder, and do not occur in the context of a severely reduced level of arousal such as comma. It is subdivided by the predominant behavioral presentation, into hyperactive, hypoactive, or mixed. Delirium is common in older adults with cancer, with a frequency ranging from 8% to 38% in the ED, up to 50% in hospitalized patients and 80% in palliative patients53. Delirium has been associated with increases in mortality, length of hospitalization, loss of independence, and caregiver distress, however, it is often inadequately diagnosed by physicians obscuring the diagnosis and delaying a proper treatment53,54.
Risk factors and assessment in the ED setting
The assessment of delirium, a complex and multifactorial disorder, starts by recognizing the disorder and identifying the probable causes. There are several tools created to aid physicians to accurately diagnose delirium. One of the most studied instruments is the confusion assessment method (CAM), while it has been validated in ED settings with a sensibility of 86-94%, it takes up to 10 min to complete making it difficult to achieve in a fast-paced emergency setting54,55. Shorter versions had been proposed with a completion time of 2 min, such as the brief CAM and 4AT test, both with similar sensibilities and recommended by the American Cancer Society55. In patients with dementia, the preferred tool is 4A’s test (4AT)55,56.
After identification of delirium, a thorough clinical assessment, medication review, and an appropriate laboratory and radiological investigation are required to identify the probable precipitating and predisposing factors (Table 2)56. Predisposing factors are preexisting characteristics of the patient that increase their vulnerability to have an episode of delirium, on the other hand, precipitating factors are those acute factors that can trigger delirium. A patient with a greater load of predisposing factors may only need one precipitating factor to present an episode of delirium.
Table 2 Predisposing and precipitating factors for delirium
| Predisposing factors | |
|---|---|
| Dementia/cognitive impairment | |
| History of delirium | |
| Frailty | |
| Alcohol misuse | |
| Visual/hearing impairment | |
| Depression | |
| Older age > 75 years | |
| Brain metastasis | |
| Radiotherapy-induced neurotoxicity – Central system radiotherapy | |
| Chemotherapy-induced neurotoxicity – Methotrexate, cytarabine, and ifosfamide | |
| Leptomeningeal disease | |
| Precipitating factors | |
| Related to antineoplastic treatment | Directly related to cancer |
| Metabolic abnormalities | Pain: pathologic fracture, intratumorally hemorrhage, acute thrombosis, superior vena cava obstruction. |
| – Nephrotoxicity | |
| – Hepatotoxicity | |
| Dehydration | Dehydration |
| – Diarrhea | – Oral intolerance. Head-and-neck tumors: |
| – Nausea/emesis | |
| Medication (initiation, abrupt suspension, or pharmacological interactions) | Electrolyte imbalances |
| – Opioids | – Malignant hypercalcemia. Multiple myeloma, lymphoma, lung, breast, renal cancer: |
| – Benzodiazepines | – Hyponatremia (SIADH). Small cell lung cancer: |
| – Corticosteroids | |
| – Antipsychotics | |
| – Anticholinergics | |
| – Antidementia | |
| – Antidepressant | |
| Infections | Cerebral edema |
| – Pneumonia | – Brain metastasis. Melanoma, lung, breast, colon, and renal cancer. |
| – Urinary infections | |
| – Intra-abdominal infection | |
| Pain | |
| – Chemotherapy or radiotherapy induced | |
| Physical restraints/instrumentation | |
| – Foley catheter | |
| – Central lines | |
| – Surgery | |
CGA-led interventions and management
The key part of delirium management is to identify and treat the underlying cause. Management must include:
- Treatment of acute medical issues: Which can be divided into related to antineoplastic treatment or directly related to cancer (Table 2)
- Drug adjustments: Inappropriate medication, abrupt suspension, or high-risk pharmacological interactions.
- Correction of reversible predisposing factors: Address sensory impairment; provide eyeglasses, hearing aids, interpreters
- Reorientation strategies and normalize sleep-wake cycle: Bright light exposure during the day and discourage napping and interruption of sleep at night
- Reassess the patient after correction of precipitating factors: If no improvement is shown re-evaluate causes.
The benefit of pharmacological management in delirium has not been demonstrated. Antipsychotic medication should only be reserved for patients with severe agitation that interrupts essential treatment, puts at risk their safety, and/or presents psychotic disruptive symptoms. While using antipsychotics, physicians must start with the lowest effective dose and follow a slow titration to avoid adverse effects. At the end of life, patients may present with refractory delirium, and in some cases, palliative sedation may be implemented55,56.
Prevention of delirium in the ED is a growing area of research. Non-pharmacological interventions, such as multifactorial programs, remain the cornerstone of delirium prevention, but in the ED setting, the feasibility and effectiveness are still in question55. In contrast, low-dose melatonin is the only pharmacological treatment that has shown potential delirium prevention benefits in patients with overnight stay in the ED55-57.
Importance of appropriate health assessment and treatment for geriatric oncology patients
The functional capacity of organ systems is reduced with increasing age. This progressive reduction in organ functional capacity creates a risk for the development of multiple chronic diseases, leading to multimorbidity, which at the same time confers an increased risk of negative outcomes. For this reason, older adults who come to the ED are already at increased risk of experiencing negative outcomes during the ED58. After an emergency visit, older adults are at greater risk for medical complications, functional decline, and poorer health-related quality of life than they were before. It has been observed that up to 27% of older adults visiting an emergency room experience readmission or death within 3 months after discharge13.
There are many aspects to consider when treating older patients with cancer as the limitation in organ functions, altered drug metabolism, polypharmacy, frailty, and comorbidity. Therefore, older adults must be provided with individualized medical, psychological, and rehabilitative care based on the findings of the CGA59,60. The use of CGA at admission increases the chances of survival and of discharge to their home59-61. Some other benefits include improved cognition, reduced death, dependence, and institutionalization.
Because the ED is considered a dynamic and practical service, it has been suggested that a CGA could delay the diagnosis or treatment of patients. However, older patients with cancer, particularly those admitted to the ED, need individualized care to avoid negative outcomes through targeted interventions. Some evolving interventions designed to address the needs of older people in the ED have been proposed.
In 2014, the Geriatric ED Guidelines were published with the objective of offering geriatric-friendly ED care recommendations by focusing on staffing, administration, physical environment, and leadership16. Furthermore, various models of medical care have evolved to provide information on urgent CGA application62-64.
The management of the older person with cancer is complex, and even more so in an acute episode, so the initial comprehensive assessment is the key to management. The CGA has been developed to promote quality of care and improve clinical outcomes in the hospital and ED setting64,65.
Conclusion
Cancer is a complex disease that must be analyzed from several points of view, and special aspects need to be emphasized for older adults. Geriatric assessment can potentially identify and comanage older adults at highest risk of serious complications or emergencies, presenting as geriatric syndromes at the emergency setting. The beneficial effects of a geriatric approach in the management of older patients with cancer, through guided interventions, are key and essential for the improvement of clinical outcomes and cancer care.
Understanding the unique presentation of older patients with cancer who experience oncologic and geriatric complications and emergencies and designing future research studies that accurately reflect their needs and proper management is critical.











 text new page (beta)
text new page (beta)