Services on Demand
Journal
Article
Indicators
Related links
Share
Revista odontológica mexicana
Print version ISSN 1870-199X
Rev. Odont. Mex vol.15 n.2 Ciudad de México Apr./Jun. 2011
Case report
Temporomandibular ankylosis. Liberation, reconstruction with crown apophyses and auricular cartilage: Presentation of clinical case
José Gregorio Ravelo Loreto* Juan Carlos López Noriega,§ Rafael Ruiz RodríguezII
* Graduated, maxillofacial and oral surgery specialty, National University of Mexico.
§ Oral and maxillofacial specialty coordinator, National University of Mexico.
II Registered in the oral and maxillofacial surgery specialty, National University of Mexico.
ABSTRACT
Temporomandibular joint (TMJ) ankylosis is the total or partial union of the articulation components. The most common cause would be macrotraumatisms associated with fractures of the condylar process during active growth process in early childhood.1,2 TMJ ankyloses in children are mainly caused by traffic accidents and falls.3 In children, this pathology is particularly interesting since in them, a phase of hypomobility can have a significant impact in the process of facial growth. It is therefore important to liberate the articulation at early stages, and provide a graft so as to allow symmetrical facial growth.4 We present a clinical case.
Key words: Temporomandibular joint ankylosis, temporomandibular joint hypomobily, coronoid process graft, auricular cartilage graft.
INTRODUCTION
The temporomandibular joint (TMJ) is one of the most complex articulations of the human body. It is classified as a gynglimoid , arthrodial, sinovial and mobile articulation. It is considered ginglymoid since it provides hinge movement in a plane, and diarthrodial for it allows sliding movements.
It is composed by a mandibular condyle fitted into the mandibular fossa of the temporal bone and the articular disc which allows the movement of the whole group . The articular disc is formed by avascular and non innervated connective fibrous tissue. In a sagital cut, according to its thickness, the disc can be divided into three regions: intermediate, anterior and posterior. From an anterior view, the disc is generally thicker medially than laterally. Its shape adopts the condyle and mandibular fossa morphology. The articular disc adheres to the capsular ligament anteriorly, posteriorly, medially and laterally. It therefore creates two different cavities which are lined with special endothelial cells forming a sinovial lining covering of these cavities. Sinovial fluid has two purposes it acts as a lubricant and also as a means to provide metabolic requirements to these tissues.5
TMJ innervation
TMJ is innervated by the trigeminal nerve which provides motor and sensorial innervation to the muscles that control it. The mandibular nerve branches provide afferent innervation. The greater part is provided by the auriculotemporal nerve. The deep temporal innervation and the masseteric nerve provide additional innervation.
TMJ vascularization
The predominant vessels are: the deep temporal artery coming from the posterior zone, the media meningeal artery coming from the anterior zone and the internal maxilar artery from the inferior zone. Other arteries are the deep auricular, the tympanic anterior and the ascending pharyngeal. The condyle is irrigated through the cancellous bone and nutritional vessels.18
Ligaments
TMJ ligaments are collagenous connective tissue ligaments which do not elongate, they only do so in case of excessive force. Ligaments do not actively participate in articular functions, they act passively, limiting movements.
TMJ presents three functional ligaments: collateral, capsular and temporomandibular. It also presents two accesory ligaments sphenomandibular and stylomandibular.
By definition, ankylosis means abnormal immobility of the articulation. Limited mobility is divided into two basic types of ankylosis: fibrous ankylosis and bone ankylosis. Fibrous ankylosis is more common and can take place between the condyle and the disc, or between the disc and the fossa. A case of bone ankylosis takes place between the condyle and the fossa, in this case the disc must be displaced in the discal space.5 This ankylosis is due to the fusion of the mandibular condyle with the base of the skull and can be partial or total. The factors cause a disturbing condition which preempts the benefits of a normal diet, and inflicts serious facial disfigurations, it also causes psychological stress and periodontal and dental health problems.6,7
There are several reports on early detection techniques, and immediate condyle resection and reconstruction to increase patient comfort and functional rehabilitation.3,8 Temporomandibular ankylosis can originate as a consequence of traumatism, or as a result of local or general systemic infections, ankylosing spondilitis, rheumatoid arthritis, or psoriasis.9-11 In trauma caused cases the proposed hyphotesis is the formation of an intrarticular hematoma, scarring and excessive bone formation, which all produce hypomobility.10,12 The majority of infections causing temporomandibular ankylosis are a result of contiguity dissemination as a result of mastoiditis or media otitis.13 The most common cause of TMJ ankylosis is the macrotraumatism associated with the fracture of the condylar process during early childhood growth stages.1,2
Ankylosis can also be classified according to location (intra-articular or extra-articular) according to type of tissue involved (bone, fibrous or fibrous-bone) or the extension of the fusion (complete or incomplete). Pseudoankylosis affects extraarticular structures (muscular hyperactivity, hyperplasia of coronoid process, or a depressed fracture of the cygomatic arch.14 Sawhney (1986),15 classifies TMJ ankylosis into four types:
a) Type I. Minimum bone fusion but extensive fibrous adhesions around the articulation.
b) Type II. Larger bone fusion specially on the exterior border of the articular surface. In these cases there is no fusion in the medial zone of the articulation.
c) Type III. There is a bone bridge between lower jaw and temporal bone;
d) Type IV. A bone mass substitutes the articulation.
Indications for the reconstruction of the TMJ are well defined. We can count the following: ankylosis, severe osteoarthritis, rheumatoid arthropathy, neoplasic condition, posttraumatic dysfunctions, congenital conditions and condylar necroses.16
Controversy still reigns when deciding upon a reconstruction method; many techniques have been described, with autologous grafts (fibula, metatarsus, clavicle illiac crest and costochondral) or alloplastic grafts (acrylic, synthetic fibers silicon and complete articular systems).3
The complications that can arise include: fracture, reankylosis morbidity of donor site, graft variable growth behavior and temporary facial paralysis.17
Surgical technique
Incision is made at the junction of the facial skin with the helix of the auricular pavillion. We extend the incision from the upper area of the helix to the lower part of the tragus. The incision is performed through the skin, subcutaneous cellular tissue (including temporoparietal fascia) up to the temporal fascia (superficial layer). We perform a retraction or ligature of vessels before proceeding to the dissection towards the deeper tissues.18 We perform a dull dissection in the upper section of the incision (the section found above the cygomatic arch) so that the flap can be retracted anteriorly in about 1.5 to 2 cm. This flap is anteriorly dissecated to the level of the superficial layer of the temporal fascia (above the fascia). Temporal vessels and the auricular temporal nerve are anteriorly retracted along with the flap. Under the cygomatic arch, dissection proceeds in a dull fashion next to the external auditory canal, in a avascular plane located between this canal and the parotid gland. The dept of the dissection at this point must be similar to the one achieved in the cygomatic arch.16
We return once more to the portion of the incision located above the cygomatic arch. Once the flap is anteriorly retracted, an incision is made through the superficial layer of the temporal fascia at a 45 degree angle starting from the root of the cygomatic arch to a point located 2 mm above the cygomatic arch, with a depth reaching the adipose filling of the temporal region.2 The fatty tissue found between superficial and deep layers of the temporal fascia is thus exposed. At the root of the cygomatic arch, the incision can be performed through the temporal fascia and the periostium of the cygomatic arch. At this plane we insert a periostium elevator, deep to the superficial layer of the temporal fascia. Movements from front to back are performed, dissecting towards the cygomatic arch. Once this dissecction is performed, we remove periostium from the lateral face of the cygomatic arch. We continue dissecting downwards, care being given not to dissect towards the medial section and perforate thus the articular capsule. Once the dissection is approximately at 1 cm under the cygomatic arch, we incise the tissue vertically (in front of the external auditory canal).18
The flap is totally retracted towards the anterior section. This flap is going to include superficial temporal fascia, fat, periostium and the temporal and cygomatic branches of the facial nerve. The dull dissection continues anteriorly until we expose the articular eminence. We incise the articular capsule thus exposing the ankylosed articulation (Figure 1a). We then proceed to the liberation of the articulation with a resection of the bone tissue through the use of low speed rotating instruments under continual irrigation with physiological solution.We perform then the osteotomy without completing the medial section. The osteotomy is performed using an ostothome. Nevertheless, in this case the elimination of the medial remains was performed with an ultrasonic device (Piezosurgery® Inc, Columbus, Ohio) which offered the following advantages; a micrometric cut which allows for maximum intraoperatory precision and security while inflicting minimum tissue damage. It equally allows for a selective incision since the vibration frequency it operates on is optimum for mineralized tissues and does not cut soft tissue. If incision of soft tissues is required, other frequencies would be needed. We obtain thus a clean surgical field which offers maximum intraoperative visibility. The high accuracy of its cut is due to the restricted scope of its micrometrical vibrations, which are only going to work on hard tissue. This allows for a osteotomy bearing no risk to injure blood vessels, nerves, and soft tissue, regardless of how close they might be.19-22 This ankylosed bone tissue must be eliminated (Figure 1b) leaving a 1.5 to 2 cm space between articular cavity and ascending branch. We must be sure to have totally eliminated the ankylosed tissue. Finally we have to verify the medial section of the region, since in this the zone, due to poor visibility, there is more risk of leaving rests of ankylosed bone tissue. This can be considered one of the causes or relapse.
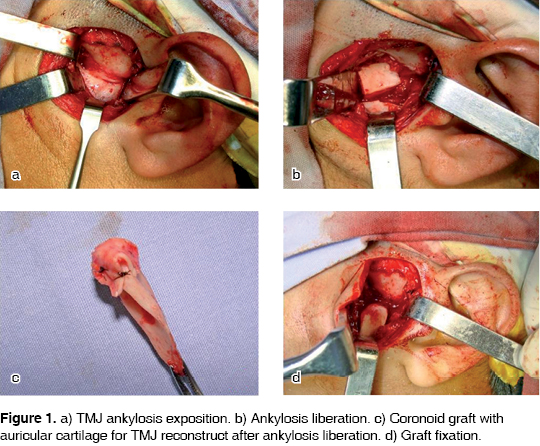
As a last step, the area is totally irrigated. We then carry on with performing opening and closing mandibular movements to verify that the articulation can move freely. When movements can not be carried out freely, we move to perform an ipsilateral coronoidectomy. If after this, movement is still restricted, we perform a contralateral coronoidectomy.12,23 We remodel the glenoid fossa and the coronoid process in cases when we are using it as a graft.23
We obtain the auricular cartilage through a 3 x 4 cm incision in the auricular posterior zone, along the rim of the auricular a shell. The proximal section of the cartilage is removed mantiaining the antihelical rim. The perchondrium is kept adhered to the convex surface of the graft. This turns out to be an advantage due to its chondrogenic potential. The removed cartridge is convex and it is fastened to the upper portion of the coroinoid graft with non absorbable suture (nylon). Once we have assembled the graft (Figure 1c) it is fixed to the ascending mandibular branch with osteosynthesis material.23 (Figure 1d).
After all this, the lower jaw is manipulated to assess the mobility degree. It is closed by planes and a soft drain is left, to be removed on the next day.24
CLINICAL CASE
A 15 year old male patient arrives at the Maxillofacial and Oral Surgery Clinic of the Graduate School of the National University of Mexico. He seeks evaluation and treatment for he encounters difficulties when opening his mouth. The patient has been referred from the orthodontics department of the same school. The patient's mother informs that the affliction begins when the patient is 7 years old. He fell, and received direct impact in the mandibular symphyseal zone, this ocurred approximately eight months before the complaint began. The patient was taken to a private doctor who discarded any mandibular fracture. After this, the patient began to experience a gradual decrease in his ability to opening the mouth. When the patient is clinically explored, he presents facial assymetry, showing a mandibular midline deviation towards the left. He also shows shorter left mandibular length when compared to the right. He presents as well retrognatia with class II occlusion and 10 mm mouth opening with left mandibular deviation when opening the mouth. He also presents inclination of the occlusal plane (Figures 2a, b, c). Skull frontal and lateral panoramic X rays are requested (Figure 2d). When these are performed, we observe a lesion compatible with left TMJ ankylosis. We arrive to a diagnosis of left temporomandibular joint ankylosis. We request computarized tomography studies (Figure 2e). We equally request a stereolithography of the patient's skull to be able to determine the extension of the ankyloses and the planning of the surgical treatment.
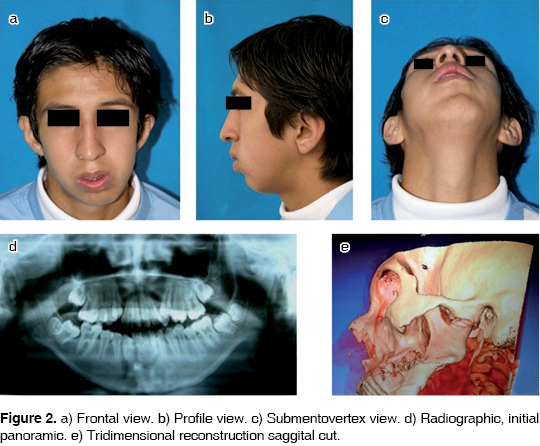
The computarized tomography reveals a type III Sawhney temporomandibular ankyloses. The patient is programmed for liberation of the articulation. The procedure is performed under general anesthesia, balanced with intubation under fiberscope. The procedure includes reconstruction of the condyle branch lower unit, with the graft of the coronoid process and the auricular cartilage.
Surgical procedure
We carry out a preauricular approach, we liberate the ankyloses, and the bilateral coronoidectomy, until we achieve unimpeded opening of the mouth. We then take an auricular cartilage graft and we fix the remodelled coronoid process. Once we assemble the graft, we secure it with two titanium bicortical screws (Walter Lorenz Surgical Inc, Gainesville, Florida), and we proceed to suture by planes. Immediate postoperative care includes the following: analgesics, antibiotics and intermaxillar fixation for two weeks. These steps are followed by a course of physiotherapy for 4 to six weeks directed at the patient performing vertical and horizontal mandibular movements. Then follow exercises to increase oral opening, through the placement of a tongue depressor between upper and lower teeth.14 Nine months later, at the postoperative control visit, the patient shows a 45 mm mouth opening (Figure 3a-d). Facial gesticulation is not compromised.
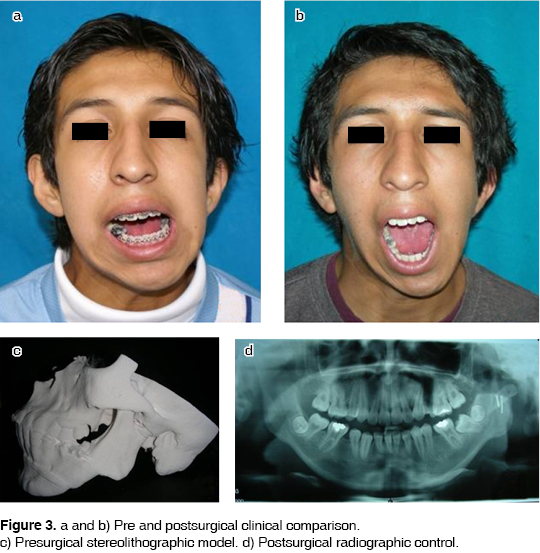
To prepare the patient for the surgical correction of his facial disharmony, he is kept under orthopedic and orthodontic treatment.
DISCUSSION
There are several schemes for the treatment of temporomandibular joint ankyloses. These schemes are geared to liberate the ankyloses and reconstruct the condyle with an autologous or alloplastic graft. Traumatism is the main cause for this pathology. Roydchoudhury,24 reported that TMJ traumatism is the etiological factor in 86% of the cases. It is therefore important to early detect this traumatism, and to treat it immediately, so as to be able to restore mandibular movement and proper nutrition and to diminish the dentofacial disharmony which could develop in the patient thus afflicted.25-28 The success and reankyloses prevention after an TMJ reconstruction, depends also on a long term patient cooperation to perform frequent mandibular exercises.10,28
The surgical approach performed in this case was carried out according to guidelines described by Al-Kayat A, Bramley P.29 In these guidelines they stress the clinical importance of the zone to approach over the cygomatic arch. They show that the temporal branch of the facial nerve lies in this condensation tissue area at an averaqge distance of 2 cm taken from the concavity in front of the external auditory canal, and presents a range of 0.8 to 3.5 cm.
Costochondral autologous grafts have been used as substitutes for the mandibular branch and condyle.30 Many studies have shown that, in children, costochondral grafts have the potential to grow.31,32 It has also been shown that umpredictable growth can occur,which sometimes warrants a second surgical intervention.33,34 The coronoid processes of patients with long standing evolution of TMJ ankyloses tend to be longer and thicker. For this reason they can be used as substitutes for mandibular condyles. Takatsuka et al,35 found that in rabbits, the condyle and its function can be substituted by an auricular cartilage graft after the discectomy of craniomandibular articulations. The auricular cartilage covers the condylar surface, precluding the onset of reankyloses. Tucker36 informed that in monkeys, the interpositional placement of auricular cartilage after a discectomy and shaving of the upper section of the condyle, the cartilage survived, and the degenerative changes or the articulation were less, than in the control side, where no auricular cartilage was placed. Thus the recurrence of ankyloses was avoided. In immediate and late postoperative periods, morbidity of the donor site was not observed.
Based on the fact that our patient was 15 years old, on the length and thickness of the coronoid process and on the fact that the patient required a coronoidectomy, we decided to use an auricular cartilage remodelled coronoid process as substitute of the mandibular condyle. We thus decrease the morbidity of the procedure.
A nine month postoperative follow up of our patient shows a 45 mm oral opening and malocclusion as consequence of the ankyloses. Radiographically, we observe the integration of the coronoid process graft.
CONCLUSION
TMJ ankylosis must be timely diagnosed and treated as soon as possible. There are several treatment schemes for the treatment of temporomandibular joint ankylosis. A good option for the patient no longer in growth period, is the liberation of the ankylosis followed by reconstruction with coronoid process and auricular cartilage. This is due to the small degree of morbidity and the success rate encountered. An appropiate surgical approach restricts potential complication risks such as damage to nerve and vascular structures. The use of ultrasonic instruments decreases damage to any of these tissues.
REFERENCES
 Address correspondence:
Address correspondence:
Rafael Ruiz MD
Cda. Félix Cuevas 38-101
Col del Valle,
03100 México, D.F.
Nota
This article can be read in its full version in the following page: http://www.medigraphic.com/facultadodontologiaunam
1. MacIntosh RB, Henny FA. A spectrum of application of autogenous costochondral graft. J Maxillofac Surg 1977; 5: 257. [ Links ]
2. Freihofer HP, Perko MA. Simultaneous reconstruction of the area of the temporomandibular joint including the ramus of the mandible in a postrauma case. J Maxillofac Surg 4: 124, 1976 Burstone CJ: Cephalometrics for orthognathic surgery. J Oral Surg 1987; 36: 269, 1987. [ Links ]
3. Hensher R. Treatment of temporomandibular joint ankylosis. In: Langdon J, Patel M (eds.), Operative Maxillofacial Surgery, London: Chapman and Hall Medical, 175–186, 1998. ISBN: 0412560003.
4. Topazian RG. Comparison of gap and interposition arthroplasty in the treatment of temporomandibular joint ankylosis. J Oraln Surg 1966; 24: 405. [ Links ]
5. Okeson, Jeffrey P. Management of tempomandibular disorder and occlusion. 5ta Edición. Editorial Mosby USA. 2003: 117-136 [ Links ]
6. Guven O. Treatment of temporomandibular joint ankylosis by a modified fossa prosthesis. J Cranio Maxillofac Surg 2004; 32: 236-242. [ Links ]
7. Karaca C, Barutcu A, Baytekin C, Yilmaz M, Menderes A, Tan O. Modifications of the inverted T-shaped silicone implant for treatment of temporomandibular joint ankylosis. J Cranio Maxillofac Surg 2004; 32: 243-246. [ Links ]
8. El-Sheikh MM. Temporomandibular joint ankylosis: the Egyptian experience. Ann Roy Coll Surg Engl 1999; 81: 12-18. [ Links ]
9. Valentini V, Vetrano S, Agrillo A, Torroni A, Fabiani F, Iannetti G. Surgical treatment of TMJ ankylosis: our experience (60 cases). J Craniofac Surg 2002; 13: 59-67. [ Links ]
10. Kaban LB, Perrott DH, Fisher K. A protocol for management of temporomandibular joint ankylosis. J Oral Maxillofac Surg 1990; 48: 1145-1151. [ Links ]
11. Mangenollo-Souza LC, Mariani PB. Temporomandibular joint ankylosis: report of 14 cases. Int J Oral Maxillofac 2003; Surg 32: 24-29. [ Links ]
12. Faerber H, Ennis RL, Allen GA. Temporomandibular joint ankylosis following mastoiditis: report of a case. J Oral Maxillofac Surg 1990; 48: 866-870. [ Links ]
13. Behc, Rezzan Tanrikulu, Belgin Go. A clinical study on ankylosis of the temporomandibular joint. Journal of Cranio-Maxillofacial Surgery 2006; 34: 100-106. [ Links ]
14. Raymond JF. Oral and maxillofacial surgery . Vol. 4, USA, Pennsylvania: Edit W.B. Saunders; 2000. [ Links ]
15. Raymond JF. Oral and maxillofacial surgery. USA, Pennsylvania: Edit W.B. Saunders; 2000; 4: 375-397. [ Links ]
16. Sawhney CP. Bonyanky losis of the temporomandibular joint: follow-up of 70 patients treated with arthroplasty and acrylic spacer interposition. Plast Reconstr Surg 1986; 77: 29-40. [ Links ]
17. Obeid GG, Connole PW. Costochondral grafting in condylar replacement and mandibular reconstruction. J Oral Maxillofac Surg 1988; 46: 177-182. [ Links ]
18. Saeed NR, Kent JN. A retrospective study of the costochondral graft in TMJ reconstruction. Int J Oral Maxillofac Surg 2003; 32: 606-609. Elsevier. [ Links ]
19. Ellis E. Surgical approaches of the facial skeleton . 2nd Edition. Editorial Lippincott Williams & Wilkins. 2006 USA. [ Links ]
20. Gruber RM. Ultrasonic surgery an alternative way in orthognathic surgery of the mandible. Int J Oral Maxillofac Surg 2005; 34: 590-593. [ Links ]
21. Robiony M. Ultrasonic bone cutting for surgically assisted rapid maxillary expansion (SARME) under local anaesthesia. Int J Oral Maxillofac Surg 2007; 36: 267-269. [ Links ]
22. Stübinger S. Intraoral piezosurgery: Preliminary results of a new technique. J Oral Maxillofac Surg 2005; 63: 1283-1287. [ Links ]
23. Koichiro UEKI. Le Fort I osteotomy using an ultrasonic bone curette to fracture the pterygoid plates. Journal of Cranio-Maxillofacial Surgery 2004; 32: 381-386. [ Links ]
24. Hong Yong Long. Modified coronoid process grafts combined with sagittal split osteotomy for treatment of bilateral temporomandibular joint ankylosis. J Oral Maxillofac Surg 2002; 60: 11-18. [ Links ]
25. Roychoudhury A, Parkash H, Trikha A. Functional restoration by gap arthroplasty in temporomandibular joint ankylosis: a report of 50 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1999; 87: 166-169. [ Links ]
26. Fortunato MA, Fielding AF, GuernseyLH. Facial bone fractures in children. Oral Surg Oral Med Oral Pathol 1982; 53: 225-230. [ Links ]
27. Alexander RW. Improvement of facial symmetry after operative relief of bony ankylosis of the jaw at the age of 10 years. Case report. Plast Reconstr Surg 1978; 62: 896-901. [ Links ]
28. El-MoftyS. Cephalometric studies of patients with ankylosis of the temporomandibular joint following surgical treatment. Oral Surg Oral Med Oral Pathol 1979; 48: 92-96. [ Links ]
29. Farmand M, Mommaerts M, Teuscher U. Facial growth after treatment of unilateral temporomandibular joint ankylosis in childhood without growth centre transplantation. A serial cephalomorphometric study. J Craniomaxillofac Surg 1989; 17: 260-270. [ Links ]
30. Al-Kayat A, Bramley P. A modified pre-auricular approach to the temporomandibular joint and malar arch. Br J Oral Surg 1979; 17: 91. [ Links ]
31. Lindqvist C. Adaptation of autogenous costochondylar grafts used for temporomandibular joint reconstruction. J Oral Maxillofac Surg 1988; 46: 465. [ Links ]
32. MacIntosh RB, Henny FA. A spectrum of application of autogenous costochondral graft. J Maxillofac Surg 1977; 5: 257. [ Links ]
33. Lindqvist C, Pihakari A, Tasanen A et al. Autogenous costochondral grafts in temporomandibular joint arthroplasty: A survey of 66 arthroplasties in 60 patients. J Oral Maxillofac Surg 1986; 14: 143. [ Links ]
34. Fukata K, Jackson IT, Topf JS. Facial lawn mower injury treated by a vascularized costochondral graft. J Oral Maxillofac Surg 1992; 50: 194. [ Links ]
35. Munro IR, Phillips JH, Griffin G. Growth after construction of the temporomandibular joint in children with hemifacial microsomia. Cleft Palate J 198; 26: 303. [ Links ]
36. Takatsuka S, Narinobou M, Nakagawa K et al. Histologic evaluation of auricular cartilage grafts after discectomy in the rabbit craniomandibular joint. J Oral Maxillofac Surg 1996; 54: 1216. [ Links ]











 text in
text in 


