Introduction
Oral diseases may affect not only a child’s quality of life, but also their emotional and physical wellbeing, cause pain, and may negatively influence a child’s growth.1In Mexico caries prevalence is still high.2According to the 2015 Mexican Oral Health Survey, only 25.0% of the children and adolescents from 2 to 19 years of age are free of caries and at least 16.0% of children around 10-14 years of age have gingival bleeding and calculus.3
It is well known that both dental caries and gingivitis have a common risk factor, a deficient oral hygiene. Consequently, improvement of children’s oral self-care must be targeted.4 Conventional educational methods like didactic dental instruction provided by teachers or health professionals have been used to change oral health behaviours in children.5Such instructions mainly provided dental knowledge, unsurprisingly no long-term behavioural changes were observed. Consequently, alternative approaches to dental education should be examined.6
Schools have an established infrastructure for education that could also be used for health education since schools constitute an environment where children not only are expected to learn but also engage actively with their peers.7School-based health promotion has been successfully used in both medical and dental studies.8,9,10,11
Alternative strategies for health promotion include Lay Health Advisors (LHAs) that are non-medical persons having personal connections with their community. LHAs are trained by health care professionals to become health educators to promote health in their own respective groups.12It has been suggested that LHA school-based peer-led education is an effective method, since information is more easily shared between children of a similar age.13 Previous research has shown that school-based peer-led education delivered by teachers was as effective as the health education provided by dental professionals.13,14We believe that children can also be educated as LHAs to become peer leaders and by attributing them such roles we can also expect their empowerment. Placing children in a leadership role when they are young can increase their self-esteem, self-efficacy, and self-empowerment; therefore, improving not only their own dental behaviours but also their feeling of wellbeing. It can also be expected that the peers they educate will be positively pressured socially to be healthy. 15
Study hypothesis. A peer-led dental education program for Mexican children will improve oral self-care more than conventional dental instruction.
Materials and methods
The study was approved by the Ethics Board of the National School of Higher Education, National Autonomous University of México (CE_17/005). The Consort diagram outlining the study process is presented in figure 1. Through the Public Educational Authorities of Leon, one of the main municipalities in Guanajuato, Mexico, eleven registered public schools were invited to participate. Four of them were chosen since they shared the same school zone and therefore had similar socio-economic characteristics (recruitment rate of 36.4%). The remaining seven schools had rural characteristics that could have influenced the results of the intervention, therefore they were not included. The current study adopted a cluster (schools-based) randomized controlled trial study design with two observation periods (baseline and after education). The sample size calculation showed that we needed a minimum of 100 children per group based on the following: a pooled variance of 0.25, 80% power, a=0.05, a minimum mean 20% difference, and a potential 15% loss to follow-up.
Allocation into study groups. All children from grades four to six with an informed parental consent agreed to participate. A random cluster allocation into study groups was performed: a control group and an intervention group each consisted of two schools. Both control and intervention groups received screening for dental treatment needs. Dental caries status was registered using the DMFT/dmft index following the indications given by the World Health Organization (WHO).16 Besides two outcome assessments were obtained: oral self-care practice (OSC-P) and oral self-care skills (OSC-S). All parents received a report of their children’s oral condition. Two types of dental education for children were used. Children from the intervention schools received a child-focused dental education consisting of a peer-led oral health education program, while children from the control group received conventional dental instruction. Data was collected from June, 2016 to July, 2017.
Study variables. Sociodemographic data including sex, age and education of the mother was reported by parents through a self-response questionnaire. Information about dental treatment needs (reported by a pediatric dentist) were collected. Two study outcomes were chosen: quality of OSC-P and of OSC-S, both indicated by dental plaque levels (%). To assess both outcomes, a TRACE disclosing solution was used to highlight dental plaque-covered areas. For assessments of OSC-P or alternatively OSC-S, a total of six photos of teeth with disclosed plaque (three per jaw: right buccal, central buccal, left buccal) were taken. Without giving any instruction, the first set of photos of teeth with disclosed plaque was used to evaluate the quality of OSC-P. To acquire information about OSC-S, each child was asked to demonstrate his or her best tooth brushing. Subsequently, the disclosing solution was reapplied to highlight plaque-covered areas and the second set of photos was taken in the same way as for the assessments of OSC-P.
The quality of oral self-care (skills or practice) was calculated for each child as a percentage of a total buccal tooth area covered with dental plaque. These percentages were calculated digitally employing the Adobe Photoshop program, counting the number of pigmented pixels and dividing them by the number of pixels of the total dental area. This method has been used previously on similar studies.17,18 To ensure blinded assessments of oral self-care, all photos of teeth with plaque were coded prior to their evaluations.
Types of dental education. The control group received a 20 minutes class-based oral presentation covering caries etiology and the importance of self-care and regular dental attendance. This lecture was provided in each classroom by one pediatric dentist, using teaching aids such as flipcharts and images.
In the intervention schools, teachers of sixth graders were asked to select 15 students to become peer leaders based on their academic achievement and ability to socialize. Peer leaders received dental training consisting of two sessions during which a dentist explained causes of oral diseases, how dental caries can be prevented, and how to perform proper oral self-care. A randomly selected small group of seven fourth and fifth graders was designated to each peer leader. The role of peer leaders was to instruct their “younger buddies” about cariogenic and non-cariogenic foods/drinks and the importance of oral self-care. Each peer-leader engaged their group of younger peers after the lunch break in daily tooth brushing. This peer-led education was discontinued after one month. The three-month follow-up was similar to the baseline assessments and consisted of the OSC-P and OSC-S assessments.
Statistical analyses. All the analyses were performed using the Statistical Package for the Social Sciences (IBM SPSS Statistics 22.0) and the threshold for statistical significance was set at p<0.05. Intra- and inter-examiner reliability was tested using a set of 30 randomly selected photos. Both examiners assessed this set of photos twice with one week in between these duplicate assessments. The Intraclass Correlation Coefficient (ICC) for the intra-examiner reliability was >0.96 for both examiners and the ICC for the inter-examiner reliability was 0.92.
An independent sample t-test compared means of dental plaque levels between the intervention and control groups and a paired sample t-test compared means between the baseline and the three-month observation within the same group.
Linear multiple regression (LMR) models were used to evaluate the joint effect of multiple predictors (baseline oral self-care levels, group affiliation, gender, age, and mother’s education) to explain the variation in OSC-P, or alternatively in OSC-S observed at the three-month follow-up point.
Results
The follow-up rate was 87.7% (figure 1). In the control group it was 88.1% and in the intervention group it was 97.3%. Children participants were mainly lost due to a change of schools and all children present during data collection agreed to a follow-up.
Table I presents sociodemographic comparisons. There were no significant proportional differences among the intervention, control and drop-outs groups in regards to gender, however the results on mother’s education are at the statistical borderline. Results on DMFT/dmft are shown in Table I.
Table I Description of the population by sociodemographic* and clinical variables‡ in Mexican school-aged children. Mexico, June 2016-July 2017
| Sociodemographic characteristics | Intervention group N (%) | Control group N (%) | Drop-outs N (%) | Significance p | ||||
| Child´s gender | ||||||||
| Girls | 95 (51.1) | 120 (60.3) | 30(54.5) | .207 | ||||
| Boys | 91 (48.9) | 79 (39.7) | 25(45.5) | |||||
| Mother´s education | ||||||||
| Primary school | 52 (28.0) | 74 (37.2) | 23(41.8) | .054 | ||||
| ≥High school | 134 (72.0) | 125 (62.8) | 32-(52.8) | |||||
| Mean SD | Mean SD | Mean SD | Significance p | |||||
| Age | 9.9±.97 | 10.1±.89 | 9.9±.99 | .064 | ||||
| DMFT | 2.4±2.4 | 2.0±2.4 | 1.7±2.1 | .131 | ||||
| dmft | 1.2±1.5 | 1.6±1.6 | 1.6±1.4 | .053 | ||||
| DMFT/dmft | 3.7±3.2 | 3.8±3.0 | 3.3±2.8 | .550 | ||||
*Chi-square test
‡Anova test
DMFT: Decayed, missing, filled teeth
Vertical comparisons in Table II compare outcomes between the two groups and horizontal comparisons compare outcomes between two different observation periods within the same group. The between group comparisons of the 1st study outcome (OSC-P) showed no statistically significant (p=0.757) baseline differences (measurement: dental plaque level (%)) between the control group (55.8 ± 12.8%) and the intervention group (55.5 ± 14.6%). At the three-month follow-up there were statistically significant (p<0.001) differences in OSC-P between the control group (63.2 ± 15.0%) and the intervention group (52.2 ± 15.6%).
Table II Oral self-care practice /skills in elementary Mexican school-aged children. Comparisons between the baseline and three months follow-up. Mexico, June 2016-July 2017
| Baseline | 3 months follow-up | Significance* | ||||
| mean ± sd | mean ± sd | |||||
| Oral self-care practice | ||||||
| Control group (n=199) | 55.8 ± 12.8 | 63.2 ± 15.0 | p<.001 | |||
| Intervention group (n=186) | 55.5 ± 14.6 | 52.2 ± 15.6 | p=.014 | |||
| Significance‡ | p= .757 | p<.001 | ||||
| Oral self care skills | ||||||
| Control group (n=199) | 38.1 ± 12.5 | 39.4 ± 12.3 | p=.222 | |||
| Intervention group (n=186) | 38.5 ± 13.2 | 32.5 ± 12.0 | p=.001 | |||
| Significance‡ | p= .758 | p<.001 | ||||
*Paired sample t test
‡Independent sample t test
Examination of the within-group before/after differences (horizontal comparisons) of OSC-P showed that in the control group, mean dental plaque levels significantly (p<0.001) increased from the baseline (55.8 ± 12.8%) to the three-month follow-up point (63.2 ± 15.0%).
In the intervention group, mean dental plaque levels significantly (p=0.014) decreased from the baseline (55.5 ± 14.6%) to the three-month follow-up (52.2 ± 15.6%).
The vertical comparisons of the 2nd study outcome (OSC-S) showed that at the baseline there were no statistically significant (p=.758) mean differences in OSC-S (measurement: dental plaque levels (%)) between the control group (38.1 ± 12.5%) and the intervention group (38.5 ± 13.2%). At the three-month follow-up, there were statistically significant differences (p<.001) in OSC-S between the control group (39.4 ± 12.3%) and the intervention group (32.5 ± 12.0%).
The before/after within-group comparisons of OSC-S (Table II) showed that in the control group there was a slight non-significant (p=.222) increase in mean dental plaque levels from the baseline (38.1 ± 12.5%) to the three-month follow-up point (39.4 ± 12.3%). In the intervention group, mean dental plaque levels significantly (p<.001) decreased from the baseline (38.5 ± 13.2%) to the three-month follow-up point (32.5 ± 12.0%).
The sample distribution according to OSC-P outcome is visualized in figure 2 and distribution according to OSC-S in figure 3. In both figures, for both study groups, dental plaque levels are compared at two observation periods (baseline, three-month follow-up). In figure 2, one can see that there was a substantial within-group variation in both study groups and at both observation periods. Overall, there was less withingroup variation in OSC-S (figure 3) as compared to OSC-P (figure 2). In the control group, the distributional pattern of OSC-S did not change from the baseline to the three-month follow-up, while in the intervention group a slight improvement of OSC-S was observed, as indicated by lower levels of dental plaque observed at the follow-up than at the baseline (figure 3).
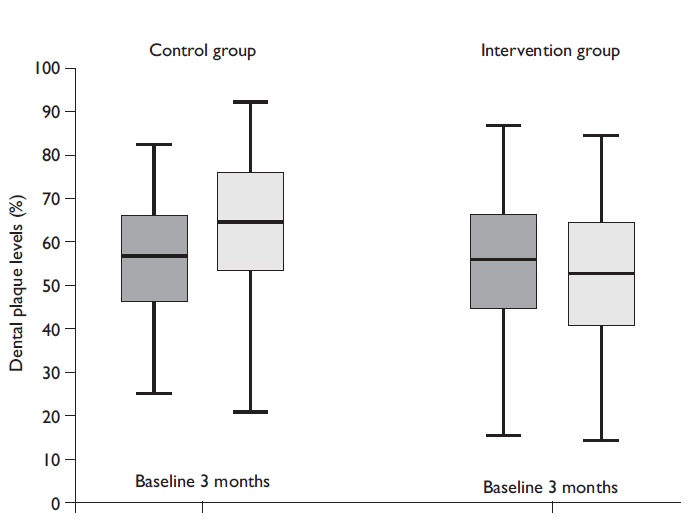
Figure 2 Oral self-care practice comparison between the baseline and three months follow-up in Mexican school-aged children. Mexico, June 2016-July 2017

Figure 3 Oral self-care skills comparison between the baseline and three months follow-up in Mexican school-aged children. Mexico, June 2016-July 2017
Table III presents results of two linear multiple regression (LMR) models, where predictors for both outcomes were studied: one being OSC-P at the three month follow-up point and the second outcome was OSC-S at the three-month follow-up point.The “enter” selection method was used to introduce the following predictors: baseline oral self-care levels, group affiliation, gender, and mother’s education. High tolerance values (all around 0.9 or higher) indicated that the assumption for the independence among multiple predictors was fulfilled in both models. The significant predictors of the outcome “OSC-P at the three-month follow-up” were: baseline OSC-P (β= .28, p<.001), group affiliation (β= .35, p<.001), and mother’s education (β=.10, p=.030). The LMR model for OSC-P was highly significant (p<.001) and predictors jointly explained a total of 20.0% (Adjusted R2 value) of the variation in OSC-P observed at the three-month follow-up point. Similarly, to the first LMR model, the LMR model for the outcome “OSC-S at the three-month follow-up” identified three significant predictors: baseline OSC-S (β= .25, p<.001), group affiliation (β= .31, p<.001), and mother’s education (β= .13, p=. 005). This model was also highly significant where predictors jointly explained 16.2% of the variation in OSC-S observed at the threemonth follow-up point.
Table III Linear Multiple Regression Models for Oral Self-Care Practice/Skills in Mexican school-aged children. Mexico, June 2016-July 2017
| Predictors | β (significance) | B (95% CI) | Tolerance | |||
| Outcome: Oral self-care practice (3 months) | ||||||
| Oral self-care practice (baseline) | .28 (p< .001) | 0.33 (0.22; 0.44) | .986 | |||
| Group affiliation | .35 (p<.001) | 11.50 (8.53; 14.50) | .969 | |||
| Gender | .06 (p=.192) | 2.04 (-0.93; 5.01) | .980 | |||
| Age | -0.03 (p=.495) | -0.60 (-2.14; 1.03) | .979 | |||
| Mother´s education | .10 (p=.030) | 3.50 (0.33; 6.60) | .983 | |||
| Model summary: Adjusted R2= .200 p<.001 | ||||||
| Outcome: Oral self-care skills (3 months) | ||||||
| Oral self-care skills (baseline) | .25 (p<.001) | 0.24 (0.15; 0.33) | .975 | |||
| Group affiliation | .31 (p<.001) | 7.80 (5.43; 10.13) | .970 | |||
| Gender | .07 (p=.127) | 1.82 (-0.52; 4.17) | .987 | |||
| Age | -0.08 (p=.097) | -1.10 (-2.34; 0.19) | .959 | |||
| Mother´s education | .13 (p=.005) | 3.54 (1.05; 6.03) | .985 | |||
Summary: Adjusted R2= .162 p<.001
Discussion
The current study compared two types of dental education: a peer-led dental education delivered by older children to their peers (intervention group) and conventional dental instruction presented by a dental professional (control group). Both types of dental education have shown an improvement of oral self-care in school-aged children.19
Our peer-led dental education, where older children served as dental health educators for their younger peers, was designed following the Lay Health Advisors (LHAs) model which was successful in other health interventions. The main difference between the LHA strategy for health promotion and other health promoting interventions is related to the delivery of health education. In LHA-based strategies the role of health education is delegated to trained non-medical professionals (older children in the current study), while in other interventions health education is commonly provided by medical professionals.20,21Although LHA-based strategies may require more time than other conventional methods, they have several advantages. They may have the potential to reduce the overall cost of health intervention. They may additionally benefit those receiving health education since LHAs are usually selected from the target group. LHA-guided health education may also lead to better engagement and a more direct approach for those being educated. The LHA-guided health interventions are also in accordance with several psychological theories targeting behavioural changes that focus on specific needs and consider specific characteristics of a targeted audience as a key to success.14
In the current study, we compared two types of oral self-care related outcomes between the two study groups at two different observation periods. Examination of OSC-P (outcome 1) allowed us to evaluate the overall quality of a child’s oral hygiene, while the assessment of OSC-S (outcome 2) helped us to evaluate the skills necessary for performing proper oral hygiene. In order to acquire valid information about both oral self-care related outcomes we organized data collection for the baseline and follow-up assessments at times not-announced in advance either to children or to their teachers.
Our study hypothesis that a peer-led dental education program for children would improve OSC-P and OSC-S better than conventional dental instruction was confirmed. As expected, we observed more improvement in OSC-S than in OSC-P. Seemingly, children do not practice daily oral self-care to the best of their ability. Another important observation of the current study is that both the quality of OSC-P and skill level was deficient in Mexican school-aged children.
Our study, similarly to other studies,22,23,24confirmed that conventional dental instruction is not the most efficient strategy for improving children’s oral self-care. An important implication of the present findings is how they can be applied in clinical dentistry. Given that a regular dental visit pattern consists of two annual follow-ups, conventional dental instruction consisting of short oral instruction (given at best twice a year) will be insufficient for effective dental health education, at least for high risk children. Therefore, for dental practitioners treating children, we recommend an increased focus on high risk children and as a first step targeting the improvement of OSC-S. This way, dentist might also observe an improvement in OSC-P. Another important finding was that the mother’s education was a significant predictor of oral self-care even after controlling for the baseline oral self-care levels and the type of dental education. This association between mother’s education and child’s oral self-care was expected, as there is ample evidence associating lower parental socioeconomic status with caries in children.25,26,27,28
We chose digital calculations of dental plaque levels for the assessments of oral self-care. We recommend this measurement method for other studies because it has several advantages. First, our interval scale measurement of dental plaque levels (theoretical range 0-100%) has an increased level of precision as compared to commonly applied categorical oral hygiene measurements.29 Second, our digital dental plaque estimation method showed both a high level of intra- and inter-examiner reliability. Third, the digital estimation of plaque will be a better and more precise method for monitoring changes in oral self-care over time. Fourth, this digital method allows blinded assessments of oral self-care, as an ability to ensure blinded outcome assessment in interventional studies increases both internal and subsequently external validity. Fifth, this method will be most suitable for field studies because plaque disclosing and subsequent photographing of teeth is a time-efficient procedure that takes approximately two minutes.
Our study limitations also need to be acknowledged. Although the assignment of the intervention was made considering the schools as clusters and not the individuals, avoiding the influence among the subjects who receive or not the intervention, the statistical analysis is carried out at an individual level, ignoring the variability coming from the clusters and assuming independent measures. However, the analysis based on clusters would have required a greater number of schools than those available.
Besides, given that we had only a short-term follow-up, we consider our loss to follow-up relatively high (12.3%). However, the ones we lost were due to children changing schools and not to children refusing health promoting interventions. Another limitation was that our recruitment rate of schools was relatively low, as only four of the eleven schools invited agreed to participate. Consequently, schools need to be better educated about the benefits of school-based health promotional programs, taking advantage of existing educational infrastructure.
School-based programs can be particularly relevant to target common risk behaviours by facilitating a collaboration of interdisciplinary teams towards health promotion.30
Conclusions
The study hypothesis suggesting that a peer-led dental education is superior to conventional dental instruction was confirmed. The significant predictors of children’s oral self-care at the three-month follow-up point were: oral self-care levels at the baseline, the type of education children received, and the mother’s education.











 text new page (beta)
text new page (beta)



