Services on Demand
Journal
Article
Indicators
Related links
Share
Salud Pública de México
Print version ISSN 0036-3634
Salud pública Méx vol.56 n.5 Cuernavaca Sep./Oct. 2014
Artículo original
Epidemiology of cervical cancer in Colombia
Epidemiología del cáncer cervical en Colombia
Nubia Muñoz, MD, MPH,(1) Luis Eduardo Bravo, MD, MSc.(2)
(1) Instituto Nacional de Cancerología. Bogotá, Colombia.
(2) Registro Poblacional de Cáncer de Cali. Cali, Colombia.
Abstract
Objective. To describe the incidence, mortality, time trends and prognostic factors for cervical cancer in Cali, Colombia, and to review the molecular epidemiological evidence showing that HPV is the major and necessary cause of cervical cancer and the implications of this discovery for primary and secondary prevention.
Materials and methods. Incidence rates of cervical cancer during a 45-year period (1962-2007) were estimated based on the population-based cancer registry of Cali and the mortality statistics from the Municipal Health Secretariat of Cali. Prognostic factors were estimated based on relative survival. Review of the molecular epidemiological evidence linking HPV to cervical cancer was focused on the studies carried out in Cali and in other countries.
Results. Incidence rates of squamous cell carcinoma (SCC) declined from 120.4 per 100 000 in 1962-1966 to 25.7 in 2003-2007 while those of adenocarcinoma increased from 4.2 to 5.8. Mortality rates for cervical cancer declined from 18.5 in 1984-1988 to 7.0 per 100 000 in 2009-2011. Survival was lower in women over 65 years of age and in clinical stages 3-4. Review of the molecular epidemiological evidence showed that certain types of HPV are the central and necessary cause of cervical cancer.
Conclusions. A decline in the incidence and mortality of SCC and an increase in the incidence of adenocarcinoma during a 45-year period was documented in Cali, Colombia.
Key words: cervical cancer; incidence; mortality; spatio-temporal analysis; survival; HPV; prevention; vaccines; straining; Colombia.
Resumen
Objetivos. Describir la tendencia temporal de la incidencia, mortalidad y los factores pronósticos del cáncer de cuello uterino en Cali, Colombia, y revisar la evidencia epidemiológica molecular que muestra que el VPH es la causa principal y necesaria del cáncer cervical y las implicaciones de este descubrimiento para la prevención primaria y secundaria.
Material y métodos. Se estimaron las tasas de incidencia de cáncer de cuello uterino durante un periodo de 45 años (1962-2007) con la información del registro poblacional de cáncer de Cali y las de mortalidad con las estadísticas de la Secretaría de Salud Municipal de Cali. Los factores pronósticos se estimaron sobre la base de la supervivencia relativa. La revisión de la evidencia epidemiológica molecular que une el VPH con el cáncer cervical se centró en los estudios llevados a cabo en Cali y en otros países.
Resultados. Las tasas de incidencia de carcinoma de células escamosas (SCC) por 100000 se redujeron desde 120.4 en 1962-66 a 25.7 en 2003-07, mientras que las de adenocarcinoma aumentaron desde 4.2 hasta 5.8. Las tasas de mortalidad por cáncer de cuello uterino por 100000 se redujeron desde 18.5 en 1984-88 a 7.0 en 2009-11. La supervivencia fue menor en las mujeres de más de 65 años de edad y en los estadios clínicos 3-4. La revisión de la evidencia epidemiológica molecular mostró que ciertos tipos de VPH son la causa central y necesaria del cáncer cervical.
Conclusiones. Se documentó la disminución de la incidencia y la mortalidad por SCC y un aumento en la incidencia de adenocarcinoma durante un periodo de 45 años en Cali, Colombia.
Palabras clave: cáncer cervical; incidencia; mortalidad; análisis espacio-temporal; supervivencia; VPH; prevención; vacunas; cribado; Colombia.
Worldwide, cervical cancer is the third most common cancer in women, and the second most common cause of death from cancer among women aged 14 to 44 years, both in developed and developing countries. The major burden occurs in the less developed world. From a total of 530 232 new cases that were estimated to have occurred in the world in 2008, 453 531 cases (86%) were diagnosed in less developed countries.1 The main public health importance of cervical cancer in these countries lies in the fact that it affects relatively young and poor women, devastating not only the women themselves, but also their families. This cancer therefore reflects more than any other cancer the substantial inequities that exist in health. In Latin America, cervical cancer is the second most common cancer among women (after breast cancer) and it is the most important cause of years of life lost, despite the fact that it is a highly preventable disease. It is estimated that if preventive programs are not improved in the region, the annual number of cases diagnosed will increase from 68000 cases in 2008 to 126 000 in 2025.2
Colombia is a middle income country with a population of 46 million and a per capita annual gross national income of 10 249 dollars (adjusted for purchasing power parity) in 2008. Although Colombia is the third largest economy in Latin America after Brazil and Mexico, it exhibits a great deal of inequity in the region, and scores poorly according to the Gini coefficient (Gini index 56.0) which measures the degree of inequality in the family income.3 Great inequity exists regarding social development and access to health care in Colombia. It is not surprising then that cervical cancer remains in Colombia the first cause of cancer mortality and the second cause of cancer incidence among women,4 despite the existence of screening programs during the last three decades. In 2008 a total of 4 736 new cases were diagnosed for an adjusted incidence rate of 21.5 per 100 000. The same year, the mortality rate was 10.0 per 100 000.1
In this article, we will describe the incidence, time trends and prognostic factors for cervical cancer in Cali, Colombia, and review the molecular epidemiological evidence showing that HPV is the major and necessary cause of cervical cancer and the implications of this discovery for primary and secondary prevention of this cancer.
Materials and methods
Incidence rates and time trends of cervical cancer were assessed during a 45 years period (1962-2007) using the database of the population-based cancer registry of Cali and the mortality statistics from the Municipal Health Secretariat of Cali. Cali Cancer Registry was founded in 1962 and it is the oldest population-based cancer registry in Latin America.5 Cases of cervical cancer were coded by histological type according to the International Classification of Diseases for Oncology (ICD-O). For analysis, cases were grouped as follows: squamous-cell carcinoma (SCC) (ICD-O codes 8050–8082), adenocarcinoma (ADC) (ICD-O codes 8140–8550, 8560, and 8570), other (ICD-O codes 8800–8932, 8990, 8991, 9040– 9044, 9120–9134, and 9540–9581) and unspecified (ICD-O codes 8000–8004, 8010–8034, 9990).6
Age-specific rates for two age groups (25-49 and 50-74) and age-standardized rates of cervical cancer incidence and mortality were calculated by the direct standardization method, using the world standard population as a reference. To describe incidence and mortality trends by calendar period, we carried out joinpoint regression analysis using the Joinpoint Regression Software. The aim of the approach is to identify possible joinpoints where a significant change in the log-linear trend occurs. To obtain the estimated annual percent change (APC), a regression line was fitted to the natural logarithm of the rates using calendar year as the response.7 In describing trends, the terms "significant increase" or "significant decrease" signify that the slope of the trend was statistically significant (p<0.05). For non-statistically significant trends (p>0.05), we used the terms "stable" (APC between -0.5 and 0.5%), "non-statistically significant increase" (APC>0.5%), and "non-statistically significant decrease" (APC<-0.5%). All statistical tests were two sided. The relative survival analysis was restricted to cervix uteri cancer cases. Records were excluded when: the year of birth or death was unknown; individuals were younger than 30 or older than 85 when diagnosed; diagnosis was established either through autopsy or death certificate only (DCO); In general, survival time was calculated as the difference in days between the date of diagnosis and the date of last observation (date of death or December 31, 2001, whichever was earliest) to a maximum of five years. Relative survival after diagnosis was estimated from the individual tumour data, using the Hakulinen approach embedded in the US National Cancer Institute's publicly accessible SEER*Stat software. The expected survival rates used to calculate Cali relative survival estimates were derived, by single year of age up to 85, from sex-specific provincial life tables (1990 to 2001) provided by DANE.8
Results
A significant decrease in incidence of SCC and in cancers not otherwise specified was observed in both age groups (25-49 years and 50-74 years), and overall, and a significant increase in ADC was observed in women under 50 years of age (table I, figure 1). Incidence rates of SCC declined from 120.4 per 100,000 in 1962-1966 to 25.7 in 2003-2007 (with a significant annual percent change of -3.4), while those of adenocarcinoma increased from 4.2 to 5.8 (annual percentage change: 0.8).
Table II summarizes the time trends in mortality rates for cervical cancer estimated for the period 1984-2011. A significant decrease in both age groups (25-49 years and 50-74 years) was observed. The age-standardized mortality rate declined from 18.5 per 100 000 during 1984-1988 to 7.0 during 2008- 2011, with a significant annual percentage change of -4.2.
The estimates of the Relative Survival at one, three and five years for two quinquenial periods (1995-1999) and (2000-2004) were: 77% (95%CI 74-79), 56% (95%CI 53-59), 48% (95%CI 45-52] and 81% (95%CI 78-83), 61% (95%CI 58-65) and 57% (95%CI 53-61), respectively.
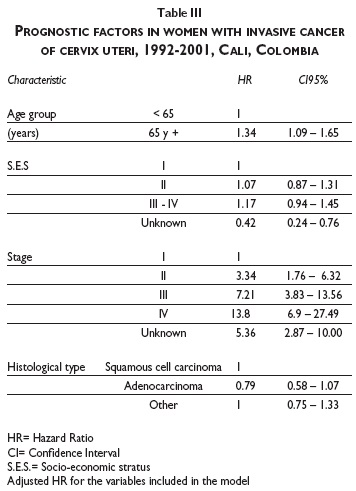
Table III shows the prognostic factors that were significant in the model. Women over 65 years of age were at 1.3 higher risk of dying from cervical cancer and women in clinical stages III and IV had 7 and 14 times higher risk respectively of dying from cervical cancer. No association was found with socio-economic level and histological type.
Discussion
A decline in the incidence and mortality of SCC and an increase in the incidence of adenocarcinoma during a 45 years period was documented in Cali, Colombia using the database of the Cali Cancer Registry. This cancer registry, the oldest in Latin America was founded in 1962. Reasons for the decline in incidence and mortality SCC are multiple and probably include: improvement in socio-economic conditions, decrease in parity rates and some effect of screening programs. The reasons for the lack of significant impact of the screening program in Colombia has been recently analyzed and will be discussed below under secondary prevention. An increase of cervical adenocarcinomas have also been reported from several developed countries in North America, Europe and Australia and have been ascribed to lack of effectiveness of Pap-based screening programs to detect these cancers in the endocervical canal and to increases in cervical HPV infection.6 To discuss the implications that the identification of HPV as the major cause of cervical cancer has in the prevention of this malignancy, a review of the molecular evidence is presented below.
A major discovery in human cancer etiology has been the recognition that cervical cancer is a rare consequence of an infection by some mucosatropic types of Human Papillomavirus (HPV). In Public Health terms, the importance of this finding is comparable to the unveiling of the association between cigarette smoking and lung cancer, or between chronic infections with Hepatitis B or Hepatitis C viruses and the risk of liver cancer. Although already in 1842 Rigoni Stern observed that mortality from cancer of the uterus was extremely rare among nuns and more frequent in married women, hinting to the possibility of a sexually transmitted agent as the main cause of cervical cancer, only during the last 25 years the human papillomavirus (HPV) has been identified as main cause of this cancer. From the 1960s to the late1980s Herpes simplex type 2 (HSV-2) was considered as the most likely cause; at that time the lack of serological assays to detect HSV-2 specific antibodies different from the HSV-1 antibodies and the absence of HSV-2 DNA in tumour specimens, casted doubt on this hypothesis.9
One of us (NM) has had the privilege of being one of the scientists that participated in the discovery of HPV as the main cause of cervical cancer and in the application of this knowledge to the prevention of this cancer.10 HPV natural history studies have now revealed that HPVs are the commonest of the sexually transmitted infections in most populations. Most HPV exposures result in spontaneous clearance without clinical manifestations and only a small fraction of the infected persons, known as chronic or persistent carriers, will retain the virus and progress to precancer and cancer. Molecular characterization and cloning of the first HPV types in the 1980s made possible the development of hybridization assays to look for HPV gene fragments in human tissue.11 Formal epidemiological evidence of an association between HPV and cervical cancer was lacking until the early 1990s.12
Using the first HPV hybridization assays developed and later on the PCR-based hybridization assays at the International Agency for Research on Cancer (IARC) the following fundamental molecular epidemiological studies to investigate the role of HPV in cervical cancer were carried out:
Case control studies
The pioneering study of this program was carried out in Spain and Colombia.13,14 In these two countries with contrasting cervical cancer rates, Spain with one of the lowest incidences and Cali with a high incidence, the first population-based case-control studies on HPV and cervical cancer were carried out; exposure to HPV was measured using the three hybridization assays developed at the time.13,14 The population-based Cancer Registry of Cali was fundamental in the identification of the incident cases of cervical cancer diagnosed during the study period in this city. The results of these studies have been considered as the first unequivocal molecular epidemiological evidence of the causal association between HPV and cervical cancer.14 Similar studies were subsequently implemented in nine other countries (Algeria, Brazil, India, Mali, Morocco, Paraguay, Peru, Thailand and the Philippines). In these 12 countries around the world we studied a total of 2500 women with cervical cancer and 2500 control women without cancer. These women were interviewed using a standardized questionnaire to elicit information on risk factors for cervical cancer and underwent a gynecological examination to collect cervical cells from the tumours and normal cervices for the detection of HPV DNA of 30 HPV types that infect the genital tract. The prevalence of HPV DNA was over 95% in the tumors cells of women with cervical cancer and it ranged from 5 to 20% in normal cervical cells of control women. These prevalences correspond to Odds Ratios (ORs) of over 100 indicating a very strong association between HPV and cervical cancer. The magnitude of the ORs allowed an epidemiological classification of 15 HPV types as carcinogenic or high-risk types, 12 as low-risk types and three types as probably carcinogenic.15 This classification has been reviewed in 2009 by the IARC leaving the following 12 HPV types as class 1 or carcinogenic: HPV 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58 and 59 HPV68 as class 2A or probably carcinogenic and 12 other types as class 2B or probably carcinogenic.16
Our case-control studies also allowed the identification of the following cofactors that acting together with HPV increase the risk of progression from HPV persistent infection to cervical cancer: tobacco, high parity, long term use of oral contraceptives and past infections with Herpes simplex type 2 and Chlamydia trachomatis.17,18 In addition, they contributed to establish the important role of male sexual behavior in the risk of developing cervical cancer.19
Survey of HPV types in invasive cervical cancers
Over 1 000 women with invasive cervical cancer from 22 countries around the world including Colombia, were included in this study. HPV DNA detection with PCR-based assays revealed that 99.7% of the cases were HPV-positive. This finding led us to propose for the first time that HPV was not only the main cause of cervical cancer, but also a necessary cause.20 No other virus has been shown to be a necessary cause.
The above two studies made possible to estimate the proportion of cervical cancer cases attributable to the main HPV types in the various geographical regions. They showed that HPV 16 and 18 account for 70% of cervical cancer and the 8 most common types (HPV 16, 18, 45, 33, 31, 52, 58 and 35) account for about 90% of cervical cancer.21 These estimates have been confirmed in a larger survey including over 10000 cases of invasive cervical cancer from 43 countries around the world, including Colombia and are being used to estimate the impact of preventive strategies based on HPV.22
Implications for prevention
The demonstration that infection with certain types of human papillomavirus (HPV) is not only the main cause but also a necessary cause of cervical cancer has led to great advances in the prevention of this disease on two fronts:
a) Primary prevention by the use of prophylactic HPV vaccines; and b) secondary prevention by increasing the accuracy of cervical cancer screening.
(i) In primary prevention by the use of prophylactic HPV vaccines; two safe and efficacious prophylactic HPV vaccines have been developed using viral like particles (VLPs); the quadrivalent vaccine (Gardasil) contains VLPs of HPV 16 and 18, responsible for about 70% of cervical cancers, a considerable proportion of other genital cancers and cancers of the oral cavity and pharynx and VLPs of HPV6 and 11 that cause about 90% of genital warts and recurrent respiratory papillomatosis (RRP). The bivalent vaccine (Cervarix) contains only VLPs of HPV16 and 18. Table IV summarizes the main results from phase-3 double-blind randomized controlled trials conducted in over 35 countries around the world, including Colombia. In young women (15-26 years old) who have not been exposed to HPV, both vaccines have been shown to prevent high-grade precancerous lesions of the cervix (CIN2/3) with efficacies close to 100%, and this protection has been shown to last at least 7-8 years.23 The quadrivalent vaccine has been shown to have in addition a high efficacy for the prevention of high-grade precancerous lesions of the vulva, vagina, and genital warts and of the anus in men.24,25 The bivalent vaccine has been reported to have a high efficacy for the prevention of persistent anal HPV infection in women. Some degree of cross-protection for HPV types phylogenetically related to HPV 16 and 18 have been reported for both vaccines. Pre- and post-licensure studies have shown that both vaccines are safe and well tolerated.
The World Health Organization (WHO) recommends a 3-dose vaccine schedule, completed over the course of 6 months, for a likely primary target population of girls within the age range of 9 or 10 years through 13 years.23 The main limitation of both vaccines is that they protect against cancers produced only by HPV 16 and 18 (about 70% of cervical cancers), and since they are prophylactic, they do not have any effect on established HPV infections or their associated lesions, (they do not have therapeutic effect). Therefore, they do not preclude the need of screening.
Both vaccines have been licensed in about 120 countries. By 2012, national HPV vaccination programs had been introduced in 39 countries, in the developed world and a few middle income countries. The United States, Australia, and Canada were among the first countries to introduce HPV vaccine into their national immunization programs in 2006-2007, and coverage is higher in Australia and Canada (over 80%), where the administration of the vaccine is school-based and lower in the US where it is clinic-based. The main challenges for the introduction of the HPV vaccine in immunization programs in low and middle income countries are: their high price and the lack of infrastructure to reach adolescents and immunize them with three doses. Great advances have been made recently in both fronts; the GAVI Alliance (GAVI) announced in the fall of 2011 that it will provide HPV vaccines for the poorest countries (GAVI- eligible countries in Latin America: Haiti and Nicaragua); the company producing the quadrivalent vaccine has offered to GAVI a price of five dollars per dose.26 For middle income countries, manufacturers are offering lower prices based on negotiations such as those conducted by the PAHO Revolving Fund. Through this fund, Latin American countries may acquire the vaccine at around 14 dollars per dose as opposed to the initial commercial price of about 120 dollars per dose. As of August 2012 five Latin American countries have introduced the HPV vaccine in their national immunization programs: Panama, Mexico, Peru, Argentina and Colombia.27 Concerning vaccine delivery, pilot projects have shown that highest coverage is reached through school-based programs, and a sub-analysis within the Guanacaste HPV vaccine trial in Costa Rica has revealed that less than three doses may confer good protection;28 schedules with less than three doses will facilitate high coverage, and these schedules are being tested in Canada, Mexico, Switzerland and Colombia. Preferably, HPV vaccines should be introduced as part of a coordinated strategy to prevent cervical cancer and should not undermine effective cervical cancer screening programs in those countries where these programs are in place. In most developing countries where effective screening programs do not exist or will be very difficult to implement, the ideal strategy will be based on vaccination of adolescent girls.
(ii) In secondary prevention by increasing the accuracy of cervical cancer screening. Well organized screening programs have been successful in reducing cervical cancer incidence and mortality in developed nations, but they have been unsuccessful in the great majority of developing countries.29 The main reasons for the lack of impact of cytology-based screening programs in Colombia have been identified. They include poor cytology quality and lack of follow-up and treatment of 30-40% of women diagnosed with high-grade cervical lesions.30
Several clinical trials have shown that HPV DNA detection assays are more sensitive but a bit less specific than cytology for detection of high grade precursor lesions of the cervix (CIN2/3) and suggest that they should be used as primary screening test instead of cytology.31 A cluster randomized trial in India has reported that a single round of screening with HPV test was followed by a 50% reduction in mortality from cervical cancer in women 30 to 59 years old after 8 years of follow-up, as opposed to not effect of cervical cytology or screening with VIA.32 The lower specificity of HPV-based screening as compared with cytology-based screening leads to the possibility of over treatment of cervical lesions, that if left untreated, will regress. Research efforts are centered now in finding the best way to triage women found positive for HPV; various biomarkers including type specific HPV 16/18, RNA, p16 are being evaluated. Cost-effectiveness evaluation of conventional cervical cytology and HPV testing for cervical screening in Colombia have shown that HPV testing every 5 years in women over 30 years of age is a cost-effective strategy, provided that the cost of the HPV test is less than 31 dollars.33 In addition, a demonstration project in very low income populations near Bogota, has shown that screening using visual inspection with acetic acid (VIA) and Lugol's iodine (VILI) is more sentive but less specific than cytology or VIA alone and provides bases to implement see and treat strategies in very deprived populations.34 The above results led to the Ministry of Health of Colombia to approve screening strategies based on scientific evidence and to include the use of the HPV test as primary screening test in the social security system, and to expand the VIA-VILI screening program to five other very low-resource areas in Colombia (Amazonas, Buenaventura, Caquetá, Guajira, Tumaco).35
Similar decisions have been taken in Mexico that decided to formulate a comprehensive strategy for the control of cervical cancer including HPV-based screening and HPV vaccination of all 11 year old girls.36
It is hope that a fast and inexpensive HPV test (CareHPV at less than five dollars) developed with funds from the Gates foundation will be shortly commercially available.37
In conclusion, the main hope to reduce the burden of cervical cancer in Colombia and in Latin American countries lies in the introduction of the prophylactic HPV vaccine to all adolescent girls and in the introduction of the HPV assay as primary screening test, and great advances have been made in both directions.38 The self-sampling of vaginal cells at home for HPV testing, is a strategy that could address the two major problems of Pap-based screening programs: the very low coverage of women at high risk and the very low sensitivity of Pap-based screening.39
Acknowledgments
The authors thank all staff at the collaborating healthcare institutions in Cali and the population-based Cancer Registry of Cali. Programa Nacional de Ciencia, Tecnología e Innovación en Salud. Departamento Administrativo de Ciencia, Tecnología e Innovación (National Program for Scientific Research and Innovation) COLCIENCIAS. This research was funded by the Department of Pathology of the School of Medicine at Universidad del Valle. This work is supported in part by grant RC.302-2007-11-06-4082-0552 Universidad del Valle-COLCIENCIAS.
References
1. Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer 2010;127(12):2893-917. [ Links ]
2. Almonte M, Murillo R, Sánchez GI, Jerónimo J, Salmerón J, Ferreccio C, et al. [New paradigms and challenges in cervical cancer prevention and control in Latin America]. Salud Publica Mex 2010;52(6):544-59. [ Links ]
3. CIA. The World Factbook 2012 [cited 2012. Dec]. Available from: https://www.cia.gov/library/publications/the-world-factbook/rankorder/2172rank.html. [ Links ]
4. Cendales R, Pardo C. Incidencia estimada y mortalidad por cáncer en Colombia, 2002-2006. Bogotá: Instituto Nacional de Cancerología, 2010. [ Links ]
5. Bravo LE, Collazos T, Collazos P, García LS, Correa P. Trends of Cancer Incidence and Mortality in Cali, Colombia. 50 years experience. Colomb Med 2012;43(4):246-255. [ Links ]
6. Vizcaino AP, Moreno V, Bosch FX, Muñoz N, Barros-Dios XM, Borras J, et al. International trends in incidence of cervical cancer: II. Squamous-cell carcinoma. Int J Cancer 2000;86(3):429-435. [ Links ]
7. Joinpoint Regression Program. 3.5.4 ed: Statistical Research and Applications Branch. Bethesda MO: National Cancer Institute, 2012. [ Links ]
8. Surveillance Research Program NCI. SEER*Stat software. Version: 7.0.9 ed. Bethesda, MD: National Cancer Institute, 2012. [ Links ]
9. Muñoz N. Model systems for cervical cancer. Cancer Res 1976;36(2 pt 2):792-793. [ Links ]
10. Muñoz N. From causality to prevention. The example of cervical cancer: my personal contribution to this fascinating history. Public Health Genomics 2009;12:368-371. [ Links ]
11. Gissmann L, zur Hausen H. Human papilloma virus DNA: physical mapping and genetic heterogeneity. Proc Natl Acad Sci USA 1976;73(4):1310-1313. [ Links ]
12. Muñoz N, Bosch X, Kaldor JM. Does human papillomavirus cause cervical cancer? The state of the epidemiological evidence. Br J Cancer 1988;57(1):1-5. [ Links ]
13. Bosch FX, Muñoz N, de Sanjosé S, Izarzugaza I, Gili M, Viladiu P, et al. Risk factors for cervical cancer in Colombia and Spain. Int J Cancer 1992;52(5):750-758. [ Links ]
14. Muñoz N, Bosch FX, de Sanjosé S, Tafur L, Izarzugaza I, Gili M, et al. The causal link between human papillomavirus and invasive cervical cancer: a population-based case-control study in Colombia and Spain. Int J Cancer 1992;52(5):743-749. [ Links ]
15. Muñoz N, Bosch FX, de Sanjosé S, Herrero R, Castellsagué X, Shah KV, et al. Epidemiologic classification of human papillomavirus types associated with cervical cancer. N Engl J Med 2003;348(6):518-527. [ Links ]
16. Bouvard V, Baan R, Straif K, Grosse Y, Secretan B, El Ghissassi F, et al. A review of human carcinogens--Part B: biological agents. Lancet Oncol 2009;10(4):321-322. [ Links ]
17. Muñoz N, Franceschi S, Bosetti C, Moreno V, Herrero R, Smith JS, et al. Role of parity and human papillomavirus in cervical cancer: the IARC multicentric case-control study. Lancet 2002;359(9312):1093-1101. [ Links ]
18. Muñoz N, Castellsagué X, de González AB, Gissmann L. Chapter 1: HPV in the etiology of human cancer. Vaccine 2006;24 Suppl 3:S3/1-10. [ Links ]
19. Muñoz N, Castellsagué X, Bosch FX, Tafur L, de Sanjosé S, Aristizabal N, et al. Difficulty in elucidating the male role in cervical cancer in Colombia, a high-risk area for the disease. J Natl Cancer Inst 1996;88(15):1068-1075. [ Links ]
20. Walboomers JM, Jacobs MV, Manos MM, Bosch FX, Kummer JA, Shah KV, et al. Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. J Pathol 1999;189(1):12-19. [ Links ]
21. Muñoz N, Bosch FX, Castellsagué X, Díaz M, de Sanjose S, Hammouda D, et al. Against which human papillomavirus types shall we vaccinate and screen? The international perspective. Int J Cancer 2004;111(2):278-285. [ Links ]
22. de Sanjose S, Quint WG, Alemany L, Geraets DT, Klaustermeier JE, Lloveras B, et al. Human papillomavirus genotype attribution in invasive cervical cancer: a retrospective cross-sectional worldwide study. Lancet Oncol 2010;11(11):1048-1056. [ Links ]
23. World Health Organization. Human papillomavirus vaccines. WHO position paper. Wkly Epidemiol Rec 2002009;84:118-131. [ Links ]
24. Muñoz N, Kjaer SK, Sigurdsson K, Iversen OE, Hernandez-Avila M, Wheeler CM, et al. Impact of human papillomavirus (HPV)-6/11/16/18 vaccine on all HPV-associated genital diseases in young women. J Natl Cancer Inst 2010;102(5):325-339. [ Links ]
25. Palefsky JM, Giuliano AR, Goldstone S, Moreira ED, Aranda C, Jessen H, et al. HPV vaccine against anal HPV infection and anal intraepithelial neoplasia. N Engl J Med 2011;365(17):1576-1585. [ Links ]
26. GAVI Alliance. Human papillomavirus vaccine. New and underused vaccines support Geneva, Switzerland. GAVI Alliance; 2012 [updated Dec 2012; cited 2012 Dec]. Available from: http://www.gavialliance.org/support/nvs/human-papillomavirus-vaccine-support/. [ Links ]
27. Muñoz N. Progress on HPV vaccine introduction in Latin America. HPV Today Latin America Special Issue 2012;27, November. [ Links ]
28. Kreimer AR, Rodriguez AC, Hildesheim A, Herrero R, Porras C, Schiffman M, et al. Proof-of-principle evaluation of the efficacy of fewer than three doses of a bivalent HPV16/18 vaccine. J Natl Cancer Inst 2011;103(19):1444-1451. [ Links ]
29. Murillo R, Almonte M, Pereira A, Ferrer E, Gamboa OA, Jerónimo J, et al. Cervical cancer screening programs in Latin America and the Caribbean. Vaccine 2008;26 Suppl 11:L37-48. [ Links ]
30. Murillo R, Wiesner C, Cendales R, Piñeros M, Tovar S. Comprehensive evaluation of cervical cancer screening programs: the case of Colombia. Salud Publica Mex 2011;53(6):469-477. [ Links ]
31. Cuzick J, Arbyn M, Sankaranarayanan R, Tsu V, Ronco G, Mayrand MH, et al. Overview of human papillomavirus-based and other novel options for cervical cancer screening in developed and developing countries. Vaccine 2008;26 Suppl 10:K29-41. [ Links ]
32. Sankaranarayanan R, Nene BM, Shastri SS, Jayant K, Muwonge R, Budukh AM, et al. HPV screening for cervical cancer in rural India. N Engl J Med 2009;360(14):1385-1394. [ Links ]
33. Andrés-Gamboa O, Chicaíza L, García-Molina M, Díaz J, González M, Murillo R, et al. Cost-effectiveness of conventional cytology and HPV DNA testing for cervical cancer screening in Colombia. Salud Publica Mex 2008;50(4):276-285. [ Links ]
34. Murillo R, Luna J, Gamboa O, Osorio E, Bonilla J, Cendales R, et al. Cervical cancer screening with naked-eye visual inspection in Colombia. Int J Gynaecol Obstet 2010;109(3):230-234. [ Links ]
35. Murillo R. Approaches to cervical cancer screening in areas with unequal health services: the example of Colombia. HPV Today- Latin America Special Issue 2012;27, November. [ Links ]
36. Lazcano-Ponce E, Lorincz AT, Cruz-Valdez A, Salmerón J, Uribe P, Velasco-Mondragón E, et al. Self-collection of vaginal specimens for human papillomavirus testing in cervical cancer prevention (MARCH): a community-based randomised controlled trial. Lancet 2011;378(9806):1868-1873. [ Links ]
37. Qiao YL, Sellors JW, Eder PS, Bao YP, Lim JM, Zhao FH, et al. A new HPV-DNA test for cervical-cancer screening in developing regions: a cross-sectional study of clinical accuracy in rural China. Lancet Oncol 2008;9(10):929-936. [ Links ]
38. Muñoz N, Franco EL, Herrero R, Andrus JK, de Quadros C, Goldie SJ, et al. Recommendations for cervical cancer prevention in Latin America and the Caribbean. Vaccine 2008;26 Suppl 11:L96-L107. [ Links ]
39. Muñoz N, Herrero R. Prevention of cervical cancer in women's hands: Mexico leads the way. Lancet 2011;378(9806):1829-1831. [ Links ]
Received on: April 4, 2013
Accepted on: July 23, 2013
 Corresponding author:
Corresponding author:
Nubia Muñoz.
Departamento de Patología, Universidad del Valle.
Calle 4B 36-00 Oficina 4003, Cali, Colombia.
E-mail: nubiamunoz@gmail.com
Declaration of conflict of interests. Nubia Muñoz is a member of the Merck HPV Global Advisory Board.













