Introduction
Bone grafts are used in many aspects in reconstructive orthopedic surgery and comprise from fractures treatments to extremities preservation in oncologic surgery.1 In spine surgery United States realized 289,000 annual surgery’s in which they use bone graft.2 Bone graft has a double function: mechanic and biological. Depending on the clinical advantage we are looking, one or the other function has more importance. In the bone-guest graft interface exists a relation, some factors can intervene in the correct incorporation of the graft with great importance in implantation zone, graft vascularization, bone-guest graft interface, immunogenic between guest and donor, conservation technic, local factors and diverse systems (hormonal, drugs, bone quality, chronic degenerative diseases) and mechanic properties (depend on size, form and type of graft used).3 Grafts have different utilities that enhance consolidation, osteogenesis, osteoinduction and osteoconduction,4 in ideal way bone graft need to have this characteristics, plus being biological compatible and provide biomechanical stability.
Bone grafts are classified by the obtaining site: bone autolog graft, bone transplant is taken from an anatomic site and implant it in other site in same person; bone allograft, bone graft is taken form one person and implant in other person (same specie); bone xenograft, tissue transferred form one specie to another spicie.5
Spine surgery is associated with no union rate on posterolateral arthrodesis of 50% without instrumentation and 10-15% with instrumentation.6
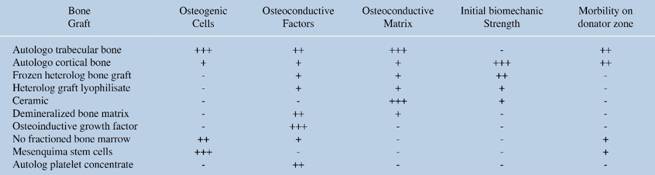
Currently complications secondary to the use of autolog grafts and allografts strategies are developed to increase the bone consolidation rate in presence of bone graft, decrease the need of its use and quantity used. Bone enhancer materials are classified as: bone extensor, bone enhancer, bone substitute8 and examples of them are ceramics,9,10,11,12,13 demineralized bone matrix (MOD),12,14,15,16,17,18,19,20 bone morphogenetic proteins,21,22,23,24,25,26,27,28 platelet rich plasma (PRP),29,30,31 bone tissue engineering (Table 1).32,33,34,35
In actuality it is well known the osteoconductive capacity of collagen matrix for bone regeneration. FibroquelMR is a biological drug formed by an irradiated collagen type 1 mixture and Polyvinylpyrrolidone, this drug stimulates bone regeneration in superior levels than the ones obtain with collagen.36 This drug effect acts on fibroblasts and macrophages modulating endogen collagen action by having effect in PDGF, TNF-α, IL-1b, ELAM-1 and VCAM-1 production, reaching levels similar to normality, with the consequent elimination of fibrous proteins. This favor matrix formation with better capacity for invasion and migration of osteoprogenitor cells.36,37,38,39,40
Two reports exist in literature about FibroquelMR used in bone genesis on skull defects in rats,31,39 but no literature found in global reports about it use in spine fusion. Autolog bone graft obtained from iliac crest bone is currently considered the gold standard, but investigation is on process to find a new alternative with superior characteristic. In time that synthetic bone grafts and growth factors start being a clinical reality, a new gold standard will be defined. The problem is to know if FibroquelMR, a biological drug formed by a irradiated collagen type 1 mixture plus Polyvinylpyrrolidone, stimulates bone regeneration at superior levels than the obtained by the use of collagen,36 when used to induce a fusion at lumbar spine vertebrae, using this drug on posterolateral lumbar fusion side, combining it with iliac crest autolog graft and autolog graft as control.
The objective in the study is to compare arthrodesis rate and quality using autolog graft of iliac crest versus autolog graft of iliac crest plus collagen type 1 + Polyvinylpyrrolidone as a bone enhancer. Valuating bone genesis activity of collagen type1 + Polyvinylpyrrolidone in situ by radiological analysis, simple view and manual exploration, and histological study of control and study side with light microscopy.
We consider as hypothesis that the combination of autolog graft + collagen type1 + Polyvinylpyrrolidone will increase the bone quality in posterolateral arthrodesis in a experimental model with New Zealand rabbits.
Material and methods
Prospective study, experimental model self-controlled in 15 New Zealand rabbits with a weight from 3.5 and 4.5 kg. Posterolateral arthrodesis at L5-L6 segment was made.
Experimental model
Surgical technique
On general anesthesia effect, done by subcutaneous injection of ketamine (35 mg/kg) and xylazina (18 mg/kg). Surgical zone was shaved, asepsis and antisepsis was realized with iodine foam. At iliac crests level 2 cm posterosuperior incisions where made, incision of fascia, subperiostic dissection of iliac crests and 2cm3 autolog graft of trabecular bone was obtained. Medial line incision at L5-L6, two paramedian incisions in fascia, dissection of multifidus and dorsal longisimo muscle, transverse apophysis was located, transversal apophysis decortication using pneumatic drill (Midas Rex® Medtronic).
Insertion of autolog graft plus 1cc of FibroquelMR, on right side of arthrodesis (study segment) and insertion of autolog graft on left side (control segment). Wound closure using absorbable suture (Poliglactin 910) 2-0 on fascia and Nylon monofilament 3-0 on skin. Rabbits had normal activity in cage until euthanasia after 8 weeks. Euthanasia was by intravenous phenobarbital administration after 8 weeks. Block resection of lumbar segment was done by anterior approach.
Radiological analysis
Posteroanterior and lateral radiographies were taken after 8 weeks of post surgery with a tube distance -chassis at 90 cm-, authors valuated them by blind study, and criteria was established, solid and no solid arthrodesis, based in the presence of trabecular pattern between transverse apophysis and articular facets posterior zone.
Manual exploration
After obtaining lumbar spine segment, macroscopic analysis was made of fused segment and manual exploration between transverse apophysis and one level up and down. This simulates the exploration of fuse by manual exploration in humans; this represents the gold standard for determining solid arthrodesis and no union. Each segment was valuated and criteria were established for solid fusion and not solid. Only fussed levels were considered with arthrodesis.
Light microscopy analysis
Once obtained the lumbar segments, fixed in formaldehyde for 24 hours, then sagittal cuts were done and fixed in ethanol 70% for a week, then samples were dehydrated in solution of ethanol 95 and 100%. Once samples were decalcify, cuts of 5 um were done and stained with heamtoxylin-eosin. Criteria were established based on the continuity of trabecular pattern between transverse apophysis and transverse apophysis of segment with arthrodesis
Results
Posterolateral L5-L6 arthrodesis: not intraoperative or postoperative complications reported. No perioperative morality reported.
Radiographic analysis: radiographic consolidation observed after 8 weeks in 12 (80%) on the 15 segments of left side (control group) versus 14 (93%) radiographic consolidation after 8 weeks on right side of arthrodesis (study group).
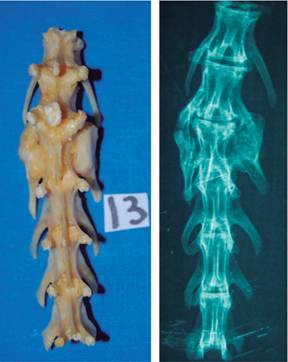
Manual exploration: 13 (86%) completed criteria of no mobility on left side of arthrodesis (control group) versus 14 (93%) with complete criteria of no mobility in right side of arthrodesis (study group) (Figure 1).
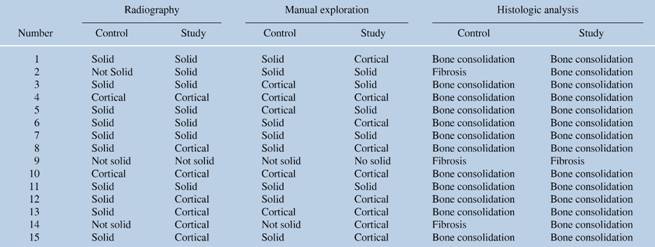
Histological analysis: bone continuity between transverse apohysis with an intercalated trabecular pattern and normal bone characteristics in 12 (80%) in left side of arthrodesis and 14 (93%) in right side of arthrodesis. It is important to mention that pattern that had cortical bone in radiographs and manual exploration, the histological analysis show better bone quality than other segments that didn’t have cortical bone generated (summary of results can be consulted in (Table 2)).
Table 2: Summary of results in 15 rabbits, we observe solid and cortical consolidation or presence of fibrous tissue in histological analysis in number 9 case.
Statistical analysis: significant statistical difference was obtained by square chi test between both groups, comparing arthrodesis versus no union, with a p value of < 0.0001.
Discussion
The collagen, specific type 1 and derivatives have been used in many areas of pharmacology. On a study done in 2003,39 determination of security of collagen polyvinylpyrrolidone (PVP collagen) was done by in vitro and in vivo studies. Wealthy Patients serum and peripheral cells of blood were valuated, before treatment and after treatment with collagen PVP. Authors observed that this mixture doesn’t stimulate lymphoid proliferation nor DNA lesion in vitro, also doesn’t induce formation of collagen type anti porcine antibodies or collagen PVP antibodies in vivo. Not metabolic, renal or hepatic dysfunction was observed with the use of collagen PVP administer intradermic and intramuscular way, in short and long term treatment. In conclusion, in this study it was demonstrated that not cellular lesion or immunologic (humoral or cellular) adverse effects were associated to the treatment with collagen PVP, even after 400 weeks of consecutive administration.
In orthopedic surgery its use was limited initially as a hemostatic agent, but many studies had been done to prove its use as a bone enhancer, because its capacity to stimulate mesenquima cells and angiotropic effect, and adhesive properties that avoid the graft migration.41
In history, high rate of attempts to create bone substitutes and bone lyophilisate to achieve a correct lumbar fusion, to decrease complications of iliac crest graft obtaining (gold standard) and achieve the increment of enhancing capacity of them and the volume that in many cases is insufficient, having from human bone lyophilisate, to morphogenetic bovine proteins.40,42
Collagen use with different substances as proteins and growth factors, are recommended as enhancers of arthrodesis consolidation, but is not recommended with bone substitutes or bone lyophilisate.43,44 After researching, no studies were found about the use of collagen type 1 + polivinilpirrolidona with autolog bone graft (iliac crest) in New Zealand rabbits. This a animal model validated that’s has characteristics that provide environment and rate of consolidation similar to the obtained in humans. This justified the realization of the present study.
We observed in this 15 rabbit series that the use of collagen type1 plus polyvinylpyrrolidone mixture with autolog graft gives significant increase in consolidation rate (p < 0.0001) than the use of autolog graft alone. In cases where consolidation was bilateral, we observed differences in quantity and quality of bone (macroscopic and histologic), therefore its use in the experimental model seems to provide some advantage. As this biological drug acts as a adhesive agent without impermeable properties seems to allow the recruitment of cellular growth factors and osteoprogenitor stem cells, both necessaries for bone consolidation. Based in this experimental model of this study we recommend the use of the Collagen type1 plus polyvinylpyrrolidone mixture as a bone enhancer, its use has a positive effect in the bone consolidation process, that traduces in better rate of arthrodesis consolidation, disadvantages is the increase in surgical costs, but decreases the need to a new approach to obtain the bone graft and allows to only use the one obtained during the decompression step.
Conclusion
The use of autolog graft plus collagen type1 and polyvinylpyrrolidone increases the consolidation rate compared to the use of iliac crest autolog graft alone in posterolateral arthrodesis done in New Zealand rabbits.
The use of collagen type1 and polyvinylpyrrolidone may have positive effects in the bone consolidation process, its use may be recommended as a bone enhancer.
It is necessary to realize a study on patients to compare its real utility.











 nueva página del texto (beta)
nueva página del texto (beta)