Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista odontológica mexicana
versión impresa ISSN 1870-199X
Rev. Odont. Mex vol.18 no.2 Ciudad de México abr./jun. 2014
Case report
Foreign body aspiration in dental office. Founded suspicion for late diagnosis. Case presentation and literature review
Adriana Ramírez Segura,* Eduardo de la Teja Ángeles,§ David Jofré Pavez,II Américo Durán Gutiérrez¶
* Second year resident, Pediatric Stomatology, (National Pediatric Institute) INP.
§ Head of the Stomatology INP (Service, National Pediatric Institute).
II Otolaryngologist, Professor at the Catholic University of Chile.
¶ Attached to the Stomatology Service INP (National Pediatric Institute).
ABSTRACT
Within the scope of pediatric medical practice, certain situations arise where timely diagnosis of a condition implies facing unforeseen situations. Clinical history is clearly paramount for the correct and precise handling of any patient, even more so for very young patients from whom obtained data can be frequently imprecise. With respect to foreign body aspiration accidents, there are specific indicators which substantiate a suspicion of that case. Nevertheless, not all cases are typical, therefore, experience of the clinical operator is essential. The present study presents the case of a one year and nine months old patient who broncho-aspirated a chrome-steel crown in a dental practice, and the situation was only diagnosed 60 days later. The present diagnosis was emitted at once when the patient arrived at the National Pediatrics Institute. To that aim, a thorax X-ray was taken. The present case can be considered a paradigm. It supports the idea that the oral cavity of very young patients must be treated by qualified specialists, and that such care must be given in centers which can guarantee the patient's safety. A foreign body can remain in the bronchii for a long time, without directly endangering the patient's life. Nevertheless, this situation would introduce the patient into a dangerous chronicity, therefore, emergency room physicians should be aware of the possibility of a substantiated suspicion of foreign body aspiration. These cases, after suitable history research and auscultation could have been avoided, and thus avoid a serious chronic situation in these patients.
Key words: Substantiated suspicion of foreign body aspiration, chrome-steel crown, accurate diagnosis.
INTRODUCTION
Foreign Body aspiration (FBA) is a life-threatening medical emergency,1 generally affecting children from 6 months of age onwards. This is a crucial stage of the cognitive development, wherein the oral region is the principal means for understanding the surrounding world. This stage can last until the child reaches 5 years of age. The greatest fatality incidence is found in 2 year old patients.1,2 Children of this age range exhibit characteristics such as exploration instinct and imitation of actions. Another factor is parent's carelessness, sometimes even force-feeding their offspring.3 Yet another characteristic of these children is the onset of easy tears or laughter as well as undertaking activities which imply fast breathing and laughter as well as bringing objects to the mouth. The immaturity of the laryngeal sphincter is the reason why many swollen objects undertake the airway route.4 In general, at other ages, children normally expel foreign bodies through coughing spells triggered by reflex mechanisms. Due to this fact, when a school-age child or teenager has aspirated a foreign body, onset of a neuromuscular disease must be contemplated, or the possibility that when the accident took place, the child might have been under the influence of alcohol or drugs. Nevertheless, it is very important to consider the possibility that a FBA could not be accidental, rather, a manifestation of child abuse.2
SIGNS AND SYMPTOMS WHICH SUBSTANTIATE THE SUSPICION OF ASPIRATION OF A FOREIGN BODY
In 40-80% of all cases, diagnosis is emitted after studying the patient's history. Nevertheless, confirmation is established with the help of imaging studies, especially bronchoscopy. In cases when the patient's circumstances allow it, a neck and thorax X-ray should be taken (in inspiration and expiration) in case the foreign body were to be radio-opaque.5
EARLY CLINICAL MANIFESTATIONS
Pediatric patients with history of foreign body aspiration mostly exhibit a clear history of asphyxia. Nevertheless, there is a small group of patients in whom signs and symptoms do not lead to a clinical interpretation of FBA. This could be due to the fact that the right bronchus is a more direct continuation of the trachea than the left bronchus. Foreign bodies preferably tend to penetrate the right lung.
Larynx
In cases when the object is large enough to fully obstruct the laryngeal light, it will cause respiratory difficulties, cyanosis and death. In cases when the obstruction is partial, the foreign object will elicit stridor, hoarseness, croupal cough, odynophagia, dyspnoea, as well as symptoms originated by the foreign object or by the inflammation caused by the lesion, even in cases where the foreign object might have migrated.
Trachea
Three characteristic signs are described for the detection of FBA in the trachea. The audible slap, which is detected by listening close to the patient while he inspires or coughs with an open mouth; the foreign body is heard while impacting against the trachea walls. The palpable hit which is equivalent to the touch fremitus of cardiac murmurs where the foreign body can be felt upon placing a finger on the trachea. The asthmatic wheezing, which is a sibilance audible with the stethoscope at the level of the trachea and undetectable at the thorax. Dysphonia is an infrequent point in cases when the foreign body is found in the larynx, nevertheless it can suggest the lesion is present in the laryngeal6 sphincter.
Bronchii
FBA characteristic clinical signs in the bronchii are cough, stridor or wheezing during expiration, decrease of air entrance into the affected lung as well as respiratory difficulties.
Esophagus
FBA characteristic clinical signs in the esophagus are nausea, hematemesis, intolerance or aversion to oral traffic. In certain cases, a body lodged into the esophagus can elicit respiratory symptoms due to the extrinsic compression of the trachea through the tracheo-esophageal septum.6
Belated clinical manifestations
Experience is paramount in order to emit a late FBA diagnosis, since clinical characteristics are not significant; the most common occurrence being persistent, hard to treat pneumonia as well as inflammatory reaction. In these cases X-rays might reveal atelactasia as well as localized lung destruction which might be discreet.7 Persistent lung overdistension can also be observed, as well as chronic bronchio-pulmonary suppuration and wheezing bronchial suppuration as well as wheezing bronchial rales similar to bronchial asthma which can persist even in the presence of specific medical treatment.8
Differential diagnosis
Chronic presence of foreign bodies is hard to diagnose. Therefore, a well-structured clinical history can enlighten the health professional as to whether he is facing a case of croup, asthma, or lower respiratory tract infection. In many cases, FBA events are masked by parents or the children themselves, due to their mistrust or fear about being responsible for this distressing situation.
CLASSIC DIAGNOSIS
Cough, fever, sputum and thoracic pain are classic symptoms of FBA. Nevertheless a poorly specialized or inexperienced clinical operator can overlook them. For these reasons FBA must be suspected in cases when the patient presents wheezing which does not respond to broncho-dilator treatment and presence of unexplained atelectases. A thoracic X-ray study is a useful diagnosis tool. Nevertheless, there are objects which are impossible to diagnose radiographically. Therefore, use of either rigid or flexible bronchoscopy can be a determining factor for a correct diagnosis. Notwithstanding the aforementioned, there are asymptomatic cases in where experience and skill are paramount for the diagnosis. Timing is a paramount factor in FBA patients in order to determine prognosis and treatment.9 Absence of clinical signs and symptoms does not discard the presence of foreign bodies in respiratory or digestive tracts, therefore, bronchoscope or panendoscopy are the two methods which allow to discard with certainty the presence of a foreign body. Urgent practice is indicated without formal contraindications and their iatrogenicity and morbidity are not significant.8
TREATMENT
When treatment is administered in the operating theatre, three main situations must be taken into consideration: detailed clinical history, imaging studies as well as suitable anesthetic handling. It is paramount to extract the foreign body and cleanse the area where it was lodged, infection must be prevented and in many instances, the use of broncho-dilators is a very valuable tool. For treatments administered under general anesthesia it is important to consider the following factors: proper oxygenation, control of cardio-respiratory reflexes, fast return of reflexes in the upper airway, prevention of deeper impactation of the foreign body, precise monitoring of oxygen saturation, electrocardiogram, carbon dioxide.9-11 Training of physicians for suspicion and diagnosis of foreign body aspiration is paramount in order to prevent complications and death. Therefore, solid medical training is paramount to prevent complications.12
COMPLICATIONS
Complications are determined by the time taken for the extraction of the foreign body. These complications can include tracheal or esophageal injuries, abrasions, lacerations, or necroses. Other more serious complications could be mediastinitis, pneumothorax, trachea-esophageal fistula and vascular damage (esophageal-aortic fistula in the cases when the FBO is lodged in the esophagus).13,14
PREVENTION
Parents must learn how not to give to their children foodstuff that can be deemed inappropriate for their age, such as peanuts or small sweets. That type of food must be kept out of their reach. Likewise, children must not be fed whenever they are running, crying or laughing. Children must be taught how to chew properly and toys with small -sized components should be used only under adult supervision.1,2,15
Stomatological care must be given by qualified specialists, so as not to endanger the child. Conduct must be properly handled as well as the use of therapeutic correctors, absolute isolation, and, if necessary, basic support FBA16 measures. Many cases of foreign body aspirations in the dental office have been reported. Even extracted teeth can be aspired.17 Due to the aforementioned facts, it would be deemed suitable that training for diagnosis and primary treatment of FBA patients should be included in advanced stomatology study plans.18
CLINICAL CASE
Assessment
Male patient, one year and eight months old apparent age. Healthy product of third pregnancy. Born through caesarean section. Breathed normally and cried at birth. The patient had been afflicted with bronchitis three months before and had suffered chickenpox(varicella). The present conditionhad its onset on 24 November 2008. The patientpresented bloody, non-cyanotic cough accompanied by a 39.5 oC fever. The condition was treated with paracetamol. Emmitted diagnosis was Upper Airway Infections (UAI). Treatment administered consisted on clarithromycin and Na Metamizole. The patient exhibited no improvement. The patient later developed a fever which was treated with double antipyretic. The patient was concurrently treated with nebulized salbutamol. No improvement was observed. Persistent fever and cough motivated the patient being brought at this National Pediatric Center. Auscultation revealed rales and murmurs. Hemodynamic and cardiac status were unaltered.
The mother informed that two months before she took the child to the dentist, who encountered difficulties in performing oral rehabilitation. The patient, during the course of treatment swallowed two crowns, out of which only one could be later recovered in an evacuation.
Figure 1 shows thorax X-rays. Right hemi-thorax hyper-reaction could be observed with presence of a foreign body in the right bronchus with parahiliary infiltrate predominantly in the right side. No consolidation data were available. Due to all the aforementioned reasons, a bronchoscopy was programmed.
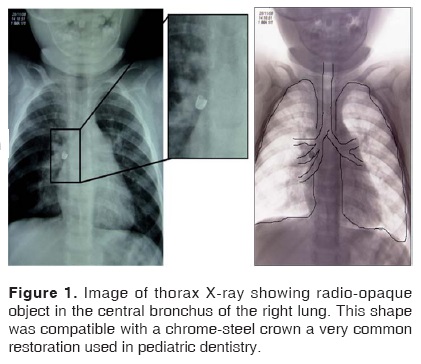
Neumology 28 November 2008
18:00
The patient was diagnosed with foreign body aspiration status at critical stage which was compatible with symptom's evolution. The patient was at high risk of developing complications due to the fact that there were infectious processes of the lower airways, pulmonary damage as well as tracheal stenosis. All the aforementioned facts warranted performance of a bronchoscopy.
Surgical procedure 28 November 2008
21:30
A bronchoscopy was performed through the mouth. Glottal and sub-glottal structures appeared normal. Main bronchial bi-furcation was reached principal, where edema was found with normal characteristics. Advance was undertaken through right pulmonary bronchus until obtaining visualization of metallic foreign body which was impacted upon the right pulmonary intermediate bronchus entrance. Tweezers were introduced in order to extract the foreign body and successfully achieved its dislodgement. A thinner bronchoscope was then introduced so as to advance to the impaction site. Impaction site was edematous and erythematosus, with presence of thick whitish mucous. Cleansing of the site was undertaken in order to leave the surgical bed clean.
EVOLUTION
Following the successful extraction of the foreign body control measures were preserved, where it wasascertained that pulmonary murmurs as well as rales became normal. The patient was maintained under antibiotic coverage, which consisted of clindamycin with fluticasone nebulations. This treatment was maintained for four days, until the patient returned to the hospital. At this visit, the patient was found to be asymptomatic, with suitable tolerance to oral way functions. The patient was deemed to present a very favorable evolution.
DISCUSSION
Behavior handling is determined by a key factor: communication. Communication is defined as the relationship between the child and the stomatologist. Communication is hard to establish when patients are either very young or psychologically immature. This is due to the fact that the cognitive development of the child is not ready to understand, negotiate or follow indications, therefore probability of accidents increases.
A study was conducted in 2006, in the greatest population of the world (China). In it, 1,088 cases of FBA were analyzed. A classification of aspired objects was made in these patients. Objects ranged from food bolus, to coins, fish-bones, dental prostheses, chicken bones, metal safety pins, lighters, buttons, toothbrushes, needles and spoons. Plastic toys, walnuts, nails, rings watches, glass fragments, etc, were found less frequently. Most common aspirated foreign bodies are coins, fish-bones and dental prostheses.19
Foreign bodies can also commonly be found in the ear, nose and throat. Family members often try to extirpate these foreign bodies when they consider they are not too impacted. Nevertheless, the best recommendation is to consult a specialist, since lay family members most frequently are unaware of anatomical structures as well as the suitable indications to properly extract a foreign body.
CONCLUSIONS
Dr. Lorenzo Perez Fernandez, a Mexican neumologist of great reputation, clearly describes the following: absence of clinical and radiological signs and symptoms does not rule out the presence of foreign bodies in the digestive or respiratory systems. Due to the aforementioned reasons, use of bronchoscopy or panendoscopy are two methods which allow to entirely discard the presence of a foreign body. Urgent practice is indicated; there are no formal contraindications and iatrogenicity and morbidity are not significant.8
Patients who have aspired a foreign body must be immediately treated. Nevertheless, some patients can present uncertain situations of foreign body aspiration; in these cases, to achieve timely detection, experience and clinical skill are paramount.
Prevention of accidents is paramount. In many instances, foreign bodies are lodged in the airways due to parent's or health professional's neglect. Therefore, all preventive measures are warranted such as specialized behavior management, physical barriers, anxiolytic drugs, etc.
It is paramount for the stomatologic area to be prepared to timely approach these cases. This can be achieved through education in the diagnosis, immediate emergency measures such as the Heimlich maneuver, or cardiopulmonary resuscitation. Above all other considerations, ethical education is basic so as to warn whether there is a suspicion of foreign body aspiration, as well as data that in late-diagnosed cases.
REFERENCES
1. Jofré PD, Ayala RF, García DP. Cuerpo extraño en vía aérea desafío, diagnóstico y terapéutica. Rev Dia. 2006; 22: 26-30. [ Links ]
2. Jofré PD. Aspiración de cuerpos extraños en la vía aérea [Internet]. Pontificia Universidad Católica de Chile, Escuela de Medicina Otorrinolaringología. Disponible en: http://www.escuela.med.puc.cl/paginas/doc [ Links ]
3. Arango M. Cuerpos extraños bronquiales en lactantes. Presentación de un caso. Rev Colomb Neumol. 1999; 11: 58-60. [ Links ]
4. Bye M, Scanlin T. Airway foreign body [Internet]. Pulmonology, Medicine, updated to October 2005. Disponible en: www.emedecine.com [ Links ]
5. Calvo MC, Rodríguez A, López J. Obstrucción aguda de la vía aérea superior en lactantes y niños. An Esp Pediatr. 1999; 51: 409-416. [ Links ]
6. Ospina J, Ludemann J. Aspiration of an extracted molar: case report. J Dent Assoc. 2005; 71: 581-583. [ Links ]
7. Ibrahim S, Ali U, Abdelaaziz W. Inhaled foreign bodies: management according to early or late presentation. Europ J Cardio-thoracic Surgery. 2005; 28: 369-374. [ Links ]
8. Pérez FL. Deglución o bronco aspiración de cuerpos extraños. "Pediatría Médica" del Instituto Nacional de Pediatría. 2001; 14: 652-656. [ Links ]
9. Conners G. Management of asymptomatic coin ingestion. Pediatrics. 2005; 116: 342-345. [ Links ]
10. Kalyanappogol VT, Kulkarni NH, Bidri LH. Management of tra-queobronchial foreing body aspirations in pediatric age group- a 10 year retrospective analysis. Ind J Anesth. 2007; 51: 20-23. [ Links ]
11. Lin HH, Lee SC, Chu HC, Chang WK, Chao YC, Hsieh TY. Emergency endoscopy management of dietary foreing bodies in the esophagus. Am J Em Med. 2007; 25: 662-665. [ Links ]
12. Saquib MM, Rauf KA, Al-bassam A. Late presentation of tra-queobronchial foreign body aspiration in children. J of tropic Pediatr. 2005; 51: 145-148. [ Links ]
13. Digoy GP. Diagnosis and management of upper aerodigestive tract foreign bodies. Otolaryngol Clin North Am. 2008; 41: 485-496. [ Links ]
14. Heim SW, Maugan LK. Foreign bodies in the ear, nose and throat. Am Fam Phys. 2007; 76: 1185-1189. [ Links ]
15. Goren S, Gurkan F, Tirasci Y. Foreign body asphyxiation in children. Ind Ped. 2005; 42: 1131-1133. [ Links ]
16. Bardella IJ. Pediatric advanced life support: Review of the AHA recommendations. Am Acad Fam Phys. 1999; 15: 1-11. [ Links ]
17. Elgazzar RF, Abdelhady AI, Sadaka AA. Aspiration of an impacted lower third molar during its surgical removal under local anesthesia. Int J Oral Maxilofacial Surg. 2007; 36: 362-364. [ Links ]
18. Ospina GI. Cuerpos extraños en el tracto aerodigestivo infantil. El papel del otorrinolaringólogo. Act ORL Cir de cabeza y cuello. ap 2005;33:36-47. [ Links ]
19. Li ZS, Sun ZX, Zou DW, Xu GM, Wu RP, Liao Z. Endoscopic management foreing bodies in de uper GI tract experience with 1088 cases in China. Gastrointest Endosc. 2006; 64: 485-492. [ Links ]
20. Sheller B. Challenges of managing child behavior in the 21st Century dental setting. Pediatr Dent. 2004; 26: 111-113. [ Links ]
21. De Nova G, Bartolomé VB, Costa FF. Odontopediatría. La evolución del niño al adulto joven. Urgencias odontológicas. Madrid: Boj JR.; 2011. pp. 805-820. [ Links ]
Note This article can be read in its full version in the following page: http://www.medigraphic.com/facultadodontologiaunam Mailing address:
Mailing address:
Dr. Américo Durán Gutiérrez
E-mail: dr_americo@hotmail.com











 texto en
texto en 


