Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista odontológica mexicana
versión impresa ISSN 1870-199X
Rev. Odont. Mex vol.16 no.3 Ciudad de México jul./sep. 2012
Case report
Fibula transplant caudal vertical distraction for reconstruction of lower jaw defect caused by firearm projectile and rehabilitated with bone-integrated implants
José Francisco Ceseña Medina,* Juan Carlos López Noriega,§ Rafael Ruiz Rodríguez,II René Jiménez Castillo¶
* Maxillofacial and Oral Surgery student, Graduate School.
§ Head of Maxillofacial and Oral Surgery Service, Graduate School.
II Specialty Professor and Inter-hospital Coordinator of Maxillofacial and Oral Surgery Specialty, attached to the Graduate School.
¶ Maxillofacial Prosthesis Specialty Coordinator, Graduate School.
National School of Dentistry, National University of Mexico.
ABSTRACT
The present study presents satisfactory aesthetic and functional results achieved after correction of facial asymmetry in a patient subject to reconstruction with fibula graft of a wound caused by firearm projectile. Equally presented in this study is the rehabilitation of the stomatognathic complex through placement of bone-integrated implants. Procedure was accomplished in four surgical phases. Previous clinical and imaging evaluation was performed with support of stereolithographic studies. The first phase encompasses osteogenic distraction in caudal direction in the chin region. In the second phase, osteogenic distraction is performed bilaterally in caudal direction in the body of the lower jaw. The third surgical phase encompasses reconstruction of the lower lip. The fourth and final surgical phase comprehends the placement of bone-integrated implants. Through careful case analysis and available diagnostics tools surgical treatment sequence could be planned. Shape and anatomical dimension of lower jaw region could be attained. Another achievement was correction of soft tissue scars caused by lower jaw reconstruction sequels. Treatment was completed with masticatory function rehabilitation with the help of an implant-supported prosthesis.
Key words: Osteogenic distraction, caudal, bone graft, implant-supported, bone-integrated implants, bone integration.
INTRODUCTION
Reconstruction of lower jaw defects caused by trauma, tumor resection or congenital defects is one of the most frequent and complex problems the maxillofacial surgeon encounters.1-3 Within available peace-time statistics, defects that require reconstruction, as sequels to firearm projectile wounds, are mainly due to suicide asttempts.16
The lower jaw plays an important role in the protection of airway, tongue support, lower dentition as well as muscles of the floor of the mouth involved in mastication, word articulation deglutition and respiration.5-7 As well as in the contour of the facial lower third, loss of mandibular continuity produces cosmetic and functional deformities due to the formation of the scar in the wound as well as contraction in masticatory muscles. This causes limitations in lateral movements, protrusion, opening and closing of the lower jow, as well as maloclusion and proprioceptive problems.
Several techniques have been proposed along the decades for the reconstruction of large bone defects of upper and lower jaws. Among these we can count the following: iliac crest costochondral graft,1 reconstruction mesh and plates (stainless steel, chrome-cobalt and titanium) micro-vascular grafts as well as resorting to osteogenic distraction procedures.8,15
OSTEOGENIC DISTRACTION
Craneofacial osteogenic distraction (OD) is an enthralling endogenous tissue engineering technique. This technique experiences ever-growing popularity and has revolutionized the treatment of many either congenital or acquired malformations.1,3,5,16,17 This technique has been widely used to elongate or repair continuity defects found in the lower jaw. It is worth mentioning that new production of bone tissue is always accompanied with neoangiogenesis of soft tissues.3,5,6,16-19
Frost's theory describes the physiological range of the mechanical stimuli to be considered as normal when compared with pathological stress. When the local mechanical signal in the bone exceeds the limit of the physiological window, this being called minimum effective force, the bone will be subject to osseous modeling or remodeling. In cases when the mechanical loads are too strong, these forces will induce a pathological overload in the area. This will then produce formation of immature bone tissue, or connective tissue.16,19,20 These facts could lead us to propose that OD is a highly feasible method for the reconstruction of atrophic alveolar ridges.3,18,21 This is due to the fact that the osteoblast detects the load stimulus and then brings about a rapid, intermediate and prolonged signaling cascade. Following this, in this process, bone growth and differentiation can be detected. Osteoblasts proliferation is followed by a process of cell differentiation and, finally, by the extra-cellular matrix mineralization.19,22 Recently, there has been a trend to direct efforts to identify specific factors associated with the bone replacement index. This reveals the anabolic role of the following factors in bone formation: β1(TGFβ1 transforming growth factors, 1 (IGF-1) insulin type growth factors, and E 2 (PGE2)n prostaglandins.12,16,19,20,23,24
Osteogenic distraction can be described as the slow and progressive exercise of forces to a bone gap, to obtain, as a result, production of new bone and soft tissues.5,17,18,20 An osteotomy is performed at the site of the bone deficiency, and a device is put into place to separate bone ridges.3,16 Bone ridges are separated upon adjacent soft tissue; this then promotes a stretching process which induces hyperplasia of adjacent soft tissues.5,16,18,19 The bone gap thus created is initially filled by fibrous connective tissue, with collagen fibers which are oriented in a parallel fashion to the vector of distraction forces.10,19,22
After this new tissue is produced, proper fixation of segments is established to promote adequate ossification.12,16,25
Pioneers of this osteogenic distraction technique studied physiological parameters associated with the process of slow bone expansion. One of these surgeons was Dr Gabriel O. Ilizarov, (Kurigen, Russia) who is the scientist most commonly associated with this technique.5,9,16,25 Dr Ilizarov, along with his colleagues, determined the percentage, rhythm, amount and type of forces needed to optimize osteogenic distraction techniques in long bones. These basic axioms are commonly called Ilizarov principles.8,19,26 Concerning the craniofacial complex, Snyder et al. were the first to report the use of osteogenic distraction in the lower jaw.27 This was also the case for McCarthy et al. They performed the first clinical application of osteogenic distraction in the lower jaws.3,25,27,28 Based on osteogenic distraction principles established by Ilizarov, it is important to define three phases ocurring during the process of osteogenic distraction. The first phase can be considered the initial or latent period. In this period, a fracture is performed aiming, through an osteotomy, to achieve separation of bone ridges. During this period, and according to multiple protocols, a certain period of time is observed. This period can vary from one hour up to 8 days.3,5,29,30 aiming at the formation and organization of a clot, and through this clot, to the arrival of cellular elements which bear the characteristics of producing fundamental substances for bone neo-formation. After this, a distraction phase is observed. Once the pre-determined latency time is observed a new period is initiated. In this period, through the use of the distraction device, a constant force is applied during a pre-determined time. This is achieved with the activation of a screw expander. This expander is universally graded, in such a fashion as to produce a 5 mm movement with every 360 degree turn. Age of patients and vascularity of the bed where distraction is to be performed are variables which will determine the rhythm of the procedure.16,26,27,30,31 In scientific literature reports can be found informing of activations performed during a 24 hour period2 in order to obtain a 1 mm distraction in that period. Therefore, every activation will be performed every 24 hours.5,22,31 Pediatric cases are different. In them, due to their greater capacity to regenerate, distraction distance, frequency and force can be increased.25,32
Once these rhythm and force variables are determined, with the newly-formed tissue objective fulfilled, the third phase comes into play. This is the phase of consolidation and mineralization of the newly formed tissue.12,33 The objective of this consolidation phase is to keep immobile the transported bone segment, achieving thus adequate element organization and condensation. This will provide resistance in this newly formed tissue as well as avoidance of undesired phenol-typing of cellular elements which continuously arrive to the newly formed gap.11,16,19,26,31 This maturation process can also be affected according to age of patient, irrigation of involved site, metabolic status of the patient, as well as resistance presented by soft tissue with respect to the distraction area.16,27,34
Based upon the aforementioned factors, and according to the bone tissue18 scarring physiology, consolidation period is deemed to be no lesser than 8 weeks. This period can be extended up to 12 weeks to ascertain the event of new bone formation and histo-distraction.3,5,17,30 Upon completion of this final phase, the distraction device can be removed and results can be assessed. It is important to stress the fact that OD proper function and evolution must be assessed through imaging techniques throughout all different stages.16,27
Multiple studies have described OD techniques. These techniques have been performed vertically as well as horizontally, according to the requirements of the anatomical site where they were performed.3,12,33 As is the case in any procedure of bone or soft tissue regeneration it is important that, once the formation of new tissues is achieved, these tissues initiate a functioning phase. This will allow the maintenance of this newly formed tissue which would otherwise become atrophic.9,11,12,16
BONE INTEGRATED IMPLANTS
Totally or partially edentulous patients experience the need to substitute missing teeth. This goal can be achieved with either conventional dentistry practice, with removable dentures, or with implant-supported prostheses.12,18
Since olden times, in ancient civilizations, there have been reports of how important it was for man to possess healthy and complete dentition. Thus, the need arose to substitute missing teeth through man-to-man tooth transplant; this evolved to the practice of re-implanting one tooth of the same individual from one place to another. At a later stage, the use of alloplastic materials was incorporated. In this system the objective was to achieve anatomical and functional rehabilitation of the mouth substituting missing teeth with the help of intra-osseous posts.35
In the 60's, in a fortuitous manner, Professor Per-Ingvar Branemark, while performing research on patella microcirculation, discovered the event of osseous integration, which he later proceeded to describe. Initially, the study was conducted in an experimental manner. At a later point, on a biological basis its use was studied, inasmuch as it pertains to dentistry, with dental implants made of titanium.36 From this point onwards, many researchers have directed their efforts towards animal research to sustain and determine proper conditions and planning for the use of these dental implants. The aim of this research was to support a dental prosthesis which could allow proper function of the dental arches3 thus achieving increased patient masticatory, phonetic and esthetic levels.11,37 More recently, in scientific literature, there have been reports of dental implant use for lower jaw reconstruction with fibula-free grafts.3,12,19,38
CLINICAL CASE PRESENTATION
We hereby present procedures performed on a 49 year old male patient, born in Mexico City and residing in Cuernavaca, Morelos. Patient granted consent for publication of study. The patient sought treatment at the Maxillofacial Prosthesis Clinic of the Graduate School, National School of Dentistry, National University of Mexico (UNAM). Inter-consultation was later conducted with the maxillofacial and oral surgery service at the same institution. The patient presented deformity in the lower third of the face caused by sequels of lower jaw reconstruction procedures caused by a gunshot 15 years before. The patient informed he had been operated on many times, when reconstruction was attempted with micro-vascular fibula graft. Free flaps from the left forearm were equally applied to substitute skin. The patient arrived at our service seeking consultation to obtain complementary treatment for his facial deformity.
In our service, a surgical protocol was established for the reconstruction of the lower jaw facial deformity. Facial esthetic analysis revealed lower jaw region asymmetry caused by placement of skin grafts. The patient also presented lack of soft tissue bone support in vertical direction in the chin and both sides of the jaw. The right side was more apparent, nevertheless, there was no severe disharmony in facial vertical thirds. The asymmetry was limited to facial contour. There was clear presence of scars and grafts. Profile's esthetic analysis showed no anterior-posterior disproportion in the upper and lower jaw relationship; this provided us with the guideline to undertake a surgical decision. In the lip region, absence of the lower lip left vermillion border was observed. As a consequence an extra-oral projection of the tongue was evident. Clinical intra-oral evaluation revealed absence of most lower teeth, isolated presence of right lower molar with partially destroyed crown, absence of vestibular pouch in anterior region, and presence of skin tissue as a result of grafting procedures to cover oral mucosa defects. With respect to inter-maxillary space, based on present occlusions and remnant molar, we found a 10 mm distance from lower mucosa surface to palate middle coronary third of upper teeth. Skull lateral radiographic studies and orthopantomography revealed cephalometric values corroborating previous esthetic assessment of the patient. This was evident in upper and lower jaw anterior-posterior relationship. Other observations were vertically deficient bone chin, as well as bilaterally deficient mandibular bodies. At a later point in treatment, a computerized tomography was requested, with tri-dimensional reconstruction, compatible with DICON software system (Microsoft certified partner ISV/Software solution). A stereolythography was also conducted (Z-printer 310, Z Corporation) at the maxillofacial prosthesis service. Upper and lower jaw anterior-posterior harmony was once more confirmed as well as existing bilateral lower jaw vertical atrophy in the chin region. In accordance with our service's protocol, surgical treatment was mainly aimed at patient's needs and expectations. The patient expressed, in priority order, concern for facial asymmetry caused by graft scarring, incontrollable, extra-oral tongue exposition and absence of teeth which prevented satisfactory phonation and mastication.
A four phase surgical treatment plan was devised in conjunction with the maxillofacial prosthesis service. In the first phase, an increase in vertical-caudal direction of the chin region would be attempted, to confer to the chin greater bone support. This procedure would also elicit distension of redundant soft tissue and lesser scar visibility with the help of OD. In the second phase, the distraction device was removed from the lower jaw region, bone distractors were bilaterally placed in jaws. Based on symmetry observed in facial-esthetic analysis, a 16 mm distraction was planned for the right side and a 10 mm distraction was planned for the left side. This was based on millimeter differences observed in vertical dimension of left side compared to right side. An attempt was made to obtain sufficient vertical bone tissue, to later be able to insert bone integrated implants longer than 10 mm. In the third surgical phase, lower jaw distractors would be removed and oral mucosa flaps would be rotated so as to reconstruct the vermillion border of left lower mid-lip. The fourth phase would involve placement of bone-integrated implants (Figure 1).

SURGICAL TECHNIQUE
First Phase: With patient under general, balanced anesthesia and naso-tracheal intubation, intra-and extra-oral region were subjected to asepsis and antisepsis. Incision was made with scalpel blade num. 15 in chin region, resecting present scar. Region was resected by planes until reaching bone tissue. An alveolar distractor (Track distractor, 15 mm, KLS Martin L.P. Jacksonville Fl) was placed. This distractor has a 15 mm distraction magnitude. This distractor had previously been adapted according to the contour shown in the stereolythographic model. The device is fixed with 2 mm thick, 10 mm long titanium screws (W Lorenz, HTX-Drive, Jacksonville, Fl). Osteotomies are recorded with oscillating saw (Stryker Corp, Kalamazoo, Mich. USA). Bone distractor is removed, oscillating saw osteotomies are joined, and osteotomy is completed with osteotomes. A bone distractor was placed once again, and distractor functionality was assessed. Plane by plane closure was undertaken, using chromic catgut 3-0 in deeper planes, and nylon 4-0 in skin planes. Hemostasis was assessed and surgery was deemed completed. After a 5 days latency period,34 ambulatory consultation took place to achieve bone distractors activation. 1 mm was distracted every 24 hours. X-rays controls were performed at the distractors middle distracting point, as well as when distraction phase was completed. Once distraction was completed, a 12 week consolidation period was observed. In this period, weekey control assessments were undertaken. At the end of the latent period a new, tridimensional reconstruction computed tomographywas taken. A new stereolythographic model was taken upon completion of the consolidation period (Figure 2).
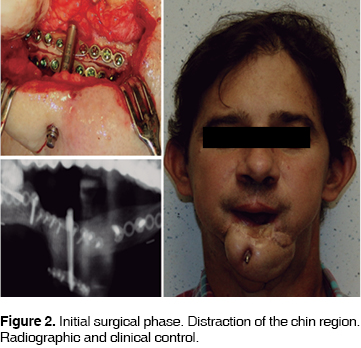
Once the consolidation period was completed, reprogramming was undertaken to withdraw the distractor from the chin region to thus later place bilateral distractors in the lower jaw body (Phase 2). Under general anesthesia and naso-tracheal intubation, an incision was made in the chin region over the previous incision scar. Dissection by planes was undertaken until bone region was approached. Distractor plates were identified, newly-formed bone tissue was clinically assessed. Distractor was then withdrawn, in the chin region an incision was performed around the distraction device rod. Suturing by planes was undertaken with 3-0 chromic catgut in deeper planes, and 4-0 nylon in skin planes. After this, an incision in the right, lower jaw basal ridge region was performed. Dissection by planes was undertaken until the bone was reached. All pre-existing previous fibula micro-vascular reconstruction materials were removed. The distractor was put into place, having previously been contoured according to the stereolythographic model. The distractor was fixated into place, osteotomies and osteotomes were marked with oscillating saw. Bone distraction functionality was assessed and recorded with oscillating saw, plane by plane closure was undertaken with chromic catgut 3-0 in deeper planes and 4-0 nylon in superficial planes. The same procedure was performed in a counter-lateral manner. Observing, as in the first phase a 5 days latency period, a 1 mm every 24 hours distractor activation was undertaken.34 The procedure was continued until reaching the desired 16mm length in the right side and 10mm length in the left side (Figure 3). Once the distraction period was completed, a 6 month consolidation time was observed, to later remove distractors under general anesthesia. A six month period was observed due to the patients recent exposure to two anesthesia events and to decrease risks of liver damage. After the six month period was observed, distractors were withdrawn (Third Phase). During procedure, presence of newly formed bone formation could be clinically observed. Bilateral bone defects were also present in the vestibular cortical region. Surgical wounds were sutured with chromic catgut 3-0 in deeper planes and 4-0 nylon in superficial planes. At this point jugal intraoral mucosa flap rotation was performed, to achieve reconstruction of the left mid-lip vermillion border (Figure 4). Two months later, a new tridimensional tomography study was undertaken to build a stereolythographic model. This model will be of use when planning the insertion of bone-integrated implants in the process of rehabilitation with prostheses supported by implants and mucosa.
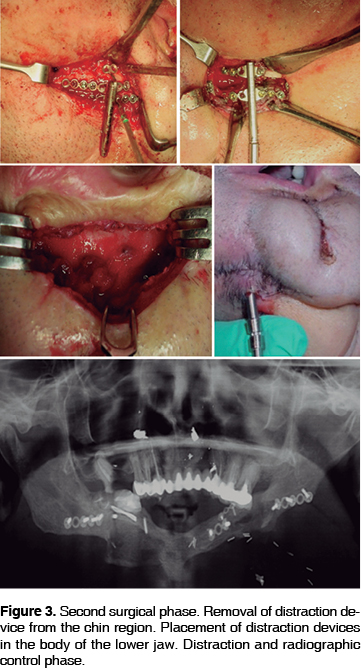

In agreement with treatment plan, it was decided to place 5 implants (IMTEC Corporation, Oklahoma, USA, ENDURE) in the lower jaw region (4th phase). Characteristics of implants were as follows: one 4.3 mm thick, 11mm long implant along the right side; two 4.3 thick, 14 mm long implants in the chin region and two 4.3 mm thick 11 mm long implants in the left side. Surgical guides were drafted according to the stereolythographic model. Placement of implants was programmed with patient under general anesthesia. Intraoral incision was performed muco-periosteal flap was raised so as to locate bone tissue. Once the surgical guide was in place, progressive burr-drilling was performed to insert implants according to the program. Some implants required two-phase placement protocol. Repositioning of flap was undertaken. Proper position and parallelism were assessed through x-ray control. Suturing was performed with 3-0 chromic catgut. Ten days after surgery, radiographic control was conducted. This same control was conducted three months after surgery, and revealed no clinical or radiographic data of inadequate integration (Figure 5). The uncovering of implants was programmed once again under general anesthesia. Locator-type prosthetic placement devices were put into place, and a transitional immediate provisional prosthesis was placed. A control visit was conducted 8 days after surgery, at this point the patient was referred to the maxillofacial prostheses service to undertake final prosthetic rehabilitation.

DISCUSSION
In our days, there are different techniques widely studied for the reconstruction of jaws with horizontal and vertical bone deficiencies. These techniques aim at providing bone support to provide sufficient bone structure which, in turn, is able to sustain a conventional prosthesis, or, as well, to provide rehabilitation involving implant support.3,9,11,12,18
Among the aforementioned techniques we can count the following: block bone grafts,18 particulate grafts which have intra-oral and extra-oral homologue donors, and finally, use of alloplastic and heterologous materials. A more recent technique used is osteogenic distraction.7,11,21,39
The main objective of all these materials and techniques was primarily to provide, or re-establish the function of the stomatognathic system, and as a secondary objective the reconstruction of anatomical shape.8
Many scientific literature publications perused, establish the fact that the best reconstructive materials are autologous type grafts. Theses grafts are required for formation of newly formed bone tissue, either through osteo-induction or osteo-conduction. Other types of heterologous materials provide a somewhat successful but limited functionality.3,7-9,11,12
Heterologous materials main advantages are the following: a) Absence of need to find an extra donor site which confers surgical procedures lesser morbidity degree. b) The fact that unlimited amounts of grafting materials is available, c) Desired bone volume instauration achieved in an immediate fashion.3,21,39 Providing thus an adequate stroma which will ease bone conduction and newly formed bone formation. Incidentally, surgical time is reduced and the need of two surgical teams is averted. Disadvantages of this technique are the following: increase in surgical and financial costs, higher degree of graft resoption,9,18 and in some allogenic-type materials, the inability to be absorbed. Other disadvantages are longer periods required for graft integration, and as a consequence, final patient rehabilitation. For all the aforementioned reasons, in the 90's a trend was retaken inasmuch as autologous type materials could provide better advantages. Reasons for this were the following: ability to offer osteo-inductive and osteo-conductive osteogenic properties, thus decreasing final rehabilitation time for the patient. Another advantage was the decrease in graft absorption degree, which in turn would reflect as greater amount of newly-formed bone tissue which then would decrease the possibility of rejection and illness transmission.3,7,11,12
After studying several scientific reports on the matter, we can propose the idea that autologous graft harvesting sites for the reconstruction of alveolar ridges, those more beneficial for the patient, were the ones having greater amounts of spongy bone. This is due to the high content of cellular elements in this bone able to form new bone material through their own cells of the normal bone tissue. Another element to be considered is the incorporation of cellular elements32 with phenotypic transformation ability towards different elements that constitute the newly-formed bone tissue maturation and formation.16 In a similar fashion, it was found that even with autologous grafts, the consistency of newly formed bone incorporating in a reticulated fashion, offered grater rates of success when compared to autologous type grafts used in block.9,18 There was the need to re-create a structure which could keep them in their receptor bed and were also capable of providing a structure, which could protect the graft from resorption due to compression of adjacent soft tissue, thus avoiding wound dehiscence.18,27,39
Considering all these facts, regeneration technique started to become popular. This was not a new technique, but its use has been increasing; we are referring to OD techniques for the maxillofacial region.1,9,18 If we decide to follow this technique, we have the previous knowledge that bone can form and adapt as response to many stimuli. These are dynamic processes dependent upon biochemical properties of bone tissue and which can regenerate and remodel bone structures.19 Many studies have shown that mechanical load is one of the main effects in bone formation and remodeling.16,18,20 In the process of bone growth and regeneration, osteoblasts and osteocytes are the main cells; they play a critical role in this process by means of inducing bone matrix synthesis and mineralization.35 Osteogenic response to mechanical stimuli depends on the applied force.4,36 OD models are influenced in magnitude to the applied force and will influence single-axis deformation. Experimental studies inform of reasons why cells proliferate and differentiate. In these studies, application of 1,000 to 2,000 μ significantly increases cellular proliferation towards an osteoblastic cell type as well as cytokine secretion.
An excessive increase in forces (above 10,000 μ) equally produces an increase in cellular proliferation as well as production of type I collagen, nevertheless, it elicits decrease in osteo-calcium expression.4,35,36
When following the techniques just described, we can regenerate sufficient amount of bone tissue to shape the anatomical form of the area to be reconstructed and offer as well sufficient bone structure to later embark on proper prosthetic rehabilitation.3,9,18
All the above has been conducted following bases and principles established by Dr Gabriel O. Ilizarov, Kurigen, Russia3,25 who mentioned the fact that small forces of same intensity applied over a bone gap at a proper rhythm, were able to promote new tissue formation of same tissue strain within the gap.2,35,36
Besides being able to achieve newly formed bone tissue, we could achieve newly formed soft tissue production5,19 this was one of the keys to success in the other reconstruction techniques. This could be considered as osteo-distraction,3 and we could waylay the need to prepare an additional surgical area to harvest the tissue to be grafted.5 This technique can be considered versatile inasmuch as it can provide several simultaneous regeneration vectors9 thereby allowing production of vertical and horizontal new tissue.3,13,16,18
This versatility allowed us to design distraction, not in cephalic direction, as was done previously, but instead in caudal direction. This could be achieved due to the fact that we possessed proper interocclusal distance to install proper therapy based on implant support.9 We needed to bear in mind that the patient rated equally important to have an appropriate oral prosthesis and to try to improve his facial contour. All these reasons led us to decide upon the aforementioned procedures in their different surgical stages.9
The goals to be met were obtaining better symmetry in facial contour, reduce previously grafted soft tissue laxity with the help of better bone support, as well as creating proper bone support for the later insertion of dental implants.3,9 Our objectives also were left lower mid-lip reconstruction and a final rehabilitation of a prosthesis supported by implants.
CONCLUSIONS
Based on the objectives outlined in this clinical case we must conclude that osteogenic distraction is a viable and effective option for the esthetic and functional reconstruction of jaws requiring rehabilitation caused by hereditary or acquired defects. Following this technique we additionally managed to decrease the difficulty encountered by soft tissues as a consequence of all previous reconstructions. This was especially so in vertical direction, and in this particular clinical case where the patient was found to possess a great amount of redundant soft tissue, as well as presence of numerous scars. The patient was suffering from lack of flexibility and fibrosis in the skin grafts located in the lower jaw region. In cases when the interocclusal state of the patient is found within the boundaries of accepted parameters, if we want to achieve proper prosthesis-implant prognosis, we can create sufficient bone tissue to achieve better facial symmetry and provide enough bone for the insertion and bone-integration of dental implants.
REFERENCES
1. Swennen GRJ, Eulzer C, Schutyser F, Hüttmann C. Assessment of the distraction regenerate using three dimensional quantitative computer tomography. Int J Oral Maxillofac Surg 2005; 34: 64-73. [ Links ]
2. Rachmiel A, Srouji S, Peled M. Alveolar ridge augmentation by distraction osteogenesis. Int J Oral Maxillofac Surg 2001; 30: 510-517. [ Links ]
3. Klesper B, Lazar F, Sie-Egger M. Vertical distraction osteogenesis of fibula transplants for mandibular reconstruction: a preliminary study. J of Cranio Maxillofac Surg 2002; 30: 280-285. [ Links ]
4. Schleier P, Hyckel P, Fried W, Beinemann J. Vertical distraction of fibula transplant in a case of mandibular defect caused by shotgun injury. Int J Oral Maxillofac Surg 2006. [ Links ]
5. Swennen G, Schliephake H, Dempf R, Schierle H. Craniofacial distraction osteogenesis: a review of the literature. Int J Oral Maxillofac Surg 2001; 30: 89-103. [ Links ]
6. Pacicca DM, Patel N, Lee C, Salisbury K, Lehmann W. Expression of angiogenic factors during distraction osteogenesis. Bone 2003; 33: 889-898. [ Links ]
7. Boyne PJ. Osseous reconstruction of the maxilla and the mandible. Quintessence Publishing Co, Inc. 1997: 3-11. [ Links ]
8. Gullane PD, Holmes H. mandibular reconstruction: new concepts. Arch Otolaryngology Head Neck Surg 1986; 112: 714. [ Links ]
9. García-García A, Somoza-Martín M, Gandara-Vila P. Alveolar distraction before insertion of dental implants in the posterior mandible. British J Of Oral And Maxillofac Surg 2003; 41: 376-379. [ Links ]
10. Uckan S, Dolanmaz D, Kalayci A, Cilasun U. Distraction osteogenesis of basal mandibular bone for reconstruction of the alveolar ridge. British J of Oral and Maxillofac Surg 2002; 40: 393-396. [ Links ]
11. Bianchi A. Prótesis implantosoportada. Bases biológicas-biomecánicas-aplicaciones clínicas. Primera edición; 2001. [ Links ]
12. Chiapasco M, Romeo E. Rehabilitación implantosoportada en casos complejos. AMOLCA 2006. [ Links ]
13. Schwartz HC. Mandibular reconstruction using the dacron-urethane prosthesis and autogenic cancellous bone: review of 32 cases. J Plast Reconstruct Surg 1984; 73: 387-92. [ Links ]
14. Tayaponsak P, O'Brien DA, Monteiro CB, Arreo-Diaz LL. Autologous fibrin adhesive in mandibular reconstruction with particulate cancellous bone and marrow. J Oral Maxillofacial Surg 1994; 52: 161-166. [ Links ]
15. Macintosh RB, Henny FA. A Spectrum of application of autogenous costocondral grafts. J Maxillofac Surg 1997; 5: 257. [ Links ]
16. Meyer U, Kleinheinz J, Joos U. Biomechanical and clinical implications of distraction osteogenesis in craniofacial surgery. J Of Cranio-Maxillofacial Surg 2004; 32: 140-149. [ Links ]
17. Moses JJ. Alveolar and skeletal distraction osteogenesis for the maxillofacial surgeon. Surgical Clinics Aaoms 2005: 137. [ Links ]
18. Block MS, Chang A. Mandibular alveolar ridge augmentation in the dog using distraction osteogenesis. J Oral Maxillofac Surg 1996; 54: 309-314. [ Links ]
19. Bouletreau PJ, Warren SM, Longaker MT. The molecular biology of distraction osteogenesis. J of Cranio Maxillofac Surg 2002; 30: 1-11. [ Links ]
20. Meyer U, Meyer T, Schlegel W, Scholz H. Tissue differentiation and cytokine synthesis during strain-related bone formation in distraction osteogenesis. British J of Oral and Maxillofac Surg 2001; 39: 22-29. [ Links ]
21. Kanno T, Takahashi T. Tensile mechanical strain up-regulates. Runx2 and osteogenic factor expression in human periosteal cells: Implications for distraction osteogenesis. 10.1016/Joms.2004.07.023. [ Links ]
22. Lynch SE, Genco RJ, Marx RE. Tissue engineering. Application in maxillofacial. [ Links ]
23. Swennen GRJ, Schutyser F, Mueller MC, Kramer FJ. Effect of platelet-rich-plasma on cranial distraction osteogenesis in sheep: Preliminary clinical and radiographic results. Int J Oral Maxillofac Surg 2005; 34: 294-304. [ Links ]
24. Shvyrkov MB, Shamsudinov AH. DD non-free osteoplasty of the mandible in maxillofacial gunshot wounds: mandibular reconstruction by compression-osteodistraction. British J of Oral and Maxillofac Surg 1999; 37: 261-267. [ Links ]
25. Hasse ARF, Örksen MP, Zimmermann CE. Bilateral mandibular distraction in adult dogs with an epiperiosteal distractor. British J of Oral and Maxillofac Surg 2005; 43: 105-112. [ Links ]
26. Kessler AP, Neukama FW, Wiltfang JB. Effects of distraction forces and frequency of distraction on bony regeneration. British J of Oral and Maxillofac Surg 2005; 43: 392-398. [ Links ]
27. Klug CN, Millesi-Schobel GA. Preprosthetic vertical distraction osteogenesis of the mandible using an l-shaped osteotomy and titanium membranes for guided bone regeneration. J Oral Maxillofac Surg 2001; 59: 1302-1308. [ Links ]
28. Yazawa M, Kishi K. Expression of bone morphogenetic proteins during mandibular distraction osteogenesis in rabbits. J Oral Maxillofac Surg 2003; 61: 587-592. [ Links ]
29. Heffez LB, Kirton M. Vector control in transportation osteogenesis. J Oral Maxillofac Surg 2005; 63: 737-746. [ Links ]
30. Suhr MAA, Kreusch TH. Technical considerations in distraction osteogenesis. Int J Oral Maxillofac Surg 2004; 33: 89-94. [ Links ]
31. Swennen G, Dempf R, Schliephake H. Craniofacial distraction osteogenesis: A review of the literature. Part II: experimental studies. Int J Oral Maxillofac Surg 2002; 31: 123-135. [ Links ]
32. Miloro M. Peterson's principies of oral and maxillofacial surgery. 2nd edition, Bc Decker Inc, 2004: 783-801. [ Links ]
33. Al Ruhaimi KA. Comparison of different distraction rates in the mandible: An experimental investigation. Int J Oral Maxillofac Surg 2001: 30: 220-227. [ Links ]
34. Robiony M, Toro C, Stucki-Mccormick SU. The ''Fad'' (Floating Alveolar Device): A bidirectional distraction system for distraction osteogenesis of the alveolar process. J Oral Maxillofac Surg 2004; 62 (Suppl 2): 136-142. [ Links ]
35. Lozada JL, Goodacre C. The history of implant dentistry. Loma Linda University Calf. [ Links ]
36. Nobel Biocare Services AG. The story about an invention that makes people smile. Sweden 2005. [ Links ]
37. Sieg P, Zieron JO, Bierwolf S, Hakim SG. Defect-related variations in mandibular reconstruction using fibula grafts. A review of 96 cases. British J of Oral and Maxillofac Surg 2002; 40: 322-329. [ Links ]
38. Askew A, Fleming PS, Downie IP. Adjunctive use of dental implants in mandibular reconstruction with a free fibular graft. British J of Oral and Maxillofac Surg 2005; 43: 341-342. [ Links ]
39. Garg-Arun K. Bone biology, harvesting, and Grafting for dental implant: rationale and clinical applications. [ Links ]
RECOMMENDED LITERATURE 1. Meyer U, Meyer T, Hans-Peter WF. The effect of magnitude and frequency of interfragmentary strain on the tissue response to distraction osteogenesis. J Oral Maxillofac Surg 1999; 57: 1331-1339. 2. Cope JB, Samchukov ML, Cherkashin AM. Biomechanics of mandibular distractor orientation: An animal model analysis. J Oral Moxillofac Surg 1999; 57: 952-962. 3. Klein C, Papageorge M, Kova' A, Carchidi JE. Initial experiences using a new implant based distraction system for alveolar ridge augmentation. Int J Oral Maxillofac Surg 2001; 30: 167-169. 4. Schmidt BL, Kung L. Induced osteogenesis by periosteal distraction. J Oral Maxillofac Surg 2002; 60: 1170-1175. 5. Demann ET, Haug RH. Do position and soft tissue affect distraction vector? an in vitro investigation. J Oral Maxillofac Surg 2002; 60: 149-155. 6. Meyer U, Meyer T, Wiesmann HP, Kruse-LöSler B. Mechanical tension in distraction osteogenesis regulates chondrocytic differentiation. Int J Oral Maxillofac Surg 2001; 30: 522-530. 7. Hibi H, Ueda M. New internal transport distraction device for reconstructing segmental defects of the mandible. British J of Oral and Maxillofac Surg 2005. 8. Rassekh C, Clements N. Reconstruction mandibular, Utmb Department Of Otolaryngology 1997. 9. Hidalgo DA. Fibula free flap: a new method of mandibular reconstruction. Plast Reconstruct Surg 1989; 84: 71. 10. Rivas B, Ochoa F et al. Mandibular reconstruction with the free vascularized fibular flap: utility of three-dimensional computerized tomography. Journal Of Reconstructive Microsurgery 1999; 15 (2). Note This article can be read in its full version in the following page: http://www.medigraphic.com/facultadodontologiaunam Mailing address:
Mailing address:
René Jiménez Castillo
E-mail: renejimenezca@gmail.com











 texto en
texto en 


