Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista odontológica mexicana
versión impresa ISSN 1870-199X
Rev. Odont. Mex vol.15 no.2 Ciudad de México abr./jun. 2011
Original research
Marginal adaptation and microleakage comparison between two zirconia oxide systems with the same cement
Adriana Juárez García,* Federico Barceló Santana,§ Enrique Ríos SzalayII
* Graduated of Oral Prosthesis and Implantology Department, División de Estudios de Posgrado e Investigación, Facultad de Odontología de la UNAM.
§ Professor, Dental Materials Laboratory, División de Estudios de Posgrado e Investigación, Facultad de Odontología de la UNAM.
II Professor, Oral Prosthesis and Implantology Department, División de Estudios de Postgrado e Investigación, Facultad de Odontología de la UNAM.
ABSTRACT
Objective: To compare the marginal fit and micro-leakage of Lava™ and Zirkon zahn® copings using the same cement as adhesive. Material and methods: Twenty extracted superior premolars were divided into two groups. Teeth in the first group were prepared to receive Lava™ copings, while teeth in the second group were prepared for Zirkon zahn® copings. Copings were prepared following each systems standard procedure. Marginal fit was measured in micrometers in eight different regions, both before and after being bound with RelyX™ U100 cement. Once thermocycled, samples were soaked in 2% fuchsin dye solution and buccolingually sliced, microleakage was measured, both in the vestibular and palatal regions. Results: A statistically significant difference in marginal fit between the two zirconia systems was found. Lava™ registered the best adaptation values: 19.7 µm before cementation and 15.0 µm after, while Zirkon zahn® reported marginal fit values of 28.1 µm (before) and 22.8 mm (after cementation). In contrast, we found no significant difference in microleakage: Lava™ averaged 314.2 µm and Zirkon zahn® 319.8 µm. Conclusion: Lava™ registered better marginal fit values than Zirkon zahn®, but no significant difference in microleakage.
Key words: Marginal fit, microleakage, zirconia, CAD-CAM.
INTRODUCTION
Both dentists and patients expect restorations to have the best functional and aesthetic features. They expect them to show the best marginal adaptation, biocompatibility, color stability, durability, adhesive strength, and resistance, the lowest thermal conductivity and a radiographic contrast similar to dentine. This has led them to demand fully ceramic restorations both for anterior and posterior teeth.1 Nowadays, several fully ceramic restoration systems show all these features,2-4 Lava™ and Zirkon zahn® among them.
Lava™ comprises a CAD/CAM procedure (scanning, computer-aided framework design and milling) for the fabrication of Zirconia Oxide structures, coated with Lava Ceram™ overlay porcelain, suited for individual anterior and posterior restorations and fixed prosthesis of up to eight units. Either a rounded shoulder or chamfer with a horizontal angle of ≥ 5° and a vertical angle of ≥ 4° are optimal preparations for scanning. These restorations can be cemented with glass ionomer or resin cements.3
Zirkon zahn® is a manual milling system for building Zirconia Oxide constructions developed by Enrico Steger.5 Acording to Steger himself, the system is well suited for individual anterior and posterior restorations as well as segments of up to 14 units. Restorations can be finished in all sorts of ways: beveled or non-beveled shoulder, chamfer or blade. They can also be cemented with glass ionomer or resin cements.6
One of the most important properties of prosthetic restorations is their marginal adaptation,7 i.e. the distance between the tooth's restoration line and its margin, or the degree of proximity and interlocking of filling material to the wall of the cavity of a tooth.8 Poor marginal adaptation or too large an opening negatively affects the restoration's strength, reduces its longevity and leads to a higher risk of recurring caries and periodontal illness.9 It can also fracture the cement, allowing the seepage of fluids, debris, and microorganisms along the interface between the restoration and the walls of the cavity preparation (microleakage). This causes marginal discoloration, pulpal irritation, secondary carious lesions and possible cement mechanical failure.10
According to ISO specification 4,049,11 from 2,000, layers of resin-based cements layers should not be wider than 50 µm.
In 2004, Francine found substantial differences among cements in their capacity of withstanding microleakage. After studying the microleakage of IPS Empress - 2 (Ivoclar -Vivadent) crowns fixed with three different cements, Gu X-H and Kern M concluded that using resin based cements significantly reduces microleakage.10
Several methods for studying porcelain zirconia systems have been proposed in the literature. Among them, Holmes12 established a uniform vocabulary for referring to the characteristics under study: internal opening, marginal opening, horizontal and vertical marginal discrepancy, short and over marginal extension, marginal absolute discrepancy and settlement discrepancy. Other studies on marginal fit,13,14 detail their evaluations in different regions: labial, mesial, distal and lingual. In all cases, good marginal adaptation is key to a successful restoration.
The goal of this study was to compare the marginal fit (on eight regions) and (palatine and vestibule) microleakage of two zirconia systems. Our hypothesis was that computer drilling and manual drilling must differ in marginal fit, both with and without cement, but must not differ in microleakage.
MATERIAL AND METHODS
The study was comparative, experimental and transversal. A pilot test was carried out using two samples of each zirconia system.
20 superior premolars were selected, all of them free of caries or restorations and extracted less than 6 months before the test. They were cleaned of any organic material with an ultrasonic scaler NSK® and placed in a glass container with water to keep them moist.
The teeth were placed in individual type III gypsum cast blocks in order to prepare metal free crowns, with a 2 mm cervical chamfer finish line between dentine and cement and a uniform 1.8mm depth. Brasselerdiamond® USA diamond burs were used: a D12M diamond bur was used in axial sides, a diamond flat end tapered D83 bur was used to prepare the vestibular, mesial, distal and palatine walls following the gingival margin, a diamond flat end tapered D82 bur was used to reduce 1.8mm off the occlusal surface, and a football shaped diamond bur D16G was used to prepare the occlusal surface. Finally, a flat end tapered Shofu™ Arkansas stone (aluminum oxide) was used to give the surface a smooth finish.
Impressions were taken following the manufacturers' instructions, using siloxane, 3M Express™ polyvinyl and Dentsply® Rim Lock trays. 12 hours later, positives were cast on GC Fuji Rock® gypsum.
The technical work necessary to make the Lava copings™ was made by the "Kobe" laboratory in Mexico City (a lab authorized by LAVA™ Milling Center), while the Zirkon zahn® copings were elaborated in the "Estudio Dental Fusión" laboratory in Cuernavaca, Morelos, Mexico.
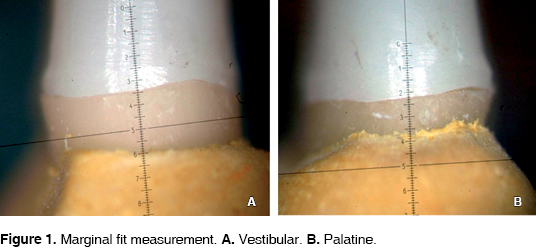
Copings were placed with digital pressure, without cement, on the premolars. Marginal fit was measured on eight regions: one vestibular, one palatal (Figure 1), three mesial and three distal (Figure 2). Measurements were obtained with a 70X magnification LOMO® MBC - 10 model microscope (approx. five microns). Copings were then cemented with RelyX™ U100 3M ESPE AG, with a 15 kg load. Immediately thereafter, marginal fit measurements were taken, as previously described.

Twenty-four hours after cementation, samples were removed from the gypsum blocks and brought to thermocycling, totaling 500 cycles between 5 °C and 55 °C: 20 seconds in each temperature, and 10 seconds at 22 °C ± 2 between them. Then, all the premolar roots were varnished and their coronal surfaces were immersed in 2% fuchsine dye solution for 24 hours. Samples were placed in resin blocks to be bucco-lingually sectioned with a Hamco Machine® Thin Sectioning Machine cutter with a 0.5 mm thick High TechProducts. In Diamond Waterine Blade 65-10,005 diamond disk.
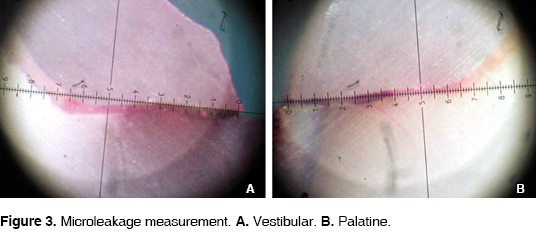
Microleakage was measured in each vestibular and lingual section using a 70X magnification LOMO® MBC-10 model microscope (approx. five microns) (Figure 3).
A photograph of each measurement was taken through the aforementioned microscope with a NIKON D 70S camera. Marginal fit values were analyzed by one way ANOVA, the group comparison by a TUKEY multiple test, and the microleakage by a t - test on Sigma stat 2.0 software.
RESULTS
Figure 4 shows the average marginal fit in microns of each zirconia system's samples before and after cementation. The ANOVA test statistical analysis shows that the group with the best marginal fit without cementing was LAVATM with an average of 19.7 µm and a standard deviation of 5.4. LAVATM also performed the best when using cement, showing an average of 15.0 µm and a standard deviation of 4.1.
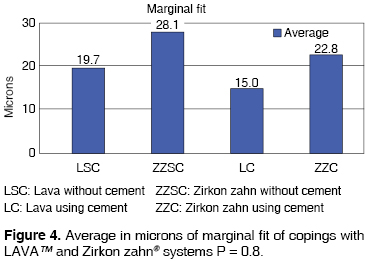
The group with least marginal fit was Zirkon zahn®, without cementing. It showed an average of 28.1 µm and a standard deviation of 3.3, followed by Zirkon zahn® using cement with 22.8 µm and a standard deviation of 5.6, all with a P of 0.8.
The TUKEY test showed a P < 0.05 statistically significant difference between the ZZCC and LC groups, the ZZSC and LSC groups, and between the ZZC and LSC groups; no other group combinations showed any statistically significant differences.
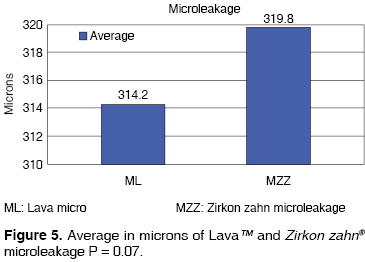
Figure 5 shows the microleakage averages in microns. Lava's microleakage was lower (314.2 µm average and a standard deviation of 194.9) than Zirkon zahn® (319.8 µm average, and a standard deviation 115.6). However the statistical analysis showed, with a 95% confidence level, that this difference is not statistical significant.
DISCUSSION
One of the main criteria to evaluate the adequacy of a restoration is its marginal fit, and there are different methods in the literature to measure it. The systems evaluated in this study, with the described methodology, show a lower marginal fit than other ceramic systems,15,16 probably because of technological development and new materials.
Similar methodologies to the one used in this study have been used to assess marginal fit. For example, authors like Shirley17 and Wolfart9 measured the samples both before and after cementing, using different loads and buco-lingually sectioning the samples.
In his work, Shirley17 reported higher marginal fit values in ceramic crowns and metal ceramic crowns after cementing. Our current study found lower values after cementation. This could be because Zirconia technology was designed to improve marginal fit.
Matty18 compared the marginal fit of Cerestore and Dicor crowns, metal ceramic crowns with metallic margin and metal ceramic crowns with ceramic vestibular margin. The four systems showed a marginal fit ranging from 56 to 81 µm. These values were higher than those obtained in this study, and the difference may be related to the different methods and systems used to assess the fit: Matty used artificial teeth, cemented the crowns with a 5 kg load and sectioned them bucolingually. He also made three vestibular and palatine measurements, and his slices were separated by 100 microns.
Francine10 compared Procera® with metal porcelain crowns, reporting values of 54 and 29 mm respectively. He used molars and cemented the crowns with a 5 kg load. The values in the present study are lower, and once again this could be due to the different methodologies used.
There are no reported studies about Zirkon zahn 's® marginal fit to compare the present study with. However there are studies of LavaTM, like Piwowarczyk and Lauer from Frankfurt University. In the 2006 Conference of the European Division of the International Association of Dental Research (IADR, PEF),19 they presented a comparative study of the marginal fit of LavaTM zirconia units, Cercon®, and DCS. Their results agree with ours in so far as LavaTM also shows the overall best marginal fit.
Beuer20 compared the marginal fit of LavaTM and Procera®, obtaining values of 50 (± 7) mm and 108 (± 13) µm respectively. Lava results in our study are lower than those reported by Beuer. This can be due to the fact that Beuer carried out his research in artificial teeth and cemented them with a load force of 50 N.
AJT Shannon et al. in the IADR journal 2007,21 published a vertical marginal opening comparison between several CAD-CAM systems: KaVo Everest (ZH, ZS), Nobel Biocare Procera ® (MOD40, Piccolo, Forte), 3M ESPE Lava™, Wieland Zeno, y Cerec inLab (InCeramZr) and a plaster control group. In their work, only Lava copings did not show a significant difference with the control group. This led them to conclude, just as we did on our own study, that Lava's marginal fit is the best.
According to G Hertlein et al,22 restorations' clinical success depends heavily on their mechanical properties and design, but also on the accuracy of the CAD-CAM process. The purpose of their study was to determine the marginal fit of restorations made with zirconia. They reached the conclusion that Lava™ shows an acceptable fit (with a lowest value of 50), and our report agrees.
Francine et al.10 mention that there is no universal technique to measure microleakage, but several diverse methodologies.23,24 Francine used a five value scale in his study where 0 meant no microleakage, 1 meant microleakage over a third of the axial wall, 2 meant microleakage over two thirds of the axial wall, 3 meant microleakage all along the axial wall and 4 meant microleakage on the occlusal surface. This was carried out to assess the effect of the following cements: zinc phosphate, glass ionomer, resin modified glass ionomer, resin base cements with Procera and metal porcelain systems. They concluded that resin based cements show low microleakage values, whereas zinc phosphate cements present higher microleakage values.
Besides studying its marginal fit, Rosentritt et al.24 measured microleakage percentages in LavaTM using different cements. In their study, RelyXTM Unicem showed the lowest percentage. In our study, we used RelyXTM U100 3M, a cement that has the same composition but different presentation and manipulation than RelyXTM Unicem.
Our study used only a single cement, so we suggest to carry on similar studies covering more materials.
CONCLUSIONS
In this study, LavaTM statistically proved to be the system with the best marginal fit, while Zircon zahn® showed the worst. Nevertheless, it must be pointed out that there was no significant difference in microleakage between both systems.
REFERENCES
 Address correspondence:
Address correspondence:
Federico Humberto Barceló Santana
Sur 73 A Número 14
Col. Ampliación Sinatel
09470 D.F. México
Phone: 55329925
E-mail: barcelo@servidor.unam.mx
Note
This article can be read in its full version in the following page: http://www.medigraphic.com/facultadodontologiaunam
1. Suárez M, González P, Pradíes G, Lozano J. Comparison of the marginal fit of Procera AllCeram Crowns with two finish lines. Int J Prosthodont 2003; 16: 229-232. [ Links ]
2. Nakaruma T, Dei N, Kojima T. Marginal and internal fit of cercec 3 CAD/CAM All – Ceramic Crowns. Int J Prosthodont 2003; 16: 244-248.
3. Technical Product Profile . Lava™, Precision Solutions, 3M ESPE, 48 pp.
4. Bindl A, Mormann WHM. Marginal and internal fit of all-ceramic CAD/CAM crown-copings on chamfer preparations. J Oral Rehabilitation 2005; 32: 441-447. [ Links ]
5. Steger E. Zirkon zahn para el procesamiento de piezas en verde de material para armazones de dióxido de zirconio. Quintessence técnica (ed. Esp.) 2006; 17: 25-34. [ Links ]
6. www.zirkonzhan.com. Visitada el 09 y 10 de enero del 2009.
7. Weaver J, Johnson G, Bales D. Marginal adaptation of castable ceramic crowns. J Prosthet Dent 1991; 66: 747-53. [ Links ]
8. Glossary of Prosthodontic Terms. J Prosthet Dent 2005; 94: 92. [ Links ]
9. Wolfart S, Martin S, Kern M. Clinical evaluation of marginal fit of a new experimental all – ceramic system before and after cementation. Int J Prosthodont 2003; 6: 587-592.
10. Francine E, Omar M. Marginal adaptation and microleakage af Procera All Ceram crowns with four cements. Int J Prosthodont 2004; 17: 529-535. [ Links ]
11. ISO 4049 : 2000 (E), pp 1-5.
12. Holmes JR, Bayne SC, Holland GA, Sulik WD. Considerations in measurement of marginal fit. J Prosthet Dent 1989; 62: 405-408. [ Links ]
13. Groten M, Axmann D, Probster L, Weber H. Determination of the minimum number of marginal gap measurements required for practical in vitro testing. J Prosthet Dent 2000; 83: 40-9. [ Links ]
14. In-Sung Yeo, Jae-Ho Yang. In vitro marginal fit of three all ceramic crown systems. J Prosthet Dent 2003; 90: 405-408. [ Links ]
15. Coli P, Karlsson. Precision of a CAD/CAM technique for the production of zirconium dioxide copings. Int J Prosthodont 2004; 17: 577-580 [ Links ]
16. May KB, Russell MM, Razzoog ME, Lang BR. Precision of fit: the Procera AllCeram crown. J Prosthet Dent 1998; 80: 394-404. [ Links ]
17. Shirley H, Hung M, Kuen-Shan H, Eick D, Chappell R. Marginal fit of porcelain-fused-to-metal and two types of ceramic crown. J Prosthet Dent 1990; 63: 26-31. [ Links ]
18. Matty F, Tjan A, Fox W. Comparison of the marginal fit of various ceramic crown systems. J Prosthet Dent 1989; 61: 527-31. [ Links ]
19. Piwowarczyk A, Lauer H. Determining the marginal fit of CAD/CAM bridge frameworks, Pan European Federation Conference (PEF; CED) #0254, 2006 . [ Links ]
20. Beuer F, Naumann M, Gernet W, Sorensen J. Precision of fit: zirconia three-unit fixed dental prostheses . September 2008. [ Links ]
21. Shanon A, Qian F, Gratton D. In-vitro marginal gap comparison of CAD/CAM zirconium copings, IADR #0828 , 2007. [ Links ]
22. Hertlein G, Franfe R, Wastian C, Watzek K. Marginal fit of zirconia restorations with three/four abutment teeth, 3M ESPE AG, Seefeld, Germany .
23. Ibarra G, Johnson G, Geurtsen W, Vargas M. Microleakage of porcelain veneer restorations bonded to enamel and dentin with a new self-adhesive resin-based dental cement. Dental Materials 2007; 23: 218-225. [ Links ]











 texto en
texto en 


