Introduction
Guillain-Barre syndrome (GBS) is an acute- onset polyradiculoneuropathy and the most common cause of acute flaccid paralysis. It is characterized by the appearance of sensory and/or motor symptoms, accompanied by decreased or absent muscle stretch reflexes and other symptoms such as facial paralysis, alteration of ocular movements, bulbar symptoms, alteration of the awake state, dysautonomia, and ataxia1. The incidence of GBS varies between population studies. In Europe and North America an incidence of 0.81-1.91 cases/100,000 people/year (median 1.11) is estimated2. However, the incidence is subject to the prevalence and outbreaks of infectious agents such as Campylobacter jejuni3. GBS has a mortality of between 3-7% described worldwide; in Mexico it is 0.16/100,000 people/year, associated with age over 50 years, need for mechanical ventilation, bulbar weakness, the severity of weakness on admission, time to maximum disability (walk), and hyponatremia4.
Hydroelectrolytic disorders are frequently associated with severe neurological diseases as a factor of poor prognosis, the most frequently affected electrolyte is sodium. In fact, hyponatremia is the most common disorder in hospitalized patients regardless of the cause of hospitalization, in GBS on admission, it is a frequent finding. A frequency of hyponatremia is 21.5-48% in hospitalized patients, being one of the poor prognostic factors, is related to alcohol abuse, anemia, hypertension, coagulopathy, concomitant malignancy, use of diuretics, or history of diarrhea5. However, hyponatremia is not a factor that it is presumed that the patient has before the onset of the disease. Rather, it is a direct complication due to different pathophysiological mechanisms, such as the syndrome of inappropriate secretion of antidiuretic hormone (SIADH)6.
Hyponatremia can become severe, and the most common treatment is fluid restriction. However, there are some datasets with published experience of tolvaptan as a treatment with controversial results7. In addition, few studies have described the characteristics of patients who have hyponatremia and its relationship with other factors or the spectrum of the GBS disease. Our study describes the clinical and electrophysiological characteristics of GBS patients with hyponatremia
Methods
In this observational, cross-sectional, comparative, and analytical study, through an ambispective cohort (January 1, 2018, to December 2021) of patients diagnosed with Guillain-Barre syndrome by Ausbury criteria were analyzed. We included all patients who had complete laboratory tests at the time of hospital admission. We excluded patients with a history of treatment with diuretics, carbamazepine or oxcarbazepine; equally, patients diagnosed with thyroid disease, adrenal insufficiency, acute kidney injury, or hyperglycemia > 200 mg/dL were excluded from the study. Patients with serum sodium levels < 135 meq/L on admission and before initiation of treatment (plasma exchanges or human immunoglobulin) were classified as hyponatremia. We obtained clinical information from the patients included: age, gender, history of previous infections, assessment of muscle strength through the Medical Research Council scale at diagnosis, GBS disability scale (at the time of diagnosis), cranial nerve involvement, presence of dysautonomia (defined as the presence of variation in blood pressure or heart rate, not explained by another medical condition such as fever, sepsis or medications, at the decision of the attending physician) on admission, the requirement for invasive mechanical ventilation (IMV), and days of hospital stay. We collected the results of cerebrospinal fluid (CSF) cytochemistry, obtaining protein levels (mg/dL) and cell count, dissociated LP was considered when presenting protein levels > 45 mg/dL with cells < 5 per field. The results of the nerve conduction studies were collected to obtain the distal compound muscle action potential (distal CMAP, millivolts mV), distal latency (milliseconds ms), and conduction velocity (m/s) of the median, ulnar, peroneal, and tibial motor nerves; Hadden's criteria were applied to classify patients into electrophysiological variants.
Ethical agreement
This study was evaluated and accepted by the local research and ethics committees of our institution.
Statistical analysis
For the distribution of continuous variables, we used the Kolmogorov-Smirnov test, and the variables were described in means (SD) or medians (IQR) according to their distribution. Categorical variables were described in frequencies and percentages. We performed a correlation analysis with the Person and Spearman test. To search for differences between groups (hyponatremia vs. no-hyponatremia), the X2 or Fisher's exact test was used for categorical variables; Student's T-test to compare means, and Mann-Whitney U-test to compare medians. A p < 0.05 was considered statistically significant. All statistical analyzes were performed using the IBM SPSS Statistics version 22.0 statistical package system.
Results
A sample of 212 patients was obtained with 152 male and 60 female subjects, mean age 45.9 ± 16 years, 39.6% of the patients had a history of diarrhea, onset of symptoms on admission (median) 5 (RIQ 3-8) days, Hughes scale at admission (median) 4 (RIQ 3-4) points, mEGOS scale at admission (median) 6 (RIQ4-7) points, mechanical ventilation requirement 32%, and cardiovascular dysautonomia 32%. The most frequent clinical variant was sensorimotor 60.4%. We had 165 CSF cytochemical studies with protein levels (median) 43 (RIQ 29-77) mgs/dL, and we had 182 nerve conduction studies, the most frequent electrophysiological variant was acute inflammatory demyelinating polyneuropathy (AIDP) 46%. The rest of the clinical and paraclinical characteristics are summarized in table 1.
Table 1 Clinical and electrophysiological characteristics of patients with Guillain-Barre syndrome
| Clinical and paraclinical variables | n = 212 |
|---|---|
| Age, mean (SD) | 45.9 ± 16 |
| Gender (male), n (%) | 152 (72) |
| Previous diarrhea, n (%) | 84 (39.6) |
| Previous respiratory tract infection, n (%) | 43 (20.3) |
| Onset of symptoms at admission (days), median (IQR) | 5 (3-8) |
| Hughes at admission (score), median (IQR) | 4 (3-4) |
| EGRIS scale, (score), median (IQR) | 4 (3-5) |
| EGOSm scale, (score), median (IQR) | 6 (4-7) |
| MRC score (points), mean (SD) | 30.1 ± 17 |
| IMV requirement, n (%) | 65 (32) |
| Cranial nerve involvement, n (%) | |
| Facial weakness | 129 (60.8) |
| Unilateral, n (%) | 21 (10) |
| Bilateral, n (%) | 78 (36.8) |
| Bulbar nerves (%) | 83 (39.2) |
| Cardiovascular dysautonomia, n (%) | 68 (32.1) |
| Clinical variants | |
| Sensory-motor, n (%) | 128 (60.4) |
| Pure-motor, n (%) | 62 (29.2) |
| Miller-Fisher syndrome/Overlap GBS, n (%) | 15 (7.1) |
| Pharyngeal-cervical-brachial, n (%) | 3 (1.4) |
| Protein/cytological dissociation, n (%) | 80/165 (48.5) |
| Protein levels in CSF (mg/dL), median (IQR) | 43 (29-77) |
| Electrophysiological variants | |
| AIDP, n (%) | 84/182 (46.2) |
| AMAN, n (%) | 62/182 (34) |
| AMSAN, n (%) | 7/182 (3.8) |
| Unexcitable, n (%) | 15/182 (8.2) |
| Equivocal, n (%) | 10 (10.6) |
| Treatment: | |
| Intravenous immunoglobulin, n (%) | 140 (66) |
| Plasma exchange, n (%) | 46 (21.7) |
| Observation, n (%) | 13 (13.8) |
| Days of hospital stay, median (IQR) | 8 (5-21) |
| Hughes ≤ 2-3 months of follow-up, n (%) | 67/162 (41.4) |
AIDP: acute inflammatory demyelinating polyneuropathy; AMAN: acute motor axonal neuropathy; AMSAN: acute motor sensory axonal neuropathy; CSF: cerebrospinal fluid; IQR: interquartile range; IVM: invasive mechanical ventilation; SD: standard deviation.
Thirty-one patients (14.6%) were classified with hyponatremia with serum sodium (mean) 130 ± 4.0 (min-max 106-134) meq/L, patients classified as non-hyponatremia had serum sodium (mean) 138 ± 2.0 (min-max = 135-146) meq/L.
In the comparative analysis between the patients with hyponatremia versus no-hyponatremia, we observed significant differences in: age (50.4 ± 14.9 vs. 43.8 ± 16.3, p = 0.03), days of hospitalization (median) (16 [IQR = 7-51] vs. 7 [IQR = 5-12] p = 0.03), dysautonomia (54.8% vs. 28.2%, p = 0.006), levels of proteins (mg/dL) in CSF (median) (105 [IQR = 59-165] vs. 39 [IQR = 28-57], p ≤ 0.001) and AIDP variant (70.4% vs. 42%, p = 0.011); in the recovery of independent gait at 3 months, there was no significant difference (34.6% vs. 42.6%, p = 0.51) (Table 2).
Table 2 Differences between patient groups with Guillain-Barre syndrome with and without hyponatremia
| Clinical and paraclinical variables | Hyponatremia (n = 31) | No-hyponatremia (n = 181) | p value |
|---|---|---|---|
| Age, mean (SD) | 50.4 ± 14.9 | 43.8 ± 16.3 | 0.03 |
| Gender (male), n (%) | 20 (64.5) | 132 (73) | 0.38 |
| Onset of symptoms at admission (days), median (IQR) | 7 (5-10) | 5 (3-7) | 0.86 |
| Days of hospital stay, median (IQR) | 16 (7-51) | 7 (5-12) | 0.003 |
| Previous diarrhea, n (%) | 9 (29) | 75 (41.4) | 0.23 |
| MRC score (points), mean (SD) | 25.3 ± 11.5 | 31.0 ± 7.7 | 0.09 |
| Hughes ≥ 3 at admission, n (%) | 31 (100) | 148 (81.7) | 0.006 |
| EGRIS scale (points), median (IQR) | 4 (3-5) | 4 (2-5) | 0.54 |
| EGOSm scale (points), median (IQR) | 6 (5-7) | 6 (3-7) | 0.03 |
| IMV requirement, n (%) | 13 (42) | 52 (28.7) | 0.14 |
| Cranial nerve involvement, n (%) | 23 (74) | 106 (58.5) | 0.1 |
| Facial weakness bilateral, n (%) | 16 (51.6) | 62 (34.2) | 0.07 |
| Bulbar, n (%) | 15 (48.4) | 68 (37.5) | 0.32 |
| Cardiovascular dysautonomia, n (%) | 17 (54.8) | 51 (28.2) | 0.006 |
| Clinical variants | |||
| Sensory-motor, n (%) | 23 (74) | 105 (58) | 0.11 |
| Pure-motor, n (%) | 7 (22.5) | 55 (30.3) | 0.52 |
| Miller-Fisher syndrome/Overlap GBS, n (%) | 1 (3.2) | 15 (8.3) | 0.13 |
| Protein levels in CSF (mg/dl), median (IQR) | 105 (59-165) | 39 (28-57) | < 0.001 |
| Variantes electrofisiológicas | |||
| AIDP, n (%) | 19/27 (70.4) | 65/155 (42) | 0.011 |
| AMAN, n (%) | 6/27 (22.2) | 56/155 (36) | 0.19 |
| AMSAN, n (%) | 1/27 (3.7) | 6/155 (3.9) | 0.99 |
| Unexcitable, n (%) | 1/27 (3.7) | 14/155 (9) | 0.70 |
| Equivocal, n (%) | 0/27 (0) | 14/155 (9) | 0.23 |
| Independent walking at 3 months, n (%) | 9/26 (34.6) | 58/136 (42.6) | 0.51 |
AIDP: acute inflammatory demyelinating polyneuropathy; AMAN: acute motor axonal neuropathy; AMSAN: acute motor sensory axonal neuropathy; CSF: cerebrospinal fluid; IQR: interquartile range; IVM: invasive mechanical ventilation; SD: standard deviation.
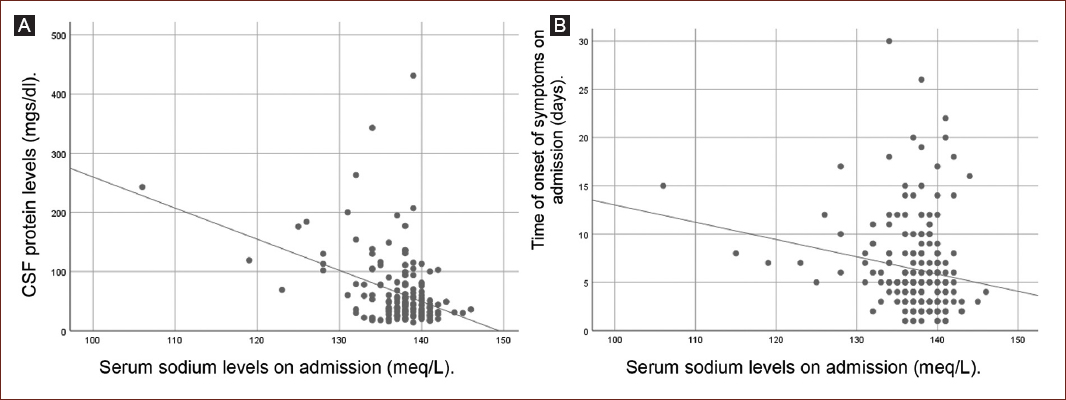
In the correlation analysis between serum sodium levels and clinical and paraclinical variables, we observed significant weak correlations with onset of symptoms on admission (days) and protein levels (mg/dL) in CSF, (Table 3 and Fig. 1).
Table 3 Correlation between serum sodium levels with clinical and paraclinical variables
| Variable | Correlation (r) | p valor |
|---|---|---|
| Age years | −0.07** | 0.31 |
| Onset of symptoms on hospital admission (days) | −0.19* | 0.006 |
| Hospital stay (days) | −0.089* | 0.22 |
| Hughes scale at admission (points) | −0.14* | 0.036 |
| MRC score at income (points) | −0.01† | 0.78 |
| mEGOS scale (points) | −0.13* | 0.050 |
| CSF protein levels | −0.31* | < 0.001 |
*spearman correlation;
†person correlation
Discussion
In this cohort, we found that 14.6% of the patients presented hyponatremia, similar other studies8. Hyponatremia is the most frequent hydroelectrolyte alteration in hospitalized patients, its etiology is multifactorial (drugs, renal, and cardiovascular alterations). In patients with GBS the pathophysiology of hyponatremia is due to different causes. One of the causes is pseudohyponatremia that occurs in some patients after intravenous infusion of human immunoglobulin9. In the case of our population, the determination of serum sodium was prior to the start of treatment.
The causes of hyponatremia in GBS have been classically described in SIADH. One of the mechanisms suggested in pathophysiology, is direct damage to hypothalamic cells, causing leakage of antidiuretic hormone (ADH) into systemic circulation. Another proposed explanation is the restoration of osmoreceptors in the hypothalamus. The most accepted mechanism is the participation of interleukin 6 was found to activate the subfornical organ and organum vasculosum in the terminal lamina, stimulating thirst and increasing vasopressin release10. One of the limitations of our study, we did not have a study of urinary electrolytes to diagnose SIADH.
Another hypothesis on hyponatremia in patients with GBS, it may be secondary to renal loss, by having an inadequate secretion of brain natriuretic peptide (BNP) after sympathoadrenal dysregulation secondary to the presence of cardiovascular dysautonomia11. The presence of hyponatremia is more frequent in patients with dysautonomia. In a cohort of 2587 patients with GBS, < 20% had dysautonomia, 14.9% present hyponatremia, SIADH 4.8% and 0.4% presented with brain salt wasting syndrome12. In our population, the presence of dysautonomia was more frequent in the hyponatremia group.
The electrophysiological variant AIDP is associated with a higher frequency of dysautonomia and increased protein in CSF, due to the great involvement of the nerve roots. When exist involvement of the cervical and thoracic roots, the roots of the paraganglionic chains of the sympathetic autonomic system are affected1. Interestingly, in our study, we observed that the population that presented hyponatremia presents more dysautonomia and AIDP variant, in addition to a greater number of proteins in CSF. Based on these observations, we hypothesize that the hyponatremia that occurs in GBS is due to cardiovascular dysautonomia, theoretically, causing cardiac alterations that cause release of atrial natriuretic peptide, which facilitates the loss of sodium at the renal level. However, this hypothesis should be taken with reservation due to the limitations of the study, requiring a prospective study measuring cardiac changes by echocardiography, measuring levels of atrial natriuretic peptide and serum electrolytes.
Hyponatremia has been studied as a factor of poor prognosis in GBS in multiple retrospective cohorts, the largest reported was by the Fondazione Ca' Granda Ospedale Policlinico di Milano Hospital study group, demonstrating the significant and independent association of hyponatremia with severe residual disability in patients13. Other studies have demonstrated the association of hyponatremia with severe clinical features in patients with GBS, such as lower MRC score, IMV requirement, prolonged hospital stays14,15. In our study, we observed that patients with GBS and hyponatremia presented clinical characteristics of severity, such as: higher score on the Hughes scale, increased hospital stay and presence of cardiovascular dysautonomia, similar other studies14,15.
Hyponatremia occurs more frequently in advanced ages and represents greater morbidity and mortality in the general population, in GBS it is not the exception. In a prospective study of GBS, an incidence of hyponatremia of 31% was detected, patients with SIADH and aged over 50 years had a more severe spectrum (longer days of hospitalization, mortality, admission to the ICU, and loss of gait)15. In our population, we did not observe differences in mean age between groups; however, we observed that patients with hyponatremia had a higher score on the mEGOS prognostic scale on admission, though there was no significant difference in the recovery of independent gait at 3 months of follow-up. We think this was because we did not have a score on the mEGOS scale 7 days after admission.
Another important point is the time of onset of hyponatremia; currently, the relationship between SIADH and GBS has been described with a median time to onset of 8.8 days, being independent treatment with immunoglobulin, which is well known to cause pseudohyponatremia16. There have been case reports of patients presenting with encephalopathy secondary to hyponatremia who, at the time of review, found GBS or the onset of SIADH symptoms with subsequent development of GBS17,18. Our previously published data involving patients with very early GBS (< 4 days of evolution) found a higher prevalence of hyponatremia (37%) without a higher prevalence of dysautonomia, being approximately double what was found in the current study and persisting when compared with other international cohorts19.
Finally, patients with hyponatremia present in the setting of neuroimmunology are frequently associated with other diseases such as autoimmune encephalitis associated with antibodies against the complex voltage-gated potassium channel, optic neuromyelitis, and Schmidt's syndrome. These findings are associated with a poor prognosis due to inflammation of the hypothalamus, but mainly as an indicator of the severity of body homeostasis and being independent of the disease. Due to this, some study groups state that the patient with GBS and hyponatremia should be considered as having a marker or predictor of the course of the disease. This may yield interesting results to determine need for ICU, discharge planning, and follow-up20,21. The patient with a history of hyponatremia due to systemic or neurological disease is more likely to have hyponatremia after the onset of GBS, since a small trigger may be enough to develop a new autonomic dysfunction even after a long time and lead to a worse prognosis in their next illness22.











 text new page (beta)
text new page (beta)