Establishing sound cancer control plans is necessary to overcome the growing cancer burden; within them, population-based cancer registries (PBCR) play an essential role in the planning and evaluation of the activities.1,2Accordingly, incidence by type of cancer has been established as a key indicator in the Monitoring Framework on Non-Communicable Diseases of the World Health Organization (WHO),3 and its collected information has been reaffirmed at the more recent 70th World Health Assembly.4 Despite PBCR being the only means to obtain cancer incidence and survival at the population level, there are enormous disparities in their coverage and quality among regions of the world.2,5 In Latin America, the PBCR included in the last volume (XI) of the serial publication Cancer Incidence in Five Continents represents less than 10% of the population.6
Mexico, the second most populated country in Latin America, has made various attempts to establish cancer registries. One of the first initiatives dates back to 1975, when the Jalisco State Cancer Registry was initiated; nevertheless, until very recent developments and changes, it has been mainly a pathology-based registry.7 In 1982, the first attempt to establish a national cancer registry had an active participation of 34 hospitals of Mexico City, extending to the states of Jalisco and Nuevo León. This initiative was replaced in 1994, by the National Histopathological Cancer Registry, an effort that lasted only until 2001.8,9Additional developments worth mentioning have been the Pediatric Cancer Registry led by the XXI Century National Medical Center of the Mexican Institute for Social Security (Instituto Mexicano del Seguro Social, IMSS), which covers circa 65% of the Mexican population; this registry covers pediatric patients of various states affiliated to IMSS.10
More recently, under the leadership of the National Cancer Institute of Mexico (Incan), the country has advanced simultaneously in the establishment of a national cancer control plan and a network of subnational PBCRs that conform the so-called National Cancer Registry. The Senate of the country created the National Cancer Registry by a law that will be further regulated.11 Upon signature of an agreement with the Incan, the Global Initiative for Cancer Registry Development (GICR) led by the International Agency for Research on Cancer (IARC) has supported cancer registration during the last years, providing assistance to the PBCR of Mérida (in the state of Yucatán) and Jalisco, amongst others.12
Herein, we present a brief overview of key aspects of the establishment of the PBCR in Mérida and the preliminary results achieved so far for the years 2015-2016.
Materials and methods
The population covered by the registry is 908 536 inhabitants of the city of Mérida (figure 1).13 Mérida is the capital and most populated city of the state of Yucatán, in the Southeast of the country. It concentrates the oncological services in the state.
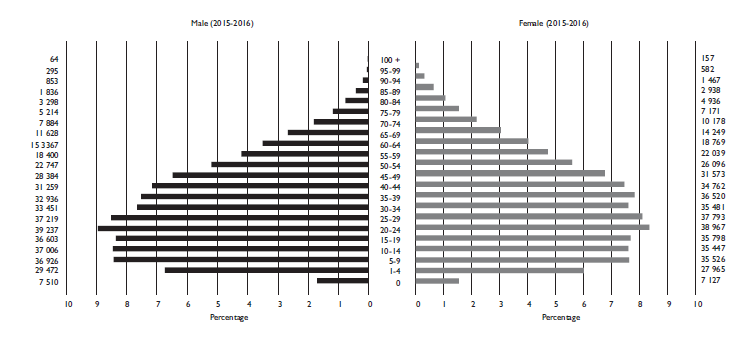
Source: National Institute of Statistic and Geography, State Government of Yucatán.13
Figura 1 Population pyramid. Mérida, Yucatán, Mexico, 2015-2016
Organization
The Mérida PBCR started in 2016 as a research project financed by the IMSS and the National Council for Science and Technology (Conacyt) after a short stay of the Cancer Registry Director at IARC. The project was approved by the National Research Commission-IMSS number R-2014-785-085. From the beginning, the office of the registry has been located at the IMSS’s high-specialty medical unit (UMAE)-IMSS hospital in Mérida.14
Information sources
For the inclusion of information sources, the sanitary census of the city of Mérida was reviewed, and establishments visited by cancer patients for diagnosis, treatment and follow-up were selected; each of theme was corroborated through a telephone call or a visit in situ, and was invited to collaborate with the Mérida-PBCR.
Table I presents the sources of information by type of source and year of inclusion. The expansion of data sources for the registry has been decidedly supported and facilitated by the Incan and the IMSS, with visits and advocacy to some of the institutions to be included, particularly during 2016 and 2017.
Table I Number of information sources included by year. Mérida, Yucatán, Mexico
| Source by type | Number of sources by year of inclusion | |||
| 2016 | 2017 | 2018 | Total | |
| High- specialized hospital | 2 | 1 | 0 | 3 |
| General hospital | 5 | 2 | 4 | 11 |
| Specialized oncology clinic | 0 | 1 | 0 | 1 |
| Chemotherapy clinic | 0 | 1 | 1 | 2 |
| Radiotherapy clinic | 0 | 0 | 1 | 1 |
| Specialized hospital | 0 | 1 | 1 | 2 |
| Alternative clinic | 0 | 0 | 1 | 1 |
| Pathology lab | 0 | 2 | 3 | 5 |
| Imaging detection clinic | 0 | 0 | 1 | 1 |
| Nuclear medicine lab | 0 | 1 | 2 | 3 |
| Oncologists and hematologists | 0 | 5 | 10 | 15 |
| Urologist | 0 | 2 | 10 | 12 |
| Neurologists and neurosurgeons | 0 | 2 | 9 | 11 |
| Pneumologists | 0 | 0 | 4 | 4 |
| Gastroenterologists and proctologists | 0 | 0 | 11 | 11 |
| Gynecologists and colposcopy | 0 | 0 | 6 | 6 |
| Administrative office | 0 | 1 | 1 | 2 |
| Total | 7 | 19 | 65 | 91 |
Case definition
The registry includes all new cancer cases diagnosed in residents of Mérida since January 1st, 2015; the date of diagnosis is applied as defined by the European Network of Cancer Registries (ENCR).15 The case definition includes, in addition to all malignant neoplasms, non-malignant tumors of the brain and the central nervous system. Residence is considered when the patient had been living there for more than six months and also had the official ID with a Mérida address to endorse it.
The bases for the cancer diagnosis include clinical tests, the presence of a specific tumor biomarker, cytology, histology of primary tumor or metastasis, and death certificate.16
Data collection
An ad hoc data collection format was designed as part of the project to collect the socio-demographic, tumor and source information as suggested by IARC.5 Data collection is both active and passive. Registrars (mainly nurses) actively visit the information sources to abstract the cancer cases from the clinical records. Some institutions provide consolidated databases, in which case the registrars review a subset of clinical records for diagnostic verification and complementary information if required. Cases of non-melanoma skin cancer are not actively sought.
Death certificates are obtained annually in electronic format from the Yucatán Ministry of Health Office. They include information regarding deaths certified in the state of Yucatán. All information is validated before being capture into the system with particular attention to the residence status in Mérida and the metropolitan area.
Processes and quality control
A Manual of procedures was written at the start of the registry and has been reviewed during the external site visits. Coding follows the International Classification of Diseases for Oncology (ICD-O-3).16 For data entry, quality checks and data analysis, the registry uses CanReg5, IARC’s free software, which facilitates identification of duplicates and of the use of non-existent codes, and also verifies internal consistency by applying standard validations..17 Main data quality indicators, e.g. the percentage of cases with microscopic verification (MV%) and percentage of cases notified by death certificate only (DCO%) are also obtained using the CanReg analysis.
The CanReg5 program was used to estimate the age-standardized incidence rates (ASR) per 100 000 inhabitants, using the direct method and the world standard population.18 All information is handled according to national confidentiality guidelines.19,20No legal framework for cancer registration was existent at the moment of initiation.
Training
During a short mentorship stay at IARC, the cancer registry director received training for setting up the PBCR; however, most of the registrars have received their training at the workplace. The team has attended several online training courses organized by the IARC Regional Hub for Latin America, and the registry director participated in a regional training course on data analysis for cancer registries.
External support
Through the GICR, two expert site visits to the Mérida PBCR took place during 2016 and 2017 respectively; visits were accompanied with specific recommendations and a particular emphasis to expand data sources. One site visit included in-depth support for CanReg5. Periodic communication between Incan, GICR and the registry director has taken place since inception.
Results
Implementation process
Data for 2015 and 2016 are presented, with collection closed in December 2018. Table I describes inclusion and access to public and private health care institutions. Briefly, at the beginning of 2016 we started on three sources of the IMSS -the high-specialty medical unit (UMAE) host of the registry and two general hospitals-; at the end of the first year of operation of the Mérida-PBCR, seven sources had been included (five public, non-IMSS, and two private); in 2017 we further incorporated 19 establishments (three public), and a larger number of sources was included in 2018. Table II shows the number of new cancer cases by (first) institution; in 2015-2016, 39.7% of the new cancer cases included were from the institution hosting the cancer registry.
Table II Number of new cancer cases, by first main source. Mérida Cancer Registry, Mexico (2015-2016)
| Source | Source by type | Health Sub-system | 2015 | 2016 | 2015-2016 | |||||||||||
| n | % | n | % | n | % | |||||||||||
| 1 | Highly specialized hospital 1 | IMSS | 437 | 42.3 | 604 | 38.0 | 1041 | 39.7 | ||||||||
| 2 | General hospital 1 | IMSS | 70 | 6.8 | 142 | 8.9 | 212 | 8.1 | ||||||||
| 3 | General hospital 2 | IMSS | 10 | 1.0 | 12 | 0.8 | 22 | 0.8 | ||||||||
| 4 | General hospital 3 | IMSS | 3 | 0.3 | 6 | 0.4 | 9 | 0.3 | ||||||||
| 5 | Specialized oncology clinic | Red Cross | 19 | 1.8 | 7 | 0.4 | 26 | 1.0 | ||||||||
| 6 | General hospital 4 | MoH | 27 | 2.6 | 84 | 5.3 | 111 | 4.2 | ||||||||
| 7 | Highly specialized hospital 2 | MoH | 1 | 0.1 | 3 | 0.2 | 4 | 0.2 | ||||||||
| 8 | Specialized clinic | MoH | 0 | 0.0 | 1 | 0.1 | 1 | 0.0 | ||||||||
| 9 | General hospital 5 | MoH | 79 | 7.7 | 123 | 7.7 | 202 | 7.7 | ||||||||
| 10 | General hospital 6 | ISSSTE | 55 | 5.3 | 86 | 5.4 | 141 | 5.4 | ||||||||
| 11 | Administrative office | MoH | 168 | 16.3 | 368 | 23.1 | 536 | 20.4 | ||||||||
| 12 | Alternative clinic | Private | 1 | 0.1 | 9 | 0.6 | 10 | 0.4 | ||||||||
| 13 | General hospital 7 | Private | 41 | 4.0 | 39 | 2.5 | 80 | 3.0 | ||||||||
| 14 | Pathology lab 1 | Private | 26 | 2.5 | 17 | 1.1 | 43 | 1.6 | ||||||||
| 15 | Pathology lab 2 | Private | 19 | 1.8 | 11 | 0.7 | 30 | 1.1 | ||||||||
| 16 | Specialized hospital 2 | Private | 1 | 0.1 | 0 | 0.00 | 1 | 0.0 | ||||||||
| 17 | Chemotherapy clinic | Private | 4 | 0.4 | 10 | 0.6 | 14 | 0.5 | ||||||||
| 18 | Pathology lab 3 | Private | 1 | 0.1 | 1 | 0.1 | 2 | 0.1 | ||||||||
| 19 | Pathology lab 4 | Private | 2 | 0.2 | 1 | 0.1 | 3 | 0.1 | ||||||||
| 20 | Pathology lab 5 | Private | 36 | 3.5 | 19 | 1.2 | 55 | 2.1 | ||||||||
| 21 | Urological clinic | Private | 3 | 0.3 | 2 | 0.1 | 5 | 0.2 | ||||||||
| 22 | Pathology lab 6 | Private | 0 | 0.0 | 2 | 0.1 | 2 | 0.1 | ||||||||
| 23 | Imaging detection clinic 1 | Private | 2 | 0.2 | 0 | 0.00 | 2 | 0.1 | ||||||||
| 24 | Imaging detection clinic 2 | Private | 2 | 0.2 | 22 | 1.4 | 24 | 0.9 | ||||||||
| 25 | General hospital 8 | Private | 24 | 2.3 | 12 | 0.8 | 36 | 1.4 | ||||||||
| 26 | Radiotherapy clinic | Private | 0 | 0.0 | 5 | 0.3 | 5 | 0.2 | ||||||||
| 27 | General hospital 9 | Private | 1 | 0.1 | 2 | 0.1 | 3 | 0.1 | ||||||||
| 28 | Imaging detection clinic 3 | Private | 0 | 0.0 | 1 | 0.1 | 1 | 0.0 | ||||||||
| 29 | Nuclear medicine lab 1 | Private | 0 | 0.0 | 2 | 0.1 | 2 | 0.1 | ||||||||
| Total | All | 1 032 | 100.0 | 1 591 | 100.0 | 2 623 | 100.0 | |||||||||
IMSS: Mexican Institute for Social Security (Instituto Mexicano del Seguro Social)
MoH: Ministry of Health
ISSSTE: Security and Social Services Institute for State Workers (Instituto de Seguridad y Servicios Sociales de los Trabajadores del Estado)
Preliminary results
During 2015-2016 a total of 2 623 new cancer cases (excluding non-melanoma skin cancer) were registered, the majority of which occurred in females (60.1%) (table III and IV). For both sexes combined, the number of new cancer cases in 2016 increased by 52% compared with 2015; this increase was stronger among females, amounting to 68% of the new cancer cases between the two years (information not shown). For 2015-2016 the cancer incidence rates (age-standardized per 100 000) for all cancers combined (except non-melanoma skin cancer) were 114.9 for males, and 145.1 for females.
Table III New cancer cases, incidence rates (ASR per 100 000) and quality indicators by cancer site, males. Mérida Cancer Registry, Mexico (2015-2016)
| Cancer site | Cases | Freq(%) | Crude Rate | ASR | MV (%) | DCO (%) | ICD10 | |||||||
| Mouth and pharynx | 20 | 1.9 | 2.3 | 2.1 | 80.0 | 10.0 | C00−14 | |||||||
| Esophagus | 21 | 2.0 | 2.4 | 2.2 | 85.7 | 14.3 | C15 | |||||||
| Stomach | 84 | 8.1 | 9.5 | 9.0 | 80.9 | 11.9 | C16 | |||||||
| Colon, rectum, anus | 89 | 8.5 | 10.1 | 9.5 | 88.8 | 5.6 | C18−21 | |||||||
| Liver | 75 | 7.2 | 8.5 | 8.3 | 54.7 | 38.7 | C22 | |||||||
| Pancreas | 22 | 2.1 | 2.5 | 2.5 | 59.1 | 22.7 | C25 | |||||||
| Larynx | 28 | 2.7 | 3.2 | 3.1 | 75.0 | 14.3 | C32 | |||||||
| Lung, trachea, bronchus | 54 | 5.2 | 6.1 | 5.8 | 68.5 | 20.3 | C33−34 | |||||||
| Pleura and other thoracic | 3 | 0.3 | 0.3 | 0.3 | 100.0 | 0.0 | C37−38 | |||||||
| Melanoma of skin | 10 | 1.0 | 1.1 | 1.1 | 70.0 | 30.0 | C43 | |||||||
| Prostate | 181 | 17.4 | 20.6 | 20.3 | 79.6 | 13.8 | C61 | |||||||
| Testis | 31 | 2.9 | 3.5 | 3.3 | 80.6 | 9.7 | C62 | |||||||
| Kidney and urinary NOS | 46 | 4.4 | 5.2 | 5.1 | 76.1 | 13.0 | C64−66,68 | |||||||
| Bladder | 35 | 3.4 | 3.9 | 3.9 | 85.7 | 8.6 | C67 | |||||||
| Brain and nervous system | 28 | 2.7 | 3.2 | 3.2 | 82.1 | 10.7 | C70−72 | |||||||
| Thyroid | 12 | 1.2 | 1.4 | 1.3 | 83.3 | 16.7 | C73 | |||||||
| Ill−defined | 53 | 5.1 | 5.8 | 5.8 | 67.9 | 28.3 | C76−80 | |||||||
| Other cancers | 112 | 10.7 | 12.3 | 10.8 | 86.6 | 6.3 | C17,23-24, 26, 31, 39-41,45-49,60, 63, 69,74-75, 86 | |||||||
| Lymphoma | 81 | 7.8 | 9.2 | 8.6 | 86.4 | 9.8 | C81−85,90,88,96 | |||||||
| Leukemia | 57 | 5.5 | 6.5 | 6.8 | 75.4 | 21.1 | C91−95 | |||||||
| All sites but C44 | 1 042 | 100 | 118.4 | 114.9 | 78.8 | 14.9 | ALLbC44 |
ASR: age standardized rate
MV: microscopic verification
DCO: death certificate only
ICD10: International Classification Diseases version 10
NOS: not otherwise specified
Among males, prostate cancer amounted to 17.4% of the new cancer cases, with an ASR of 20.3 per 100 000, followed by colorectal cancer (8.5%; ASR of 9.5 per 100 000) and stomach cancer (8.1%; ASR 9.0 per 100 000) (table III). Among females, breast cancer was the most commonly diagnosed cancer type, amounting to 31.6% of the new cancer cases, with an ASR per 100 000 of 45.1 per 100 000. It was followed by cervical cancer (12% and ASR of 17 per 100 000) and by corpus (7.6% and ASR of 11.2 per 100 000) (table IV). Childhood cancers (0-16) accounted for 106 cases representing 4% of all new cancer cases, the majority (54 cases) among boys (51%); the most affected age were infants 1-4 years old, with 39.6% of cases. Distribution according to the International Classification of Chilhood Cancer (ICCC) diagnostic groups21 showed that the majority were leukemias, myeloproliferative and myelodysplastic diseases, with 44 cases (41.5%); lymphomas and reticuloendothelial neoplasms, with 16 cases (15.1%), and malignant bone tumors, with 11 cases (10.4%).
Table IV New cancer cases, incidence rates (ASR per 100 000) and quality indicators by cancer site, females. Mérida Cancer Registry, Mexico (2015-2016)
| Cancer site | Cases | Freq(%) | Crude Rate | ASR | MV (%) | DCO (%) | ICD10 | |||||||
| Mouth & pharynx | 7 | 0.4 | 0.7 | 0.6 | 100.0 | 0.0 | C00−14 | |||||||
| Esophagus | 9 | 0.6 | 1.0 | 0.8 | 77.8 | 11.1 | C15 | |||||||
| Stomach | 63 | 4.0 | 6.7 | 5.6 | 76.2 | 15.9 | C16 | |||||||
| Colon, rectum, anus | 74 | 4.7 | 7.9 | 6.4 | 93.2 | 6.8 | C18−21 | |||||||
| Liver | 52 | 3.3 | 5.5 | 4.5 | 59.6 | 28.9 | C22 | |||||||
| Pancreas | 21 | 1.3 | 2.2 | 1.8 | 57.1 | 28.6 | C25 | |||||||
| Larynx | 8 | 0.5 | 0.9 | 0.8 | 87.5 | 12.5 | C32 | |||||||
| Lung, trachea, bronchus | 29 | 1.8 | 3.1 | 2.7 | 65.5 | 20.7 | C33−34 | |||||||
| Pleura and other thoracic | 7 | 0.4 | 0.8 | 0.5 | 85.7 | 14.3 | C37−38 | |||||||
| Melanoma of skin | 14 | 1.0 | 1.5 | 1.2 | 100.0 | 0.0 | C43 | |||||||
| Breast | 499 | 31.6 | 53.3 | 45.1 | 88.0 | 5.0 | C50 | |||||||
| Cervix | 188 | 12.0 | 20.1 | 17.0 | 87.2 | 9.0 | C53 | |||||||
| Corpus and uterus NOS | 120 | 7.6 | 12.8 | 11.2 | 87.5 | 4.2 | C54−55 | |||||||
| Ovary and adnexa | 78 | 4.9 | 8.3 | 7.2 | 79.5 | 11.5 | C56 | |||||||
| Kidney and urinary NOS | 39 | 2.5 | 4.2 | 3.7 | 76.9 | 15.4 | C64−66,68 | |||||||
| Bladder | 19 | 1.2 | 2.0 | 1.7 | 89.5 | 5.3 | C67 | |||||||
| Brain and nervous system | 16 | 1.0 | 1.7 | 1.8 | 75.0 | 18.8 | C70−72 | |||||||
| Thyroid | 55 | 3.5 | 5.9 | 5.0 | 92.7 | 5.5 | C73 | |||||||
| Ill−defined | 59 | 3.7 | 6.5 | 5.4 | 71.2 | 27.1 | C76−80 | |||||||
| Other Cancers | 113 | 7.2 | 12.4 | 7.2 | 81.4 | 12.4 | C17,23-24,30-31,40-41,45, C48-49,51-52,57, C6, 74-75 | |||||||
| Lymphoma | 69 | 4.4 | 6.4 | 6.9 | 91.3 | 7.3 | C81−85,90,88,96 | |||||||
| Leukemia | 42 | 2.6 | 4.5 | 4.8 | 73.8 | 23.8 | C91−95 | |||||||
| All sites but C44 | 1 581 | 100 | 168.8 | 145.1 | 84.1 | 10.1 | ALLbC44 |
ASR: age standardized rate
MV: microscopic verification
DCO: death certificate only
ICD10: International Classification Diseases version 10
NOS: not otherwise specified
Regarding indices of data quality, 78.8% of the cases among males and 84.1% among females were microscopically verified; 14.9% and 10.1% of the cases among males and females respectively, were diagnosed by death certificate only.
Discussion
This is the very first report of a recently established Mexican population-based cancer registry, and its results need to be interpreted with caution, as the registry still needs to consolidate. Nevertheless, it allows to highlight some important factors in both the operation and the preliminary results that provide useful orientation for the development of PBCR that Mexico is undergoing.
It is not usual or recommended to start a PBCR as a research project, yet this has been reported also for a Colombian registry.22Although this may be an interesting option for starting operations and providing some stability at the beginning of a registry, it calls for great caution, as its sustainability is not guaranteed. The implementation process of the Mérida PBCR may be interpreted as a hospital-based registry (HBCR) that subsequently became a PBCR. Nevertheless, we wish to stress that the aim was always to establish a PBCR with a very limited number of variables that would hardly comply with those required for an HBCR; we do not recommend starting an HBCR in order to convert it to a PBCR.5 In case of the Mérida PBCR, the initial data collection at the hospital hosting the registry facilitated capacity building and acquisition of specific skills, such as case abstraction and coding, among registrars. Starting the registration at the UMAE Mérida has favored the capture of significant number of cases, as the IMSS is the largest provider of medical care in Mexico.14 The fact that, at the start of the Mérida PBCR, no legal framework existed to support cancer registration in the country, along with the lack of experience of the operation of this type of cancer registry, delayed the inclusion of other institutions as data sources, particularly those not pertaining to the IMSS’ health system (where the registry started). As mentioned above, the launching of the Mérida PBCR required important efforts by the registry director, as well as support from both local and national institutions like Incan, the Ministry of Health of Yucatán, and the IMSS.
Despite the difficulties and associated efforts to expand data collection to new information sources, it must nevertheless be recognized that in this case the most important sources in terms of the number of cases were included already from the start. The high proportion of cases from the institution that hosted the registry is consistent with its level of high specialization, given that it is the sole institution of its kind in the city, and with the 60% coverage of Mexican population by the IMSS.14
The Mérida PBCR has met the international standards since its inception; the quality data indicators obtained so far are comparable with those of many of the neighboring countries.6Data analysis and consistency checks have been greatly facilitated by the use of CanReg5.
The involvement of the Incan and of the GICR, via a formal agreement, in an early phase of the implementation of the registry has strengthened commitment, collaboration, and periodic communication. Partnerships are key to support different aspects of cancer control programs and cancer surveillance; concrete examples of partnership involvement in cancer registration in the region have been highlighted before.23,24,25In addition, mentoring and tailored support -critical components of the GICR (http://gicr.iarc.fr/en/)- are crucial ingredients for success in knowledge transfer.12
Cancer incidence results for Mérida during this period need to be taken with extreme caution and must be validated once full coverage of the PBCR has been achieved and the registry operations have become stabilized. The cancer incidence rates (per 100 000) observed in Mérida during 2015-2016 for all cancers combined among females (ASR of 145.1) are similar to the estimated rates for Mexico in Globocan 2018 (ASR 149.6); among males, they were much lower (ASR 114.9 versus 136.5) compared to estimates Globocan 2018 (ASR per 100 000). Nevertheless, the distribution of the most common cancers (prostate, breast and cervix) and the overall quality indices are consistent with local and regional reports.6,26
Furthermore, findings like the sex disparity -with 66% of cases occurring in females, in whom mouth, pharynx and melanoma skin cancers were all microscopically verified- clearly indicate limitations in coverage. Although these limitations are being tackled with the current inclusion of 91 information sources in the registry, there is a need to evaluate whether case findings include radiology departments with tomography.
The high percentage of pediatric cancers (4%) among the male population probably also reflects underregistration among males of all ages. Notably, the percentage of lymphomas in children (15.1%) has been also documented by Fajardo-Gutierrez and colleagues for the Yucatán state and deserves further investigation.27 The most frequent pediatric cancer, as expected, was acute leukemia, which in Mexico can be diagnosed at an early stage and therefore can have better opportunities for survival.28,29
Conclusion
Beyond the described limitations, the present report provides an important input to guide the establishment of the cancer registry network that is currently underway in Mexico. At the same time, advances have motivated the approval of the Cancer Registry Law by the Congress in 2017, which will provide an unprecedented support for the registry network. We underscore the importance of commencing directly as a PBCR supported by the current Mexican legal framework and securing a budgetary line. While results need to be interpreted with extreme caution, this first report clearly highlights the efforts made to achieve sustainability, coverage, and quality within international standards. Continuous collaboration of local health care providers, local and national authorities, and international partners should allow attainment of these objectives in the near future.











 nueva página del texto (beta)
nueva página del texto (beta)


