INTRODUCTION
Since the beginning of the SARS-CoV-2 pandemic, several factors associated with severe disease and COVID-19 related mortality have been described. The impact of increasing age, type 2 diabetes mellitus, cardiovascular diseases, immunosuppression, chronic lung diseases, malignancy, chronic kidney disease, chronic liver disease, and among other comorbidities, has been widely described in numerous reports1-10.
In young, non-comorbid (non-obese, diabetic, or hypertensive) adults, the need for invasive mechanical ventilation (IMV) has been reported in 6%11. Even though up to 3.6% of all COVID-19 deaths occur in patients younger than 65 years with no comorbidities, in Mexico, this may be as high as 17.7%12. Although prognostic factors in younger and otherwise healthy patients have been proposed13-17, there is still a lack of information regarding prognostic factors in this population. In this prospective cohort study, we aimed to identify factors associated with in-hospital death or need for IMV in young and otherwise healthy patients hospitalized with COVID-19.
METHODS
Patients and settings
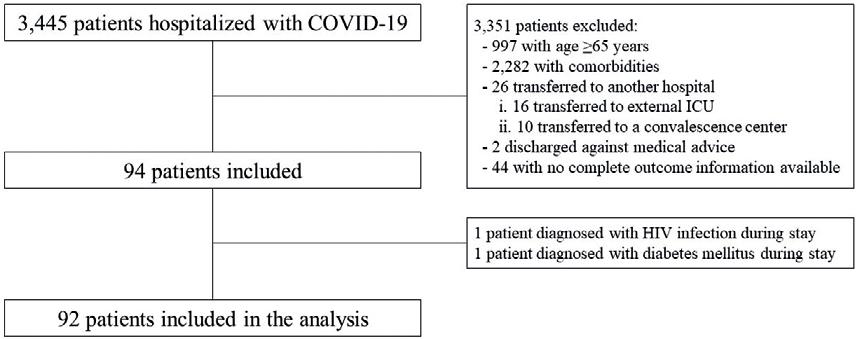
We conducted a prospective cohort study in a COVID-19 reference center in Mexico City. We included all adult patients admitted with a positive SARS-CoV-2 real-time polymerase chain reaction (RT-PCR) between March 15, 2020, and September 30, 2021. We excluded patients aged 65 or older and those with previous underlying comorbidities or who were diagnosed with a chronic illness during stay, transferred to other facilities before discharge or discharged against medical advice, or whose records had incomplete information regarding the outcomes. Data were prospectively collected using the electronic medical record. Patients were followed-up from admission to death or discharge. The composite primary outcome was in-hospital death or the need for IMV. Secondary outcomes included the need for IMV during follow-up, days on IMV, length of stay (LOS), development of hospital-acquired pneumonia/ventilator-associated pneumonia (HAP/VAP) as defined by accepted criteria18, and pulmonary embolism (PE).
For study purposes, a case was considered mild/moderate when no or mild pneumonia was present; severe when pulse oximetry (SpO2) was < 93%, PaO2/FiO2 ratio < 300, respiratory rate ≥ 30 breaths per minute, or ≥ 50% lung involvement was seen in chest CT; and critical when either shock, need for IMV, or multi-organ failure were present19. In addition, risk for disease progression was evaluated using the Nutri-CoV score20. Laboratory parameters, including SARS-CoV-2 RT-PCR cycle threshold (Ct) values, were reported using cutoff values that have been associated with COVID-19 outcomes21,22. Data regarding the Nutri-CoV score and Ct value were retrospectively collected.
Our study represents a sub study of our institution's prospective cohort study, which was approved by the Institutional Review Board (Reference 3333). Because of the observational nature of the study, written informed consent was waived.
Statistical analysis
A non-probabilistic, consecutive sampling of all admitted patients was implemented. Because widespread data were not yet available at the beginning of the study (March 2020), no prespecified sample size was calculated. As the study progressed, a sample size was calculated. Considering a primary outcome frequency of up to 6% in younger patients without comorbidities11, we estimated a sample of at least 76 patients to find up to 3 prognosis predictors with a mean absolute prediction error of 5%23. Data were described using mean and standard deviation or median and interquartile range (IQR) according to Shapiro-Wilk normality test. Relative risk (RR) and 95% confidence interval (95%CI) for primary outcome were calculated. Finally, a multivariate analysis using a multiple logistic regression model was done to identify factors independently associated with the primary outcome. The model included variables of clinical significance with a p < 0.2 in bivariate analysis. Adjusted odds ratio (aOR) and 95% CI were estimated. Because pulse oximetry was included in the model, severity on admission (which uses pulse oximetry data for assessment) was not included in the logistic regression model. Because age was also included in the model, the Nutri-CoV score (which uses age and pulse oximetry data for assessment) was not included in the logistic regression model. Since tocilizumab prescription was not standardized at any point during the study period and may be susceptible to selection bias24, it was not included in the logistic regression model. Because steroids are known to reduce COVID-19 associated mortality25, the variable was included in the logistic regression model. Two-sided p < 0.05 was considered statistically significant. Missing data were not replaced. The analysis was performed using STATA version 15.1 (Texas, USA).
RESULTS
During the study period, 92 hospitalized patients were included (Fig. 1). The primary outcome occurred in 16/92 (17%) patients. The need for IMV occurred in 16/92 (17%) and death in 12/92 (13%). The 12 patients who died also required IMV. Median LOS in the entire cohort were 6.5 days (IQR 4-9.5). Total follow-up time across the cohort was 911 days. In survivors, LOS and IMV duration was 7 and 12 days, respectively. HAP/VAP occurred in 7/92 (8%) and PE in 2/92 (2%). The majority were men (53/92 [58%]) and the median age was 50 years (range 25-64). The median time from symptom onset to admission was 9 days (IQR 5-11). On admission, 3 (3%), 86 (93%), and 3 (3%) patients were considered as moderate, severe, and critical cases, respectively. Low RT-PCR cycle threshold (Ct ≤ 24) values were reported in 26/86 (30%). The median time from symptom onset to admission did not influence the RT-PCR CT value (median time of 8 days [IQR 5-10] in the Ct ≤ 24 group vs. 9 days in the Ct > 24 group [IQR 7-12], p = 0.15). None of the patients included were yet vaccinated. Steroids were prescribed in 57 (62%), and 3 (3%) were placed on IMV on admission. No patients received remdesivir as part of their standard of care. By the end of June 2020, 36 (39%) patients had been included and by the end of December 2020, 69 (75%) patients had been included.
In the bivariate analysis, increasing Nutri-CoV score (RR 1.54, 95%CI 1.23-1.91, p < 0.01), lower RT-PCR Ct values (RR 2.6, 95%CI 1.1-6.5, p < 0.05) (Fig. 2), and higher D-dimer levels (RR 4.7, 95%CI 1.9-11.7, p < 0.01) were associated with the primary outcome. In multivariate analysis, male sex (aOR 7.1, 95%CI 1.1-46.0, p < 0.05), D-dimer levels > 1000 ng/mL (aOR 9.0, 95%CI 1.6-49.1, p < 0.05) and RT-PCR Ct values ≤ 24 (aOR 14.3, 95%CI 2.0-101.5, p < 0.01) were independently associated with the primary outcome. Results are summarized in Table 124,25.
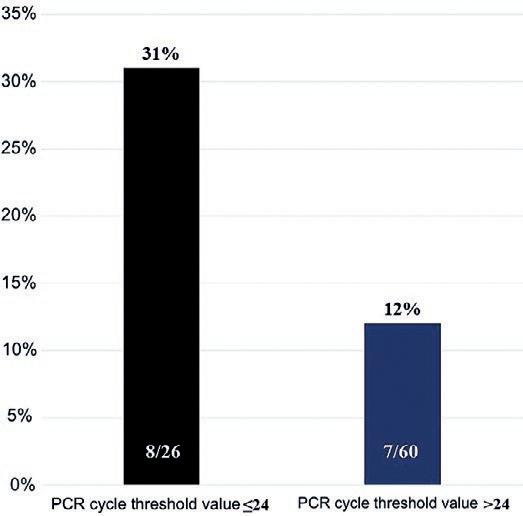
Figure 2. Primary outcome occurrence according to PCR threshold values. Relative risk for primary outcome 2.6 (95%CI 1.1-6.5), p = 0.0320.
Table 1. Results
| Characteristic | All patients (n = 92) (100%) | Presented the primary outcome (n = 16) (17%) | Did not present the primary outcome (n = 76) (83) | Bivariate analysis RR (95%CI), (p) | Multivariate analysis* aOR (95%CI), (p) |
|---|---|---|---|---|---|
| Male sex- n (%) | 53 (58) | 12 (75) | 41 (54) | 2.2 (0.8-6.3), 0.121 | 7.1 (1.1-46.0), 0.041 |
| Age, years – median (IQR) | 50 (40-56) | 53 (43-58) | 50 (38-55) | 1.0 (1.0-1.1), 0.182 | 1.1 (1.0-1.2), 0.077 |
| Age 18-25 years, n (%) | 1 (1) | 0 | 1 (1) | ||
| Age 26-35 years, n (%) | 14 (15) | 1 (6) | 13 (17) | ||
| Age 36-45 years, n (%) | 19 (21) | 4 (25) | 15 (20) | ||
| Age 46-55 years, n (%) | 34 (37) | 5 (31) | 29 (38) | ||
| Age 56-64 years, n (%) | 24 (26) | 6 (38) | 18 (24) | ||
| Body mass index, kg/m2 – median (IQR) | 23.8 (21.1-24.9) | 23.4 (22.9-24.4) | 24.0 (23.3-24.5) | 0.8 (0.6-1.2), 0.241 | |
| Pulse Oximetry < 90% – n (%) | 71 (77) | 15 (94) | 56 (74) | 4.4 (0.62-31.6), 0.0822 | 2.3 (0.2-30.9), 0.541 |
| Nutri-CoV score – median (IQR) | 7 (4-11) | 11 (10-14) | 5 (4-8) | 1.5 (1.2-1.9), < 0.001 | |
| Low Risk, n (%) | 18 (20) | 0 | 18 (24) | ||
| Moderate Risk, n (%) | 28 (30) | 1 (6) | 27 (36) | ||
| High Risk, n (%) | 31 (34) | 7 (44) | 24 (32) | ||
| Very High Risk, n (%) | 15 (16) | 8 (50) | 7 (9) | ||
| RT-PCR cycle threshold value ≤ 24 – n (%) n = 86 | 26 (30) | 8 (53) n = 15 | 18 (25) n = 71 | 2.6 (1.1-6.5), 0.0320 | 14.3 (2.0-101.5), 0.008 |
| C-reactive protein > 10 mg/dL – n (%) n = 88 | 45 (51) | 11 (73) n = 15 | 34 (47) n = 73 | 2.6 (0.9-7.6), 0.0590 | 2.2 (0.4-11.0), 0.351 |
| Total lymphocyte count < 800 cells/µL – n (%) | 49 (53) | 10 (63) | 39 (51) | 1.5 (0.6-3.7), 0.4151 | |
| D-dimer >1000 ng/mL – n (%) n = 87 | 21 (24) | 9 (60) n = 15 | 12 (17) n = 72 | 4.7 (1.9-11.7), 0.0004 | 9.0 (1.6-49.1), 0.012 |
| Lactate dehydrogenase > 245 U/L – n (%) n = 87 | 73 (84) | 15 (94) n = 16 | 58 (82) n = 71 | 2.9 (0.41-20.1), 0.2356 | |
| Ferritin >500 ng/mL – n (%) n = 87 | 44 (48) | 9 (56) n = 16 | 35 (46) n = 76 | 1.4 (0.6-3.4), 0.4580 | |
| Treatment with tocilizumab – n (%) | 6 (7) | 3 (19) | 3 (4) | 3.3 (1.3-8.5), 0.0293 | |
| Treatment with corticosteroids – n (%) | 57 (62) | 11 (69) | 46 (61) | 1.4 (0.5-3.6), 0.5380 | 1.1 (0.2-6.3), 0.895 |
95%CI: 95% confidence interval; aOR: adjusted odds ratio; ICU: intensive care unit; IQR: interquartile range; NIH: National Institutes of Health; RT-PCR: real time-polymerase chain reaction; RR: relative risk.
*Area under the curve 0.85, pseudoR2 0.289, n = 80. Exploratory models including Nutri-CoV category, and tocilizumab were constructed, and independent associations between the primary outcome and RT-PCR cycle threshold value ≤ 24, and D-dimer > 1000 ng/mL were observed.
DISCUSSION
In our study, male sex, high D-dimer levels, and RT-PCR Ct value ≤ 24 were associated with the need for IMV and in-hospital mortality in previously healthy and young patients hospitalized with COVID-19. Although in Mexico it has been reported that 17.7% of COVID-related deaths could occur in younger and non-comorbid patients12, a lack of information regarding prognostic factors in this population exists. Male sex has been reported to be associated with increased mortality in patients across all age groups. This independent association is believed to be influenced by sex-driven differences in the immune response to infection26. D-dimer levels correlate with coagulopathy and although the molecular mechanism of COVID-19-associated coagulopathy has not been completely elucidated, high levels of D-dimer have been independently associated with a worse prognosis27. Our results suggest that male sex and high D-dimer levels play a role in the prognosis of healthy young adults. Controversy exists regarding the prognostic importance of RT-PCR Ct values. Our results, in accordance with previous reports21,22,28-30, suggest that a low Ct value (particularly ≤ 24), which may reflect a higher viral load in swab samples, is associated with a worse prognosis. Contrary results have been published, but it has been proposed that symptom onset could have acted as a confounder31. In our study, this confounder was accounted for. In the previous reports, it has been suggested that the magnitude of the inoculum, specific environmental conditions, specific cellular responses, and genetic predisposition could play a role in the prognosis of patients with no other identified risk factors13-17. The latter have not been studied consistently and are difficult to assess in daily clinical evaluations.
We found a high frequency of death and need for IMV in our cohort. Our results differ from other reports, as death and need for IMV have been reported to occur in < 5% and 10%, respectively, in younger, non-comorbid patients with COVID-1911. More research is needed to clarify the reason of these differences. We did not find an independent association between the primary outcome and other factors, such as higher levels of C-reactive protein, ferritin or lymphopenia32,33. These findings could be partly explained by the fact that we excluded older and comorbid patients, as it has been proposed that important variations in laboratory markers could exist between COVID-19 patients across different age groups34. Despite the latter, to the best of our knowledge, no specific differences in laboratory markers have been reported to predict mortality across different age-specific groups. The fact that steroid treatment was not associated with the outcome calls for further study. In the age adjusted analyses of the RECOVERY trial results, steroid treatment was associated with lower mortality in patients aged < 70 years25, although comorbidities were not accounted for. To the best of our knowledge, no solid data regarding steroid use in the specific subset of young and healthy adults have been reported. This finding must be interpreted cautiously. Of note, we support steroid treatment regardless of age or comorbidities as recommended by published guidelines35,36. The frequencies of HAP/VAP and PE were lower than those previously reported37,38, which could be partly explained by the fact that our cohort was comprised of non-elderly and non-comorbid adults. The LOS and duration of IMV are compatible with previous reports39,40.
Our study presents limitations that must be acknowledged. Ours was an observational single-center study. Because mortality only occurred in patients with a need for IMV, our results may only reflect factors associated with that outcome. Still, we decided to analyze and report the primary composite outcome because of the prespecified analysis plan. In addition, we chose to study both in-hospital mortality and the need for IMV as a composite outcome because both endpoints represent devastating consequences for the patient and the health-care system, and also because not all the patients that require IMV may be necessarily started on such therapy. To minimize this bias, we chose to use a composite outcome. We included three patients admitted with moderate COVID-19; because of the low frequency of moderate cases, we believe no significant bias was present. Because of the large study period, and even though we reported the inclusion rate at important cut-off points in time (e.g., end of June 2020 or mid-February 2021, when steroid and remdesivir treatments were standardized in our center, respectively), we cannot account for the effect of the learning curve process and the rapidly changing standard of care, which may have resulted in variable treatment prescriptions and outcomes across time. Still, we believe that our cohort study is relevant to better understand complex phenomena in an understudied population. Our results suggest that further study remains needed.
In conclusion, male sex, higher levels of D-dimer, and low SARS-CoV-2 RT-PCR Ct value on nasopharyngeal swab at diagnosis are independently associated with increased in-hospital mortality and need for IMV in younger and otherwise healthy COVID-19 patients.











 nueva página del texto (beta)
nueva página del texto (beta)



