Background
Gunshot wounds can result from projectiles or fragments generated during explosions1 and constitute the most common cause of penetrating head trauma, or traumatic brain injury (TBI). Mortality rates associated with firearm injuries vary between 21% and 88%,2 with some authors reporting a survival rate as low as 9%.1 TBI is most frequently inflicted by smallcaliber projectiles (0.22-0.38) with low velocity (less than 304.8 m/s) and launched at a range of less than 50 meters.3
It is important to note that injuries caused by firearm projectiles differ from those resulting from traffic accidents, falls, and sports-related incidents, primarily due to the extent of tissue loss, anatomical disruption, bleeding, and tissue maceration.4 These differences are related to factors such as the energy and shape of the projectile, the angle of injury, and the characteristics of the affected tissues. As the projectile traverses the brain parenchyma, it inflicts damage to the surrounding tissue, leaving a path of permanent injury. In addition, it is preceded by a sonic wave that also causes damage. Highvelocity projectiles, on the other hand, generate cavitation that progressively expands and collapses, creating additional brain damage with each expansion-collapse cycle.1,3
Despite the indication of decompressive craniectomy (DC) as a treatment, it presents debatable results. For instance, the evaluation of DECRA (Decompressive Craniectomy in Patients with Severe Traumatic Brain Injury) through RESCUEicp (Randomized Evaluation of Craniectomy Surgery
for Uncontrollable Elevation of Intracranial Pressure) and RESCUE-ASDH (Randomized Evaluation of Craniectomy Surgery for Patients undergoing acute subdural hematoma evacuation) has shown increased rates of disability in survivors after traditional DC.5
Therefore, articulated craniotomy (HC), also called "hinge" or "floating" type, is presented as an alternative to traditional DC. This surgical technique enables adequate decompression and reduction of intracranial pressure while eliminating the need for a secondary cranioplasty, with improved outcomes anticipated (Table 1).6
Table 1 Gressot Functional Outcome Prediction Staging System. One point is assigned when the Glasgow Coma Scale (GCS) ranges from 3 to 5 points, non-reactive pupils are observed, and the patient's age exceeds 35 years. Two points are assigned if the projectile trajectory results in a bihemispheric and posterior fossa lesion.9
| Points | Probability of mortality | Probability of good prognosis |
|---|---|---|
| 0 | 25% | 55% |
| 1 | 30% | |
| 2 | 55% | 10% |
| 3 | 75% | 0% |
| 4 | ||
| 5 |
Case presentation
We present the case of a 38-year-old male patient who was the victim of an assault while leaving his residence. The patient sustained polytrauma to the skull resulting from a firearm projectile, with the entry point located in the right eye (Figure 1A). This projectile caused a fracture of the orbit involving its posterior, lateral, medial walls, roof and floor of the orbit, and complete loss of the right eyeball and extraocular muscles, accompanied by exposure of brain matter within the bilateral frontoparietal region (Figure 1B). The projectile’s exit orifice contributed to the multifragmented and comminuted fracture (Figure 1C).
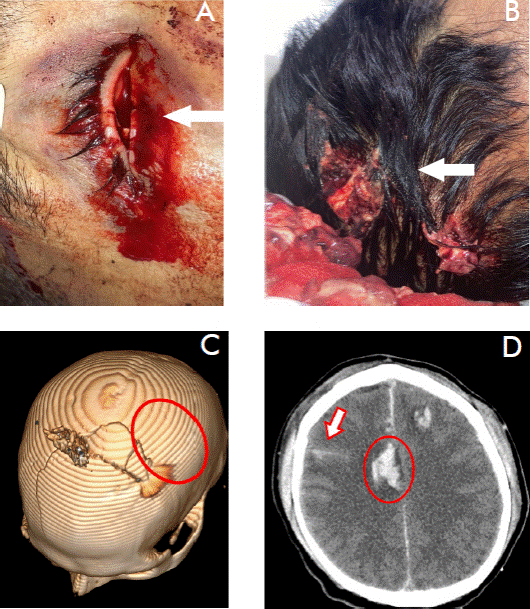
Figure 1 A) Entry point of the projectile through the right eyeball (arrow). B) Skull wound with exposure of brain mass (date). C) 3D reconstruction of the skull using computed tomography (CT); view from the cranial vault displaying the projectile exit orifice (circle). D) Bilateral subarachnoid hemorrhage (SAH) (arrow) and parasagittal hemorrhagic contusions (circle).
Notably, the horizontal direction of the firearm projectile inflicted damage to both hemispheres, accompanied by bilateral subarachnoid hemorrhage (SAH), parasagittal hemorrhagic contusions and cerebral edema, as depicted in Figure 1D.
In addition, the patient sustained multiple bullet wounds in both lower limbs, characterized by entry wounds on the lateral sides and exit wounds on the medial sides.
Paramedical personnel arrived ten minutes after the event; the patient was found awake, with a Glasgow Coma Scale (GCS) of 15 (O4, V5, M6), demonstrating coherent and congruent language, with the brain exposure described earlier.
Initially, the patient was transferred to the General Hospital of Axapusco, a regional hospital, where he presented with a GCS score of 8 points (O2, V2, M4). In response, advanced airway management, medical treatment, and resuscitation were started in accordance with the ATLS Guidelines for trauma management. Subsequently, he was transferred to the 1º de Octubre Regional Hospital for specialized neurosurgical care. The surgical treatment was performed 8 and a half hours after the injury.
The initial diagnosis, carried out by sagittal CT scan of the skull, revealed the trajectory of the projectile and the extent of the lesion. The injury affected even the portion of the corpus callosum and cingulum. Consequently, it was decided to performed a hinge type bilateral frontoparietal decompressive craniectomy, with haematoma evacuation, without removing the bone in the midline to avoid damaging the superior sagittal sinus (Figure 2 A).
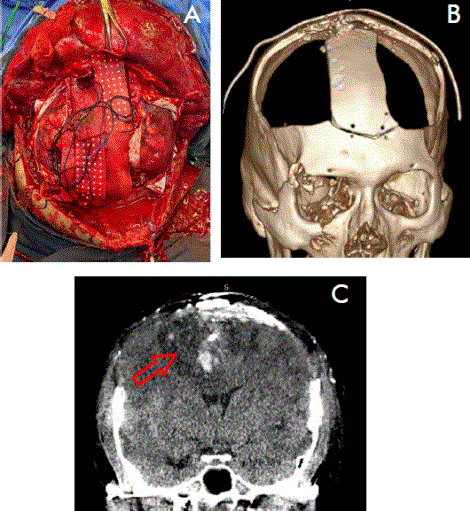
Figure 2 A) Transoperative control and B) 3D reconstruction of postoperative CT. C) Postoperative control with CT; coronal section of the skull
During the surgical procedure, a coexistence of a subdural hematoma and a cortical contusion (cortical burst) was found in the right precentral and left postcentral gyrus, accompanied by dura mater tearing. Accordingly, a complete opening of the dura mater was performed, with the portion near the superior longitudinal sinus being preserved. Bone splinters were removed, performing control of moderate bleeding within the superior longitudinal sinus by means of compression and the use of cottonoids for one hour and 30 minutes during the surgical procedure (Figure 2B).
Considering the patient’s initial neurological status and the lesions found during the intraoperative period, extubation was not attempted. The patient was admitted to the Intensive Care Unit (ICU) with a score of 5 points on the modified Rankin scale (a standard measure of neurological disability), where he remained sedated for 3 days, after which a neurological assessment was made, demonstrating an adequate response. The patient spent an additional two days in the ICU without sedation, resulting in a total ICU stay of five days. During this period, he underwent a tracheostomy and gastrostomy procedure. Next, he was extubated and transferred to the neurosurgery service, with a modified Rankin scale score of 4. He remained under the same care plan for 17 days. Upon discharge from the hospital, he had a modified Rankin scale score of 3, left brachiocrural hemiparesis, strength rated at 3/5 on the Daniels scale, total loss of the eye, tracheostomy and gastrostomy.
As part of the postoperative management, the patient was referred for rehabilitation. A postoperative control was conducted one month and twenty-two days after the surgery, utilizing a CT scan of the skull in the coronal section, which revealed the re-expansion of the encephalic tissue (Figure 2C). In addition, at a follow-up appointment, the patient presented a GCS score of 11 points, left hemiparesis, with strength rated at 4/5 on the Daniels scale. He no longer required tracheostomy or gastrostomy support, exhibited oral tolerance, coherent language, and adequate vocalization, and showed no signs of complications. However, the prognosis for his function and quality of life remains guarded.
Discussion
Within the injuries caused by firearms, two categories can be distinguished; the primary lesion, which is determined by the ballistic characteristics of the projectile, and secondary injury, which is generated by bone and metal fragments.7 The mortality associated with such injuries depends on the location of the wound and its trajectory. Notably, bihemispheric wounds, as seen in the case described earlier, have a particularly high mortality rate, with Martins et al. reporting rates as high as 96.2% and 100% for posterior fossa wounds.8 Consequently, it is observed that 70% of patients with TBI die within the first 24 hours post-injury, and patients with TCE have a survival rate of less than 10%.9
On a separate note, the greatest challenge neurosurgeons face when treating gunshot wounds is to decide between performing surgery and guaranteeing patient survival at any cost or pursuing a higher quality of survival in selected patients. The dilemma lies in deciding which type of patients are candidates for surgical treatment, considering not only the trajectory of the projectile but also the patient's hemodynamic status and their GCS score upon arrival at the emergency department.10
Nevertheless, there exists a consensus that when a patient arrives at the emergency room, the priority should be stabilization, including the ABCD (Airway, Breathing, Circulation, Disability) assessment for all trauma patients. Once the scalp lesion has been identified, complementary imaging studies should be performed, since they can determine the trajectory of the projectile and the affected structures. Furthermore, these studies help to determine an adequate treatment plan, including the type of surgery to be performed. Consequently, CT of the skull with bone reconstruction has become the preferred study.11
In relation to patient management, Graham et al 12 argue that surgical treatment is viable in patients with a GCS score ranging from 6 to 8, with satisfactory results in 20% of cases. On the other hand, patients with bihemispheric or multilobular involvement of the dominant hemisphere tend to have poorer results. In contrast, Joseph et al. advocate for a more aggressive approach in patients with a low GCS score (3 to 5) or those with bihemispheric lesions, asserting that this approach can enhance survival capacity, increasing from 10% to 46%.13
In cases of minor injuries caused by firearm projectiles, such as non-penetrating injuries like tangential injuries, they require surgical lavage and debridement with subsequent antibiotic therapy. Conversely, focal lesions with active hemorrhage, bone or metallic fragments, and without mass effect require surgical exploration, specifically through a targeted craniotomy to the affected areas. Finally, severe injuries, such as transventricular or bihemispheric injuries, demand extensive surgical intervention, including debridement, hematoma drainage, decompressive craniectomy, dural repair, and management by stereotaxis.2,14
According to a RESCUEicp study,15 which focused on demonstrating the effectiveness of decompressive (bifrontal) craniectomy compared to medical treatment in cases of intracranial hypertension, it was concluded that this surgical procedure reduced the duration of ICU stays and lowered mortality rates in affected patients. However, the survivors did not achieve adequate functionality, experiencing a higher incidence of vegetative states or neurological sequelae.
Qiu et al.11 conducted randomized studies in 2009 to compare the outcomes of decompressive craniectomy performed at different time intervals following trauma, that is, within the first 24 hours (early) and after 24 hours (late), against medical treatment. These studies revealed that early unilateral decompressive craniectomy in patients with radiographic signs of herniation was superior in reducing intracranial pressure, decreasing mortality, and leading to improved functional outcomes for the patients.
Because the patient in the clinical case met the criteria for surgical treatment as indicated by the Gressot staging system for predicting functional outcomes, the decision was made to proceed with bifrontal decompressive craniectomy, supported by the tomography findings. This approach resulted in favorable functional outcomes for the patient.
Conclusion
Penetrating brain injuries caused by firearm projectiles continue to pose challenges and carry a high mortality rate for neurosurgeons. However, some predictive factors, such as the Glasgow Coma Scale score below 9 at admission, accurate identification of the structures affected by the wound trajectory, the timing of surgical intervention following the injury, and the patient’s age, allow to decide a surgical approach that leads to a favorable prognosis with an adequate functional evolution aligned with the patient’s age, as demonstrated in the presented case. In this context, aggressive management was essential, specifically the implementation of decompressive craniectomy and debridement within the first 12 hours after trauma. Notably, despite the location of the lesions and the potential complications, such as surgical wound infections, permanent neurological deficits, cerebrospinal fluid fistula, and infection in the right eye due to direct projectile injury, these complications did not manifest in the patient. The favorable recovery without associated complications, in this case, can likely be attributed to the prompt management based on the predictive factors previously described. In conclusion, the preferred surgical treatment is early decompressive craniectomy when the criteria outlined in the Gressot staging system for predicting functional results are met.











 nueva página del texto (beta)
nueva página del texto (beta)



