Background
The first case report related to Kambo was published in 1925 by the Frenchman Constantin Tastevin. It is a ritual that consists in inoculations of Kambo, the skin secretion of the toxic Brazilian frog Phyllomedusa bicolor and has been practiced worldwide, especially in South America, because of the belief that this secretion can purify the mind and spirit against negative energy, enhancing the immunological system, and sharpening the senses and physical abilities of hunters; currently, people use Kambo out of interest or to cure multiple diseases.1 This ritual is known by different names, including Kambô, kampu, vaccino da floresta and also sapo, which means "toad" in Spanish.2
Case report
A 41-year-old male with no relevant medical history, Marijuana user since he was 24 years old (last consumption three months ago), reported one-year untreated generalized anxiety disorder with panic attacks every 72 hours and claustrophobia. In order to reduce this symptomatology, he decided to try a ritual that consists in inoculations of Kambo.
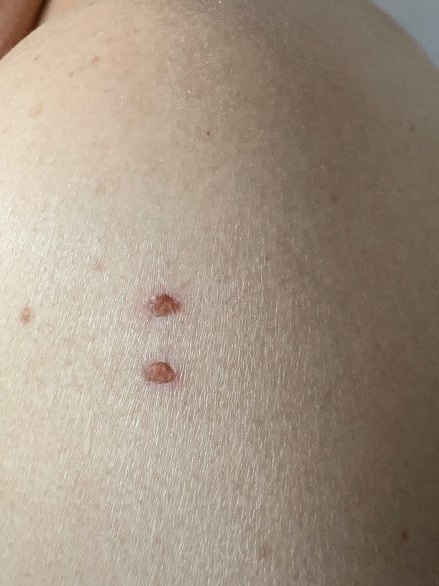
Before the ritual he was hydrated with 1 liter of water, then he was burned in two points on the left shoulder, where the gelatinous Kambo substance was applied (Figure 1). After 30 minutes, he started vomiting during 10 minutes, at least 40 times, then he experienced generalized tremors for 20 minutes, at the end of which he started with moderate holocranial headache, fatigue, vertigo, and paresthesias in both hands. For the next 24 hours, he continued with slight dizziness without auditory alterations, paresthesias in the index finger of the left hand, and bilateral palmar hyperhidrosis. Five days later he required a neurological consultation because of hand paresthesia and generalized anxiety. During the physical examination, vital signs were found normal, the general aspect showed only scars on the left shoulder (Figure 1). At the neurological examination, the patient was alert, conscious, oriented in person, place and time, without alterations in language; he had an anxious expression and distal tremor of hands with sweating, his motor system had a score of 5/5 in generalized strength according to the Medical Research Council (MRC) Scale for Muscle Strength, muscle stretch reflexes (bicipital, styloradial, patellar and Achilles) were bilaterally normal, and Babinski reflex was negative in both lower limbs; regarding the exteroceptive sensory system, hypoesthesia was found in the left index finger, the rest without alterations, and hypopallesthesia of 2 seconds in the lower limbs and 10 seconds in the upper limbs; cerebellar signs without alterations; atavistic or meningeal signs were not present; gait disturbance, steppage type, and positive Romberg's sign were recorded. His blood tests, including complete blood count, comprehensive metabolic panel, liver panel, serum electrolytes (Na+, K+, Cl-, Ca+2, Mg+, P+), C-reactive protein levels, and general urine test were normal, and only minor dyslipidemia was found (cholesterol 210 mg/dl and triglycerides 280 g/dl). Electrocardiogram and electroencephalogram were normal.
A subacute Kambo frog poisoning was diagnosed, and the patient received 50 mg of oral prednisone during one week - the dosage was decreased throughout a month - 10 mg of diphenidol every six hours for one week, and 20 mg of paroxetine every day for six months. After six months of follow-up, the patient became asymptomatic.
Discussion
A case of a male with an acute and subacute Kambo Frog poisoning in Mexico is reported. The clinical manifestations are secondary to bioactive peptides applied to burned skin, which in a matter of minutes enters the lymphatic system and subsequently the blood. Different peptides are found in the excretions of Phyllomedusa skin: tachykinins, which act in the gastrointestinal system by increasing the smooth muscle contractility, salivation and secretion of lacrimal glands, and are vascular vasodilators that cause central arterial hypotension, increasing the excitability of neurons; sauvagine, a neuropeptide with an effect similar to corticotropin-releasing hormone, and cerulein, an oligopeptide with a similar function to cholecystokinin, that acts on cholecystokinin type A receptors causing a strong contraction of the smooth musculature and increased intestinal transit, and gastric and pancreatic secretions, it also induces contraction of the gallbladder, relaxation of the sphincter of Oddi, delayed gastric emptying and hyperglycemia. Furthermore, the effect of cerulein causes explosive vomiting in the first minutes of the ritual, moderate elevation of blood pressure, tachycardia and generalized tremor, as well as a sudden loss of electrolytes and physical fatigue. In this case, the patient also experienced a transient sensory polyneuropathy (due to affectation of the exteroceptive modality with localized hypoesthesia to the left index finger and hypopallesthesia in the lower extremities) that had not been described before in this toxic event, however, it was not possible to perform a nerve conduction study. The substances that can be related to this neuropathy are tachykinin, mediated through the B receptors that participate in mechanisms linked to pain, dermorphins and deltorphins, as well as Mu opioid agonists that act on Mu and Delta receptors of the central nervous system involved in analgesic effects, however, phyllocerulein, phylloquinine, adenoreregulin and others, can also cause similar or other effects, that are yet to be determined.3
Two phases have been described in Kambo intoxication: the first phase, that usually lasts 15-30 minutes, is characterized by nausea, abdominal pain, and abundant and frequent vomiting, which are momentary as in our patient. However, severe complications have been reported in this stage: altered consciousness, symptomatic seizures, psychomotor agitation, psychosis, hallucinations, fever, esophageal rupture, systemic inflammatory response syndrome, and even death.4 The second phase includes the persistence of acute symptoms, syndrome of inappropriate antidiuretic hormone secretion, acute toxic hepatitis, and dermatomyositis. Our patient presented the classic acute symptoms, however, he persisted with focal sensory neuropathy.
The treatment of Kambo poisoning is essentially symptomatic, and is based on the clinical manifestations, for example, antiseizure medications, antipsychotics, or steroids, all with good response.5 In this case, prednisone, diphenidol and paroxetine were indicated.











 nueva página del texto (beta)
nueva página del texto (beta)