Background
The Artery of Percheron or Percheron Artery was first described in 1973 by Gérard Percheron as an infrequent perforating thalamic anatomical variant present in 11 to 33% of the population. It should be noted that the irrigation of the anterior and inferior midbrain and thalamus is provided by the internal carotid artery, while the medial, lateral, and posterior territories are irrigated by the vertebrobasilar system. Percheron artery originates from a single pedicle, and can express a complex clinical syndrome, being the origin of 0.1 to 6% of all cerebral infarctions.1-3
The paramedian artery derives from the proximal P1 segment of the posterior cerebral artery, and supplies the ventral medial thalamus, the hypothalamus, as well as the mesencephalic subthalamic junction, superior part of the brainstem, encompassing the interpeduncular nuclei, the decussation of the superior cerebellar peduncles, anterior portion of the periaqueductal gray matter, medial part of the red nucleus, and nucleus of the third and fourth cranial nerves.4-5
In anatomical terms, it is a common trunk emerging from the posterior cerebral artery between the basilar artery and the posterior communicating artery, supplying both paramedial territories of the thalamus and territories of the rostral midbrain region.6-7
Presentation of the case
A 49-year-old male patient with a chronic degenerative history of systemic arterial hypertension. He came to the emergency department five hours after suddenly developing holocranial headache of intensity 9/10 and altered level of consciousness with progressive deterioration, until reaching deep stupor. The patient presented with complete dense right pyramidal syndrome and required advanced airway management with strict neurological monitoring.
Extubating was achieved with adequate airway progression; the patient persisted with the previously described pyramidal syndrome, without cranial nerve involvement and without alteration of sensitivity, with a rating of four according to the modified Rankin scale prior to discharge.
Likewise, the protocol for cerebral infarction was performed and the following results were obtained in laboratory studies: normal blood chemistry, lipid profile and thyroid profile; imaging studies: electrocardiogram and transthoracic and transesophageal echocardiogram without alterations; carotid ultrasound with evidence of atherothrombotic plaque with bilateral involvement of 40% right and 70% left (not being a candidate, by assessment of interventional neurology and radiology, for prosthesis); simple cranial tomography at 12 and 48 hours without data of hemorrhage or early data of ischemia. Simple magnetic resonance imaging of the brain was also performed (Figure 1), which showed bilateral thalamic hyperintensity in Fluid-Attenuated-Inversion-Recovery (FLAIR) with diffusion restriction in Diffusion Weighted Imaging (DWI), and Percheron syndrome was integrated due to the involvement of the bilateral territory corresponding to the paramedian artery derived from the proximal P1 segment of the posterior cerebral artery.
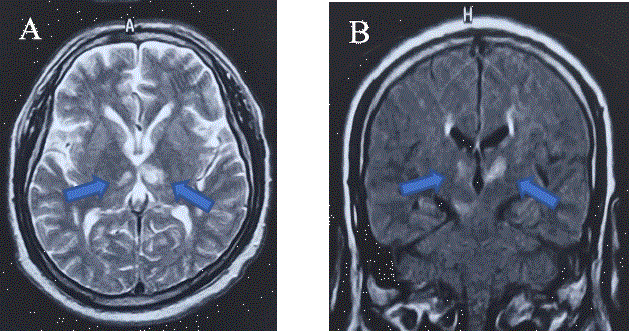
Figure 1 A) Axial T2 FLAIR MRI showing bilateral ischemic infarction in the thalamic region without evidence of white matter lesions, and without evidence of hemorrhage or infarct complications (blue arrows). B) DWI is observed with diffusion restriction and with lesions present in bilateral thalamic region (blue arrows), in a coronal section without presence of infarct complications, without hemorrhage or midline displacement.
Discussion and conclusion
The artery of Percheron syndrome is called by some authors chameleon stroke due to its varied and unusual aspect, which may present internuclear ophthalmoplegia, LV paresis, Edinger Westphal nucleus alteration, hemiplegia and movement disorders. Initially, in the reported case, hemorrhage was suspected in the first instance. However, the diagnosis was reached through an imaging study of ischemic cerebral infarction, performing diagnostic protocol and concluding atherothrombotic origin.8
There are four imaging patterns of presentation syndrome: 43% present as bilateral paramedian thalamic and mesencephalic infarction, 38% with bilateral paramedian thalamic lesion only, 14% with lesion in the anterior thalamic nucleus, bilateral paramedian thalamic and midbrain and 5% bilateral paramedian and anterior thalamic. In turn, the V sign is a distinctive V-shaped hyperintensity pattern observed along the surface of the midbrain in the interpeduncular fossa; in this case this sign was not found.9,10
It is important to keep in mind the differential diagnoses of clinical importance, whether of vascular origin, such as cerebral venous thrombosis, basilar cap syndrome and one and a half syndrome, or other pathologies that can bilaterally affect the thalamus not being vascular, such as osmotic demyelination syndrome, anoxic ischemic encephalopathy, Wilson's disease, toxoplasmosis, human immunodeficiency virus, CreutzfeldtJakob and Fahr's disease.11-12
The aim of this review is to provide the reader with information about the anatomical support and imaging correlation patterns of previous case reports and the case presented.
The importance of considering differential diagnoses and overlaps with other syndromes should be emphasized, as this will determine how quickly the quality of life of these patients can be improved. Finally, it is also significant to know that cerebral infarction has late expressions such as anxiety, depression or other atypical symptoms of unusual evolution.13-14
Authors’ contributions
Sebastián León Vallejo: main research, writing - revision and editing. Perla Karina Anzures Gómez: support research, writing - original draft. César Camacho Becerral: support research. Daniel Reyes Ortega: support research. Luis Humberto Torres Pérez: support research. Gustavo González González: resources, validation.











 nueva página del texto (beta)
nueva página del texto (beta)


