Introduction
Mondors disease is defined as thrombophlebitis of the superficial veins of the dorsum of the penis1. Braun-Falco first reported isolated phlebitis in the dorsal vein of the penis in 18582, but the disease is named after Henri Mondor, a French surgeon responsible for describing a series of cases of thoracoepigastric vein thrombosis in female patients in 19393,4.
It manifests acutely as a subcutaneous indurated band that generates regional pain and episodic palpitations5; it is generally self-limiting in a range of 4-8 weeks6. It is an uncommon condition, with unknown pathophysiology, although there are hypotheses that indicate that the most common etiology is inflammation of the venous drainage of the penis together with Virchow's triad secondary to surgeries in the region, genital trauma, neoplasms, excessive exercise7 blood stasis due to prolonged erection, vigorous sexual activity, bladder overdistension, and use of PDE inhibitors5,6.
It affects sexually active men between 18 and 70 years of age, its incidence is 1.39% in a population between 20 and 40 years of age8; although it is believed to be higher, it is underdiagnosed because patients do not seek medical attention due to stigma9. The diagnosis is clinical, confirmed with Doppler ultrasound, where the main finding is the thrombosed vein in grayscale with the absence of flow; magnetic resonance angiography is also an option to confirm the diagnosis, as the venous network of the dorsum of the penis is dilated10,11.
Treatment aims to control pain and reduce inflammation; non-steroidal anti-inflammatory drugs are widely used1. In addition to sexual abstinence, anticoagulant drugs, such as heparin, may be given in the acute phase of the disease6.
Case report
A 24-year-old male patient with a history of epilepsy was treated with magnesium valproate and the rest of the history was denied. For 3 months before his evaluation, he has had localized pain in the dorsum of the penis that is exacerbated by morning erections and at the time of urination due to the manipulation of the penis, sexual abstinence in this period due to pain.
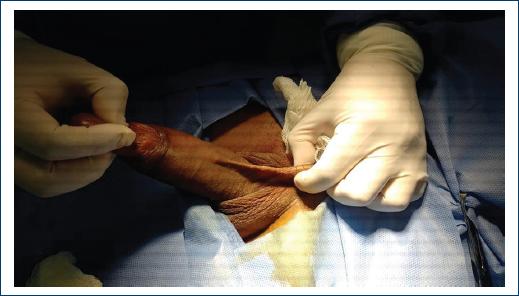
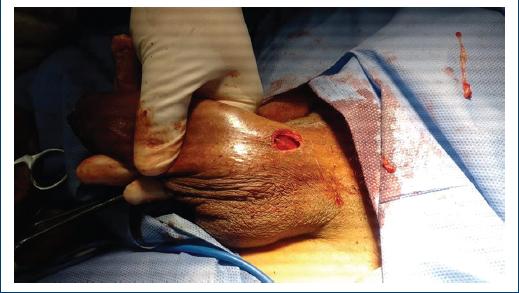
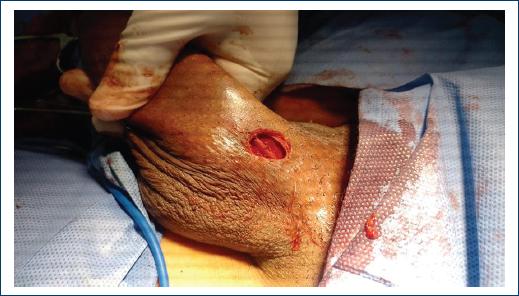
She received previous treatment with antiplatelet and phlebotonics without any improvement, in addition to non-steroidal anti-inflammatory drugs without response; physical examination reveals stony and rosy tissue, which runs from the base of the penis and continues along the entire dorsum of the penis to the balanopreputial sulcus (Figs. 1 and 2). Resection of the superficial vein of the dorsum of the penis was performed with histopathological findings of thrombophlebitis, vein fragments with thrombi in the recanalization phase and fibrosis of the intima and hypertrophy of the muscle; and focally infiltrate chronic inflammatory lymphocyte in the intima and tunica media (Figs. 3 and 4).
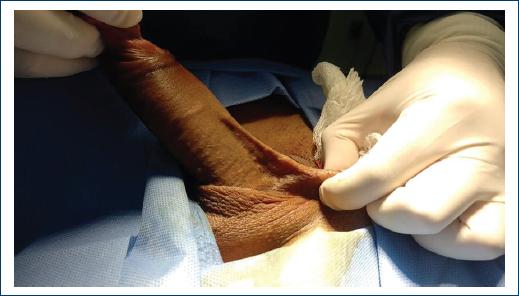
Figure 1 Stone band and curling on the back of the penis, shows fibrosis on the back of the penis one from the base.
Discussion
The cases reported in the literature found a benign condition as the most frequent cause of superficial thrombosis of the dorsal vein of the penis12, the risk factor associated with the patient was vigorous sexual activity. Conservative medical treatment is the first option, consisting of sexual abstinence, pain relief, and control of inflammation with non-steroidal anti-inflammatory drugs; in addition, the improvement of circulation, only in the case of patients with underlying hypercoagulability problems with phlebotonics and anticoagulant. However, when thrombophlebitis persists for more than 8 weeks due to failure in first-line management, surgical correction based on resection of the superficial vein of the penis is resorted to.
In the reported case, a proximal and distal approach was performed, a procedure similar to performing a saphenectomy, with the aim of performing a minimally invasive surgery that does not compromise the patient's sexual functioning and performance due to complications such as pain in erection and fibrosis of the penis. In 2009, Salmon et al.13 proposed a non-invasive technique to solve Mondor's disease, manual axial distraction, which provides patients with a fast, effective solution without adverse effects; it consists of applying firm pressure with distraction to several points of the thrombosed vein until the tension is overcome.
Prognosis depends on the underlying disease that led to dorsal penile vein thrombophlebitis; a report by Özkan in 2015 with 30 patients resolved with medical treatment reported that no permanent deformity of the penis or erectile dysfunction was found during the follow-up of the cases. Our patient had a satisfactory evolution with morning erections and the beginning of sexual life at 6 weeks.
Conclusion
It is a rare condition that is usually self-limiting and only requires pharmacological treatment. The choice of surgical treatment is made when the patient is resistant to conservative treatment after 8 weeks; surgical management should be less invasive to avoid complications such as fibrosis or erection pain and consequently improve the patient's quality of life.











 nueva página del texto (beta)
nueva página del texto (beta)