
Choque cardiogénico: El tratamiento en el futuro cercano
Cardiogenic shock: treatment of the near future
Efraín Gaxiola,* Ulises Ramírez–Sánchez**
* Jefe del Departamento de Cardiología Intervencionista. Instituto Cardiovascular de Guadalajara.
** Médico adscrito al Servicio de Cardiología. Hospital Regional Universitario SSA.
]]>Correspondencia:
Dr. Efraín Gaxiola.
Avenida Hidalgo 930. Col. Artesanos,
Guadalajara, Jalisco 44290.
Tel (33) 3827 1668; (33) 3827 1669, Fax (33) 3827 1670.
Correo electrónico:efraingaxiola@yahoo.com
Resumen
Durante la última década, la mortalidad del choque cardiogénico ha disminuido significativamente debido a la implementación de estrategias de reperfusión coronaria asociadas al uso de balón intraaórtico de contrapulsación. Sin embargo, a pesar de estas medidas la mortalidad es aún muy elevada. Actualmente y en los siguientes años, las medidas están encaminadas a acortar los tiempos para lograr la reperfusión coronaria y diferentes estrategias para preservar y prolongar la viabilidad celular miocárdica.
]]> Palabras clave: Choque cardiogénico. Infarto agudo del miocardio. Angioplastía coronaria. Stent coronario.
Summary
The mortality rate for cardiogenic shock has decreased over the past decade. These improvements are presumed to reflect increased use of intraaortic ballon counterpulsation and coronary reperfusion strategies which, by restoring patency to the infarct–related artery, can limit infarct size. Despite these therapeutic measures, mortality rates remain elevated. Current strategies are aimed at decreasing reperfusion times and measures to preserve and prolong myocardial cell viability.
Key words: Cardiogenic shock. Acute myocardial infarction. Primary percutaneous coronary angioplasty. Coronary stent.
Introducción
El choque cardiogénico (CHC) (ocurre en aproximadamente 6% a 7% de los infartos agudos del miocardio (IAM).1,2 Aunque éste ocurre con mayor frecuencia en los pacientes (pts) con IAM con elevación del segmento ST, puede también ocurrir en pts con síndromes isquémicos coronarios agudos (SICA) sin elevación del segmento ST.3
Históricamente la mortalidad del CHC era del 80–90%.4 Durante la última década se ha observado una reducción en la mortalidad hospitalaria en el rango del 56% al 74%.1 La disminución en la mortalidad observada los últimos años se ha atribuido al uso incrementado del balón intra–aórtico de contrapulsación (BIAC) y a las estrategias de reperfusión coronaria..5,6 El estudio SHOCK7 demostró que los pts con CHC sometidos a implantación de BIAC y una estrategia de revascularización urgente tenía mayor sobrevida a un año comparado con la estrategia de implantación de BIAC y fibrinólisis seguida de estabilización farmacológica intensiva. Este beneficio se observó en pts menores de 75 años de edad.
]]> Tratamiento actual del choque cardiogénico
El tratamiento actual del CHC debe incluir el uso de BIAC, terapia de reperfusión lo más pronto posible mediante intervención coronaria percutánea (ICP) y aunque no ha sido demostrado en estudios aleatorizados, algunos autores sugieren beneficio adicional con el uso de stents coronarios y antagonistas de la glucoproteína IIb/IIIa (A–GP IIb/IIIa).8,9
Los lineamientos actuales sobre manejo del CHC por parte del panel de expertos del Colegio Americano de Cardiología y de la Asociación Americana del Corazón (ACC/AHA), sugiere recomendación clase I para realizar ICP primaria o cirugía de revascularización coronaria de emergencia (CRCE) en pts menores de 75 años de edad con IAM con elevación del segmento ST que desarrollen choque en las 36 h de inicio del IAM y que puedan ser tratados en las siguientes 18 h de inicio del estado de CHC. Se considera razonable (Clase Ha) realizar ICP o CRCE en pts seleccionados con edad >75 años.10 La Figura 1 sugiere un flujograma de manejo para pts con CHC.

Nuevos enfoques en el tratamiento del choque cardiogénico
A pesar de obtener una angioplastía exitosa, el registro SHOCK mostró una mortalidad a 30 días del 38%;11 esto pudiera sugerir la existencia de daño miocárdico irreversible al momento de la reperfusión y que a pesar de ello, no se logre una detención de los efectos deletéreos de todos los factores humorales e inflamatorios secundarios al estado de choque. Además de la noción clásica donde se sugiere que la necrosis del 40% de la masa ventricular izquierda lleva a una disfunción severa e irreversible del corazón que condiciona caída del gasto cardíaco y con ello una serie de manifestaciones secundarias a hipoperfusión sistémica, se conoce actualmente que el estado de CHC origina un estado inflamatorio sistémico con activación de complemento, liberación de citocinas inflamatorias, expresión incrementada de la sintasa de óxido nítrico y que todos estos factores llevan a un estado inapropiado de vasodilatación sistémica12 (Fig. 2).
De tal manera que las estrategias actuales y futuras, tanto farmacológicas como intervencionistas en el tratamiento del pte con IAM y potencialmente con CHC están destinadas a: 1) Mejorar la perfusión miocárdica, 2) prevenir el daño miocárdico y la alteración del estado metabólico y 3) la reparación del daño muscular.
]]> Estrategias para mejorar perfusión tisular
Sin duda, la introducción de los A–GP IIb/IIIa contribuyen a la obtención de un flujo tisular de mejor calidad, tanto en su asociación con fibrinolíticos así como con ICP, pero desafortunadamente esta mejoría en la calidad de la perfusión no se ha reflejado en disminución de la mortalidad.13,14 También se han evaluado medidas para disminuir y extraer la cantidad de trombo intracoronario mediante dispositivos de trombectomía percutánea y estrategias para prevenir embolismo distal durante ICP, aunque estas estrategias también han mejorado la calidad del flujo coronario, no han demostrado disminución de mortalidad y otros eventos clínicos mayores.15
Prevención del daño miocárdico y alteración del estado metabólico
Existen varias estrategias que se han evaluado para prevenir la muerte celular miocárdica así como evitar la alteración del estado metabólico, entre las cuales se encuentran: a) Inhibidores de complemento, b) Bloqueadores de la sintasa de óxido nítrico, c) Hipotermia, d) Oxígeno hiperbárico intracoronario, e) Adenosina, f) Solución glucosa–insulina–potasio (GIK).
Inhibidores del complemento: El complemento es un mediador importante del daño inflamatorio y su activación en el IAM se ha asociado a varias situaciones: IAM de gran tamaño y malos resultados clínicos,16 asociado al daño por isquemia/reperfusión al activar leucocitos y células endotelíales, daño celular directo, regulación a la alta ("up–regulation") de genes involucrados en producción de citocinas y actividad incrementada de la sintasa de óxido nítrico.17 Se ha evaluado el uso de pexelizumab, un anticuerpo anticomplemento C5 asociado a ICP primaria y a fibrinólisis. La asociación con fibrinólisis no se reflejó en disminución del tamaño del IAM,18pero al asociarse a ICP, aunque aparentemente no disminuyó tamaño del infarto, sí mostró una disminución significativa en sobrevida a 6 meses cuando pexelizumab se administró en bolo e infusión intravenosa durante 20 h comparado con placebo o comparado con pexelizumab en bolo sin infusión (la mortalidad respectivamente fue de 3.2%, 7.4% y 3.2%, p = 0.018).19 Esto originó que se planeara el estudio APEX–MI con cerca de 8,500 pts con infarto tratados mediante esta estrategia para definir con mayor objetividad el papel de la inhibición del complemento en estos pts.
Bloqueadores de la sintasa de óxido nítrico (S–ON): Los pts con CHC tienen una expresión incrementada de la S–ON. El ON a dosis bajas produce relajación vascular y tiene efecto inotrópico positivo, en cambio, a dosis altas, como ocurre en el estado de CHC, produce inhibición directa de la contractilidad miocárdica, supresión de la "respiración" mitocondrial en miocardio no isquémico, tiene efecto sobre metabolismo de la glucosa, efecto proinflamatorio, respuesta disminuida a catecolaminas e inducción de vasodilatación sistémica.12 Los inhibidores de la S–ON bloquean los efectos deletéreos asociados a cantidades elevadas de ON en pts con CHC. Cotter y colaboradores20 mostraron que la administración del inhibidor de la S–ON (L–NAME –N–Nitro–L–Arginina–Metil Ester–: 1 mg/kg en bolo e infusión 1 mg/kg/h x 5 h) en 30 pts con CHC refractario a las medidas convencionales, se asoció con disminución en la mortalidad a 30 días (27% con L–NAME vs 67% con placebo, p = 0.008), además de aumento significativo de la presión arterial y gasto urinario en las primeras 24 h posteriores a su administración. Este es el único estudio aleatorizado que ha mostrado efectividad en disminución de mortalidad de una medida farmacológica en pts con choque cardiogénico. La población fue pequeña y necesitará de reproducción de resultados en estudios de mayor escala.
Hipotermia: La hipotermia se ha usado durante décadas en cirugía cardíaca y pediátrica para la preservación de tejidos así como en pts con eventos neurológicos donde la hipotermia inducida se ha asociado a mejoría en sobrevida y en recuperación neurológica.21 Dos estudios aleatorizados han comparado ICP e inducción de hipotermia ligera mediante sistema endovascular de enfriamiento con ICP sola en pts con IAM de menos de 6 h de evolución (COOL–MI TCT 2003 W. O'Neill y ICE–IT TCT 2004 C. Grines). En ambos estudios, la ICP asociada a hipotermia inducida mostró disminución del tamaño del infarto en localization anterior y en pts con temperatura < 35° C. Parece ser que el beneficio es mayor cuando la hipotermia logra inducirse antes de la reperfusión. El estudio LOW–TEMP con mayor número de pts se está realizando actualmente y buscará definir con mayor objetividad el papel de la hipotermia en este escenario.
Oxígeno hiperbárico: Estudios experimentales han mostrado disminución del daño originado en situaciones de isquemia–reperfusión, los mecanismos potenciales propuestos incluyen: mejor liberación de O2 al tejido isquémico, inhibición de la adherencia y "taponamiento" por leucocitos, disminución del edema tisular y efecto antagónico de la peroxidación de lípidos. El estudio AMI–HOT presentado por el Dr. W. O 'Neill en el ACC 2004 incluyó pts con IAM de < 24 hrs de evolución, estos pts fueron sometidos a ICP e implante de stent y posterior a ello se dejaba un catéter de perfusión en la coronaria tratada para infundir oxígeno hiperbárico durante 90 min, el otro grupo de pts fue sometido sólo a implante de stent y la terapia convencional. El objetivo primario fue evaluar el tamaño del infarto y la movilidad segmentaria a 14 días. El estudio mostró mejoría en la movilidad segmentaria a 14 días sólo en pts con IAM de < 6 h de evolución y que fueron sometidos a ICP e infusión intracoronaria de oxígeno hiperbárico. Este estudio sentó las bases para que se lleve a cabo otro estudio aleatorizado con mayor número de pts e incluyendo sólo IAM de < 6 h de evolución.
Adenosina y solución glucosa–insulina–potasio (GIK): Ninguna de estas dos medidas farmacológicas ha mostrado beneficio sobre mortalidad o eventos clínicos mayores en pts con IAM. Aunque adenosina asociada a fibrinólisis ha mostrado reducción en el tamaño del infarto en pts con IAM anterior cuando se administra a dosis de 70 µg/kg/min durante 3 h, no ha mostrado disminución en incidencia de insuficiencia cardíaca ni mortalidad.22 Recientemente, el estudio CREATE–ECLA23 que evaluó la solución GIK en más de 20,000 pts con IAM no mostró beneficio sobre mortalidad.
]]> Otras estrategias: Se han evaluado numerosos fármacos en un intento por disminuir el tamaño del infarto y/o proteger del deterioro metabólico celular, pero ninguno de ellos ha mostrado beneficio en este escenario. Entre las estrategias evaluadas que no han mostrado beneficio se encuentran: Inhibidores de adhesión de neutrófilos, bloqueadores de canales de calcio, inactivadores de radicales libres (hSOD –superoxido dismutasa–), agentes surfactantes con propiedades antitrombóticas y hemorreológicas (ej. reothrex), antioxidantes (trimetazidina), donadores de ON (ej. Molsidomina), corticoesteroides, algunos inhibidores del complemento e inhibidores del intercambio Na–Hidrógeno (ej. cariporide, eniropide).24
Estrategias para regeneración muscular miocárdica: Existen actualmente varios estudios pequeños publicados y otros en evolución que tienen como objetivo originar o regenerar músculo cardíaco en los sitios donde la necrosis miocárdica se ha consumado.25 Las estrategias incluyen el uso de células troncales o "células madre" embrionarias, células madre "adultas", células madre de médula ósea, cultivo de células de músculo esquelético entre otras. Aunque algunos estudios iniciales han sido alentadores, existen todavía muchas interrogantes y preocupaciones asociadas al uso de estas diferentes técnicas: pueden originar un sustrato arritmogénico, reacción inflamatoria local, disincronía en la contracción muscular, no se conoce la cantidad de células a implantar ni el tiempo ideal cuando deba llevarse a cabo, si debe ser una aplicación única o deben realizarse varias sesiones, etc.
Conclusiones
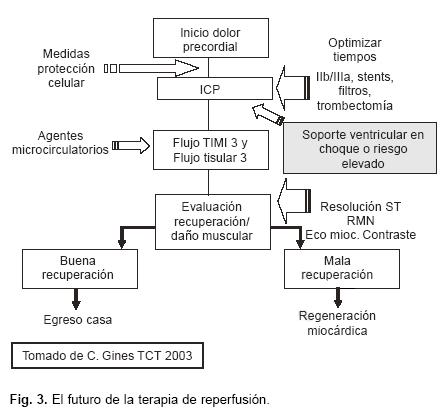
Si partimos del hecho de que a mayor tiempo de oclusión coronaria, mayor necrosis miocárdica, y que finalmente la cantidad de miocardio dañado en forma irreversible es el determinante de la función cardíaca y la aparición de CHC, entonces, las medidas actuales en el manejo del pte con IAM deben ir encaminadas a disminuir el tiempo de oclusión coronaria mediante la implementación expedita de las estrategias de reperfusión. Las estrategias de reperfusión deben ser apoyadas con medidas que protejan el estado metabólico de los cardiomiocitos e idealmente con estrategias que prolonguen el tiempo de tolerancia a la isquemia para que la necrosis miocárdica no se desarrolle o se desarrolle en forma más tardía y permita la implementación de estrategias protectoras de los cardiomiocitos (Fig. 3).
Referencias
]]>1. Goldberg, RJ, Gore, JM, Thompson, CA, Gurwitz JH: Recent magnitude of and temporal trends (1994–1997) in the incidence and hospital death rates of cardiogenic shock complicating acute myocardial infarction: The second National Registry of Myocardial Infarction. Am Heart J 2001; 141: 65. [ Links ]
2. Holmes DR Jr, Bates ER, Kleinman NS, et al: Contemporary reperfussion therapy for cardiogenic shock: The GUSTO–1 trial experience. Global Utilization of Streptokinase and Tissue Plasminogen Activator for Occluded Coronary Arteries. J Am Coll Cardiol 1995; 26: 668. [ Links ]
3. Holmes DR Jr, Berger PB, Hochman, JS et al: Cardiogenic shock in patients with acute ischemic syndromes with and without ST–segment elevation. Circulation 1999; 100: 2067. [ Links ]
4. Goldberg RJ, Gore JM, Alpert JS, et al: Cardiogenic shock after acute myocardial infarction. Incidence and mortality from a community wide perspective, 1975–1988. N Engl J Med 1991; 325:1117. [ Links ]
5. Hasdai D, Harrington RA, Hochman JS, et al: Platelet glycoprotein IIb/IIIa blockade and outcome of cardiogenic shock complicating acute coronary syndromes without persistent ST–segment elevation. J Am Coll Cardiol 2000; 36: 685. [ Links ]
6. Hands ME, Rutherford JD, Muller JE, et al: The in–hospital development of cardiogenic shock after myocardial infarction: Incidence, predictors of occurrence, outcome and prognostic factors. J Am Coll Cardiol 1989; 14: 40. [ Links ]
7. Hochman JS, Sleeper LA, White HD, et al: One–year survival following early revascularization for cardiogenic shock. JAMA 2001; 285: 190 192. [ Links ]
8. Giri S, Mitchel J, Azar RR, et al: Results of primary percutaneous transluminal coronary angioplasty plus abciximab with or without stenting for acute myocardial infarction complicated by cardiogenic shock. Am J Cardiol 2002; 89: 126. [ Links ]
9. Chan AW, Chew DP, Bhatt DL, et al: Long–term mortality benefit with the combination of stents and abciximab for cardiogenic shock complicating acute myocardial infarction. Am J Cardiol 2002; 89: 132. [ Links ]
10. Antman EM, Anbe DT, Armstrong PW, et al: ACC/AHA guidelines for the management of patients with ST–elevation myocardial infarction–executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). Circulation 2004; 110: 588. [ Links ]
11. Webb JG, Sanborn TA, Sleeper ScD, Carere RG, Buller CE, Slater JN, et al: Percutaneous coronary intervention for cardiogenic shock in the SHOCK Trial Registry. Am Heart J 2001; 141: 964–70. [ Links ]
12. Hochman JS: Cardiogenic shock complicating acute myocardial infarction. Expanding the paradigm. Circulation 2003; 107: 2998–3002. [ Links ]
13. Martínez–Ríos MA, Rosas M, González H, et al: Relevance of the combined TIMI flow/perfusion index to effective assessment of reperfussion regimens with or without tirofiban in ST–elevation myocardial infarction. Insights from SASTRE–STEMI study, a randomized clinical trial. Am J Cardiol 2004; 93: 280–287. [ Links ]
14. Montalescot G, Borentain M Payot L, et al :Early vs late administration of glycoprotein IIb/ IIIa inhibitors in primary percutaneous coronary intervention of acute ST–segment elevation myocardial infarction. A meta–analysis. JAMA 2004; 292:362–66. [ Links ]
15. Gorog DA, Foale RA, Malik I: Distal myocardial protection during percutaneous coronary intervention. When and where? J Am Coll Cardiol 2005; 46: 1434–45. [ Links ]
16. Beranek JT: C–reactive protein and complement in myocardial infarction and postínfarction heart failure. Eur Heart J 1997; 18: 1834–1836. [ Links ]
17. Mathey D, Schofer J, Schafer HJ, Hamdoch T, Joachim HC, Ritgen A. Early accumulation of the terminal complement–complex in the ischaemic myocardium after reperfussion. Eur Heart J 1994; 15: 418 423 [ Links ]
18. Mahaffey KW, Granger CB, Nicolau JC, Ruzyllo W, Weaver WD, Theroux P, et al: Effect of Pexelizumab, an anti–C5 complement antibody, as adjunctive therapy to fíbrinolisis in acute myocardial infarction. The COMPLY Trial. Circulation 2003; 108: 1176–83. [ Links ]
19. Pexelizumab, an anti–C5 complement antibody, as adjunctive therapy to primary percutaneous coronary intervention in acute myocardial infarction. The COMMA Trial. Circulation 2003; 108: 1184–90. [ Links ]
20. Cotter G, Kaluski E, Milo O, Blatt A, Salah A, Hendler A, et al: LINCS: L–NAME (a NO synthase inhibitor) in the treatment of refractory cardiogénico shock. A prospective randomized study. Eur Heart J 2003; 24: 1287–95. [ Links ]
21. The Hypothermia after Cardiac Arrest Study Group. Mild Therapeutic Hypothermia to Improve the Neurologic Outcome after Cardiac Arrest. N Engl J Med 2002; 346: 549–556. [ Links ]
22. Ross AM, Gibbons RJ, Stone GW, Kloner RA, Alexander RW for the AMISTAD–II Investigators A Randomized, Double–Blinded, Placebo–Controlled Multicenter Trial of Adenosine as an Adjunct to Reperfiission in the Treatment of Acute Myocardial Infarction (AMISTAD–II). J Am Coll Cardiol 2005; 45: 1775–80. [ Links ]
23. The CREATE–ECLA Trial Group Investigators*. Effect of Glucose–Insulin–Potassium Infusion on Mortality in Patients With Acute ST–Segment Elevation Myocardial Infarction: The CREATE–ECLA Randomized Controlled Trial. JAMA 2005; 293: 437–446. [ Links ]
24. Kloner RA, Rezkalla SH: Cardiac protection during acute myocardial infarction: where do we stand in 2004? J Am Coll Cardiol 2004; 44: 276–86. [ Links ]
25. Dimmeler S, Zeiher AM: Wanted! The best cell for cardiac regeneration. J Am Coll Cardiol 2004; 44: 464–466. [ Links ] ]]>