Trastornos de coagulación en el cirrótico
Coagulation disorders in cirrhosis
Felix I. Téllez-Ávila,* Norberto C. Chávez-Tapia,* Aldo Torre-Delgadillo*
* Departamento de Gastroenterología. Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán.
]]> Reimpresos:
Recibido el 5 de octubre de 2006. ]]> Aceptado el 8 de marzo de 2007.
ABSTRACT
The liver plays a central role in the clotting process. In this organ are sintetizated the major part of the coagulation factors. Historically, was considered that alteration in liver function causes important bleeding disorders. However, actual evidence is not in agreement with this asseveration. Decreased synthesis of clotting and inhibitor factors, decrease clearance of activated factors, quantitative and qualitative platelet defects, hyperfibrinolysis and intravascular coagulation are some of the defects observed in liver diseases. Thrombotic events, even if rare in cirrhotic patients, occur manly in the portal and mesenteric veins. The aim of the present work is to review the present evidence in coagulation disorders and liver disease.
Key words. Cirrhosis. Coagulation.
RESUMEN
El hígado participa de manera importante en el proceso de la coagulación. En él se sintetizan la mayor parte de los factores pro- y anticoagulantes. De manera histórica se ha considerado que las alteraciones en la función de este órgano provoca trastornos predisponentes para eventos de sangrado. La evidencia actual pone en tela de juicio esta aseveración. En los casos de hepatopatía se hacen evidentes alteraciones en el número y funcionamiento de las plaquetas, disminución de la síntesis de factores de la coagulación, disfibrinogenemia, alteraciones en la fibrinólisis, deficiencia de vitamina K y cambios similares a los ocurridos en la coagulación intravascular diseminada (CID). El presente trabajo está dirigido a revisar los conocimientos actuales respecto a las alteraciones de la coagulación presentes en los pacientes con hepatopatías.
Palabras clave. Cirrosis. Coagulación.
]]> INTRODUCCIÓN
El hígado tiene un papel clave en el proceso de la coagulación, ya que representa el órgano en el cual se sintetizan la mayoría de los factores de la coagulación así como sus inhibidores. Por años se ha considerado que alteraciones en el funcionamiento del hígado provocan, a su vez, repercusiones en la coagulación que pueden llegar a poner en riesgo la vida de los pacientes con algún padecimiento hepático.1 Es bien conocido que los pacientes con hepatopatías crónicas presentan de manera frecuente alteraciones en las pruebas de coagulación, así como episodios importantes de sangrados principalmente de origen gastrointestinal. El asociar estos dos fenómenos como causa-efecto ha sido históricamente un fenómeno "natural". Debido a que las pruebas de coagulación disponibles en la actualidad miden la actividad in vitro y no in vivo1 de la coagulación, así como otros factores que se describirán a continuación, actualmente se cuestiona la importancia clínica de los defectos observados en los pacientes cirróticos.2,3 Las alteraciones de la hemostasia en los pacientes cirróticos se pueden observar a varios niveles en donde se involucran factores tanto procoagulantes como anticoagulantes: alteraciones en el número y funcionamiento de las plaquetas, disminución de la síntesis de factores de la coagulación, disfibrinogenemia, alteraciones en la fibrinólisis, deficiencia de vitamina K y cambios similares a los ocurridos en la coagulación intravascular diseminada (CID).
El objetivo de este trabajo, más que realizar una disertación, es presentar al lector las evidencias actuales sobre las alteraciones en los factores involucrados en el proceso de la coagulación en los pacientes con hepatopatía crónica.
ALTERACIONES PLAQUETARIAS
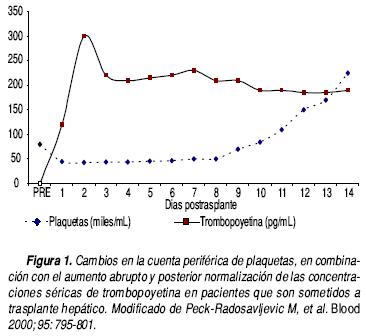
La trombocitopenia es una alteración común en pacientes cirróticos. Se reporta con una frecuencia entre 30-64% de este grupo de pacientes.4 La cifra generalmente es mayor de 30,000 plaquetas/mm3 y no se asocia de manera frecuente con sangrados espontáneos. Se acepta que la causa de esta disminución de las cifras plaquetarias en los pacientes con cirrosis es debido a la esplenomegalia, la cual a su vez, en este grupo de pacientes es secundaria a hipertensión portal. A pesar de esta disminución en la cuenta periférica de plaquetas, la cifra total puede ser incluso normal y encontrarse hasta 90% del total secuestradas en el bazo, se sabe que a pesar de ello, estas plaquetas son capaces de participar de manera activa en el proceso de hemostasia. A pesar de lo anterior, no se ha podido demostrar una asociación entre las dimensiones del bazo y la disminución en la cuenta plaquetaria. La descompresión del sistema portal por cualquier método (quirúrgico o espontáneo) no corrige esta alteración,5 por otro lado existen estudios en pacientes con cirrosis por virus C que demuestran que por medio de la embolización esplénica parcial con microesferas es posible aumentar las cifras plaquetarias en sangre periférica;6,7 se debe mencionar que hasta el momento se trata de estudios retrospectivos con un número de pacientes pequeño. El factor que parece tener mayor importancia es la disminución de la producción de trombopoyetina (TPY), la cual es una citocina producida en el hígado. La TPY es responsable de la maduración de los megacariocitos y de la formación de plaquetas maduras. Los niveles de esta citocina se encuentran disminuidos en pacientes con hepatopatía crónica8 y se ha observado que posterior al trasplante hepático sus cifras séricas aumentan de manera paulatina con la consecuente elevación de las cifras plaquetarias9 (Figura 1). En un estudio realizado en pacientes con fibrosis/cirrosis por VHC tratados con interferón pegilado10 se evaluó la respuesta de las cifras plaquetarias y de TPY en aquellos con respuesta viral sostenida, se demostró que las cifras plaquetarias aumentaron de 15.5 ± 6.8 x 104 a 19.9 ± 5.8 xlO4 (p < 0.01); las cifras de TPY aumentaron de 1.65 ± 0.94 a 2.06 ± 1.22 fmol/mL (p = 0.073). Estos resultados son consistentes con datos obtenidos en otros estudios recientes.11 Los datos anteriores sugieren que en los pacientes cirróticos la disminución de la TPY secundaria a la disfunción hepática es responsable, al menos en parte, de la trombocitopenia observada. Otros factores estudiados en las alteraciones plaquetarias son la destrucción por mecanismos inmunológicos,12 deficiencia de ácido fólico13 y el uso de alcohol.14 La coexistencia de coagulación intravascular diseminada, sepsis, falla hepática aguda y situaciones específicas como el síndrome HELLP (hemolisis, elevación de enzimas hepáticas y plaquetas bajas) pueden contribuir a las alteraciones mencionadas.

DISMINUCIÓN DE LA SÍNTESIS DE FACTORES DE COAGULACIÓN
]]> El hígado es el órgano encargado de la síntesis de la mayoría de los factores de coagulación (Cuadro 1). Clásicamente se ha relacionado la disminución de los factores de la coagulación con la gravedad del daño hepático y pronóstico de las enfermedades hepáticas. Las pruebas utilizadas actualmente para la medición de la actividad de los factores de la coagulación representan una actividad "in vitro" y no "in vivo", que sólo se ven alteradas cuando los niveles plasmáticos de los factores procoagulantes están por debajo de 30-40% de sus cifras normales. La medición de cada uno de los factores de manera independiente ha mostrado ser útil en algunas situaciones especiales. Los criterios del King's Collage para falla hepática fulminante refieren al TP mayor de 100 como un predictor importante de mortalidad, sin importar la etiología.15 La disminución de la cantidad de factor V, con cifras totales menores a 20% (menores de 30 años) y 30% (mayores de 30 años) del normal, se han utilizado como criterio de trasplante hepático en pacientes con falla hepática fulminante y encefalopatía hepática grados 3-4.16El TP se encuentra sin alteraciones o ligeramente prolongado en los estadios tempranos de la enfermedad hepática. A medida que avanza la enfermedad la importante disminución de los factores de la vía extrínseca (principalmente el factor VII) se ven reflejados en el alargamiento del TP. Con el mayor avance de la enfermedad, los factores XI y XII también se ven afectados, con lo cual se puede observar una afección manifestada con alargamiento del tiempo parcial de tromboplastina (TTP).17 El TP es utilizado en varios modelos pronósticos de la gravedad de la hepatopatía (Child-Pugh, Mayo End-Stage Liver Disease [MELD]).18-19 El INR (International Normalized Ratio, razón normalizada internacional) se incluye en varios modelos de evaluación de gravedad y pronóstico de las enfermedades hepáticas como los mencionados. Este parámetro se creó para disminuir la variabilidad de los resultados obtenidos entre los pacientes tratados con anticoagulantes orales cuando la medición se realiza en diferentes laboratorios con distintos reactivos. Hasta el momento no se ha validado el uso de INR en lugar del TP en pacientes con hepatopatía crónica.20,21 Algunos factores de coagulación pueden encontrarse con cifras normales o inclusive elevadas en el transcurso de una enfermedad hepática crónica. El factor VIII y el fibrinógeno debido a su síntesis extrahepática, disminución de su depuración hepática o bien, al ser reactantes de fase aguda, se encuentran en esta circunstancia.
Inhibidores habituales de la coagulación sintetizados en el hígado como antitrombina III (AT III), la proteína C y la proteína S se encuentran en niveles séricos por debajo de lo normal en las enfermedades hepáticas crónicas.22 En general estas alteraciones no se manifiestan como episodios de trombosis. Se piensa que lo anterior es consecuencia de un estado de "balance" al cual llegan estos pacientes al disminuir tanto los factores pro- como los anticoagulantes. Existen estudios que exponen datos contrarios a esta situación, Northup, et al.23 en un estudio de casos-controles realizado en pacientes cirróticos encontró una prevalencia de 0.5% de trombosis venosa profunda y tromboembolia pulmonar. La albúmina se documentó como marcador útil para riesgo de trombosis independientemente de las cifras plaquetarias e INR.
DISFIBRINOGENEMIA
La polimerización anormal de los monómeros de fibrina es una anormalidad presente en 60-70% de los pacientes con cirrosis.24 Esta polimerización deficiente se observa aun con cifras de TP, TTP y fibrinógeno normales. La disfibrinogenemia vista en los pacientes con cirrosis es un fenómeno reversible secundaria a un aumento en la actividad de la enzima sialiltransferasa debido a la reexpresión del gen fetal en los hepatocitos.25 El resultado es una cantidad excesiva de residuos de ácido siálico en la molécula de fibrinógeno que interfiere con la actividad enzimática de la trombina.25
HIPERFIBRINÓLISIS
Los pacientes con cirrosis se encuentran en un estado persistente de hiperfibrinólisis. Los estudios habituales como el TP y TTP no son capaces de detectar esta alteración. La disminución del tiempo de lisis de euglobina, aumento de dímero-D y otros productos de degradación de la fibrina, así como el aumento del activador tisular del plasminógeno en los pacientes cirróticos son marcadores de la presencia de esta alteración. El inhibidor del activador del plasminógeno, α2-antiplasmina y el inhibidor de la fibrinólisis activable por trombina se encuentran en cifras normales o por debajo de su nivel normal.26,27 El origen de este trastorno en pacientes con hepatopatía avanzada se desconoce hasta el momento. Algunos autores proponen a la permeación de ascitis hacia el torrente circulatorio como factor etiológico;28 sin embargo, existen controversias al respecto.29 El desarrollo de un estado de hiperfibrinólisis en los pacientes con ascitis sometidos a derivación del líquido ascítico hacia la circulación general apoya el concepto. Otro dato importante a favor del probable papel etiológico de la ascitis es que la hiperfibrinólisis se encuentra presente en 93% de los pacientes con ascitis comparado con 33% presente en pacientes con cirrosis sin ascitis.28 La traslocación bacteriana con presencia en el torrente sanguíneo de bacterias provenientes del tubo digestivo es otra de las probables etiologías.29 La trascendencia clínica de estos trastornos sobre la tendencia al sangrado no está claramente establecida.
]]> DEFICIENCIA DE VITAMINA K
Esta alteración no es secundaria a la patología de base, pero se encuentra frecuentemente asociada con la hepatopatía crónica. La desnutrición y la mala absorción de esta vitamina liposoluble son los principales factores asociados. La vitamina K requiere de sales biliares para su absorción, por lo cual la colestasis intra- o extrahepática puede afectar la misma. Los factores II, VII, IX y X, así como las proteínas C y S requieren de la presencia de vitamina K para su síntesis y función adecuadas. La vitamina K es un cofactor para la γ-carboxilación de los residuos de ácido glutámico en la región amino terminal. Los residuos γ-carboxilados permiten la unión de los iones calcio los cuales son esenciales para la adecuada actividad funcional de estos factores dependientes de vitamina K. En la hepatopatía crónica, se observan niveles detectables de precursores descarboxilados de los factores K dependientes (PIVKA, por sus siglas en inglés, precursors induced by vitamin K absence), lo anterior en consistencia con lo expuesto.30 La protrombina descarboxilada es posible detectarla en altas cantidades en pacientes con hepatocarcinoma, la cual es idéntica desde el punto antigénico a la presente en pacientes que reciben tratamiento con anticoagulantes orales. Esta molécula ha sido postulada como un marcador tumoral del carcinoma hepatocelular.31
COAGULACIÓN INTRAVASCULAR DISEMINADA (CID)
La cirrosis descompensada comparte algunas anormalidades de la coagulación con el patrón observado en la CID. Lo anterior ha llevado a postular un estado persistente de CID de bajo grado en estos pacientes.32 Este concepto es materia de serias controversias.33 Nuevos estudios de laboratorio como la determinación de los fragmentos de protrombina F1 + 2, fibrinopéptido A, fibrina soluble, dímero-D, complejo trombina-antitrombina, entre otros, permitieron el reconocimiento de una coagulación intravascular acelerada y fibrinólisis (CIAF) en los pacientes con cirrosis.34 Esta CIAF no es parte de la cirrosis "estable", pero se observa hasta en 30% de los pacientes con cirrosis descompensada y se asocia con el grado de gravedad de la enfermedad.33 El diagnóstico de CID en los pacientes cirróticos es de especial dificultad y se basa en la presencia de un evento desencadenante, deterioro progresivo del paciente, reducción desproporcionada de factor V y disminución de factor VIII (previamente normal).
TROMBOSIS
Las alteraciones de la coagulación en pacientes con cirrosis se manifiestan generalmente por eventos de sangrado. No obstante, la presencia de complicaciones trombóticas a diferentes niveles es un fenómeno bien reconocido en pacientes con hepatopatía crónica.35 La localización más frecuente de trombosis en los pacientes cirróticos es la vena porta y las venas mesentéricas. La prevalencia de trombosis portal no neoplásica oscila de 8 a 16%.36 Entre los factores etiológicos propuestos para este estado protrombótico se encuentran la estasis provocada por la hipertensión portal y algunos de origen genético no relacionados desde el punto de vista etiológico con la hepatopatía, como alteraciones en el factor V37 y la mutación G20210A en la protrombina.38,39
En las figuras 2 y 3 se ilustran los diferentes mecanismos involucrados en los trastornos de coagulación en los pacientes cirróticos, así como el "balance" alcanzado.
]]>

TRATAMIENTO
El sangrado espontáneo no relacionado con hipertensión portal es un fenómeno poco común en los pacientes cirróticos a pesar de las alteraciones mencionadas. El tratamiento de los trastornos en la coagulación en los pacientes cirróticos se encuentra justificado sólo en situaciones específicas: sangrado activo persistente, antes de procedimientos diagnósticos o de tratamiento invasivos y estados prequirúrgicos. Los productos disponibles para la corrección de estas alteraciones incluyen derivados hematológicos y no hematológicos.
El plasma fresco congelado (PFC) contiene todos los factores e inhibidores de la coagulación. La dosis recomendada es de 10-20 mL/kg peso. El efecto del PFC es de inicio rápido, pero dura un máximo de 12-24 horas. La administración está indicada en casos de sangrado persistente para lograr un INR por debajo de 240 o para corregir el TP por arriba de cuatro segundos.41 Cuando no corrigen los tiempos de coagulación a pesar de la administración adecuada de PFC se debe considerar la posibilidad de CID. En ocasiones, la cantidad necesaria de PFC podría ser considerada como contraindicada en algunos pacientes con sangrado variceal activo, ya que en este grupo de pacientes se considera manejarlos con una "hipotensión permisiva", por el riesgo de persistencia o mayor cantidad de sangrado al aumentar la presión en el flujo portal.42 Por otro lado, no debe ignorarse el riesgo de infecciones trasmitidas por este medio así como otras complicaciones secundarias a su administración.43
El uso de crioprecipitados se justifica en los casos de CID con un fibrinógeno menor de 100 mg/dL. Se recomienda utilizar una unidad de crioprecipitado por cada 10 kg de peso, con lo cual se espera un incremento aproximado de 50 mg/dL. Los crioprecipitados contienen factor VIII, fibrinógeno, vWF, fibronectina y factor XIII. En pacientes en los cuales el manejo de líquidos es un problema, el uso de crioprecipitados parece ser una alternativa útil.44
El uso de factor VII recombinante representa actualmente una alternativa prometedora en los pacientes con cirrosis.45 Existen estudios donde el uso de factor Vila ha mostrado reducir la necesidad de paquetes globulares en pacientes sometidos a trasplante hepático,46 reduce la intensidad del sangrado en pacientes con trasplante hepático complicado47 y en pacientes con sangrado variceal agudo;48 en casos de falla hepática fulminante ha demostrado ser de utilidad para la corrección de la coagulopatía.49 No obstante lo anterior, la evidencia de su utilidad clínica real aún no se encuentra clara.21,50
La transfusión de plaquetas se encuentra justificada sólo en ciertos escenarios. Su uso profiláctico sólo se justifica en pacientes que serán sometidos a algún procedimiento invasivo y cifras menores de 60,000/mm3. Un concentrado plaquetario incrementa la cuenta periférica aproximadamente en 10,000/ mm3. La dosis recomendada es un concentrado por cada 10 kg/peso.51
]]> La deficiencia de vitamina K en el paciente cirrótico no es consecuencia directa de la enfermedad hepática. En casos donde se encuentra asociada a la misma, la administración de 30 mg de vitamina K en una sola dosis o dividida en tres diferentes puede corregir el TP. La administración intravenosa tiene efecto rápido (6-8 horas). La administración subcutánea no tiene una absorción uniforme por lo cual no se recomienda. Existen presentaciones para su administración oral como el bifosfato de menadiol.Agentes antifibrinolíticos como la protinina, el ácido epsilon aminocaproico y ácido tranexámico han sido utilizados en estos pacientes. Su mecanismo de acción es por medio de la inhibición de la activación del plasminógeno y la actividad de la plasmina. Estos medicamentos han probado reducir las pérdidas sanguíneas y los requerimientos transfusionales durante las cirugías de hígado y el trasplante hepático.52,54
REFERENCIAS
1. Tripodi A, Salermo F, Chantarangkul V, Clerici M, Cazzaniga M, Primignani M, Manucci PM. Evidence of normal thrombin generation in cirrhosis despite abnormal conventional coagulation tests. Hepatology 2005; 41(3): 553-8. [ Links ]
2. Mannucci PM. Abnormal hemostasis tests and bleeding in chronic liver disease: are they related? No. J Thromb Haemost 2006; 4(4): 721-3. [ Links ]
3. Reverter JC. Abnormal hemostasis tests and bleeding in chronic liver disease: are they related? Yes. J Thromb Haemost 2006; 4(4): 717-20. [ Links ]
4. Bashour FN, Teran JC, Mullen KD. Prevalence of peripheral blood cytopenias (hypersplenism) in patients with nonalcoholic chronic liver disease. Gastroenterology 2000; 95(10): 2936-9. [ Links ]
5. Karasu Z, Gurakar A, Kerwin B, et al. Effect of transjugular intrahepatic portosystemic shunt on thrombocytopenia associated with cirrhosis. Dig Dis Sci 2000; 45(10): 1971-6. [ Links ]
6. Palsson B, Verbaan H. Partial splenic embolization as pretreatment for antiviral therapy in hepatitis C virus infection. Eur J Gastroenterol Hepatol 2005; 17(11): 1153-5. [ Links ]
7. Foruny JR, Blazquez J, Moreno A, Bercena A, et al. Safe use of pegylated interferon/ribavirin in hepatitis C virus cirrhotic patients with hypersplenism after partial splenic embolization. Eur J Gastroenterol Hepatol 2005; 17(11): 1157-64. [ Links ]
8. Kawasaki T, Takeshita A, Souda K, et al. Serum thrombopoietin levels in patients with chronic hepatitis and liver cirrhosis. Am J Gastroenterol 1999; 94(7): 1918-22. [ Links ]
9. Peckradosavljevic M, Wichlas M, Zacherl J, et al. Thrombopoietin induces rapid resolution of thrombocytopenia after orthotopic liver transplantation through increased platelet production. Blood 2000; 95(3): 795-801. [ Links ]
10. Yagura M, Tanaka A, Tokita H, Kamitsukasa H, Harada H. Factors regarding increase of platelet counts in chronic hepatitis C patients with sustained virological response to interferon-Relation to serum thrombopoietin levels. Hepatol Res 2005; 33(3): 211-5. [ Links ]
11. Rios R, Sangro B, Herrero I, Quiroga J, Prieto J. The role of thrombopoietin in the thrombocytopenia of patients with liver cirrhosis. Am J Gastroenterol 2005; 100(6): 1311-16. [ Links ]
12. Samuel H, Nardi M, Karpatkin M, Hart D, Belmont M, Karpatkin S. Differentiation of autoimmune thrombocytopenia from thrombocytopenia associated with immune complex disease: systemic lupus erythematosus, hepatitis-cirrhosis, and HIV-1 infection by platelet and serum immunological measurements. Br J Haematol 1999; 105(4): 1086-91. [ Links ]
13. Peltz S. Severe thrombocytopenia secondary to alcohol use. Postgrad Med 1991; 89(6): 75-6, 85. [ Links ]
14. Latvala J, Parkkila S, Niemela O. Excess alcohol consumption is common in patients with cytopenia: Studies in blood and bone marrow cells. Alcohol Clin Exp Res 2004; 28(4): 619-24. [ Links ]
15. O'Grady JG, Alexander GJM, Hayllat KM, et al. Early indicators of prognosis in fulminant hepatic failure. Gastroenterology 1989; 97: 439-45. [ Links ]
16. Bismuth H, Samuel D, Castaing D, et al. Orthotopic liver transplantation and subfulminant hepatitis. The Paul Brousse experience. Ann Surg 1995; 222: 109-19. [ Links ]
17. Paramo JA, Rocha E. Hemostasis in advanced liver disease. Semin Thromb Hemost 1993; 19: 184-90. [ Links ]
18. Pugh RNH, Murray-Lyon IM, Dawson JL, et al. Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 1973; 60: 646-9. [ Links ]
19. Forman LM, Lucey MR. Predicting the prognosis of chronic liver disease: an evolution from child to MELD. Mayo end-stage liver disease. Hepatology 2001; 33: 473-5. [ Links ]
20. Rovert A, Chazouilleres O. Prothrombin time in liver failure: time, ratio, activity percentage, or international normalized ratio? Hepatology 1996; 24: 1392-4. [ Links ]
21. Ramsey G. Treating coagulopathy in liver disease with plasma transfusions or recombinant factor Vila: an evidence-based review. Best Pract Res Clin Haematol 2006; 19(1): 113-26. [ Links ]
22. Amitrano L, Guardascione MA, Brancaccio V, Balzano A. Coagulation disorders in liver disease. Semin Liver Dis 2002; 22(1): 83-96. [ Links ]
23. Northup PG, McMahon MM, Ruhl AP, Altschuler SE, Volk-Bednarz A, Caldwell SH, Berg CL. Coagulopathy does not fully protect hospitalized cirrhosis patients from peripheral venous thromboembolism. Am J Gastroenterol 2006; 101(7): 1524-8. [ Links ]
24. Drin FG, Thomson JM, Dymock IW, et al. Abnormal fibrin polymerization in liver disease. Br J Haematol 1976; 34: 427-37. [ Links ]
25. Narvaiza MJ, Fernandez J, Cuesta B, Paramo JA, Rocha E. Role of sialic acid in acquired dysfibrinogenemia associated with liver cirrhosis. Ric Clin Lab 1986; 16(4): 563-8. [ Links ]
26. Van Thiel DH, George M, Fareed J. Low levels of thrombin activatable fibrinolysis inhibitor (TAFI) in patients with chronic liver disease. Thromb Haemost 2001; 85: 667-70. [ Links ]
27. Colucci M, Binetti BM, Branca MG, Clerici C, Morelli A, Semeraro N, Gresele P. Deficiency of thrombin activatable fibrinolysis inhibitor in cirrhosis is associated with increased plasma fibrinolysis. Hepatology 2003; 38(1): 230-7. [ Links ]
28. Agarwal S, Joyner KA Jr, Swaim MW. Ascites fluid as a possible origin for hyperfibrinolysis in advanced liver disease. Am J Gastroenterol 2000; 95(11): 3218-24. [ Links ]
29. Piscaglia F, Donati G, Giannini R, Bolondi L. Liver cirrhosis, ascites, and hyperfibrinolysis. Am J Gastroenterol 2001; 96(11): 3222. [ Links ]
30. Blanchard RA, Furie BC, Jorgensen M, et al. Acquired vitamin K dependent carboxylation deficiency in liver disease. N Engl J Med 1981; 305: 242-8. [ Links ]
31. Nakamura S, Nouso K, Sakaguchi K, Ito YM, Ohashi Y, Kobayashi Y, et al. Sensitivity and specificity of Des-Gamma-Carboxy Prothrombin for Diagnosis of Patients with Hepatocellular Carcinomas Varies According to Tumor Size. Am J Gastroenterol 2006; 101: 1-6. [ Links ]
32. Violi F, Ferro D, Basili S, et al. Association between low grade disseminated intravascular coagulation and endotoxemia in patients with liver cirrhosis. Gastroenterology 1995; 109: 531-9. [ Links ]
33. Ben-Ari Z, Osman E, Hutton RA, Burroughs AK. Disseminated intravascular coagulation in liver cirrhosis: fact or fiction? Am J Gastroenterol 1999; 94(10): 2977-82. [ Links ]
34. Joist JH. AICF and DIC in liver cirrhosis: Expressions of a hypercoagulable state. Am J Gastroenterol 1999; 94: 2801-3. [ Links ]
35. Northup PG, McMahon MM, Ruhl AP, Altschuler SE, Volk-Bednarz A, Caldwell SH, Berg CL. Coagulopathy does not fully protect hospitalized cirrhosis patients from peripheral venous thromboembolism. Am J Gastroenterol 2006; 101(7): 1524-8. [ Links ]
36. Yerdel MA, Gunson B, Mirza D, et al. Portal vein thrombosis in adults undergoing liver transplantation: risk factors, screening, management, and outcome. Transplantation 2000; 69: 1873-81. [ Links ]
37. Erkan O, Bozdayi AM, Disibeyaz S, Oguz D, Ozcan M, Bahar K, et al. Thrombophilic gene mutations in cirrhotic patients with portal vein thrombosis. Eur J Gastroenterol Hepatol 2005; 17(3): 339-43. [ Links ]
38. Amitrano L, Guardascione MA, Ames PR, Margaglione M, Iannaccone L, Brancaccio V, Balzano A. Increased plasma prothrombin concentration in cirrhotic patients with portal vein thrombosis and prothrombin G20210A mutation. Thromb Haemost 2006; 95(2): 221-3. [ Links ]
39. Walker AP. Portal vein thrombosis: what is the role of genetics? Eur J Gastroenterol Hepatol 2005; 17(7): 705-7. [ Links ]
40. Everson GT. A hepatologist's perspective on the management of coagulation disorders before liver transplantation. Liver Transplant Surg 1997; 3: 646-52. [ Links ]
41.Youssef WI, Salazar F, Dasarathy S, Beddow T, Mullen KD. Role of fresh frozen plasma infusion in correction of coagulopathy of chronic liver disease: a dual phase study. Am J Gastroenterol 2003; 98(6): 1391-4. [ Links ]
42. García-Tsao G. Current management of the complication of cirrhosis and portal hypertension: variceal hemorrhage, ascites, and spontaneous bacterial peritonitis. Gatroenterology 2001; 120: 726-48. [ Links ]
43. MacLennan S, Williamson LM. Risks of fresh frozen plasma and platelets. J Trauma 2006; 60(6 Suppl.): S46-S50. [ Links ]
44. French CJ, Bellomo R, Angus P. Cryoprecipitate for the correction of coagulopathy associated with liver disease. Anaesth Intensive Care 2003; 31(4): 357-61. [ Links ]
45. Bernstein D. Effectiveness of the recombinant factor Vila in patients with the coagulopathy of advanced child's B and C cirrhosis. Semin Thromb Hemost 2000; 26: 437-8. [ Links ]
46. Niemann CU, Behrends M, Quan D, Eilers H, Gropper MA, Roberts JP, Hirose R. Recombinant factor Vila reduces transfusion requirements in liver transplant patients with high MELD scores. Trans Med 2006; 16(2): 93-100. [ Links ]
47. Gala B, Quintela J, Aguirrezabalaga J, Fernandez C, Fragüela J, Suarez F, Gomez M. Benefits of recombinant activated factor VII in complicated liver transplantation. Transplant Proc 2005; 37(9): 3919-21. [ Links ]
48. Jimenez-Saenz M. Recombinant factor Vila for variceal bleeding: when, why, and how? Gastroenterology 2005; 128(4): 1150-1. [ Links ]
49. Pavese P, Bonadona A, Beaubien J, Labrecque P, Pernod G, Letoublon C, Barnoud D. FVIIa corrects the coagulopathy of fulminant hepatic failure but may be associated with thrombosis: a report of four cases. Can J Anaesth 2005; 52(1): 26-9. [ Links ]
50. Shao YF, Yang JM, Chau GY, Sirivatanauksorn Y, Zhong SX, Erhardtsen E, et al. Safety and hemostatic effect of recombinant activated factor VII in cirrhotic patients undergoing partial hepatectomy: a multicenter, randomized, double-blind, placebo-controlled trial. Am J Surg 2006; 191(2): 245-9. [ Links ]
51. Murphy MF, Wallington TB, Kelsey P, Boulton F, Bruce M, Cohen H, et al. British Committee for Standards in Haematology, Blood Transfusion Task Force. Guidelines for the clinical use of red cell transfusions. Br J Haematol 2001; 113(1): 24-31. [ Links ]
52. Porte RJ, Molenaar IQ, Begliomini B, et al. Aprotinin and transfusion requirements in orthotopic liver transplantation: a multicentre randomized double-blind study. EMSALT Study Group. Lancet 2000; 355: 1303-9. [ Links ]
53. Kang Y, Lewis JH, Navalgund A, et al. Epsilonaminocaproic for treatment of fibrinolysis during liver transplantation. Anesthesiology 1987; 66: 766-73. [ Links ]
54. Dalmau A, Sabate A, Acosta F, et al. Tranexamic acid reduces red cell transfusion better than epsilon-aminocaproic acid or placebo in liver transplantation. Anesth Analg 2000; 91: 29-34. [ Links ] ]]>