
Users' and providers' perspectives on technological procedures for 'normal' childbirth in a public maternity hospital in Salvador, Brazil
Perspectivas de usuarios y proveedores sobre procedimientos tecnológicos para el parto 'normal' en una maternidad pública de Salvador, Brasil
Cecilia McCallum, PhD; Ana Paula dos Reis, MSc
Institute of Collective Health, Federal University of Bahia. Salvador Bahia, Brazil
]]>
ABSTRACT
OBJECTIVE: To reveal the effect of cultural practices on the way in which normal birth is conducted in a public hospital in Brazil.
MATERIAL AND METHODS: This article about a public maternity hospital in Salvador, Brazil, compares the points of view of providers and users on four technological normal childbirth procedures: trichotomy, episiotomy, oxytocin infusion, and epidural analgesia. Fieldwork carried out from 2002 to 2003 combined qualitative and quantitative methods.
RESULTS: Institutional practices make childbirth unnecessarily difficult for women. Nonetheless, most women accept the conditions because the medical procedures make sense according to their cultural understandings. Service providers support the use of such procedures, although doctors are aware that they contradict recommendations found in scientific medical literature. This article argues that from the perspective of both providers and users, the technological procedures are infused with a culturally specific set of meanings and values.
CONCLUSIONS: Policymakers must address the cultural understandings of both users and health care professionals in order to improve maternal healthcare in public hospitals in Brazil.
Key words: obstetric delivery techniques; health services; culture; Brazil
RESUMEN
OBJETIVO: Revelar el efecto de las prácticas culturales en el parto normal en un hospital público en Brasil.
MATERIAL Y MÉTODOS: Este artículo sobre el parto en una maternidad pública de Salvador, Brasil, compara el punto de vista de los proveedores de servicios de salud y los usuarios de dichos servicios con respecto a cuatro procedimientos para el parto normal: tricotomía, episiotomía, infusión de oxitocina y analgésico epidural. La investigación, realizada entre 2002 y 2003, utilizó métodos cualitativos y cuantitativos. ]]>
RESULTADOS: La práctica institucional hace que el parto sea innecesariamente dificultoso para las mujeres, sin embargo, la mayoría de ellas aceptan las condiciones, porque los procedimientos médicos tienen sentido dentro de su comprensión cultural. Los proveedores de servicios apoyan el uso de los procedimientos, aunque los doctores están concientes de que están en contra de las recomendaciones estipuladas en la literatura médica científica. El artículo sostiene que desde el punto de vista de ambos, los proveedores de servicios y los usuarios, los procedimientos tecnológicos están cargados de significados y valores culturalmente específicos.
CONCLUSIONES: Para lograr mejorar los cuidados en las maternidades de los hospitales públicos del Brasil, los diseñadores de políticas deben tomar en consideración los entendimientos culturales tanto de los usuarios como de los profesionales de salud.
Palabras clave: parto obstétrico, técnicas; servicios de salud; cultura; Brasil
This article discusses childbirth practices in a public maternity hospital in Salvador, Brazil (population approximately 2.5 million).1 , 2 It compares the points-of-view of users ages 15 to 24 years and providers on four technological procedures for normal birth: trichotomy and episiotomy (routinely used), oxytocin infusion (frequently used), and epidural analgesia (rarely used). It shows that institutional usage shapes the physiology of birth to the detriment of women but that, nonetheless, most women comply with the procedures, which make sense according to their cultural understandings. Providers perpetuate usage although some (especially doctors) are aware that some aspects go against recommendations in the scientific medical literature. The article argues that from both providers' and users' perspectives, the technological procedures are infused with a culturally specific set of meanings and values. It concludes that policymakers must address the cultural understandings of both users and health care professionals in seeking to improve maternal healthcare in public hospitals in Brazil.
In such hospitals in Salvador most women give birth vaginally using low-tech procedures. The caesarean section rate in this sector varies between less than 10% and around 30%,3 unlike the 80% to 100% characteristic of the private sector.*,4 These figures reflect differences between racial populations with respect to the birth experience in the city: 80% of its population is low-income and negro [a category currently used by sociologists of race to encompass both the census terms preto (black) and pardo (brown)],5,6 so the clientele of each sector is, respectively, largely either black or white. Consequently, low-tech childbirth procedures are common for black women, whereas high-tech procedures are more common for white women.
A majority of these women are young. National census data show that between 1980 and 2000, the contribution of women aged 15 to 19 years to the fecundity rate in Brazil rose from 7.1% to 19.4%.7,8 In 1998, 58.8% of live births in public hospitals in the northeast region (composed of nine states, including Bahia) were to women aged 10 to 24, and in Salvador, the public maternity wards admit more women aged 15 to 24 than in any other age category.9 In the facility studied, approximately half of all births are to women aged 15 to 24.
Material and Methods
]]> The facility studied is an important public maternity and teaching hospital, with 80 beds and roughly 8 000 admissions annually (according to hospital records for 2003). Over half of the admissions are for spontaneous births. The caesarean rate is less than 25%. The facility studied is a referral center for high-risk pregnancies, although it only has intensive care for premature babies and not for women. The Obstetric Center (OC) is comprised of two wards: one has five beds and the other has four. There are two delivery rooms: one has three obstetric beds and the other has one. Two rooms are equipped for performing surgeries. There is a small unit with six cribs where newborns are observed for about an hour after delivery.Research at the facility studied combined quantitative and qualitative methods to obtain a broad view of the institution and of providers and the young patients. A social anthropologist (aided by the senior researcher and four assistant researchers) carried out participant observation in the hospital between March 2002 and March 2003. To obtain information on the patients' perspectives, the team recorded semi-structured interviews with women aged 15 to 24, including 26 interviews with women who had recently given birth at the hospital. The interviews generally took place in the women's homes, lasting up to three hours. The research team observed WHO recommended ethical procedures approved by the Brazilian Ministry of Health's Ethical Committee, including obtaining informed consent and guaranteeing informant anonymity. Of 13 users interviewed aged 15 to 19, 10 were primipara, as were six of the 13 users aged 20 to 24. All births to these women were by vaginal delivery, except four caesarean deliveries. Eight user informants aged 15 to 19 were consensually married or in a steady relationship with their baby's father and five were single. Ten of the users aged 20 to 24 were consensually married, one was widowed during pregnancy, and two were single. Table I summarizes the socio-economic characteristics of user informants.

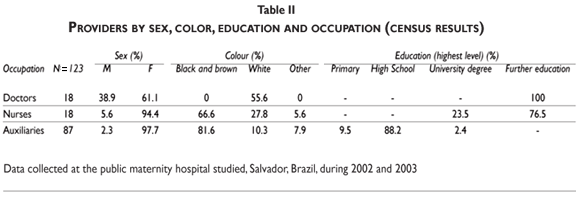
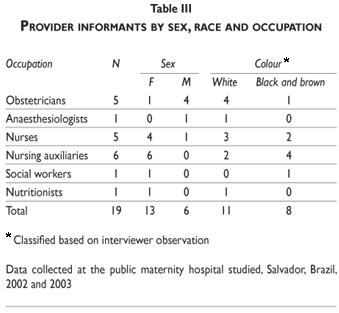
To obtain information on providers and their perspectives, the research team administered a structured questionnaire to 127 staff with formal links to the facility and who work directly with the young women. The total possible universe was 143. The response rate was 89% and there were seven refusals to participate and nine losses. Table II is a socio-economic profile of the census respondents. The field researcher also carried out in-depth interviews with 19 health care professionals (table III).
Results
In Salvador, women's first substantial contact with the medical world often occurs as a result of a first pregnancy. Thus, in 2002, 31% of all hospital admissions were for conditions requiring gynaecological intervention, especially childbirth, incomplete abortion or miscarriage.9 Admission to hospitals is particularly difficult for a woman in labor, for many reasons: Poor antenatal care does not prepare her; There is no guarantee of a bed (women often go to different hospitals until they are admitted); the hospital stay is also difficult because the model of the birth process employed by providers is dismissive of the psychological and social aspects of the birthing experience. The facility studied is dominated by the constant measuring of cervical dilation, which must be 4 to 5 cm to warrant admission. No companions are allowed in the OC, even for adolescent patients. Women are required to remain lying down, except when using the bathroom. The experience is characterized by physical discomfort and fear, especially of pain, and by strong feelings of abandonment, which increase as labor progresses.10
Because the facility studied is a teaching hospital, women sometimes undergo an excessive number of check-ups for cervical dilation. Progress should be marked on the partogram, though not all providers consult this every time. As in other public maternities in Salvador, data on the chart is rarely complete and little attention is paid to legibility.** The attending doctors or the obstetric nurse periodically check the baby's heartbeat with the aid of a pinard stethoscope or, occasionally, a portable electronic foetal detector. A woman is moved from the labor ward to the delivery room when her cervix is fully dilated and the baby has crowned. On a short delivery bed with stirrups for her feet, she lies on her back, her legs wide apart up in the air, her pelvis at the edge. In this position, she is encouraged to push the baby out. Some babies are delivered by an obstetrician or by an obstetric nurse, aided by a nursing auxiliary. Most often, a resident or a medical student presides.
The manner in which technology is employed in the Obstetric Center follows an established hierarchy, with senior doctors at the top and nursing auxiliaries at the bottom. The senior doctors are in charge of high-tech procedures. Aided by residents or other doctors, they perform caesarean sections and curettages, though residents sometimes preside. Residents and fourth or fifth year medical students trained in obstetrics perform most vaginal deliveries (and obstetic nurses if the presiding doctor is not opposed, as is common in Brazil).11,4 Occasionally, senior doctors perform low-tech deliveries. Nursing auxiliaries care for women in labor under the nurse's supervision. It is not uncommon for auxiliaries to deliver babies born accidentally in the labor ward. Sometimes, in their absence, women give birth alone.
Patients' and providers' views on this form of organizing childbirth differ in many respects. The idea that childbirth ought to occur in hospitals and not at home is an undisputed "fact" for our female informants. Home birth is thought of as old-fashioned and dangerous to the safety of both mother and child. Women prefer hospital birth because it allows them access to the professionals' technical skills and to birthing technology. They like having access to high-status obstetricians (especially young, good-looking white men). Informants also report some pleasure associated with the warm showers, free meals and clean clothes. The facility studied is valued as "hygienic" and "modern". One informant, for example, told us that she felt that the air in hospitals is "special", "different". She continued, "It is so much cleaner than the air at home. A baby born at home could become ill from infection, borne by the dirt in the air".
]]> Though ill prepared for hospital birth during antenatal exams, women have some knowledge of what to expect from friends and relatives. They know that they have to enter the hospital without family members or a partner to support them during labor. Stories heard at home, school or at work prepare primigravida women for the possibility that providers could be unfriendly or express disapproval of adolescent pregnancy through harsh comments, as elsewhere in Brazil.12Our research partially corroborated women's perceptions of providers. For example, Dr. Fernando (obstetrician) expressed little sympathy for patients, especially adolescents. He said:
A girl of fifteen is more unprepared to give birth than a woman of thirty. So the hysterical attack is always worse. It's a lack of emotional structure, really. In the fifteen year-old, instead of studying, she's giving birth! The third child, sometimes! But I think that it is not a thing about age, it's social class. It's a bit more inherent to the social class. I think the poorer people, the more ignorant ones, are not as curious as people who are more enlightened.
Dr. Fernando insisted that the women pretend to experience extreme pain rather than actually suffering it. In Brazilian culture, he explained, entry into motherhood is supposed to involve extreme suffering. For him, enabling emotional support of patients is peripheral to the true aim of medical practice. Like most providers at the facility studied, he says that his job is to come as close to technical perfection as possible, a good "outcome" for mother and baby. He thinks women singularly lack cooperation to this end.
However, Dr. Fernando's opinions about the women were not typical of the providers as a whole, among whom we found a range of attitudes (figure 1). Mauricio (obstetric nurse) told us:
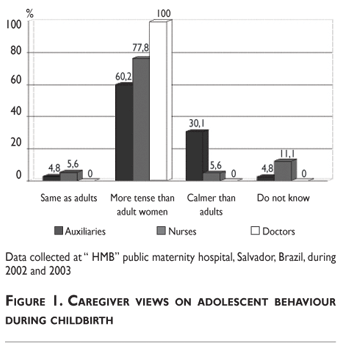
]]>
A woman generally comes here with the impression that she will suffer. Suffering really does happen, and sometimes it comes from some professionals who say certain things I think that in order to improve the experience of childbirth, a series of factors are involved [including] the adoption of a politics of humanization of childbirth.
Providers at the facility are not required to consider the psychological aspects of childbirth nor are they trained to deal with adolescents. Mauricio pointed out that institutional restrictions placed on them negatively affect women's experiences. They work under difficult conditions, including an atmosphere of suffering generated by constant moaning and screaming. Many complain about the low pay and some doctors see their work as "practically voluntary". They are pressured to deal with many patients at once, resulting in fatigue and stress, and they have little time to spend on pleasantries. Thus, tensions often surface when women scream or do not comply with the doctor's instructions. Standard technological procedures for normal birth at the facility substantially contribute to this scenario.
Three of these procedures are well known to women: trichotomy, intravenous infusion of oxytocin; and episiotomy. Epidural analgesia is not commonly known. They refer to trichotomy, which is routine at the facility, as either "shaving pubic hairs" or simply as "doing", and women fully comply with it. First-time mothers (based on advice from friends and relatives) shave themselves in the final weeks of pregnancy so as not to have to undergo shaving at the time of admission to hospital. Shaving oneself is also a means to facilitate relations with providers. One 22 year-old user told us:
My aunt used to say that I should do it beforehand. She said that when you go all hairy the doctors get mad. Sometimes when they do it themselves, they are brusque, they cut you. So I was scared. [I said to myself]: "You know what? I will do it at home! I will go ultra-clean!"
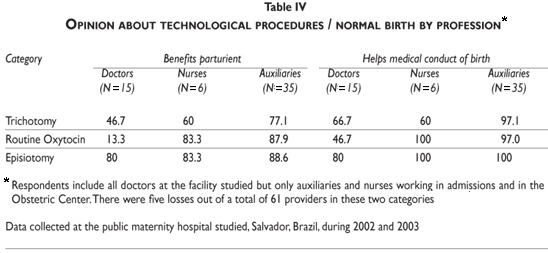
Thus trichotomy is understood by women to be a hygienic measure. Arriving "done", they make sure providers see them as clean, well-informed, modern urban dwellers; and they distance themselves from negative stereotypes associated with extreme poverty. Many providers interviewed, including the head of the Obstetric Center, consider trichotomy important for facilitating suture after episiotomy. In other words, they opt for it on technical grounds. As part of the census study, we asked 61 facility providers (those directly involved with childbirth and admission) their opinion about trichotomy (table IV). Fifty-six responded and five refused to comment on this and other procedures or declared that they had no opinion. Sixty-one percent of respondents thought that trichotomy benefits the parturient and 75% said that it helps the medical conduct of birth. The nursing auxiliaries were most enthusiastic in support of it, the doctors the least. The nurses occupy the middle ground.
Why the variation in responses? We suggest that the auxiliaries, and to a lesser extent the nurses, accept that institutional routine defines good practice, but also that they are strongly influenced by popular notions about hygiene. The obstetricians, on the other hand, are aware of the recommendations against the use of trichotomy in the medical literature and some felt moved to give the "correct" answer. Nevertheless, the in-depth interviews show that providers, like users, associate body hair, poverty and dirt. Paula (obstetric nurse) links a perceived "need" for trichotomy to class:
It's not for every patient. It depends on the clientele. It's not a question of discrimination, but the patient in a private hospital, she has a different kind of behavior. The patient who is poor, miserable, she does not know much about hygiene, about hospital infection. Our patient is a patient of a very low level, so the pubic hair is also a very big focus of infection. Pubic hair has a great deal of bacteria.
Paula added that nowadays the patients have "evolved" and so they arrive at the hospital shaven. Dr. Ester (obstetrician) also agreed that the facility's users live in a state of very poor hygiene, making trichotomy necessary. But Dr. Luis (obstetrician) disagrees. The women are misinformed, he says; they think that the pubic hairs interfere somehow in the expulsion of the baby. Mauricio noted that doctors following the consensus in the medical science literature see clipping the hairs as sufficient. He points out that some doctors prefer to disregard the literature. Mauricio and Cristina (nursing auxiliary) suggest that this preference results from prejudice towards patients.
Thus, trichotomy is a measure of respectability and hygiene for users and many providers. In Brazil, any body hair on women is seen as ugly and dirty, so this finding is not surprising. However, though the women think that shaving beforehand shows providers that they are clean and modern, many providers think of the women as the opposite: essentially "low level", as Paula put it. In other words, users' and providers' views regarding the users differ.
Obstetricians at the facility frequently speed up labor by applying an intravenous infusion of oxytocin, referred to by users as "soro" (literally, "saline solution") or as "that medicine they put in the soro". Informal interviews with users, corroborated by recorded interviews, indicated that women expect its use but fear its effects. They are often aware that it will speed up and strengthen contractions, but also increase pain. However, there was some resistance. Some spoke of secretly unhooking drips or neglecting to call the auxiliary when the soro finished. Others considered it necessary, telling of how they bore the increased pain bravely. Some expressed the suspicion that providers used oxytocin deliberately to make their pain worse, revealing a lack of confidence in the humaneness of their providers.
The increase of pain and discomfort attributed to oxytocin is addressed in the medical literature. WHO's review recommends caution in its use and suggests standing up and walking around as an effective alternative method for shortening labor.15 This has the added advantage of decreasing rather than increasing pain.16 We asked 56 providers working in the OC and in admissions whether oxytocin should be used routinely. Eighty-two percent said "no," yet when asked whether routine use of oxytocin benefits the parturient, 61% responded "yes" (table IV). However, 13 of the 16 doctors surveyed disagreed. The most enthusiastic in support of oxytocin application were the nurses and auxiliaries. These responses show that the doctors, divided on routine oxytocin use, tend to give the "correct" answer from a technical point-of-view. This does not, however, reflect reality in the OC, where the drug is administered routinely (except at night). Defending this usage, a senior medic insisted that WHO recommendations on oxytocin do not apply to public maternities in Brazil, pointing to difficulties related to the institutional "reality" and to the nature of the clientele. Dr. Alexandre (obstetrician) explained:
]]> Cristina (nursing auxiliary) explained that routine use occurs "to facilitate the increase of 'production'", adding that all doctors at the birth facility are subject to intense institutional pressure to get babies delivered fast, even those opposed to using it in every case.Oxytocin, like any medicament, has to be used according to certain criteria. It cannot be made into routine. Now in public service you have to really accelerate the births, because you need the bed, you have patients to be seen to I think there is no harm in oxytocin at all, either for the mother, or for the baby, as long as it is used according to certain criteria.
Despite the fact that oxytocin increases the pain that women suffer, no pain relief is made available to parturients at the facility. Public maternities in Salvador do not offer epidural analgesia (a spinal injection that numbs from the waist down) for normal birth even though the national public health insurance system (SUS) provides funding. Most female informants (all but one) had never heard of such relief and when told about it, wanted to know more. One 16 year-old informant said, "I don't know about anesthesia. Does it exist? I mean, I knew that there is an anesthetic for injecting in the vagina when you are about to have the baby. But this other kind, I never heard of it!" Another informant (22, mother of three) reported, "When I was in all that pain, I thought to myself, 'Oh God in heaven, can it be that [pain relief] doesn't exist?' I was thinking that it didn't, and so I felt that I had to feel my pain". Another, age 24, when asked whether she knew about the existence of a technology of effective pain relief, exclaimed, "No. I didn't know. That's just great . [ironically] Now that I've had my kids! But only in private clinics, isn't that so? It would be fantastic, because it is [emphatic] REAL pain. I felt terrible pain in my backbone".
We asked the providers at the facility about the non-use of epidural analgesia. In agreement with the consensus in the medical literature, they say that epidural analgesia should not be used routinely in normal birth. Its serious drawbacks include prolonging labor and increasing the need for medical interventions such as the use of forceps. Indeed, WHO states: "Methods requiring a large number of technical facilities like epidural analgesia are only applicable in well-equipped, well-staffed hospitals".13 (The authors go on to state that the most desirable method of pain relief in all settings is the non-pharmacological one of "personal attention to the woman and tender, loving care").
Dr. Alexandre (obstetrician) detailed the impediments to introducing epidural analgesia at the facility studied:
The operational cost is very great. And after that there aren't enough anesthesiologists to give anesthesia to all the patients. You don't have enough beds for this either.
The directors of public maternities and obstetric centers in Salvador have neither pressed for the release of SUS funding for epidural analgesia nor actively campaigned to make pain relief available. The failure to pursue the possibility of using the analgesia at the facility studied certainly derives from the perception, expressed by nurses and doctors, that the infrastructure and staffing arrangements at this institution would not permit its use. Andrea (nurse) also referred to a general dissatisfaction among doctors with the SUS payment arrangements.
We found that some of the facility's doctors use epidural analgesia routinely during vaginal delivery with their private patients. In effect, providers accept that poor women must suffer in labor, while private patients need not. One doctor criticized colleagues who allegedly think poor women are better adapted to bear pain. In addition, there is a perception among providers that, culturally speaking, a display of pain enhances the passage into motherhood. Hence, pain relief is not a high priority. Thus, there is little chance that women who suffer unusually extreme pain in labor, can expect to receive pain relief in the near future.
The only painkiller readily available to all patients at the facility studied is an injection applied to the perineum before episiotomy (the cut administered to the perineum shortly before expulsion of the baby). Women know about and expect to have an episiotomy. They call it the "cut" (corte) and subsequent suturing the "sewing up", (costura) and take it for granted that the surgery requires the skills of a doctor. Women consider episiotomy necessary in order to "give passage" to the baby and to avoid tearing of the perineum. They assume that only a doctor can perform the procedure. These views underlie the overwhelming preference for hospital birth in Salvador; access to obstetricians' surgical skills is available only in such institutions.
Episiotomy is the technological procedure associated with normal birth that doctors, nurses and nursing auxiliaries most strongly support. Twenty-three percent of the 56 providers questioned believe that episiotomy should be used routinely, 84% believe that episiotomy benefits the parturient and 93% believe that it helps the medical conduct of birth (see table IV for more details).
]]> According to WHO recommendations, the procedure should only be performed if there are signs of foetal distress, insufficient progress during delivery, or (hard to diagnose) threatened third-degree tear down to the anus and rectal muscles which happens in 0.4% of deliveries.13 WHO concludes that, "liberal use of episiotomy is associated with higher rates of perineal trauma, and lower rates of women with intact perineum There is no evidence of a protective effect of episiotomy on the foetal condition".13WHO warnings against liberal use of episiotomy are ignored at the facility studied. All parturients with vaginal deliveries (except those who accidentally give birth in the labor ward) undergo the procedure. Some providers interviewed expressed ambivalence about its routine use. But the medical director of the facility was firmly in favor of it. He did not believe that WHO recommendations are applicable in a blanket sense in every context, nor to every type of client.
Discussion
Discussing normal birth, both users and providers have health outcomes for mother and baby as a priority. Users go to the hospital because they perceive it as a "safer" context for birth, with access to technology and expertise. Providers agree. Thus, users are largely (but not completely) "compliant" with the technological procedures administered during normal birth at the facility. These represent a safe and modern form of birth. Nevertheless, we found differences between the two groups, and amongst the providers, on the following points: the nature of the women to whom the procedures are administered, the nature of the procedures and the reasons for administering them, and the wider rationale behind day-to-day usage.
Talking about technological procedures during normal birth, providers differ in their expressed opinions, with the highest declared support for the technological procedures of trichotomy, oxytocin infusion and episiotomy evident among auxiliaries, the lowest among doctors. In practice, providers do not question them (with the exception of one doctor). Thus, the "house routines" are maintained despite recognition among some senior providers that they do not always conform to recommendations about good obstetric practice in the medical science literature. Providers who say they do not wholeheartedly support the house routines explained failure to alter these routines with reference to institutional needs and to the nature of the women users.
Women are largely unaware of institutional demands and attribute many aspects of their negative experiences to an alleged lack of humaneness amongst providers. Providers, though recognizing some colleagues' failings, explain these failings emphasizing such factors as job dissatisfaction, bad working conditions, lack of training to deal with the adolescent clientele, and the effects of the institutional dynamics. Some informants drew attention to the fact that the hospital is compared to a model that treats each birth as part of a factory production line, a metaphor often used to describe the organization of care in Euro-American maternity hospitals.15 Under this model, technological routines enhance productive efficiency. Their continued use is seen as inevitable for three main reasons: the severe administrative and financial limitations on running a public hospital in Brazil; a rooted belief that, in fact, the procedures are appropriate in this case or even "good practice"; and, linked to the latter, the perceived nature of the clientele.
Providers see the women as poor, culturally backward, lacking in self-control and unclean. Some providers are openly critical of them, some more sympathetic. The fiercest criticism is directed at young adolescents. Some providers argue that the nature of the women render necessary specific features of care, such as trichotomy. In addition, the maintenance of the routines were defended on technical grounds: the routine use of the procedures were portrayed as necessary, non-harmful or even beneficial.
Obstetric practice at the facility's OC seems, at first sight, to be determined by the importance attributed to technology and biomedical science and to institutional needs. Women and the birth process must fit into the time and space allotted them in the model. In this sense, the facility adopts a variant of the "technocratic model" of birth used in North American hospitals.16 Providers reason that the requirements of the institution justify the use of oxytocin. Though they recognize that women experience an increase in pain, according to the model it must remain unalleviated since epidural analgesia, the only effective technological way of relieving pain, is impractical.
The notion of the "technocratic model" is helpful in analyzing the embeddedness of institutional practices at the facility studied. But the authors of this study suggest that the weight of opinion concerning the women also plays a fundamental role in maintaining the status quo. There is a clear sense in which the suffering experienced by the facility's users is taken as "normal." An analysis of the deeper symbolic logic that informs the usage of technological procedures for normal birth, in line with anthropological studies of childbirth in Brazil17,18 and elsewhere,15,16 gives substance to the view that attitudes toward the women, made up of concepts of race, class and gender, play a fundamental role in sustaining hospital practice. These come into play through the sets of meanings involved in the application of technology.
]]> In Salvador, hospitals and doctors are valued symbols of modernity and this, in turn, is associated with a Euro-Brazilian appearance.4 Technological intervention on the body bestows status. Thus technological procedures are attributed value due to the symbolic work they perform, not just their overt "technical" effects. This is clearly the case for trichotomy and episiotomy. For users at the facility, voluntary trichotomy prior to admission is a symbolic act. By shaving, a woman places herself in a proper relationship to modernity, preparing for the encounter with technology and the doctors at the hospital. She makes her body "clean" and thus ready and fit for a technological birth. From the provider's point-of-view, she is indeed ready for the surgical application of medical science. But, behind the provider's discourse there is a sub-text; a deeper set of meanings. An unshaven woman has failed to clean the dirt of her own environment off her body. She brings the unhygienic atmosphere of her hovel to the purified atmosphere of the Obstetric Center. This view makes a mockery of women's belief that by shaving they show themselves as respectable, savvy patients. Providers regard users as only temporarily cleansed, soon to return to the hovel. Similarly, the hair, a powerful symbol of low status and social exclusion, will soon grow back.As a symbol, episiotomy turns a low-tech hospital birth into a proper technological occasion as a concentrated symbol of "modernity", not least because it is conducted by a white technician in a hygienic setting. Again, two sets of contrasting meanings come into play. As a scientific surgical intervention on the body, episiotomy evokes its symbolic opposite: non-technological home birth, redolent of backwardness and rural life and associated with blackness and the lower classes. Thus, we argue, the symbolic construction of a complex notion of modernity through hospital practices turns upon a more insidious construction of race and class difference. Hospital practice symbolically reinforces race, class and gender inequality.
It is likely that the findings for the facility studied are applicable elsewhere in the public sector in Salvador, and in Brazil. They reveal the rootedness of hospital practice in both cultural understandings and institutional constraints. Both should be addressed in rethinking policy for Brazilian public maternity care. Specifically, policymakers should seek to rectify the deep-seated support among providers for the routine use of technological procedures that current medical science finds to be unnecessary or harmful. Their apparent indifference or apathy with respect to the psychological and social aspects of birthing requires challenging. The substantial number of providers who favor the humanization of childbirth should be supported. Specifically, the authors suggest including or strengthening critical discussion of the application of routine trichotomy, episiotomy and oxytocin, in the movement already in place to "humanize" childbirth.18-21 Finally, user's knowledge and cultural attitudes also need to be addressed. It is likely that until women are empowered with a better understanding of the technological procedures discussed in this article, birth in public maternities in Brazil will remain an unnecessarily harrowing experience.
Acknowledements
This investigation received financial support from the Special Program for Research, Development and Research Training in Human Reproduction, World Health Organization. We are grateful to the Social Science Research Initiative on Adolescent Sexual and Reproductive Health at WHO for intellectual support for the research. Special thanks to Iqbal Shah, and to Kate Kosterzewa for her excellent editorial advice. We thank MUSA, the Study Program in Gender and Health (ISC/UFBA) for support of the project, especially Greice Menezes, Estela Aquino (our co-investigator) and Luisa Elvira Belaunde. The article is based on a paper given at the ASA 5th Decennial Conference on "Anthropology and Science"; Manchester, July 14th to 18th, 2003, panel: "Science and the Cultural Politics of Reproductive Technologies," convened by Tulsi Patel. Thanks goes out to her and to the participants for their helpful comments.
References
1. IBGE. Síntese de indicadores sociais 2000. Rio de Janeiro: IBGE, 2001. [ Links ]
2. Sansone L. Negritude sem etnicidade. Salvador/Rio de Janeiro: EDUFBA/Pallas, 2004. [ Links ]
3. SESAB. Saúde reprodutiva no estado da bahia: adolescentes e jovens nos serviços de saúde reprodutiva. Rio de Janeiro: SESAB/SUS/BEMFAM et al, 2000. [ Links ]
4. McCallum C. Explaining caesarean section in Salvador da Bahia, Brazil. Sociol Health Illn 2005; 27:215-242. [ Links ]
5. Reichmann R, ed. Race in contemporary Brazil. University Park, PA: The Pennsylvania State University Press, 1999. [ Links ]
6. Telles E. Racismo à brasileira: uma nova perspectiva sociológica. Rio de Janeiro: Relume Dumará, 2003: 103-135. [ Links ]
7. IBGE teen. Accessed 23 August 2006. Available at: www.ibge.gov.br [ Links ]
8. IBGE. Censo demográfico 2000: nupcialidade e fecundidade resultados da amostra. Rio de Janeiro: IBGE, 2000. [ Links ]
9. DATASUS. Accessed 23 August 2006. Website Available at: http://tabnet.datasus.gov.br/cgi/ deftohtm.exe?sih/cnv/piba.htm [ Links ]
10. McCallum C, Dos Reis AP. Childbirth as ritual in Brazil: Young mothers experiences. Ethnos 2005;70:335-360. [ Links ]
11. Riesco MLG, Tsunechiro MA. Formação profissional de obstetrizes e enfermeiras obstétricas: velhos problemas ou novas possibilidades? Estudos Feministas 2002; 10:449-459. [ Links ]
12. Béhague DP. Beyond the simple economics of cesarean section birthing: women's resistance to social inequality. Culture, Medicine and Psychiatry 2002; 26:473-507. [ Links ]
13. World Health Organization. Care in normal birth: a practical guide. WHO/FRH/MSM/96.24. [Accessed August 21, 2000]. Available at: http://www.who.int/reproductive-health/ publications/MSM_96_24/care_in_normal_birth_practical_guide.pdf . [ Links ]
14. Hemminki, E. A trial on continuous human support during labor: feasibility, interventions and mother's satisfaction. J Psychom Obstet Gynecol 1990; 11:239-250. [ Links ]
15. Martin E. The woman in the body: a cultural analysis of reproduction. Boston: Beacon Press, 1987. [ Links ]
16. Davis-Floyd RE. Birth as an American rite of passage. Berkeley: University of California Press, 1992. [ Links ]
17. Mott ML, org. Bibliografia comentada sobre a assistência ao parto no Brasil. Revista Estudos Feministas 2002; 10:493-507. [ Links ]
18. Tornquist CS. Armadilhas da nova era: natureza e maternidade no ideário da humanização do parto. Revista Estudos Feministas 2002; 10:483-492. [ Links ]
19. Brasil. Política nacional de atenção integral à saúde da mulher: princípios e diretrizes / Ministério da Saúde, Secretaria de Atenção à Saúde, Departamento de Ações Pragmáticas Estratégicas. Brasil: Ministério da Saúde 2004:80. [ Links ]
20. Diniz CSG. Entre a técnica e os direitos humanos: possibilidades e limites da humanização da assistência ao parto. Thesis Sao Paulo: Universidade de São Paulo, 2001. [ Links ]
21. Misago C, Kendall C, Freitas P, Haneda K, Silveira D, Onuki D, et al. From 'culture of dehumanization of childbirth' to 'childbirth as a transformative experience': changes in five municipalities in north-east Brazil. Int J Gynaecol Obstet 2001:75 suppl 1:S67-S72. [ Links ]
]]> Received on: January 5, 2006
Address reprint requests to: PhD Cecilia McCallum. Federal University of Bahia. Av. Princesa Isabel 801, 204, Edificio Firenze, Salvador Bahia 401 30 030 Brazil. E-mail: cecilia.mccallum@uol.com.br
* Aquino E, Franco I, Marinho L. Saúde, sexualidade e direitos repodutivos: a situação das mulheres na Bahia. Unpublished Research Report, 1995.
** Menezes G, Aquino E. Mortalidade materna na Bahia: 1998. Relatório de atividades. Universidade Federal da Bahia, Instituto de Saúde Coletiva e Secretaria de Saúde do Estado da Bahia. 2002. Mimeo.