Although the knowledge and number of several consensus meetings show an increasing trend in the last decades1-8, the need to review some controversial topics to update the common language that we are currently using for the diabetic foot syndrome still remain.
To review the global and regional contributions of the Saint Elian Wound Score System (SEWSS) for the diabetic foot syndrome are the aim of this report.
Definition of the diabetic foot
Since 1998, once the Diabetic Foot definition9 was published by the World Health Organization, scarse efforts to define this complex condition were made. A relevant task was performed by the consensus of the International Working Group on the Diabetic Foot (IWGDF)10. Definitions were consensuated on the knowledge that preveails during those meeting. Although in the first definition the IWGDF agreed to differentiate the severity grades for ischemia, they were not applied the same criteria for the rest of variables, describing “leg” involvement instead the foot. Unfortunately, in the following consensus the terms grading, wound and foot were omitted until the 2015 meeting when the word foot was included again11. The relevance to differentiated the severity grade using an score system (absence = 0, mild = 1, moderate = 2, and severe = 3) for single or multiple wound variables was addressed and validated by Lavery12 for infection, DEPA13 for depth and the San Elian System14 for location (site), anatomic aspects and foot zones, ischemia, infection, edema, neuropathy, area, depth, and wound healing phase. The diabetic foot definition like many published classifications shows bias because it does not include all the relevant wound variables. For instance, one paper15 exclude ischemia and infection as a wound factor, mixing area, depth, gangrene, and ulcer size in one variable when each one was previously validated as a single significant independent factor14,15. The resultant controversies from the author preferences to select variables according to their personal view could influence the decisions to define the diabetic foot inside the task groups. The last 2015, IWGDF definition of diabetic foot11 omitted the term wound and, the severity grades that were not considered as part of the destruction of tissues caused by PAD, infection, or advanced neuropathy (Charcot). The 2016, Saint Elian definition include severity grades and the description of wound variables that cause and aggravate the risk of lower extremity amputations and death. Therefore, considering the evolving concept of the “Diabetic Foot Attack (DFA)” that will be posteriorly described within this paper the authors reasoned the Diabetic Foot definition as follow: Is a syndrome clinically manifested by an acute or chronic attack, featured by one or more foot wounds with differences in etiology and severity grades of extent, depth, anatomic zones and aspects, infection, ischemia, edema, and neuropathy increasing amputations and death risk in persons with diabetes. This definition clearly differentiates diabetic foot wounds from soft tissue infections and venous or arterial ulcers of the lower extremities in people with Diabetes Mellitus. Also clarify that ulcer is a term that not define the diabetic foot and means only a kind of wound.
Classification and score
While many classification systems have been validated in study populations, little is known about their interobserver reliability. Two concordance studies between observers in different popular classifications were recently published. Santema et al.16 founded in an interobserver analyses a moderate agreement comparing the Meggitt-Wagner and the University of Texas classifications for diabetic foot ulcers, that demonstrates that both systems appear not to be useful as single instrument and should always be used in combination with additional clinical information to avoid erroneous interpretations. Recently, Forsythe et al.17 evaluate the interobserver reliability of three scoring systems for diabetic foot ulceration (Perfusion, Extent, Depth, Infection, Sensation, Site, Ischemia, Neuropathy, Bacterial Infection, and Depth and UTC). These classification systems may be reliably used by multiple observers, for example, when conducting research and audit. However, they demonstrate only slight to moderate reliability when used by a single observer on an individual subject and may therefore be less helpful in the clinical setting, when documenting ulcer characteristics or communicating between colleagues. The absence of internal and external validation for many popular classifications system is a current problem because their use in centers where the amputations rate is high. Some classifications were validated for other groups (external) without the mandatory initial internal validation18. The progress to validate a score system must include all identified wound variables, avoiding bias of variables selection. Unfortunately, current classifications show bias because they are excluding important wound variables and their differentiation by severity grades. The Saint Elian score is a system submitted to scruttiny under the rigurous scientific process of internal14 and external validation19-25 that provide a comprehensive model to approach the above-mentioned purposes.
Relevance of the San Elian System in diabetic foot wounds14,25-36.
Diagnosis
After clinical assessment and non-invasive studies data collections are recorded on the clinical chart including the levels of severity to the ten different categories as follows: (a) primary location, (b) topographic aspects, (c) number of affected zones, (d) ischemia, (e) infection, (f) edema, (g) neuropathy, (h) depth, (i) area, and (j) wound healing phase (Table 1). All are subcategorized with an ascending severity score from mild (1 point) to severe (3 points).
Table 1 Saint elian score system. Clinical practice recommendations of the diabetic foot -IDF 2017
| Factors | Score (Severity) | |||
|---|---|---|---|---|
| 1 (Mild) | 2 (Moderate) | 3 (Severe) | Score | |
| (1) Primary zone (location) | Phalanges | Metatarsal | Tarsal | |
| (2) Topographic aspects (location) | Dorsal or plantar | Lateral or medial | Two or more | |
| (3) Zone number | One | Two | Three | |
| (4) Ischemia | Palpable pulses slightly diminished ABI (0.89-0.7) TBI (0.74-0.60) |
Scarcely palpable pulses ABI (0.69-0.5) TBI (0.59-0.30) |
Non palpable pulses ABI < 0.5 TBI < 0.30 |
|
| (5) Infection | Erythema < 2 cm. Purulent discharge, warmth, tenderness | Erythema > 2 cm Muscles, tendons or bone or joint infection. |
Systemic inflammatory Response Syndrome. Secondary hyper or hypoglycemia | |
| (6) Edema | Periwound | One Foot or leg | Bilateral secondary to comorbidities | |
| (7) Neuropathy | Protective Sensation diminished (128 HZ tuning fork, SWM, Vibratip, Ipswich) | Protective Sensation absent (128 HZ tuning fork, SWM, Vibratip, Ipswich) | Diabetic neuroosteoarthropathy (DNOA)-Charcot | |
| (8) Area | Small < 10 cm2 | Medium 11-40 cm2 | Big > 40 cm2 | |
| (9) Depth | Superficial (skin) | Tendons, fascia, muscles | Deep joint and bones | |
| (10) Wound healing phase | Inflammatory | Granulating | Epithelialization | |
| Score sum | ||||
| Final score | Grade (Severity) | Prognosis | ||
| < 10 | I (Mild) | Likely successful wound healing. No LEA | ||
| 11-20 | II (Moderate) | Partial foot-threatening; outcome related to “state-of-the-art” therapies used and associated with a good patient biological response. < 30% LEA | ||
| 21-30 | III (Severe) | Limb- and life-threatening; outcome unrelated to “state-of-the-art” therapies because of poor biological patient response. > 70% LEA | ||
Check the severity column and annotate the score (1-3) at the right column. Score 0, for absence of the aggravating factor (ischemia, infection, edema or neuropathy. WFA: waveform analysis SWM: Semmes Weinstein Monofilament. LEA: Lower extremity amputations.
Prognosis
The maximum score achievable is 30 points. When a score sum of 10 points or fewer (if zero value was scored for aggravating factors) was obtained, it was graded as I (mild, likely successful wound healing). A moderate score of 11-20 points was graded as II (partial foot threatening; outcome related to “state-of-the-art” therapies used and associated with a good patient biological response), and 21-30 points was graded as III (limb- and life-threatening; outcome unrelated to “state-of- the-art” therapies because of poor biological patient response).
Treatment
Focused on medical and surgical treatment of aggravating factors (Ischemia, infection, edema, and neuropathy) according to the severity score (0-3) and wound healing phases acceleration. Recently a paper37 reported the term “DFA” to describe the wounded Diabetic Foot Syndrome. The DFA report, describes three types including ischemia, infection, and Neuropathy (Charcot). According to the San Elian System the DFA include the addition of edema and the mixed attack considering five types of foot attack. The DFA is a devastating presentation with an acutely inflamed foot with rapidly progressive skin and tissue necrosis, associated at times with significant systemic symptoms (Fig. 1). It could rapidly escalate over hours from an apparently simple injury, to limb-threatening proportions. This may be an entirely new presentation or a sudden deterioration on the background of a known neuropathic diabetic foot ulcer, limb ischemia, or both, wherein delays in recognition or intervention pose a significant risk of major amputation.
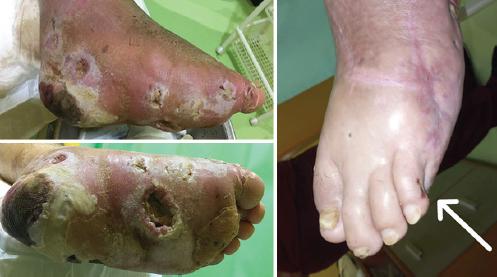
Figure 1 The picture shows a combined mixed devastating Diabetic Foot Attack (DFA) including, infection, edema, Charcot foot and their remission (Saint Elian Grade III scoring 23 points). The arrow point out the DFA remission after the treatment under the Saint Elian System. Then, the Stage III start with a very high risk for a new DFA, amputations, or death.
The San Elian Triage for the DFA in the Emergency room.
The SEWSS severity Grades and score provide a guideline to priorize the immediate medical treatment of diabetic foot persons according to their chance of benefiting from such care to survive or limit the damage and extremity function (Table 2).
Table 2 The Saint Elian severity triage for survival and function of the diabetic foot
| Priority 1 | Priority 2 | Priority 3 | Priority 4 |
|---|---|---|---|
| Saint Elian Grades III and II (> 17 score) Severe Diabetic Foot Attack secondary to ischemia, infection, edema and Charcot or a mixed combination. | Saint Elian Grades III and II (> 17 score) moderate Diabetic Foot Attack secondary to ischemia, infection, edema and Charcot or a mixed combination. |
Saint Elian Grade II (< 17 score) mild Diabetic Foot Attack secondary to any type of attack. |
Gangrene of the entire foot limb- but not life threatening problem |
Follow-up of healing progress26
The score of ten severity factors and grade for prognosis within the checklist format is recorded from daily to every week, as necessary. Score changes in progress of wound healing permit to implement proactive therapeutics actions (Table 3).
Table 3 Follow up table for healing progress of diabetic foot wounds*
| Patient name |
|---|
| Date |
| Date |
| Medical and surgical Treatment** |
| FACTORS (score 1-3) |
| Location (1-3) |
| Aspects (1-3) |
| Number of Zones (1-3) |
| Ischemia (0-3) |
| Infection (0-3) |
| Edema (0-3) |
| Neuropathy (0-3) |
| Area (1-3) |
| Depth (1-3) |
| Wound healing phase (1-3) |
| Score |
| Difference |
| Grade |
| Physician name and signature |
*Saint Elian System scores the wound severity as many times as necessary, at least 1 time/week.
* Surgical operations (debridement, minor and major amputations, bypass, angioplasty, etc.) and/or adjuvant therapies (Negative Pressure Therapy, bioengineered skin, growth factors, stem cells, antimicrobial therapy, etc.).
Prevention
The system provides a platform for primary, secondary, and tertiary prevention according to the Leavel and Clark model and the foot risk classification of the IDF (Table 4). The referral and counter referral process for three levels of care is included. The potential value of this system is that the influence of population-dependent parameters may be important to be included within a detailed and unified score to inform the work of colleagues developments else-where toward reducing amputations in the diabetic patient31.
Table 4 Foot risk classification – international diabetes federation 2017
| Risk Category | Characteristics | Follow-up | Treatment Plan |
|---|---|---|---|
| 0 Low risk | Normal plantar sensation | Re-check in 12 months | Patient education, daily inspection, proper footwear. Routine foot care as needed. Yearly follow-up, tight glycemic control necessary to maintain this risk category |
| 1 moderate | Loss of protective sensation (LOPS) | Re-check in 6 months | Patient education, proper footwear, soft molded insoles. Routine foot care as needed. Daily self-inspection. Six month follow-up. |
| 2 high risk | LOPS with either high pressure or poor circulation (PAD) or structural foot deformities or onychomycosis | Re-check in 3 months | Patient education, proper footwear with possible modifications custom molded insoles fitted into footwear with possible modifications to relieve areas of pressure. Scheduled routine foot care. Daily self-inspection. |
| 3 Very High Risk | History of ulceration amputation or neurophatic fractures | Immediate referral if active ulcer or Charcot foot.
Re-check in 1 month if history of ulcer or Charcot foot |
Patient education. Extra depth footwear with custom modification custom molded insoles with modifications to relieve pressure, offload with cast as necessary, scheduled routine foot care. Daily self- inspection. |
Stages of risk progress for Foot Attack, amputations, and death.
Persons with Diabetes Mellitus may progress from low risk stage to foot attack remitting to a posterior high risk stage or conversely to a major amputation or death. The progress stages are described as follow: (a) Stage I Low Risk Foot. Persons with diabetes mellitus and foot at risk without wound history and no wound at patient presentation; (b) Stage II The Foot Attack that could progress to heal with or without minor amputations or conversely, lead to major limb amputation or death; and (c) Stage III High Risk Foot. After the Foot Attack. History of a wound healed with minor amputations with their feet at a higher risk for limb lose or to develop a new wound.
The global and the latinamerican impact of the San Elian System
The San Elian Latin American System is widely referred as part of peer-review papers14,19-23,25,26,28,29,30,33-36, books chapters27,30,32, awards keynote lectures38, and guidelines1-8,24, including the global milestone contribution to the IDF -Clinical Practice Recommendations of the Diabetic Foot-20171. The relevant keynote lectures included: (1) the Multidisciplinary International Limb and Amputations prevention Conference. Classificazioni del piede diabético: la classsificazione di San Elian e migliori di altre? Milán, . 2013;(2) the San Elian comprehensive surgical approach for diabetic foot wounds. Diabetic Foot International Summer School of Surgery, Bergamo Italia, 2017; (3) Certification for Physicians to prevent the Diabetic Foot Syndrome: The Saint Elian System. International Diabetes Federation Congress. Abu Dhabi-2017; and (4) The Saint Elian score for the diabetic foot syndrome: A dynamic and detailed system to reduce lower-extremity amputation: the foot attack in LATAM. IDF- Global Congress, Busan, Korea-2019. The Regional Contribution for the Americas is published as part of several diabetic foot guidelines of different medical societies and the Minister of Heath in Chile39 and Mexico40,41. Included as one of the main classification system in several clinical practices guidelines of different multidisciplinary medical associations, the San Elian model presented by latinamerican delegates integrated a final and current document: The Declaratory of the Diabetic Foot Summit of the Americas, that was held in Mexico City42.
In conclusion, the Latinamerican SEWSS provides a validated tool with global relevance. The key message is to be able to treat diabetes and to prevent any possible complication. Once the DFA develops the system provide a comprehensive checklist to score wound severity at patient presentation and during the follow-up of healing progress to achieve better outcomes. The devastating five types of DFA according to San Elian aggravating factors include the ischemic attack as the first cause of legs amputations. This report reviewed the regional and global contribution of the SEWSS for definition, classification, diagnosis, treatment, prevention including a new triage system and the progress of DFA stages as an useful tool to prevent mortality and major amputations.











 nueva página del texto (beta)
nueva página del texto (beta)


