Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista odontológica mexicana
versión impresa ISSN 1870-199X
Rev. Odont. Mex vol.20 no.1 Ciudad de México ene./mar. 2016
https://doi.org/10.1016/j.rodmex.2016.02.007
Case reports
Implant-supported nasal prosthesis. Clinical case report
a Graduate Maxillofacial Prosthesis Specialty. Graduate and Research School, National School of Dentistry, National University of Mexico (UNAM).
b Professor Maxillofacial Prosthesis Specialty. Graduate and Research School, National School of Dentistry, National University of Mexico (UNAM).
In our days, functional and esthetic reconstruction is one of the problems most frequently encountered when treating patients with facial defects. This reconstruction entails to choose among rehabilitation materials to use in each case. Extra-oral implants play an important role in prosthetic support, they bear influence into esthetic, functional and psychological aspects, granting better quality of life to the patient. The aim of the present study was to functionally and esthetically rehabilitate the patient as well as improve his quality of life with the use of an implant-supported nasal prosthesis.
Keywords Maxillofacial prosthesis; facial defects; nasal prostheses; implants; magnets
Un reto en el tratamiento integral de pacientes con defectos faciales, es la reconstrucción con fines funcionales y estéticos, que conlleva a la elección de la rehabilitación y material a utilizar en cada caso. Los implantes extraorales juegan un papel importante en el soporte protésico, influyendo en los aspectos psicológicos, funcionales y estéticos, aportando al paciente una mejor calidad de vida. El objetivo de este trabajo es rehabilitar estética y funcionalmente, y mejorar la calidad de vida del paciente ofreciéndole, una prótesis nasal implantosoportada.
Palabras clave Prótesis maxilofacial; defectos faciales; prótesis nasales; implantes; magnetos
INTRODUCTION
Prosthetic rehabilitation is the means by which an artificial device is placed to substitute an organ lost due to many causes that might be congenital, traumatic or surgical in nature.1
The nasal pyramid is a frequent site for location of skin tumors such as basal cell carcinoma, epidermoid tumor and melanoma. These tumors must be surgically treated, and in some cases, security margins can be corrected by means of esthetic surgery. In some cases, to avoid relapse, the defect might be left open.2
Technological advances have influenced facial prostheses. After the Second World War, acrylic resins and silicon materials began to be used to manufacture prostheses. With the introduction of bone integration in the extra-oral region many of the retention and stability problems encountered with conventional prostheses were solved; this represents an important advance for the retention of this type of prostheses. Bone integration allows the use of silicon at its full potential, eliminating thus the use of adhesives, securing suitable retention and fine borders, generating better esthetic results and providing more security to the patient.3
Systemic diseases which might impair bone metabolism would represent a contraindication to the use of bone integrated implants.4 Among these diseases we can count: osteoporosis, fibrous dysplasia, «Paget's disease» or deforming osteitis (osteitis deformans), multiple myeloma, psychiatric conditions and uncontrolled addictive behaviors. Other aspects to be considered, are inability to preserve implant hygiene which would compromise diagnosis as well as lack of easy access to the patient in order to preserve suitable maintenance therapy.5
Patients who have received radiation treatment must be carefully selected, since they might exhibit lesser rate of success than non-radiated patients. Secondary effects will depend on radiotherapy intensity: with low pre-operative bases, it has been found that local control is improved with a dosage of 34.5 Gy, divided into 15 fractions of 2.3 Gy during 19 days, which would be equivalent to 39.6-44 normally fractioned Gy. In the head and neck, radiation can reach up to 70 Gy in 35 fractions of 2 Gy per session, five times a week, this is to say the treatment would last seven weeks.6 It is worth mentioning that ideal radiation site should be the head and neck region, otherwise there would be no direct implication to maxillofacial rehabilitation with implants. Hyperbaric oxygenation enhances bone integration success. It is administered before placing the implants. The procedure consists on 20 sessions of hyperbaric oxygen as well as ten additional sessions after implant placement in order to favor bone formation and avoid implant loss.7
HISTORICAL BACKGROUND
Since ancient times, man has tried to restore facial deformations and defects which alter their appearance. Egyptian mummies have been found with artificial noses, eyes and ears. Around 1950, Amboise Pare described the first maxillofacial prosthesis. Maxillofacial prosthesis science is the branch of dentistry that involves esthetic and functional rehabilitation of structures located outside the mouth as well as within it. It employs artificial means whose objective is not only re-establishing suitable shape and function, but also to preserve remaining tissue in good repair. In 1977, Anders Tjenström (Sweden) expanded the concept of bone-integration to the cranio-facial region, creating thus new possibilities to rehabilitate the face with implant-supported oral-maxillofacial prostheses.8
CASE REPORT
74 year old male patient, born in Capulhuac, State of Mexico. The patient was referred to the Head and Neck Service of the National Cancer Institute of Mexico (Instituto Nacional de Cancerologia de Mexico).
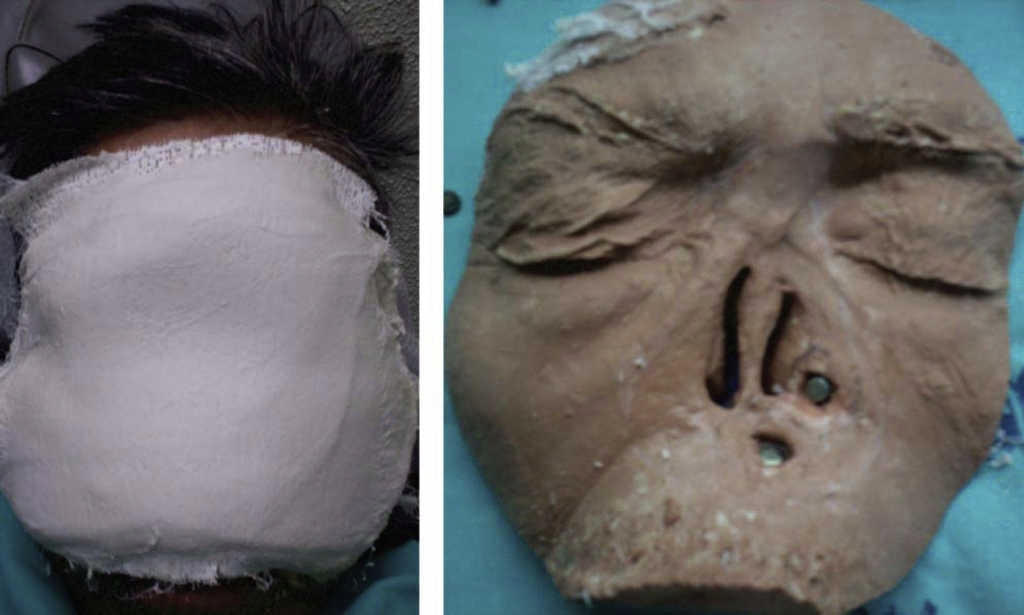
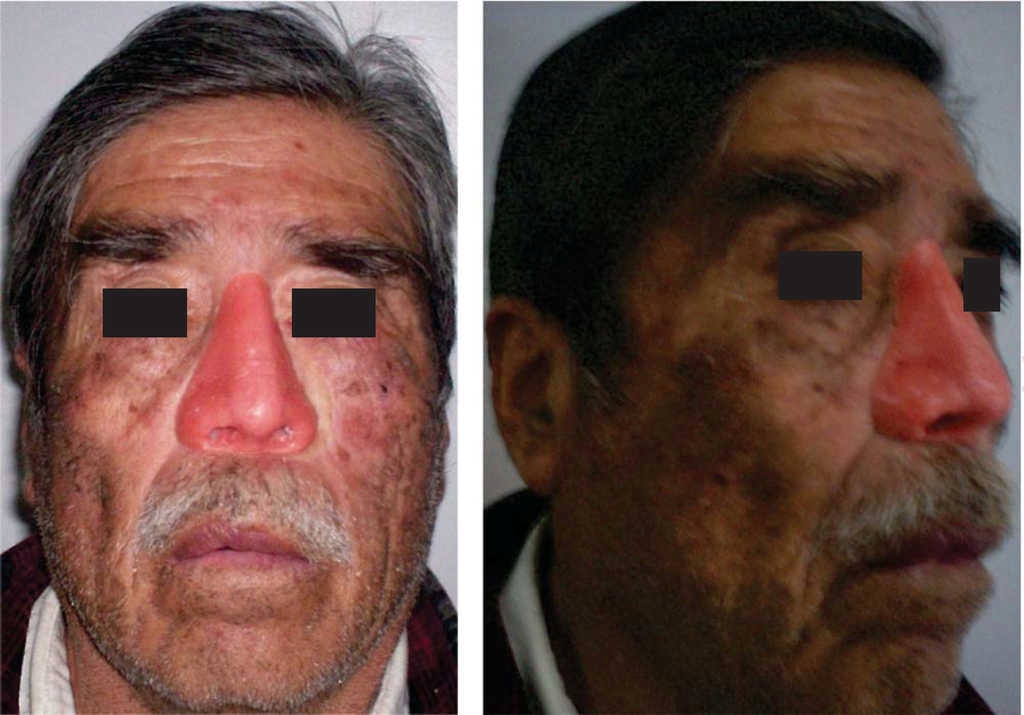
Clinical assessment revealed destroyed nasal cartilage as a result of surgical resection of a tumor lesion (Figures 1 and 2). The resulting surgical defect was inadequate to satisfy the patient's esthetic requirements and was hindering his social activities. Therefore, nasal prosthetic rehabilitation with different retention means (adhesive and implant-supported) was suggested and pros and cons were carefully explained to the patient.

Figures 1 and 2 Patient with destroyed nasal cartilage after surgical intervention. Defect covered in gauze.
The patient selected use of an implant-supported nasal prosthesis, manufactured with a base of acrylic resin, medical-grade silicon and magnets.
METHODOLOGY
Implant placement
With the help of a tomography, a suitable place was found with sufficient bone to place implants. Three implants were placed (Strauman nose implants. REF 043.030S, LOT 1025, 4.1 mm diameter, 6.0 mm length) at the maxillary bone close to the area where nasal bones were once located.
Healing and maintenance
After surgery and during bone integration period (three months) implant healing and maintenance was undertaken. This procedure was achieved with a gel and solution of neutral pH super oxidation solution (Estericide) to prevent and control infections of tissues surrounding the implants. For our patients, curative periods were on alternate days all during healing time. After two months, healing plug was replaced by the Titan magnetic device, which would become the receptor of the future prosthesis. This prosthesis will carry in its back magnets which will be antagonists to the magnets screwed to the implant. The patient was requested to attend the maxillofacial prosthesis clinic of the National Cancer Institute. Clinical exploration revealed a clean defect with suitable healing, therefore it was decided to undertake a nasal prosthetic treatment (Figure 2).
Obtaining the working model
In order to obtain the impression of the defect, the area to be impressed was circumscribed. Before the impression, Vaseline was applied to eyebrows and eyelashes in order to avoid their shedding; remaining nasal tissues were protected with a damp gauze to avoid flexure. Transfer impression pins were placed, in order to transfer by mean of an analogous pin the exact location of the pins and thus be able to work on the plaster model which represented the patient's face.
Facial impression was obtained with gauze and dental plaster reinforced alginate. Analogue pins were dental plaster reinforced alginate. Analogue pins were placed at that time and were immersed in plaster. The positive version was obtained with type IV plaster (Figures 3 and 4).
Resin base plate
This plate was manufactured with the aim of containing the magnets, it will become the back section of the prosthesis. It was manufactured in self-curing clear acrylic, which was placed after placing the magnets on the laboratory implant. A powder-liquid mix was placed on the model previously treated with plaster-acrylic separator in the desired area. After the acrylic had set, the resin plate was removed from the model in order to trim excesses and polish it.
Wax modeling and test on patient
A nose-shaped wax pattern was achieved on the plaster model. This nose shaped mold must be adequate to the face's morphology, according to visual recognizance as well as consultation with patient's former photographs. After adaptation and formation of marginal contours, the wax pattern was located and tested on the patient (Figures 5 and 6).
Prosthesis muffling and de-waxing
A prosthodontics muffle was used. Material employed was type III plaster (Stone) for the base of the muffle. When the plaster had set, two layers of plaster-acrylic separator were applied so as to be able to place the counter-muffle and incorporate type IV plaster (vel-mix). Once the muffle plaster had set, the muffle was placed in a press and taken to a pot with water and boiled for approximately 15 minutes. The press was then removed and the muffle was opened so that molten wax could flow out. More hot water with detergent was incorporated, and the two muffle counterparts were brushed with a plastic bristle brush, so as to avoid permanence in the plaster of wax and grease remnants.
Intrinsic characterization and silicon pressing
With the patient present, skin color as well as face discolorations, moles etc were replicated. Silicon intrinsic characterization was achieved with «flock» synthetic fibers (textile fibers) which replicate basic skin tone. They were made in different shades according to the area to be replicated, to later be put in position according to the desired effect.
It ojo WHATwas placed in the muffle with a thin spatula, in different sections according to the color given to each silicon portion (medical grade), the remaining silicon was placed in the other areas of the muffle. The muffle was then closed joining both counter-sections. It was then taken to a hydraulic press with 350-400 kg pressure. To be then left to vulcanize for 24 hours.
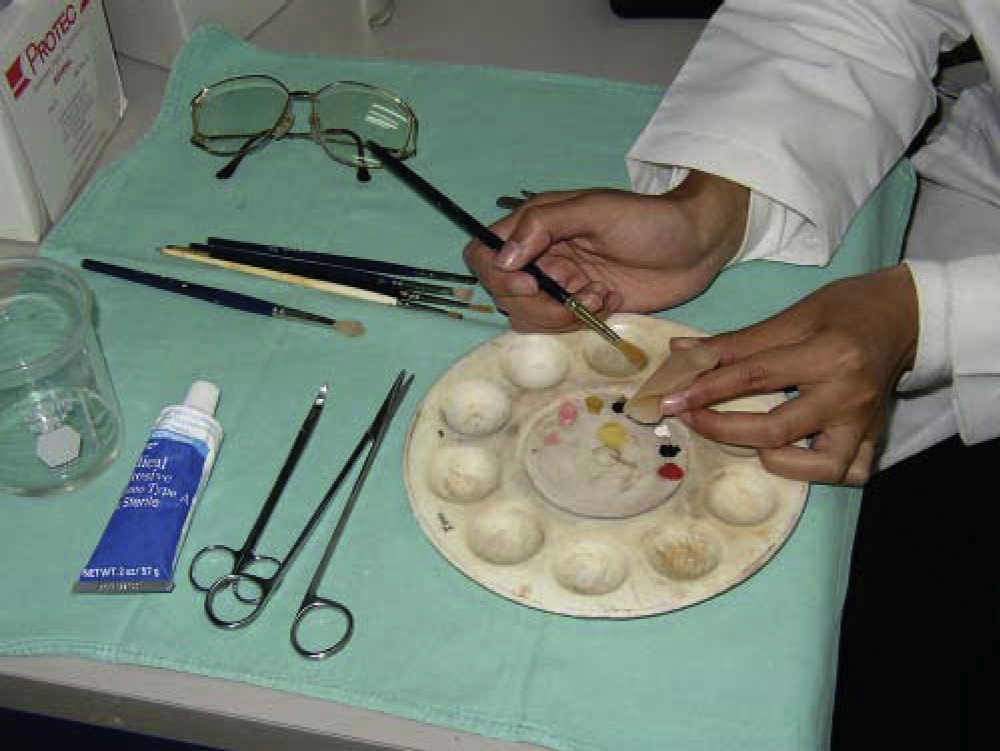
Extrinsic characterization
The silicon prosthesis was retrieved in order to trim it and proceed to extrinsic characterization. This characterization was undertaken with oil paints and use of acrylic monomer to dilute. They were painted on the prosthesis with brushes so as to provide details of the patient skin color. Finally, when the color of the prosthesis was deemed satisfactory, a medical grade silicon layer was placed, so as to seal applied color and avoid color fading (Figure 7).
After this, the prosthesis was delivered to the patient and he was instructed in its care (Figures 8 and 9).
During the following follow-up appointment, the patient did not exhibit any complaint or discomfort and was satisfied with obtained esthetic result.
DISCUSSION
Patients are faced with the dilemma of whether to choose surgical techniques or prosthetic rehabilitation. Many surgical techniques have been put forward for nasal reconstruction procedures: among them we can count rotated flaps, cartilage internal and external grafts as well as autologous implants. With the advent of micro-vascular surgical techniques, the potential for a more favorable nose surgical reconstruction is imminent. Nevertheless, the prominent location of the nose as well as the complexity of its anatomical configuration render surgical reconstruction very difficult. In maxillofacial rehabilitation, the prosthetic option for nasal defects is more viable, especially when defects are of a great size. Furthermore, it is an ideal option in cases when financial aspects of rehabilitation are taken into consideration. It must also be mentioned that adhesive retention prostheses are not the ideal rehabilitation option they should only be used in cases when the patient meets with requirements previous to implant supported rehabilitation. With the use of implants as a retention means, the patient feels more secure, and avoids the discomfort of having to cleanse adhesive residues after each use. He feels safer in daily life without worrying about the prosthesis falling out when sneezing, sweating or crouching. In summary, extra-oral implants offer better retention and stability to facial prostheses than adhesives, and they provide the patient with esthetic satisfaction contributing thus to a better quality of life.9
CONCLUSION
Mutilations in the maxillofacial area are doubtlessly those which more affect physical appearance. Any nose defect becomes a hindrance to the patient's normal daily activities. Nasal defects can be restored by surgical reconstruction or prosthetic reconstruction. Post-surgical defects due to loss at the nasal region leave sequels that compromise esthetics as well as the emotional state of the patient. This problem disappears with placement of an implant supported prosthesis.
REFERENCES
1. R. Keerl, R. Weber, W. Scholtes, W. Draf, G. Heieis, D. Trainer. Prosthetic rehabilitation after craniofacial surgery. Skull Base Surgery. 1996, 6: 207-213 [ Links ]
2. J.C. Lemon, S. Kiatamnuay, L. Gettleman, J.W. Martin, M.S. Chambers. Facial prosthetic rehabilitation: preprosthetic surgical techniques and biomaterials. Curr Opin Otolaryngol Head Neck Surg. 2005, 13: 255-262 [ Links ]
3. Cirugía plástica y Estética, Cirugía Craneomaxilofacial, Estética dental y Implantes; Isla de Nelson 2, Madrid 28035. Tumores de la nariz/reconstruccion nasal. Disponible en: http://www.drlalinde.com/tumores_faciales/nariz.htm. [ Links ]
4. S.G. Borgia. Asociación Brasilera de Enseñanza Odontológica (ABENO). Prótesis buco-maxilo-facial sobre implantes extraorales San Pablo 2007. 2007; [ Links ]
5. M.R. Arcuri, W.E. LaVelle, A. Fyler, G. Funk. Effects of implant anchorage on midface prostheses. J Prosthet Dent.. 1997; 78:496p [ Links ]
6. P. Rubin. Odontología clínica Enfoque multidisciplinaria para médicos y estudiantes. Octava ed. Saunders elservier science. Disponible en: http://books.google.com.mx/books?id=-whwqAxkacMC%26pg=PA736%26lpg=PA736%26dq=fracciones+en+radioterapia%26source=bl%26ots=X55B2KSfTL%26sig=N_oXzslG-pIMNJ9iOSsvh5RZ4b8%26hl=es%26ei=JJDfSajsKJfmnQe4pKCxCQ%26sa=X%26oi=book_result%26ct=result%26resnum=9. [ Links ]
7. Sosa, et-al. Prótesis Faciales Retenidas con Implantes e Imanes: Presentación de Tres Casos Clínicos en Pacientes Oncológicos de Prótesis Maxilofacial del Instituto Nacional de Cancerología. Cancerología. 2008, 3: 71-76 [ Links ]
8. S.G. Borgia. Asociación Brasilera de Enseñanza Odontológica (ABENO). Prótesis buco-maxilo-facial sobre implantes extraorales: estado actual. 2007; [ Links ]
9 S.S. Guttal, N.P. Patil, R.K. Nadiger, A. Hasti. Nasal prosthesis for a patient with mammalian bite injury. The Journal of Indian Prothodontic Society.. 2007; 7:43p [ Links ]
REFERENCES
— P.F. Allen, G. Watson, I. Stassen, A.S. Mcmillan. Peri-implant soft tissue maintenance in patients with craniofacial implant retained prostheses. Int J Oral Maxillofac Surg.. 2000; 29:99p [ Links ]
— R. Alvi, J. McPhail, K. Hancock. Closed-field titanium magnets for the retention of complex craniofacial prostheses. Br J Plast Surg.. 2002; 55:668p [ Links ]
— D.E. Tolman, P.F. Taylor. Bone-anchored craniofacial prosthesis study: irradiated patients. Int J Oral Maxillofac Implants.. 1996; 11:612p [ Links ]
— S. Lundgren, P.K. Moy, J. Beumer 3rd, S. Lewis. Surgical considerations for endosseous implants in the craniofacial region: a 3-year report. Int J Oral Maxillofac Surg.. 1993; 22:272p [ Links ]
— W.S. Oh, E. Roumanas, J. Beumer 3rd.. Maxillofacial restoration after head and neck tumor therapy. Compend Contin Educ Dent.. 2007; 28:70p [ Links ]
— M.M. Abu-Serriah, D.A. McGowan, K.F. Moos, J. Bagg. Extra-oral craniofacial endosseous implants and radiotherapy. Int J Oral Maxillofac Surg.. 2003; 32:585p [ Links ]
— E.D. Roumanas, T.L. Chang, J. Beumer. Use of osseointegrated implants in the restoration of head and neck defects. J Calif Dent Assoc.. 2006; 34:711p [ Links ]
— A.C. Cheng, E.W. Leong, N.T. Khin, A.G. Wee, C.K. Fung, C.M. Lee. Osseointegrated implants in craniofacial application: current status. Singapore Dent J.. 2007; 29:1p [ Links ]
*This article can be read in its full version in the following page: http://www.medigraphic.com/facultadodontologiaunam
Received: July 2010; Accepted: August 2010











 texto en
texto en