Services on Demand
Journal
Article
Indicators
Related links
Share
Revista odontológica mexicana
Print version ISSN 1870-199X
Rev. Odont. Mex vol.17 n.3 Ciudad de México Jul./Sep. 2013
Case reports
Glenoid fossa fracture: case report
Carlos Alain Rodríguez Piña,* José Ernesto Miranda Villasana§
* Maxillofacial and Oral Surgeon, Private Practice, Veracruz, Veracruz, Mexico.
§ Professor in charge of the Oral and Maxillofacial Surgery Course, Regional Hospital Gral Ignacio Zaragoza, ISSSTE, Mexico DF, Mexico.
ABSTRACT
Emergency rooms have seen a gradual increase of patients afflicted by craniofacial fractures. Mandible fractures can be classified according to their anatomical location. The most frequent fractures are angle fractures (36.3%) and body of the mandible fractures (21.2%). Coronoid process fractures are uncommon (0.25%)1 Zygomatic arch, condylar or coronoid process fractures can mask a fracture of the glenoid fossa, since, clinically, there is restriction of mandibular movements. The case here presented is that of a 38 year patient afflicted with fractures of the maxillary-zygomatic complex, coronoid process as well as right glenoid fossa.
Key words: Glenoid fracture, facial trauma, coronoid process.
INTRODUCTION
Mandibular fractures are increasingly frequent lesions encountered in the emergency room. Anatomical location of a fracture greatly depends on amount of force and direction of the noxious agent. Lateral-medial forces exerted upon the mandible can result in a fracture at the impact site, as well as another fracture on the opposite side. Up to the present date, in spite of studies conducted on this subject, an explanation has not been found to clarify the manner in which the force of a certain trauma is directed towards the coronoid process or the glenoid fossa.
Lesions in the glenoid fossa are related to condylar fractures; both can be considered temporomandibular joint (TMJ) traumatic events. They are susceptible to develop sequels such as ankylosis, chronic pain as well as articulation dysfunctions.
From 1963 to 1985, 11 cases of glenoid fossa fractures had been reported. Treatments were varied, among which the following could be found: craniotomy with reduction or condylectomy, subcondylar osteotomy with inter-positional graft placement, condylectomies, elastic traction and division of the condyle at neck level, leaving the condylar head joined to the cranial fossa. Chuong in 1994 reported the case of a cranial fossa fracture due to impact of the condyle against its surface. This elicited total rupture of the retro-disk insertion triggering thus the anterior dislocation of the disk.2,3
CASE REPORT
38 year old male patient attending emergency room after a car accident which resulted in maxillofacial trauma.
CLINICAL CHARACTERISTICS
The patient's neurological state remained stable; from the clinical point of view, the following lesions were identified: unilateral ecchymosis on both eyelids, restriction of mandibular movements (14 mm approximate opening) as well as Battle's sign (Figures 1 and 2).
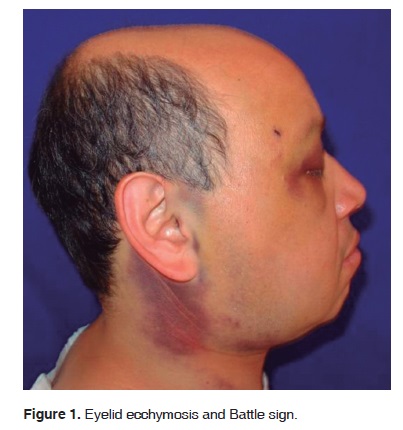
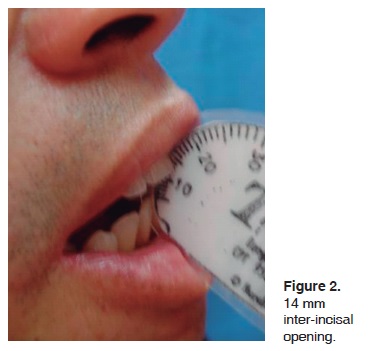
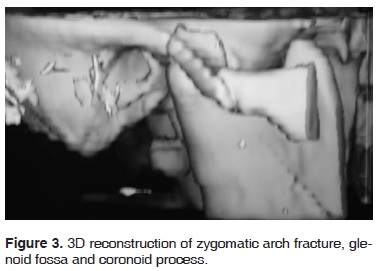
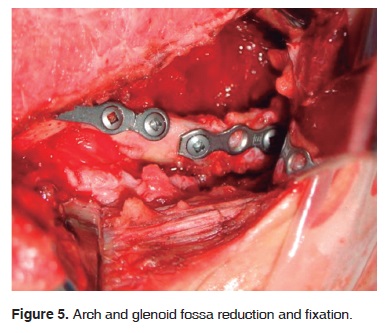
Surgical intervention with general anesthesia and naso-tracheal intubation with fiberscope was conducted five days after the trauma (Figure 3). Subciliary and Dingman approaches were undertaken to reduce and fixate zygomatic-maxillary fractures. Sub-mandibular and «E» modified retro-auricular approaches were then employed for mandibular and articular components (Figure 4). Unsteadiness of the coronoid processes was observed; this led to the decision to remove it. Glenoid fossa and zygomatic arch segments were aligned and fixated with titanium mini-plates (KLS Martin, L.P. Jacksonville, Florida) on the external aspect of the glenoid fossa (Figure 5).
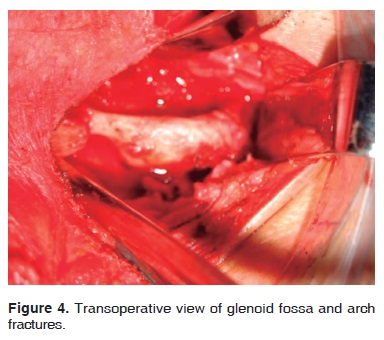
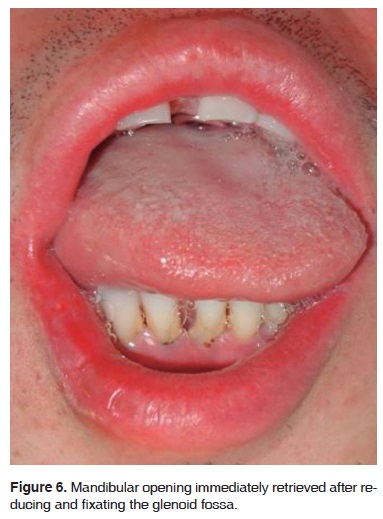
18 months after the surgical procedure, the patient evolved satisfactorily, at that point he enjoyed normal mandibular movement patterns (Figure 6).
DISCUSSION
Glenoid fossa fractures are rather infrequent and can be clinically confused with condylar fractures, due to the following: restriction and deviation of mandibular movements, pre-auricular pain and dental occlusal pattern alteration. During a physical examination, retro-auricular ecchymosis could suggest mid-floor cranial affection.2
An intra-cranial displacement of the condyle causes disruption of the glenoid fossa, thus, intracranial components such as meningeal or cerebrospinal elements could result affected. This would then enforce the need to conduct a multidisciplinary treatment, with special care to include a neurosurgery team.3
Age is a factor directly related to facial bone structure shape, size, and malleability. This is especially true in mandibular condyle, glenoid fossa and ear canal. All aforementioned elements must be taken into consideration so as to decide between use of a conservative or surgical treatment, as well as deciding upon which materials are to be used (plates, mini-plates, wire, silicon).3,4
Knowledge of anatomical relationships among condyle, disc and fossa is paramount. It is also necessary to bear in mind the possibility of damaging neighboring vascular structures as well as the ear canal. When the lamina dura is torn, the possibility of a subdural hematoma is greater since the posterior cerebral artery is damaged.4,5
Due to the anatomical proximity towards the medial and posterior regions, the fine bones of the ears (ossicles) are susceptible to lesions which impact the condyle towards the fossa.6,7
In normal situations, the condylar neck is thinner than the head, therefore, the former can fracture much more frequently than the latter. Some authors support the idea that the presence of disk and adjacent muscles dissipate traumatic forces, and this should be sufficient to prevent the condyles's intracranial projection.3,8
The fossa's medial portion is thin when compared to the lateral portion which is almost twice as thick. This portion is additionally reinforced by the zygoma and temporal support. Nevertheless, some anatomical alterations bear particular importance; this would be the case of a small, ovoid condyle which more fully transmits the force and breaks the glenoid fossa resistance thus eliciting fracture of the skull middle floor.8-11
The use of more specialized image studies such as tomography and tri-dimensional reconstruction and their incorporation in emergency rooms, have simplified diagnosis of glenoid cavity fractures, which heretofore was so difficult to achieve with only the use of conventional X rays.12-14
From the anatomical perspective, the articular eminence represents the TMJ's anterior limit. This structure is also susceptible to sustain isolated fractures such as reported by Radecki, Keith and Tay.15-17
CONCLUSIONS
In this particular case of glenoid fossa fracture, it was decided to perform reduction and fixation of glenoid fossa segments. This decision was reached after considering the significant displacement of segments and mandibular movement limitations. The fact that neither the condyle was fractured nor did it penetrate into the cranial cavity was particularly interesting.
Deciding to reduce and fixate the glenoid fossa must be based on factors such as degree of displacement of fracture segments and involvement of the medial cranial fossa as well as the patient's age.
Patients who have sustained TML trauma must be the subject of follow-up sessions. Adults might experience chronic pain or mandibular hypo-mobility, children are at greater risk of developing fibrous or bone ankylosis.18
The main objectives of glenoid fossa treatments must be directed to achievement of neurological stability, suitable control of bone segments in the skull, retrieval of mandibular mobility and dental occlusion, and, in the case of young patients, preservation of growth potential. Timely and strict physiotherapy are also paramount in order to achieve satisfactory long term results.
REFERENCES
1. Ogundare BO, Bonnick A, Bayley N. Pattern of mandibular fractures in a urban major trauma center. J Oral Maxillofac Surg. 2003; 61: 713. [ Links ]
2. Chuong R, Piper MA. Open reduction of condylar fractures in conjunction with meniscal repair. J Oral Maxillofac Surg. 1988; 46: 257. [ Links ]
3. Chuong R. Management of mandibular condyle penetration into the middle cranial fossa: case report. J Oral Maxillofac Surg. 1994; 52: 880. [ Links ]
4. Pirok DJ, Merrill RG. Dislocation of the mandibular condyle into the middle cranial fossa. Oral Surg. 1970; 29: 13. [ Links ]
5. Baldwin AJ. Superior dislocation of the intact mandibular condyle into the middle cranial fossa. J Oral Maxillofac Surg. 1990; 48: 623. [ Links ]
6. Anson BJ, McVay CB. Surgical anatomy. Philadelphia PA, Saunders, 1971; I: 134. [ Links ]
7. Antoniades K, Karakasis D, Daggilas A. Posterior dislocation of mandibular condyle into external auditory meatus: A case report. Int J Oral Maxillofac Surg. 1992; 21: 212. [ Links ]
8. Christiansen RC. Condylar penetration into the middle cranial fossa. J Craniomandibular Disorders. 1989; 3: 100. [ Links ]
9. Whitacre WB. Dislocation of the mandibular condyle into the middle cranial fossa: review of literature and report of a case. Plast Reconstr Surg. 1966; 38: 23. [ Links ]
10. Wish-Baratz S, Arebsburg S, Alter Z. Anatomical relationships and superior reinforcement of the TMJ mandibular fossa. J Craniomandibular Disorders. 1992; 6: 171. [ Links ]
11. Paulette SW, Trop R, Webb MD et al. Intrusion of the mandibular condyle into the middle cranial fossa: Report of a case in a 11 year old girl. Pediatric Dentistry. 1989; 11: 68. [ Links ]
12. Ianetti G, Martucci E. Fracture of the glenoid fossa following mandibular trauma. Oral Surg. 1980; 49: 405. [ Links ]
13. Copenhaver RH, Dennis MG, Kloppedal E. Fracture of the glenoid fossa and dislocation of the mandibular condyle into the middle cranial fossa. J Oral Maxillofac Surg. 1985; 43: 974. [ Links ]
14. Melugin MG, Indresano AT, Clemens SP. Glenoid fossa fracture and condilar penetration into the middle cranial fossa: report of a case and review of the literature. J Oral Maxillofac Surg. 1997; 55: 1342. [ Links ]
15. Radecki CA, Wolf SM. Solitary fracture of the articular eminence. Oral Surg Oral Med Oral Pathol. 1990; 69: 768. [ Links ]
16. Keith O, Jones GM, Shepherd JP. Fracture of the articular eminence: report of a case. Int J Oral Maxillofac Surg. 1990; 19: 79. [ Links ]
17. Tay ABG, Peck RHL. Solitary fracture of the articular eminence: a case report. J Oral Maxillofac Surg. 2001; 59: 808. [ Links ]
18. Silvennoinen U, Izuka T, Oikarinen M. Analysis of possible factors leading to problems after non surgical treatment of condylar fractures. J Oral Maxillofac Surg. 1994; 52: 793. [ Links ]
 Mailing address:
Mailing address:
José Ernesto Miranda Villasana
E-mail: ernestomiranda@prodigy.net.mx
Note
This article can be read in its full version in the following page: http://www.medigraphic.com/facultadodontologiaunam











 text in
text in 


