Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista mexicana de cardiología
versión impresa ISSN 0188-2198
Rev. Mex. Cardiol vol.26 no.4 México oct./dic. 2015
Review
Definitions, mechanisms and prognostic factors of right ventricular dysfunction in congenital heart disease
Análisis de la interdependencia ventricular en pacientes con cardiopatía congénita con disfunción sistólica y diastólica del ventrículo derecho
Horacio Márquez-González,* Lucelli Yáñez-Gutiérrez,* Diana López-Gallegos,* Christopher O Camargo-Zetina,* Irais C Ortiz-Vázquez,** Moisés Jiménez-Santos,*** Jaime Alfonso Santiago-Hernández,**** Homero Alberto Ramírez-Reyes,**** Carlos Riera-Kinkel*****
* Servicio de Cardiopatías Congénitas.
** Servicio Gabinetes.
*** Servicio de Tomografía.
**** Servicio de Hemodinamia.
***** División de Cirugía Cardiotorácica.
UMAE Hospital de Cardiología Centro Médico Nacional Siglo XXI.
Correspondence to:
Horacio Márquez-González
UMAE Hospital de Cardiología.
Av. Cuauhtémoc 330,
Col. Doctores, 06720,
Del. Cuauhtémoc, México, D.F.
Conmutador: 56276900, ext. 2203
E-mail: horacioinvestigacion@hotmail.com
ABSTRACT
The right ventricle (RV) and its dysfunction have been directly associated to negative prognosis in patients with ischemic heart disease. In congenital heart disease (CHD), right ventricle dysfunction results from volume (diastolic) and pressure (systolic) overload mechanisms, considering the many embryonic alterations they hold. Currently, there are no operational definitions to classify right ventricle dysfunction (RVD) in patients with congenital heart disease; and both prognostic or recovery factors are different to those in patients with right coronary ischemic disease. In this paper, we review causes of RVD, etiologic mechanisms and related prognostic variables.
Key words: Right ventricular dysfunction, congenital heart disease, systolic dysfunction, diastolic dysfunction.
RESUMEN
El ventrículo derecho (VD) y su disfunción han sido directamente asociados con un pronóstico desfavorable en pacientes con cardiopatías isquémica. En las cardiopatías congénitas (CC) la disfunción ventricular derecha resulta de mecanismos de sobrecarga, ya sea de volumen (diastólica) o de presión (sistólica), considerando las múltiples alteraciones embriológicas. No hay hasta el momento, una definición operacional para clasificar la disfunción del ventrículo derecho (DVD) en pacientes con CC y tanto los factores pronósticos como de recuperación son diferentes si se comparan con cardiopatía isquémica. En este artículo, se revisan las causas de DVD así como mecanismos etiológicos probables y factores pronósticos.
Palabras clave: Disfunción ventricular derecha, enfermedades congénitas del corazón, disfunción sistólica, disfunción diastólica.
INTRODUCTION
New surgical procedures have allowed the survival of patients with congenital heart disease (CHD); nowadays, global life expectance of these patients is barely 15% lower to that of healthy 45-year population.1 However, arrythmias and heart failure are among the main causes of death (20-35%).2
This increase regarding individuals with congenital heart disease, have allowed cardiologists to be more in touch with these patients that nowadays survive through adult life.
The causal mechanisms of ventricular dysfunction in CHD differ to those of adult patients with ischemia; that is why the knowledge of these mechanisms is important to understand RVD development.
Right ventricle (RV) has an important role on the pathophysiology of many congenital heart defects. Its importance has been underestimated for long time, with its relevance now coming to light. This paper reviews the role of RV on congenital heart disease.
RV EMBRIOLOGY
The embryonic development of the heart is fundamental for the understanding of CHD; on complex cases, these alterations are established prior to 7th week of development.3
The cardiogenic plate is originated on the 3rd week of gestation, between day 20 and 21. Afterwards, at the beginning of week 4, both endocardialtubes located at the lateral ends of the trilaminar embryo are fused originating the heart tube, which contracts for the first time on day 23.
From this moment on, the heart loop turns on itself forming a curl-like structure, where the primitive heart chambers can be found. Both auricles are connected to each other, and the primitive left auricle has continuity with the primitive ventricle, which will originate the left ventricle, thus forming the first atrioventricular connection. The primitive ventricle connects to the bulbuscordis (which will form the right ventricle) and ends on the truncus.4
The auricular septum starts and ends on the 5th week with the growth of the septum primum and secundum; meanwhile, at the beginning of week 6, the interventricular septum originates on the apex of the single ventricle.
After this, the truncus arteriosus starts to form: the inferior branch emerges from the endocardic cushions and the superior branch does so from the notochord migration. These branches turn 180o inside the truncus until they meet again and split the great vessels from the start.
By the end of week eight, the heart has completed its formation; at this time, congenital heart defects such as Tetralogy of Fallot (TOF), atrioventricular and ventriculoarterial discordances, pulmonary atresia and its variants(with and without interventricular septal defect) and atrioventricular valves pathology that causes univentricular hearts are already established (Figure 1).5,6
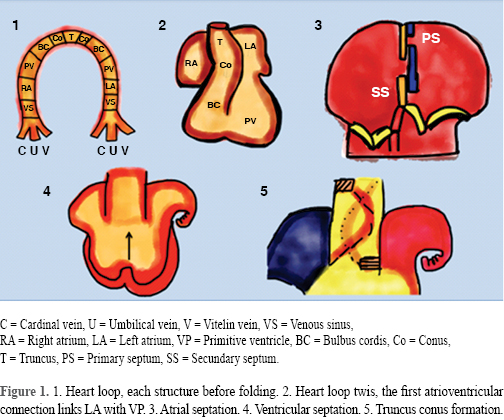
GROSS ANATOMY OF THE RIGHT VENTRICLE
To consider a heart chamber as a ventricle, the next three features are required:
• An Inlet, which will relate to the tricuspid valve (by embryonic rulea valve follows any ventricle). Pathologic conditions, such as classical tricuspid atresia or Ebstein anomaly will condition variations on size and development of the muscular component of the RV.7• A muscular component: The RV has the shape of a pyramid and has more trabeculas than the left ventricle (due to the existence of the 3 muscular bands: parietal, septomarginal and moderator band). CHD with alterations of RV inlet or outlet produce hypertrophy of muscular structures, reducing the ventricular area. Volume overload will present if there are interventricular septum defects as well.8
• Outlet: area from the muscular component of the RV to the pulmonary valve. It contains the infundibulum (site of defects such as TOF). Any circumstance that alters or obstructs this place will cause pressure increase within the RV.9
HEMODYNAMICS OF RV
The main function of RV is to receive the systemic venous return and to distribute it through a closed circuit to pulmonary circulation that will return to the left ventricle to be again distributed to the rest of the body.
To act as a bomb, the RV contracts through 3 separate mechanisms: 1) free-wall movement, 2) longitudinal fiber contraction (from the tricuspid valve towards theapex) and 3) horizontal fiber traction from the free wall towards the interventricular septum (the latter synergistic with the left-ventricle, LV, contraction). Unlike the contralateral ventricle, the RV has not an energetic rotation contraction because it has not a circular shape, and because the pressure to overcome is under the systemic one.10
It can be concluded that the RV exerts a smaller contraction force and time because of the fact that the resistance to beat in almost a third lower from the systemic one.
CHANGES ON CONGENITAL HEART DISEASE
On pathological conditions such as right coronary ischemia, the sudden damage of the RV causes acute dysfunction that will result on heart dilation and failure to deviate blood flow towards the pulmonary riverbed, thus causing LV dysfunction by reducing preload.11
On the particular case of CHD, the damage mechanism is established from birth, and this vicious mechanic causes a series of shape and function changes inside the RV, that will explain why these patients have to be analyzed in a different way that those with ischemia.
Right ventricle dysfunction (RVD) in CHD is divided in two types:
• Systolic dysfunction: Or by pressure increase; caused by obstruction to the outlet of the RV on CHD such as TOF, pulmonary atresia with interventricular septal defect, pulmonary valve or infundibular stenosis and Ebstein anomaly. All of these CHD cause after load increase of the RV; the increase on resistance that the heart must overcome results on concentric ventricle hypertrophy.12,13• Diastolic dysfunction: Or by volume overload; includes conditions such as interatrial and interventricular defects, patent ductus arteriosus, coronary fistulas towards the RV or anomalous pulmonary venous connection. These CHD cause a left-to-right shunt that diverts more volume towards the RV, with increase on the pulmonary bed resulting on pulmonary arterial hypertension; the ventricle will present diastolic pressure increase.14,15
Both mechanical principles are not mutually excluding, and could coexist on the same patient on the evolution of heart disease. We didn't include univentricular hearts because the anatomical, functional and hemodynamical alterations make classification in any type difficult (Figure 2).

NEED OF A DEFINITION
In 1963, the World Health Organization (WHO) defined RV claudication as the hypertrophy resulting from heart conditions that affect pulmonary structure and function;16 recently, the term dilation of RV has been added to this definition.17
Right ventricular dysfunction (RVD) is yet an unexplored ground, especially in CHD that relies on both the mechanisms previously explained.18
Staging of functional class has a direct proportional relationship with right and left ventricular claudication.19 Vizzardi E and cols20 defined for their association study of echocardiographic factors with RVD exclusively the following: Functional Class over II by the New York Heart Association (NYAH), hemodynamic decompensation episodes over six months and the need of diuretic therapy.20,21 On table I, some definitions of RVD used by some authors in different conditions are shown; these can vary hence the need to have a standard definition that will allow to identify RVD worldwide is evident.
CHANGES OF RVD ON THE CHD PATIENT AFTER CORRECTIVE SURGERY
New surgical techniques have allowed the increase of survival rates in patients with CHD. Changes on the primary lesion of each CHD allow ventricles to adapt and recover a near-to-physiological condition. Although some basic research studies have shown that changes of the myocardiac fiber from the original lesion are irreversible, it is currently acknowledged that there is an adaptation of muscle fibers that can make it return to a basal-like state.
Also, these type pf patients have other diseases associated to surgical procedures, such as residual defects, atrioventrocular block, valve disease or fistulas that could affect RV dynamics.22
FACTORS ASSOCIATED TO RVD PROGNOSIS
A great number of studies have investigated the prognostic variables associated to the development or recovery from RVD:
• Clinical: Huxley and colsanalyzed the presence of clinical variables for the development of RVD on open population; they found that lasting tachycardia with an odds ratio (OR) of 2.09 (IC-95%, 1.07-4.1) or resuscitation maneuvers with an OR = 4.20 (IC 95%, 2.21-7.9). An asian multicentric study which enrolled 543,694 participants, associated predictive factors for right or left chronic heart failure. Such risk factors were: body mass index (BMI) with a hazard ratio (HR) of 1.68 (1.34-2.11), a BMI over 30 with a HR of 1.69 (1.17-2.43), and female gender with a HR (1.02-1.89).23 Pedal edema, cervical veins distention, ascites and dyspnea were found to be early signs of RVD associated with bad pre-surgery prognosis in patients without CHD on symptoms questioning and physical exam.24 Supraventricular tachycardia with increase of cardiothoracic index are early signs of RV distortion related to early mortality increase. Other findings on physical exam, such as visible jugular pulse, the presence of a third heart sound, enlarged liver and Kussmaul sign in patients with ischemic lesion of RV have been statistically associated with worse prognosis.25• Echocardiography, CHD and RV: echocardiography is the preferred tool in the follow-up of patients with CHD, especially in those that involve RV. The standardized measurements of RV function and structure have shown a predictive power on clinical practice, especially on patients with pulmonary arterial hypertension (PAH). The tricuspid anular plane systolic excursion (TAPSE) less than 18mm on patients with PAH has a HR = 5.7 to predict death in a 1-2 year period.26 The Tei indexon RV has a HR of 1.3 for each increase unit to predict mortality on post-op patients and transplantation patients with values > 0.83, showing a death-free probability less than 4% for a 5 year period.27 Specifically, on patients with CHD and Eisenmenger syndrome, independence to predict mortality has been shown, auricular area > 25 cm2 (HR = 5.91, IC-95% of 2.6-11), relationship between right and left auricle over 1.5 (HR = 8.9, IC-95% of 2.9-27) and right auricle pressure over 10 mmHg (HR = 4.6, IC-95% of 1.59-11.5).28
• CHD and PAH: PAH is defined as the mean arterial pulmonary pressure over 25 mmHg or systolic at rest over 30 mmHg. Septal or interventricular defects are the most common cause of CHD; they coexist with a volume increase on the pulmonary bed, thus conditioning PAH.
In ICUs, RVD in patients with these conditions mortality is > 40% when compared to those without RVD. Despite accurate selection protocols may help to determine the best surgical candidates, post-op PAH crisis presents in 20% of cases. There is little information about these patients after shunt correction, but most evidence concludes that with more exposition time to volume overload in pulmonary bed, there is less probability for recovery.29 Hypertrophy of RV occurs when its walls are persistently overloaded with volume; if this phenomenon continues, dilation will occur. In the post-surgery period, when the RV is "stunt" because of manipulation, the ability for contraction decreases, causing decrease of cardiac output, conditioning heart failure.
• Ventricular interdependency (VI): Defined as the relation between both ventricles (the structure and function of one can determine the other).30 This phenomenon was initially described on left valve heart disease, specifically on cases of regurgitation that conditioned retrograde overload to pulmonary bed (thus affecting RV). Borrayo and cols described in a sample of patients with right coronary ischemia this phenomenon (RV to LV), also affecting left chambers function.31 Patients with CHD (prolonged RV damage) behave differently from those with ischemic damage; that is why concepts of RVD cannot be used in a general way. There are animal models that have tried to explain this association; concluding that VI is related to the mechanism of RVD; meaning that in systolic failure of RV, pressure increase on the RV outlet causes hypertrophy of its wall, causing systolic pressure to be the same as the one in the RV, increasing oxygen requirements and coronary flow that can be decreased in the RV, causing less contraction force.32 On diastolic dysfunction, volume overload causes chamber dilation of the RV, that can displace the interventricular septum and cause obstruction on the RV outlet, also reducing preload.27 This mechanism is not entirely pure; this can be explained by the fact that some CHD such as TOF have septal defects and outlet obstruction in which VI has a mixed cause. VI remains still as an unexplored topic in CHD, and requires investigation.
• Liver function: There is a direct relationship between RV and liver, owed to flow continuity (previously described in terms of cardiac cirrhosis, heart-liver failure).33 CHD that cause liver failure are those that cause an increase on ventricular pressure by volume, such as: tricuspid regurgitation, post-op Fontan patients, pulmonary atresia with septal interventricular defect. Retrograde volume increase on venous space causes an increase on pressure, resulting on perisinusoidal edema, endothelial degeneration and remodeling. Initially inflammation causes the release of liver enzymes (AST, ALT, LDH); on chronic stages, there is a dysfunction on liver metabolism: albumin and blood glucose alterations.34 Cowger and cols found an OR of 1.86 (1.02-3.4) with albumin levels below 3 g/dL, differences between LDH levels with an OR of 1.001 (1-1.002), SGTP > 80 UI/L with an OR of 3.2(1.6-6-25) and increases of total bilirubin levels > 2 mg/dL, OR of 3.59 (1.8-7.1) in patients that developed RVF after placing a left ventricle-support device.23
• Natriuretic peptides (NP): These are peptidic substances of similar structures but genetically different. There are 4 types: atrial (ANP), brain (BNP) both of cardiac origin; C-type (CNP; of endothelial origin) and recently discovered D-type (DNP), found in snakes. Those useful from a clinical perspective are ANP and BNP.35 CHD characteristically have effort limitation, related to heart failure syndrome (Cyanotic CHD and specially patients with Fontan circulation) that cause an increase on this effort limitation and also in neurohormonal activation. Law and cols36 showed that BNP values were increased on patients with Fontan procedure that had an increase on filling pressures (RV or LV) and more severe disease (according to the score that considers dyspnea with routine activities, need of hospitalization and/or use of IV vasoactive drugs or diuretics for the treatment of heart failure). By applying a cut level of 40 pg/mL, BNP sensitivity to detect heart disease associated with ventricular dysfunction was 85% with an 81% specificity, a positive predictive value of 92% and a negative predictive value of 68%.37
CAN RVD BE A RECOVERING CONDITION?
The mechanism of function recovery in RVD is not completely understood. The myocardium has the ability of remodeling and volume adaptation, once the factors that caused failure are corrected. In chronic heart failure, remodeling mechanisms are described:38 cellular hypertrophy, myocites changes on excitation-contraction mechanism, loss of myofilaments (myocytolysis), β-adrenergic desensibilization, abnormal myocardium metabolism due to mitochondrial alterations and loss of cytoskeleton.
Actual theories support the fact that timely management of ischemic lesions and antihypertensive and pulmonary anti-congestion treatment could favor myocardial cell to adapt to lesion and "recover" its normal condition.
There are no studies that evaluate heart remodeling after surgery in CHD. An asian study analyzed recovery form left ventricular failure after acute infarct through measuring prognostic factors al time 0 (event), 2 weeks and 6 months after. This study found that the associated factors in the multivariate analysis were:39 ejection fraction of RV, mitral regurgitation decrease, diastolic ventricular diameter of RV and dosage of beta blockers. We consider that these variables could be used to evaluate recovery from ventricular failure in CHD.
CONCLUSIONS
RVF in CHD is a reality directly associated with the prognosis of these patients. This review allows us to reflect on the necessity to perform causality and prognosis studies on this topic that will help us answer research questions and also, that the data obtained from these future studies will have a positive impact on survival and life quality of patients with CHD.
REFERENCIAS
1. Zomer C, Vaartjes I, Uiterwaal C, van der Velde ET, Lambert FM et al. Circumstances of death in adult congenital heart disease. International Journal of Cardiology. 2012; 154: 168-172. [ Links ]
2. Rudiski LG, Lai WW, Afilalo J, Hua L, Handschumacher M, Chandresekaran K et al. Guidelines for echocardiographic assessment of the right heart in adults: A report from the ameriacan society of Echochardiography. J Am Soc Echocardiogr. 2010; 23: 685-713. [ Links ]
3. Gómez-Gómez M, Danglot-Banck C, Santamaría-Díaz H, Riera-KinkelC.Desarrollo embriológico y evolución anatomofisiológica del corazón (Primera Parte). Rev Mex Pediatr. 2012; 79: 92-101. [ Links ]
4. Moorman A, Webb S, Brown NA, Lamers W, Anderson RH. Development of the Heart: formation of the cardiac chambers and arterial trunks. Heart. 2003; 89: 806-814. [ Links ]
5. Salazar-García M, Sánchez-Gómez C, Contreras-Ramos A, Carrillo-Ávalos BA, Revilla-Monsalve MC, Palomino-Garibay MA. Los segmentos cardiacos primitivos, su implicación en la cardiogénesis normal aplicada a la cardiología pediátrica. Arch Cardiol Mex. 2006; 76: S46-57. [ Links ]
6. Espínola-Zavaleta N, Muñoz-Castellanos L, González-Flores R, Kuri-NivónM.Tronco arterioso común en adultos. Arch Cardiol Mex. 2008; 78: 210-216. [ Links ]
7. Muñoz-Castellanos L, Martinez-Ascencio ME, Kuri-Nivon M. Estudio morfopatológico de 101 corazones portadores de defecto septal interventricular. Arch Cardiol Mex. 2005; 75: 393-401. [ Links ]
8. Muñoz-Castellanos L, Kuri-Nivon M. Doble salida de ventrículo derecho. Enfoque embriológico. Arch Cardiol Mex. 2012; 82: 273-281. [ Links ]
9. Muñoz-Castellanos L, Ramírez-Marroquín S, Kuri-Nivon M.Tetralogía de Fallot con atresia pulmonar: Morfopatología y anatomía quirúrgica. Arch Cardiol Mex. 2010; 80: 141-153. [ Links ]
10. Ho SY, Nihoyannopoulus P. Anatomy, echocardiograhpy, and normal right ventricular dimension. Heart. 2006; 92: i2-i13. [ Links ]
11. Petitjean C, Rougon N, Cluzel P. Assessment of myocardial function: a review of quantification methods and results using taffed MRI. J Cardiovasc Magn Reson. 2005; 7: 501-516. [ Links ]
12. Lee CY, Chang SM, Hsiao SH, Tseng JC, Lin SK, Liu CP. Right heart function and scleroderma: insights from tricuspid annular plane systolic excursion. Echocardiography. 2007; 24: 118-125. [ Links ]
13. Segovia C. Etiología y evaluación diagnóstica en la insuficiencia cardiaca. Rev Esp Cardiol. 2004; 57: 250-259. [ Links ]
14. Giunta A, Tirri E, Maione S, Cangianiello S, Mele A, De Luca A et al. Right ventricular diastolic abnormalities in systemic sclerosis. Relation to left ventricular involvement and pulmonary hypertension. Ann Rheum Dis. 2000; 59: 94-98. [ Links ]
15. Greyson C. Pathophysiology of right ventricular failure. Crit Care Med. 2008; 36: S57-S65. [ Links ]
16. Guadalajara-BooJF.Entendiendo la insuficiencia cardíaca. Arch Cardiol Mex. 2006; 74: 431-477. [ Links ]
17. Corson P, Anand F, Remme WJ, Cody R. Mode of death in advance heart failure the comparition of medical, pacing and desfibrillation therapy is heart failure trail. J Am Coll Cardiolgy. 2005; 46: 2329-2334. [ Links ]
18. Cho YK, Ma JS. Right ventricular failure in congenital heart disease. Korean J Pediatr. 2013; 56: 101-106. [ Links ]
19. Cleland JG, Daubert JC, Erdmann E, Freemantle N, Gras D, Kappenberger L, Tavazzi L. Cardiac resynchronization-heart failure (CARE-HF) study investigators. The effect of cardiac resynchronization on morbidity and mortality in heart failure. N Engl J Med. 2005; 352: 1539-1549. [ Links ]
20. Vizzardi E, D'Aloia A, Caretta G, Bordonali T, Bonadei I, Rovetta R et al. Long-term prognosis value of longitudinal strain of right ventricle in patients with moderate heart failure. Hellenic J Cardiol. 2014; 55: 150-155. [ Links ]
21. Cowger MJ, Koelling TM, Pagani FD, Aaronson KD. The right ventricular failure risk score: a pre-operative tool for assessing the risk of right ventricular failure in left ventricular assist device candidates. J Am Coll Cardiol. 2008; 51: 2163-2172. [ Links ]
22. Bronicki RA, Chang AC. Management of the postoperative pediatric cardiac surgical patient. Crit Care Med. 2011; 39: 1974-1984. [ Links ]
23. Huxley RR, Barzi F, Woo J, Giles G, Lam TH, Rahimi K et al. A comparison of risk factors for mortality from heart failure in Asian and non-Asian populations: an overview of individual participant data from 32 prospective cohorts from the Asia-Pacific Region. BMC Cardiovascular Disord. 2014; 14: 61. [ Links ]
24. Matthews JC, McLaughlin V. Acute right ventricular failure in the setting of acute pulmonary embolism and chronic pulmonary hypertension; a detailed review of the pathopysiology, diagnosis and managment. CurrCardiol Rev. 2008; 4: 49-59. [ Links ]
25. Rubin LJ, Badesh DB. Evaluation and management of the patient with pulmonary arterial hypertension. Ann Intern Med. 2005; 143: 282-292. [ Links ]
26. Forfia PR, Fisher MR, Mathai SC. Tricuspid annular displaccement predict survival in pulmonary hypertension. Am J Respir Crit Care Med. 2006; 174: 1034-1041. [ Links ]
27. Yeo TC, Dujardin KS, Tei C. Value of Doppler -derived index combining systolic and diastolic time intervals in predicting outcome in primary pulmonary hypertension. Am J Cardiol. 1998; 81: 1157-1161. [ Links ]
28. Moceri P, Dimopoulus K Liodakis E, Germanakis I, Kempny A, Diller GP et al. Echocardiographic predictos of outcome in Eisenmenger syndrome. Circulation. 2012; 126 (12): 1461-1468. [ Links ]
29. Ryan J, Huston J, Shelby K, Hatton N, Bowman L, Tian L et al. Right ventricular adaptation and failure in pulmonary arterial hypertension. Can J Cardiol. 2015; 31: 391-406. [ Links ]
30. Taylor R, Covell J, Sonnenblick E, Ross J. Dependence of ventricular distensibility on filling of the opposite ventricle. Am J Physiol. 1967; 213: 711-718. [ Links ]
31. Borrayo-Sánchez G, Contreras-Rodríguez A, Careaga-Reyna G, Antezana-Castro J, Argüero-Sánchez R. Interdependencia ventricular sistólica con el desplazamiento del plano auriculoventricular en pacientes con primer infarto del miocardio. Evaluación y propuesta de clasificación. Cir Ciruj. 2004; 72: 465-470. [ Links ]
32. Hoffman D, Sisto D, Frater RW, Nikolic SD. Left-to-right ventricular interaction with a non contracting right ventricle. J Thorac Cardiovas Surg. 1994; 107: 1496-1502. [ Links ]
33. Mahrous-Foudad Y, YehiaR. Hepato-cardiac disorders. World J Hepatol. 2014; 6 (1): 41-54. [ Links ]
34. Wong F, Villamil A, Merli M, Romero G, Angeli P, Caraceni P. Prevalence of diastolic dysfunction in cirrosis and its clinical significance. Hepatology. 2011; 51 (Suppl 1): A475-A476. [ Links ]
35. Kalra PR, Clague JR, Bolger AP, Anker SD, Poole-Wilson PA, Struthers AD et al. Myocardial production of C-type natriuretic peptide in chronic heart failure. Circulation. 2003; 107: 571-573. [ Links ]
36. Ir A, Bar-Oz B, Perles Z. N-terminal pro-B-type natriuretic peptide: reference plasma levels from birth to adolescence, elevated levels at birth and in heart diseases. Acta Paediatr. 2004; 93: 603-607. [ Links ]
37. Ohuchi H, Takasugi H, Ohashi H. Stratification of pediatric heart failure on the basis of neurohormonal and cardiac autonomic nervous activities in patients with congenital heart disease. Circulation. 2003; 108: 2368-2376. [ Links ]
38. Mann D, Barger P, Burkhoff D. Myocardial recovery and the failing heart: myth, magic o molecular target? J Am Coll Cardiol. 2012; 60: 2465-2472. [ Links ]
39. Duan HY, Wu XS, Han ZH, Guo YF, Fang SJ, Zhang XX et al. Factors influencing recovery of left ventricular structure in patients with chronic heart failure. Chin Med J (Engl). 2011; 124 (18): 2868-2873. [ Links ]
Nota
Este artículo puede ser consultado en versión completa en: http://www.medigraphic.com/revmexcardiol














