Servicios Personalizados
Revista
Articulo
Indicadores
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Salud Pública de México
versión impresa ISSN 0036-3634
Salud pública Méx vol.51 supl.4 Cuernavaca ene. 2009
ORIGINAL ARTICLES
Energy and nutrient intake among Mexican school-aged children, Mexican National Health and Nutrition Survey 2006
Consumo de energía y nutrimentos en niños mexicanos en edad escolar, Encuesta Nacional de Salud y Nutrición 2006
Mario Flores, MD, MSc; Nayeli Macías, MSc; Marta Rivera, MSc; Simón Barquera, MD, MSc, PhD; Lucía Hernández, MSc; Armando García-Guerra, MSc; Juan A Rivera, MSc, PhD
Centro de Investigación en Nutrición y Salud, Instituto Nacional de Salud Pública. Cuernavaca, Morelos, México
ABSTRACT
OBJECTIVE: To estimate energy, nutrient intake and diet adequacy in school-aged children based on the Mexican National Health and Nutrition Survey 2006 (ENSANUT 2006).
MATERIAL AND METHODS: Food intake data from food frequency questionnaires was analyzed for 8 716 children aged 5 to 11 years. Energy and nutrients intake and adequacy were obtained. Comparisons were made at regional, urban/rural areas, socioeconomic status (SES) and nutrition status (body mass index and height/age).
RESULTS: Median energy intake was 1501 kcal/d (percent adequacy: 88.0). Overweight and obesity prevalence was 25.5%. Stunting prevalence was 10%. Children at lowest SES, indigenous and from rural communities showed the highest inadequacies for vitamin A, folate, zinc, and calcium. Overweight children and those highest SES had higher risk of excessive intakes.
CONCLUSIONS: Coexistence of over and undernutrition reflects a polarized model of nutrition transition among Mexican children.
Key words: diet; micronutrients; malnutrition; nutrition surveys; children; Mexico
RESUMEN
OBJETIVO: Estimar el consumo y adecuación de energía y nutrimentos en niños escolares mexicanos que participaron en la Encuesta Nacional de Salud y Nutrición 2006 (ENSANUT 2006).
MATERIAL Y MÉTODOS: Se analizaron datos de frecuencia de consumo de alimentos en 8 716 niños de entre 5 y 11 años de edad. Se calcularon la ingesta y la adecuación de energía y nutrimentos. Se hicieron comparaciones por región, área urbana/rural, nivel socioeconómico (NSE) y estado nutricio (índice de masa corporal y talla/edad).
RESULTADOS: La mediana de ingestión de energía fue 1 501 kcal/día (% adecuación 88.0); 25.5% de los niños tuvieron sobrepeso u obesidad; 10%, retardo en talla. Los niños con menor NSE, los indígenas y los de comunidades rurales mostraron mayores inadecuaciones dietarias de vitamina A, folato, zinc y calcio. Los niños con sobrepeso y los de mayor NSE presentaron más riesgo de ingestiones excesivas.
CONCLUSIONES: La coexistencia de malnutrición por exceso y por deficiencia evidencia una transición nutricional polarizada en niños mexicanos.
Palabras clave: dieta; micronutrientes; desnutrición; encuestas nutricionales; niños; México
A series of nationally representative health and nutrition surveys (1988, 1999 and 2006) have shown a "polarized model of nutrition transition" in Mexico.1,2 This nutrition transition model is characterized by a rapid increase in nutrition-related chronic diseases and a reduction of infectious diseases and nutritional deficiencies.3
At the same time, excessive energy intakes and reductions in physical activity have been documented as possible contributing factors to the current epidemic of nutrition-related chronic diseases in Mexico.4
However, recent studies have shown that micronutrient deficiencies and iron deficiency anemia are still significant public health problems, affecting the most vulnerable age and gender groups.5,6 The consequences of nutrition deficiencies during childhood lead to growth retardation, decreased learning capacity and impaired immune response. Additionally, under-nourishment is causally related to a higher risk of chronic disease in adulthood.7,8 The coexistence of excess and deficiency conditions complicates the epidemiologic panorama in Mexico.
Nowadays, public health decision-makers have to deal with both sides of malnutrition, and this is the greatest challenge that the public health system in Mexico has to overcome.
The objective of this paper is to estimate and compare energy, nutrient intake and dietary adequacy according to biological, social and nutritional characteristics in a nationally representative sample of Mexican children 5 to 11 years of age.
Material and Methods
Data for this analysis were obtained from the Mexican National Health and Nutrition Survey 2006 (ENSANUT 2006). In summary, the ENSANUT 2006 included a probabilistic sample of 48600 households representative at national, regional and state levels. The sampling framework for selecting the households was provided by the National Institute of Statistics, Geography and Informatics (INEGI: Instituto Nacional de Estadística, Geografía e Informática). The ENSANUT 2006 sample included preschoolers, school-aged children, adolescents, adults and elderly males and females. The methods of the ENSANUT 2006 are described in detail elsewhere.9
For sampling and analytical purposes, the ENSANUT 2006 divided the country into four regions: north (Baja California, Baja California Sur, Coahuila, Chihuahua, Durango, Nuevo León, Sonora, Tamaulipas); center (Aguascalientes, Colima, Estado de México, Guanajuato, Jalisco, Michoacán, Morelos, Nayarit, Querétaro, San Luis Potosí, Sinaloa, Zacatecas); Mexico City, and south (Campeche, Chiapas, Guerrero, Hidalgo, Oaxaca, Puebla, Quintana Roo, Tabasco, Tlaxcala, Veracruz, Yucatán). Locations with 2500 or more inhabitants were classified as urban and those with 2 499 or less inhabitants were considered rural.
Data collection: To obtain dietary information, a random subsample of approximately one-third of the 48600 total households participating in the ENSANUT 2006 was selected. Dietary information was obtained for 9383 children from 5 to 11 years of age. A semi-quantitative food frequency questionnaire (FFQ) was administered to mothers or caregivers by standardized personnel.10 The questionnaire included 101 food items classified in 14 groups. The interviewers asked for the days of the week, times of the day, portion sizes and total of portions consumed for each food item during a seven-day period before the interview.9 Trained personnel converted the reported consumptions into grams or milliliters of food items at the time of the interview.
Individuals with energy intakes above 5 standard deviations or with less than 25% of adequacy were eliminated from the analysis (n= 667) because they were considered "outliers".11,12Aberrant food consumptions were manually reviewed and revised when a clear mistake was detected or eliminated if the value was not plausible. Reported atypical consumptions and adequacies were reviewed case by case and corrected when possible. If the value was not biologically plausible and information to correct it was not available, the data was eliminated.
To weigh the children, a Tanita scale (Tokyo, Japan, model 1631) with precision of ± 200 g was used. The accuracy of the scale was verified with a standard weight of 5.0 kg. The height was measured with a stadiometer (Seca, Mexico, City, model 206) that was placed perpendicular to a regular surface. All measurements were obtained by trained and standardized personnel using international protocols.13
The ENSANUT 2006 obtained socioeconomic information such as household conditions, basic services (such as water disposal and drainage) and possession of domestic appliances. With this information, an indicator of socioeconomic status (SES) was obtained by principal components factor analysis, as described elsewhere. The first single factor was used, which explained approximately 40% of the variance, and was divided into tertiles.12
To have an approximation of indigenous ethnicity, the mother or caregiver was asked if the child spoke an indigenous language. If the answer was "yes," the child was considered "indigenous."
Data analysis: Once the dietary information was collected, energy and nutrient consumption were calculated using a comprehensive database compiled from diverse sources.* To obtain the average of energy and nutrients consumed daily, the total obtained was divided by seven.
The percent adequacy was calculated using the reference values proposed by the United States Institute of Medicine (IOM).14-19 The estimated average requirement (EAR) was used to estimate protein, iron, zinc, vitamin C, retinol equivalents and folic acid adequacies.14-17 Dietary heme iron was calculated as the total daily quantity of iron originating from meat, poultry and fish, and non-heme iron was obtained by summing the iron from all other sources. In most cases, approximately 40% of iron from meat products is heme iron.18 For calcium, the adequate intake (AI) reference value was used.19 Energy adequacy was calculated using the estimated energy requirements,20 considering weight, height, age and physical activity. 10The energy requirement was calculated based on the body mass index (BMI) of well-nourished children.
To assess the risk of inadequate intakes, the proportion of children below the corresponding EAR was calculated. In a normal population, it is expected that 50% of individuals do not reach their EAR, thus the proportion of individuals above this number reflects the excess prevalence at risk.14-19
To estimate the risk of excessive macronutrient intakes, a percent contribution of macronutrients to total energy intake of > 65% was considered for carbohydrates, > 35% for fat, and > 30% for protein.12
Statistical analysis started with descriptive statistics as well as the evaluation of normality for continuous variables and simple tabulations for categorical variables. Due to the skewed distributions of energy and nutrient intakes and adequacies, medians and inter-quartile ranges were used for comparing them across categories of interest.
Sampling weights (expansion factors) were calculated as the inverse of the selection probability for each individual, according to the sampling scheme used.19 All calculations were weighted by expansion factors and adjusted for sampling (clustering) effects using the STATA 9.0 SVY module for complex surveys. A statistically significant level of 0.05 was used.
Screening for implausible reporters: After excluding outliers from the analysis, the remaining individuals (n= 8716) were classified as plausible or as under- or over-reporters using a ± 1 standard deviation (SD) cutoff for reported energy intake (rEI) as a percentage of predicted energy requirement (pER). Individuals were considered plausible reporters if rEI as a percentage of pER was within the ± 1 SD cutoff.21
Anthropometric indicators: A cutoff of -2.0 SD was used for classifying children as stunted based on individual height-for-age z-scores, according to international sex and age-specific references.22 BMI was calculated as weight in kilograms divided by height in meters squared. The sex- and age-specific cutoff values for BMI suggested by Cole were used to classify children's weight status as normal, overweight or obese. Cole's cut off values for children are equivalent to BMI classification of overweight (25 kg/m2) and obesity (30 kg/m2) in adults.23
Results
Data are presented for 8716 school children (ages 5 to 11 years) who had valid dietary information. This sample represents approximately 14.3 million school-aged children.
Sociodemographic and anthropometric characteristics of children are shown in Table I. Mean age was 8.21 ± 1.97 years. Distribution by sex was close to 50% each. About one-third of the children (29.4%) lived in rural areas. The proportion of indigenous children was 6.5% and mean BMI was 17.7 ± 3.21.

Chronic malnutrition (that is, stunting: height-for-age z-score< -2.0) was present among 10.0% of children. Prevalence of overweight or obesity was 25.5%.
Children with valid dietary information differed from children excluded from analysis with respect to sex (49.4% and 54.4% females, respectively) and age (mean age was 8.3 years and 8.0 years, respectively) (p< 0.05).
Energy and macronutrient intakes: Estimated daily energy and nutrient intakes and adequacies are shown in Table II by region and area of residency. The estimated median energy intake was 1 501 kcal/d (percent adequacy [PA]= 88%). Median protein intake was 42.5 g/d (PA= 202%) and median carbohydrate intake was 233 g/d (PA= 110%); median fat intake was 45.2 g/d (PA= 80%) and median fiber intake was 14.0 g/d (PA= 52%).
The highest energy and fat intakes were observed in Mexico City, with the exception of saturated fat and carbohydrates, which was higher in the northern region. A slight difference in carbohydrate intake was observed across regions and between rural and urban areas. The lowest energy, protein, saturated fat and fiber intakes were observed in the southern region. Children in rural areas had the highest consumption of fiber. Differences among regions were statistically significant (p< 0.05)
Micronutrients. Median total iron intake was 9.1 mg/d (PA= 186%) and median heme iron intake was 0.18 mg/d; national median vitamin A intake was 260.5 mcg RE/d (PA= 108%) and median vitamin C intake was 62.1 mg/d (PA= 214%); median folic acid intake was 167.6 mcg/d (PA= 82%), median zinc intake was 5.8 mg/d (PA= 108%) and median calcium intake was 763 mg/d (PA= 75%).
The highest intakes of iron, heme iron and folic acid were observed among children from the northern region. Children living in the Mexico City region had the highest intakes of vitamin A, vitamin C, zinc and calcium (p< 0.05).
The lowest iron, heme iron, vitamin C, folic acid and zinc intakes were observed in the southern region, whereas the lowest calcium intake was observed in the northern region. Micronutrient intakes were higher in urban areas as compared to rural areas (p< 0.05).
Evaluation of risk for inadequate energy and nutrient intakes. The prevalence of cases below the energy requirement and the percentage at risk of dietary inadequacies for micronutrients is presented in Table III, according to sociodemographic characteristics and nutritional status.
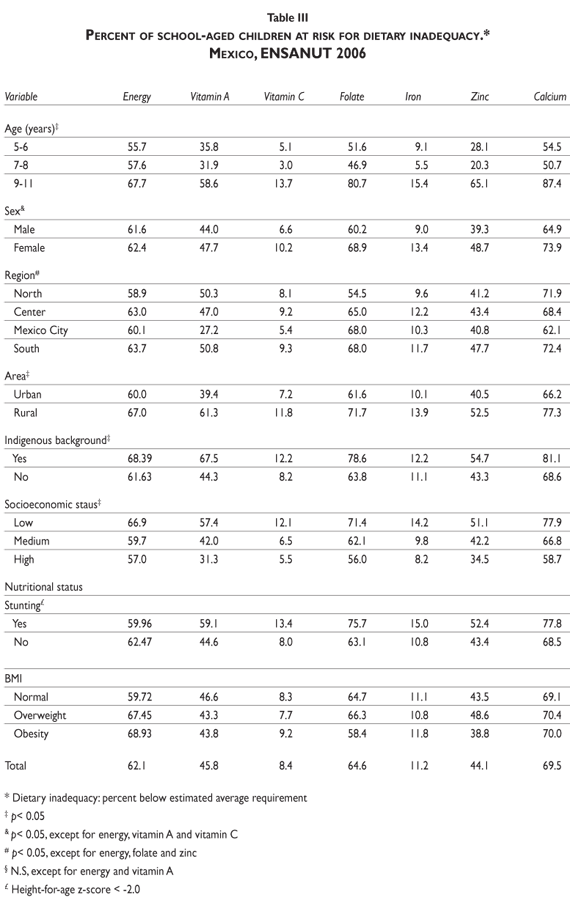
For energy and most nutrients, the proportion of children at risk of inadequacy was higher among older children (9 to 11 years), children from rural areas (with the exception of folic acid), indigenous children, and among children of low SES (p< 0.05).
Differences were also observed among regions; the southern region presented a higher proportion of children at risk, except for iron, which showed the highest prevalence of children at risk of inadequacy (p< 0.05) to be in the central region. The northern region had the lowest proportion of children at risk of dietary inadequacies of energy, folic acid, and iron (p< 0.05).
The proportion of children at risk of inadequate energy intake was higher among non-stunted children compared to children who had growth retardation, while the risk of dietary micronutrient inadequacies was higher among stunted children (p< 0.05).
In relation to BMI status, the prevalence of inadequate intakes of energy, vitamin C and iron were higher among children who were obese. Inadequate intakes of folic acid, zinc and calcium were more frequent among overweight children. The proportion of children at risk for inadequate vitamin A intake was higher among children with normal BMI.
The macronutrient composition of diets: The macronutrient composition of diets in terms of percent contribution to total energy intake is shown in Table IV; carbohydrates accounted for 63% of energy intake, protein accounted for 11.4% and fat, 28%.

The highest proportion of energy from carbohydrates was observed among children who were older, lived in rural areas, stunted children and children with low SES. The opposite occurred with the proportion of energy from fat, with the highest proportion being among children who were either overweight or obese. The percent contribution of saturated fat to total energy intake decreased with age, was higher in the northern region, and was related to better SES conditions.
Risk of excessive macronutrient intakes: The proportion of children at risk of relative excessive macronutrient (carbohydrate and fat) intakes according to sociodemographic characteristics and nutritional status is shown in the right panel in Table IV. There were no children who had excessive intakes of protein (> 30% of total energy intake). Moreover, there were no children who simultaneously had excess fat and excess carbohydrate intakes.
The proportion of excess carbohydrate intake was 44.7% and the prevalence of excess fat intake was 14.3%.
Opposite tendencies were observed in relation to the risk of excessive dietary intakes of carbohydrate and fat. For example, excessive carbohydrate intake (EC) increases with age, while the risk of excessive fat intake (EF) decreases (p< 0.05). The highest prevalences of EC were observed in the southern and central regions, which also had the lowest prevalences of EF. The highest prevalences of EF were observed in the northern and Mexico City regions (p< 0.05). EC was likely to be associated with low SES chronic malnutrition and indigenous ethnicity. On the other hand, EF was more frequent among non-indigenous children, children with better SES conditions, and among children who were overweight or obese (p< 0.05).
Notably, children who had carbohydrate intakes exceeding the recommendations also had higher risks of dietary insufficiency for energy and most micronutrients compared to children without excessive carbohydrate intakes (p< 0.05). These children also had higher fiber intakes compared to other children (p< 0.05) (results not shown).
Implausible reporters: Percent adequacy of energy intake among plausible, under- and over-reporters is shown in Table V. Of the children studied, nearly 70% were classified as plausible reporters, while roughly 14% were classified as under-reporters and roughly 17% as over-reporters. The proportion of under-reporters was higher among girls (14.5%) compared to boys (13.8%) (p< 0.001). A negative correlation was observed between BMI and percent adequacy of energy intake (r= -0.08, p< 0.001).
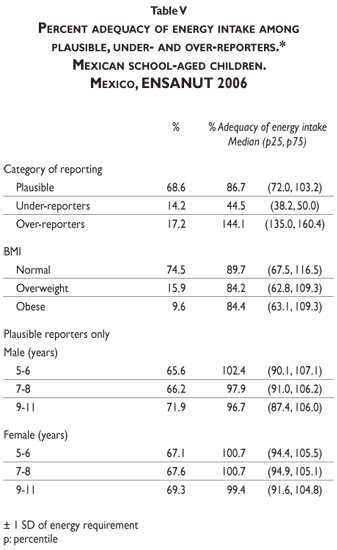
The proportion of under-reporters was higher among older children (9-11 years), which is also the group with the highest prevalence of overweight and obesity.
Notably, the percent adequacy of energy intake was lower among children with overweight or obesity compared to children with normal BMI (p< 0.001). This coincides with results shown in Table III, in which the proportion of children at risk of dietary energy inadequacy was higher among overweight and obese children. These findings suggest that energy under-reporting is related to overweight and obesity in this representative sample of Mexican school-aged children.
Discussion
Significant differences in energy, macronutrient and micronutrient intakes across regions, socioeconomic characteristics, and nutritional status were found in this sample of Mexican school-aged children who participated in the ENSANUT 2006.
A mixed picture has emerged for risks of dietary inadequacies –particularly of vitamin A, folate, zinc and calcium– among children of low SES, rural and indigenous children, as well as for risks of excessive fat intakes among those of higher SES and among children living in more developed regions.
Results are in accordance with a previous study of school-aged children, conducted by the author, which used data from the 1999 National Nutrition Survey (NNS-99).24 That study identified two contrasting dietary patterns: a "rural" pattern (43% of children) which was associated with poverty, high carbohydrate intake, and increased risk of dietary micronutrient deficiencies; and a "western" pattern which was related to excessive fat intake and an adjusted 45% increase in the risk of overweight or obesity. In that study, among children with a "rural" dietary pattern, corn tortillas and corn-based foods accounted for approximately 52% of energy intake, in contrast with 21% among children with a "western" diet, whereas with meat, poultry, dairy and industrialized foods the percent contribution to diet was higher among children with a "western" diet.
While in the present study we did not analyze foods, food groups or dietary patterns, one could argue that the observed clustering of dietary risks of deficiencies and excessive intakes could follow the same logic, and that both studies are consistent with a "polarized" model of nutrition transition in Mexican children.
Even though there are differences among methodologies, sampling, and timeframes, it is pertinent to compare the present findings with the results of the NNS-99 for the same age group.12 In general terms, energy and nutrient intakes seem to be higher in the present study than in those observed in the NNS-99. For example, median percent energy adequacy was 88% in the present survey, which contrasts with 69% in the NNS-99. In turn, vitamin A, vitamin C, iron and zinc median percent adequacies seem to have doubled since the NNS-99. However, a significant reduction in the risk of dietary inadequacies between the NNS-99 and the current survey was observed for vitamin C and iron only (47% vs. 8.4%, and 23% vs. 11%, respectively).
There are some aspects that have to be considered to explain the higher energy and nutrient intakes and adequacies observed in the current study in comparison with the previous nationally representative NNS-1999 data.
First, epidemiological studies based on different nationally representative surveys have documented that an actual increase in food consumption, as well as a significant shift towards energy-dense foods is occurring in Mexican population.4
Second, even though different portion sizes were used for different age groups, the FFQ used in the current survey may overestimate intakes to some degree, as it has been seen that longer FFQs tend to overestimate nutrient intakes compared to short FFQs. The FFQ used in this survey has 101 food items, whereas Block's FFQ for children (aged 8-17 years), for example, has only 77 food items.25
Third, improved and updated food composition tables that focus on micronutrients that have been a problem in the Mexican diet are now being used by the authors. The result of this updating process can lead to an apparent increase in micronutrient intakes.
Fourth, a considerable effort on the part of the Mexican government to fight malnutrition and micronutrient deficiencies among the poor is being carried out, and has been shown to be of considerable success. For example, a randomized effectiveness study showed that Progresa, a large-scale government program that distributes nutritional supplements to preschool children, is associated with better growth in height and lower rates of anemia in low-income rural Mexican infants.26 It is notable that consumption of these micronutrient-rich nutritional supplements by other family members –particularly by older siblings– has been reported,27 which could be having some impact on dietary micronutrient intakes by school-aged children. More importantly, other programs are currently in place to improve diets among the poor,28 while nationwide corn and flour micronutrient fortification programs could also be contributing to higher micronutrient intakes in the whole population.29
Fifth, median energy adequacy among children in the high SES was 96% in the current survey, compared to 80% for the same group in the NNS-99. One would expect that among those with better SES conditions, percent energy intake adequacy would be close to 100%. Thus, the previous 1999 survey could have underestimated energy and nutrient intakes.12
In relation to energy intake, in the present study energy intake under-reporting was positively associated with BMI, which coincides with other studies among children. However, the proportion of plausible reporters is higher in our study, while the proportion of under-reporters is 14% in the present study, which is much lower than the 34% observed in another study.30 A sensitivity analysis was carried out that included plausible reporters only (n= 5 939) and slight differences (< 3%) were observed in relation to most energy and nutrient intakes and adequacies at national and regional levels.
These considerations taken together support the validity of the current estimates.
One problem that deserves special attention is the case of iron intakes in this population. As has been shown, the risk of dietary iron deficiency seems to be low, roughly 11%, while the median percent adequacies are 185%. However, this percent adequacy is based on the recommendation by IOM,31 for which a bioavailability of 10% for heme iron was considered. Recent estimates of the bioavailability of iron in the diet of Mexican children suggest that a 10% bioavailability is high for this population due to the considerable presence of dietary inhibitors of iron absorption.16 Estimates of iron bioavailability in the diets of Mexican children, depending on different assumptions on body iron stores, showed that bioavailable iron in their diets ranged between 0.14 and 0.37 mg/d, which represents 2.7% to 6.1% of iron bioavailability.16 These findings indicate that the present study may underestimate the actual problem of dietary risk of iron deficiency in Mexican children.
In summary, the analysis of dietary data for school-aged Mexican children who participated in a national survey showed that risks of dietary deficiencies of vitamin A, folate, zinc and calcium continue to be significant public nutrition problems among this population. On the other hand, there seems to be no problem with energy and macronutrient intakes, in terms of dietary deficiency, among Mexican school-aged children. Moreover, certain groups of these children could be at risk of excessive energy and macronutrient intakes. This has to be taken into consideration when designing massive interventions aimed to reduce the risk of dietary deficiencies in Mexican children. To avoid these risks and related health problems in Mexican children, a nationwide effort to promote a healthy diet and lifestyle should be of the greatest priority.
References
1. Rivera J, Shamah T. Análisis crítico de la mala nutrición durante las últimas décadas en México: Resultados de niños. Salud Publica Mex 2007;49:E267-E269. [ Links ]
2. Popkin BM. The nutrition transition in low income countries: An emerging crisis. Nutr Rev 1994;52:285-298. [ Links ]
3. Drewnowski A, Popkin BM. The nutrition transition: New trends in the global diet. Nutr Rev 1997;55:31-43. [ Links ]
4. Rivera J, Barquera S, Campirano F, Campos I, Safdie M, Tovar V. Epidemiological and nutritional transition in México: Rapid increase of non-communicable chronic diseases and obesity. Public Health Nutr 2002;14:113-122. [ Links ]
5. Mejía F, Shamah-Levy T, Ramírez I, Rivera JA, Villalpando S. Prevalencia de anemia en niños de 1 a 12 años de edad: resultados de una encuesta probabilística nacional. Salud Publica Mex 2003;45:490-498. [ Links ]
6. Villalpando S, Montalvo-Velarde I, Zambrano N, García-Guerra A, Ramírez-Silva CI, Shamah-Levy T, et al. Vitamins A, and C and folic acid status in Mexican children under 12 years and women 12-49 years: a probabilistic national survey. Salud Publica Mex 2003;45 Suppl 4:S508-S519. [ Links ]
7. Engle PL, Black MM, Behrman JR, Cabral de Mello M, Gertler PJ, Kapiriri L, et al. International Child Development Steering Group. Strategies to avoid the loss of developmental potential in more than 200 million children in the developing world. Lancet 2007;369:229-242. [ Links ]
8. Dietz WH. Health consequences of obesity in youth: Childhood predictors of adult disease. Pediatrics1998;101:518-525. [ Links ]
9. Olaiz G, Rivera J, Shamah T, Rojas R, Villalpando S, Sepúlveda J. Encuesta Nacional de Salud y Nutrición 2006. Cuernavaca, México: Instituto Nacional de Salud Pública, 2006. [ Links ]
10. Ramírez-Silva CI, Mundo-Rosas V, Rodríguez-Ramírez SC, Vizuet-Vega NI, Hernández-Carapia N, Jiménez-Aguilar A. Encuestas dietéticas: recordatorio de 24 horas y frecuencia de consumo de alimentos. In: Shamah- Levy T, Villalpando- Hernández S, Rivera-Dommarco J. Manual de procedimientos para proyectos de nutrición. Cuernavaca, México: Instituto Nacional de Salud Pública, 2006:27-108. [Consulted 2009 April 29]Available at: http://www.insp.mx/Portal/insp_publica/proy_nutricion.pdf. [ Links ]
11. Barquera S, Rivera J, Espinosa-Montero J, Safdie M, Campirano F, Monterrubio E. Energy and nutrient consumption in Mexican women 12-49 years of age. Analysis of the National Nutrition Survey 1999. Salud Publica Mex 2003;45 Suppl 4:S530-S539. [ Links ]
12. Barquera S, Rivera J, Safdie M, Flores M, Campos-Nonato I, Campirano F. Energy and nutrient intake in preschool and school age Mexican children: National Nutrition Survey 1999. Salud Publica Mex 2003;45 Suppl 4:S540-S550. [ Links ]
13. Lohman T, Roche A, Martorell R. Anthropometrics standardization reference manual. Champaign (IL): Human Kinetics Books, 1988. [ Links ]
14. A Report of the Panel on Macronutrients, Subcommittees on Upper Reference Levels of Nutrients and Interpretation and Uses of Dietary Reference Intakes, and the Standing Committee on the Scientific Evaluation of Dietary Reference Intakes. Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein, and amino acids (macronutrients). Washington, DC: Institute of Medicine, The National Academies Press, 2005: 589-630. [ Links ]
15. Panel on Dietary Antioxidants and Related Compounds, Subcommittees on Upper Reference Levels of Nutrients and Interpretation and Uses of DRIs, Standing Committee on the Scientific Evaluation of Dietary Reference Intakes, Food and Nutrition Board, Institute of Medicine. Vitamin C. In: Dietary reference intakes for: Vitamin C, Vitamin E, selenium and carotenoids. Washington, DC: Institute of Medicine, The National Academies Press, 2000: 95-185. [ Links ]
16. Institute of Medicine. Dietary reference intakes for Vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium and zinc. Washington, DC: Institute of Medicine, The National Academies Press, 2000. [ Links ]
17. A Report of the Standing Committee on the Scientific Evaluation of Dietary Reference Intakes and its Panel on Folate, Other B Vitamins, and Choline and Subcommittee on Upper Reference Levels of Nutrients, Food and Nutrition Board, Institute of Medicine. Folate: In: Dietary reference intakes for: Thiamin, riboflavin, niacin, vitamin B6, folate, vitamin B12, pantothenic acid, biotin and choline. Washington, DC: Institute of Medicine, The National Academies Press, 2000: 196-305. [ Links ]
18. Tseng M, Chakraborty H, Robinson DT, Mendez M, Kohlmeier L. Adjustment of iron intake for dietary enhancers and inhibitors in population studies: Bioavailable iron in rural and urban residing Russian women and children. J Nutr 1997;127:1456-1468. [ Links ]
19. Standing Committee on the Scientific Evaluation of Dietary Reference Intakes, Food and Nutrition Board, Institute of Medicine. Calcium. In: Dietary reference intakes for: Calcium, phosphorus, magnesium, vitamin D and fluoride. Washington, DC: Institute of Medicine, The National Academies Press, 2000: 71-145. [ Links ]
20. Institute of Medicine. Energy. In: Dietary reference intakes for energy, carbohydrates, fiber, fat, protein and amino acids (macronutrients). Washington, DC: Institute of Medicine, The National Academies Press, 2005:107-264. [ Links ]
21. Huang T, Howarth N, Lin B-H, Roberts SB, McCrory M. Energy intake and meal portions: associations with BMI percentile in U.S. children. Obes Res 2004;12(11):1875-1885. [ Links ]
22. Kuczmarski RJ, Ogden CL, Grummer-Strawn LM, Flegal KM, Guo SS, Wei R, et al. CDC growth charts: United States. Advance data from Vital and Health Statistics; Num. 314. Hyattsville (MD): National Center for Health Statistics, 2000. [ Links ]
23. Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000;320:1240-1243. [ Links ]
24. Flores M, Rodríguez S, Macías N, Barquera S. Patrones dietarios de niños mexicanos en edad escolar. Brasil: Memorias Congreso de la Sociedad Latinoamericana de Nutrición, 2006. [ Links ]
25. Cade JE, Burley VJ, Warm DL, Thompson RL, Margetts BM. Food-frequency questionnaires: a review of their design, validation and utilisation. Nutr Res Rev 2004;17:5-22. [ Links ]
26. Rivera JA, Sotres-Alvarez D, Habicht JP, Shamah T, Villalpando S. Impact of the Mexican program for education, health, and nutrition (Progresa) on rates of growth and anemia in infants and young children: a randomized effectiveness study. JAMA 2004; 291:2563-2570. [ Links ]
27. Zarco A, Mora G, Pelcastre B, Flores M, Bronfman M. Aceptabilidad de los suplementos alimenticios del Programa Oportunidades. Salud Publica Mex 2006;48:325-331. [ Links ]
28. Gonzalez-Cossío T, Rivera-Dommarco J, Gutiérrez JP, Neufeld L, Rodríguez S, Gonzales D, et al. Evaluación del estado de nutrición de niños menores de 5 años y sus madres y gasto en alimentos de familias de localidades marginales de México. Recolección de datos del primer seguimiento 2005. Informe final. Cuernavaca, Morelos: Instituto Nacional de Salud Pública, 2005. [ Links ]
29. Hernandez M, Sousa V, Villalpando S, Moreno A, Montalvo I, Lopez-Alarcon M. Cooking and Fe fortification have different effects on Fe bioavailability of bread and tortillas. J Am Coll Nutr 2006;25(1):20-25. [ Links ]
30. Fiorito LM, Ventura AK, Mitchel DC, Smicklas-Wright H, Birch LL. Girls' dairy intake, energy intake and weight status. J Am Diet Assoc 2006;106:1851-1855. [ Links ]
31. Institute of Medicine. Dietary reference intakes for: Vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium and zinc. Washington, DC: Institute of Medicine, National Academies Press, 2000. [ Links ]
Received on: April 11, 2008
Accepted on: February 10, 2009
Danone de México provided an unrestricted grant which made this work possible.
Address reprint requests to: Dr. Mario Flores. Head of Department. Data analysis. Centro de Investigación en Nutrición y Salud. Instituto Nacional de Salud Pública. Av. Universidad 655, col. Santa María Ahuacatitlán. 62100 Cuernavaca, Morelos, México. E-mail: mflores@correo.insp.mx
* Instituto Nacional de Salud Pública. Database for nutritient values for food. Compiled by the Instituto Nacional de Salud Pública, 2004 (unpublished document).
‡ Stata 9.0. Stata Corporation. College Station, TX. USA. 2001.














