Servicios Personalizados
Revista
Articulo
Indicadores
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Salud Pública de México
versión impresa ISSN 0036-3634
Salud pública Méx vol.50 supl.2 Cuernavaca ene. 2008
ARTÍCULO DE REVISIÓN
Intellectual disability: definition, etiological factors, classification, diagnosis, treatment and prognosis
Discapacidad intelectual: definición, factores etiológicos, clasificación, diagnóstico, tratamiento y prognosis
Gregorio Katz, MD,I; Eduardo Lazcano-Ponce, MD, ScD.II
ICapacitación y Desarrollo Integral AC, Universidad Nacional Autónoma de México
IICentro de Investigación en Salud Poblacional, Instituto Nacional de Salud Pública. Cuernavaca, Morelos, México
ABSTRACT
Etiology and classification: Causal factors related with cognitive disability are multiples and can be classified as follows: Genetic, acquired (congenital and developmental), environmental and sociocultural. Likewise, in relation to the classification, cognitive disability has as a common denominator a subnormal intellectual functioning level; nevertheless, the extent to which an individual is unable to face the demands established by society for the individuals age group has brought about four degrees of severity: Mild, moderate, severe and profound. Diagnostic: The clinical history must put an emphasis on healthcare during the prenatal, perinatal and postnatal period and include the results of all previous studies, including a genealogical tree for at least three generations and an intentional search for family antecedents of mental delay, psychiatric illnesses and congenital abnormalities. The physical exam should focus on secondary abnormalities and congenital malformations, somatometric measurements and neurological and behavioral phenotype evaluations. If it is not feasible to establish a clinical diagnosis, it is necessary to conduct high-resolution cytogenetic studies in addition to metabolic clinical evaluations. In the next step, if no abnormal data are identified, submicroscopic chromosomal disorders are evaluated. Prognosis: Intellectual disability is not curable; and yet, the prognostic in general terms is good when using the emotional wellbeing of the individual as a parameter. Conclusions: Intellectual disability should be treated in a comprehensive manner. Nevertheless, currently, the fundamental task and perhaps the only one that applies is the detection of the limitation and abilities as a function of subjects age and expectations for the future, with the only goal being to provide the support necessary for each one of the dimensions or areas in which the persons life is expressed and exposed.
Key words: intellectual disability; etiological factors; classification; diagnosis; treatment and prognosis
RESUMEN
Etiología y clasificación: múltiples factores causales están relacionados con la discapacidad cognoscitiva y pueden clasificarse de la siguiente manera: genéticos, adquiridos, (congénitos y de desarrollo), ambientales y socioculturales. Del mismo modo, en cuanto a la clasificación, la discapacidad cognoscitiva tiene como común denominador un nivel de funcionamiento intelectual por debajo de lo normal; sin embargo, la medida en que una persona es incapaz de afrontar las demandas establecidas por la sociedad para su grupo de edad ha dado origen a cuatro grados de severidad: ligera, moderada, severa y profunda. Diagnóstico: el historial clínico debe hacer énfasis en el cuidado de la salud durante el periodo prenatal, perinatal y postnatal e incluir los resultados de todos los estudios previos, incluyendo un árbol genealógico de al menos tres generaciones y una búsqueda intencional de antecedentes familiares de retraso mental, enfermedades psiquiátricas y anomalías congénitas. El examen físico debe concentrarse en anomalías secundarias y en malformaciones congénitas, mediciones somatométricas, y evaluaciones del fenotipo neurológico y conductual. Si no es posible establecer un diagnóstico clínico, se deben hacer estudios citogenéticos de alta resolución en adición a las evaluaciones clínicas metabólicas. Si no se identifican datos anormales, el siguiente paso consiste en la evaluación de trastornos cromosómicos submicroscópicos. Prognosis: la discapacidad intelectual no es curable, sin embargo el prognóstico es bueno en términos generales cuando se usa como parámetro el bienestar emocional del individuo. Conclusiones: el tratamiento para discapacidad intelectual requiere de un enfoque amplio. Sin embargo, la tarea principal y quizás la única que tiene aplicación es la detección de las limitaciones y habilidades en función de la edad y expectativas para el futuro de la persona, con el único fin de proporcionar el apoyo necesario para cada una de las dimensiones o áreas en las que se expresa y expone la vida del individuo.
Palabras clave: discapacidad intelectual; factores etiológicos; clasificación; diagnóstico; tratamiento y prognosis
Intellectual disability (ID) is an abnormality that has enormous social effects; it not only affects the people who suffer from it but also the family and society as a group. Millions of people worldwide have intellectual disability and prevalence is calculated to be 1 to 3% in developed countries.1 In Mexico, according to INDESOL (National Social Development Institute) calculations, there are 2 925 000 persons with some type of intellectual disability.2 In spite of this fact, knowledge of its causes is very limited and the etiological diagnosis in developed countries is almost always established as being a little less than half of the subjects affected.3 The frequency with which exogenous and genetic causes are identified varies; some authors have reported proportions ranging from 17 to 47%.4,5 Of course these differences are attributed to the selection of the population studied, the degree of mental delay, the heterogeneity of study protocols, technological advances and case definitions. This article outlines basic concepts related to intellectual disability as a function of diagnosis, treatment and prognosis.
Definition
According to the tenth revision of the WHO (World Health Organization):
Intellectual disability (ID) is a disorder defined by the presence of incomplete or arrested mental development, principally characterized by the deterioration of concrete functions at each stage of development and that contribute to the overall level of intelligence, such as cognitive, language, motor and socialization functions; in this anomaly, adaptation to the environment is always affected. For ID, scores for intellectual development levels must be determined based on all of the available information, including clinical signs, adaptive behavior in the cultural medium of the individual and psychometric findings.
On the other hand, the American Association on Intellectual and Developmental Disabilities (AAIDD) indicates that in addition to a significantly sub-average intellectual functioning, concomitant limitations are observed in two or more areas of adaptive skills, described in table I, and the disorder presents itself before the age of 18.
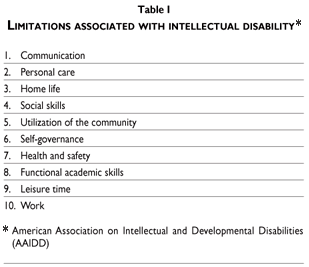
In summary, intellectual disability is characterized by evident limitations in intellectual functioning and adaptive conduct, the latter expressed as conceptual, social and practical adaptive skills. Therefore, for the study of ID, according to the AAIDD, five dimensions must be considered (table II), one of which was recently included: the dimension composed of participation, interaction and social networks. This definition not only agrees with the International Association for the Scientific Study of Intellectual Disability (IASSID), but also with the recent World Health Organizations International Classification of Functioning, Disability and Health (ICF).

Etiopathogeny
Causal factors related with cognitive disability are described in table III and can be classified as follows: genetic, acquired (congenital and developmental), environmental and sociocultural.

Genetic factors
Chromosomal or hereditary disorders6
The greatest number of cases are patients with Down syndrome,7 an anomaly that occurs in 15 of every 10000 births and is due to chromosome 21 trisomy or the translocation of chromosomes 21 and 15. Other much less frequent chromosomal abnormalities are those of the fragile X chromosome syndrome,8 Prader-Willi syndrome,9 Rett syndrome, neurofibromatosis,11 tuberous sclerosis,12 Lesch-Nyhan syndrome,13 adrenoleukodystrophy14 and other very rarely occurring related conditions.
Hereditary factors
Hereditary factors include phenylketonuria,15 galactosemy,16 Mowat-Wilson syndrome,17 Tay-Sachs disease,18 and glycogen deposit disease, among others. These illnesses can be easily diagnosed when intra-hospital births are involved, during which neonatal metabolic screening can be conducted; however, when the latter is not conducted a considerable risk is presented since such causal factors for mental delay are not identified.
Acquired factors
Congenital
Can be grouped as follows:
1. Metabolic: neonatal hypothyroidism;
2. Toxic: lead poisoning,20 fetal alcohol syndrome,21 prenatal exposure to substances;22 and
3. Infectious: rubella,23 Cytomegalic Inclusion Body Disease,24 syphillis,25 toxoplasmosis,26 simple herpes (genital type II).27
Developmental
During the prenatal period, possible pregnancy complications exist, such as toxemia28 and uncontrolled diabetes,29 intrauterine malnutrition,30 vaginal hemorrhages,31 placenta previa32 and umbilical cord prolapse.33
During the perinatal period, there are common birth complications: prolonged fetal suffering with neonatal anoxia,34 asphyxia related with suffocation,35 inadequate application of high forceps36 or a poorly applied Kristeller maneuver.37
During the postnatal period, complications are observed such as encephalopathy from hyperbilirubinemia (kernicterus),38 encephalic traumatism39 and infections40 (encephalitis and meningitis).
Environmental and sociocultural factors
Epidemiological studies have consistently reported a notable link between poverty and intellectual disability. The available evidence suggests that this connection reflects two distinct processes. The first establishes that a relation exists between poverty and exposure to a wide range of environmental and psychosocial factors;41 the second indicates that families with members who suffer from intellectual disability have an increased risk of catastrophic expenses that considerably affect poverty levels. These factors are direct causes of the disproportionate increase in the incidence of intellectual disability in developing countries.42 Interactions have been reported between scarcity and poor prenatal, perinatal and postnatal health care, adolescent maternity, family instability, poor natal health care due to multiple and inadequate caregivers and health professionals, low level of stimulation and education, in addition to infant mistreatment.
Classification
Cognitive disability has as a common denominator a subnormal intellectual functioning level; nevertheless, the extent to which an individual is unable to face the demands established by society for the individuals age group has brought about four degrees of severity:43 mild, moderate, severe and profound. The characteristics of individuals in these age groups have little in common with those of other age groups and, therefore, distinguishing the limitations of each one in order to establish intervention guidelines, is fundamental. Cognitive disability is classified according to the characteristics outlined in table IV.

Diagnosis
Subjects with intellectual disability and comorbidities, especially those that are psychiatric in origin, have less social capital than individuals with ID who do not have psychiatric disorders.44 In addition, the absence of legislation in developing countries, the lack of knowledge about ID, the stigmatization and discrimination as well as the lack of training and infrastructure for establishing a diagnosis significantly delays possibilities for intervention and the utilization of specific services.45 The cultural context establishes denial on the part of the parents who are faced with the possible diagnosis of intellectual disability. It is indisputable that parents take on the diagnosis of mental delay with great difficulty, to the extent that the doctor frequently chooses not to confort this reality in the attempt to avoid the intense pain that it represents. It is unquestionable that the acceptance of a condition that signifies a life of constant difficulties is not easy for anyone.
All parents expect to be gratified by their children and hope that they will be intelligent, brilliant students, triumphant and, subconsciously, expect then to become "a second, corrected and better version of themselves". Nevertheless, upon confirmation of the diagnosis, their expectations are destroyed becoming overwhelmed by a sense of loss, not to mention the obligation of having an unwanted child. This news often provokes feelings of guilt in the parents and outright aggression between them, in addition to hostile reactions toward the doctor; consequently, it is necessary to be prepared and to provide the support needed.
The initial reaction is denial. Then, during the first years, the parents justify the discrepancies during the critical development periods while becoming more demanding as the child grows up, without results. The impossibility of attaining the expected goals generates a great deal of frustration and can lead to serious errors in childrearing, which without doubt, significantly affects the psychological development of these children. As a result, parents must face the correct diagnosis so as to minimize the denial mechanism (among other issues that will be described later). A great deal of empathy is required on the part of the doctor when reporting the diagnosis. Parents need to perceive security and confidence from health professionals; know that they will not face the problem alone and that they will receive guidance throughout the long and arduous path.
If the deficit is notable, the diagnosis can be made earlier, but the effect is more devastating. It is necessary, therefore, to provide support for accepting the diagnosis; only in this way can the search for "magic cures" brought on by pain and denial be avoided. This not only provokes catastrophic expenses but also extremely traumatic experiences; each time, the failures become evident.
When there is organic evidence, the initial diagnosis and the need to confront the parents almost always falls on the gynecologists or pediatricians (neonatologists). If a moderate or mild mental disability is involved, the diagnosis is generally established by personnel in the field of education. A referral to a doctor is recommended only if an incorrect diagnosis is established, if behavioral problems are present or if the family requires guidance. On occasion, when a diagnosis is determined by the educational institution, a doctor will be consulted to corroborate the diagnosis or to advise the parents as to treatment for behavioral disorders that prevent the childs normal development in school or at home. In these cases, the use of instruments for the diagnosis is essential, such as psychometric tests, developmental scales, abilities and adaptive behavior tests or psychopedagogical tests. These instruments are highly useful for psychologists. Once the diagnosis is corroborated, the parents should be advised as to the existing abilities and the expectations on the part of the school or family, since an incompatibility could result in aberrant behavior.
In Down syndrome, establishing a diagnosis at birth is indispensable given that the characteristic features of this disorder are evident; consequently, once the grief is overcome, there is a greater tendency for acceptance on the part of the parents and society, which allows for less to be demanded of them. As for their intellectual capacity, there is a large discrepancy because it can vary from profound to mild disability, and in the case of mosaicism (partial trisomy), even an average intelligence is possible. Currently, some still believe that people with this syndrome live for just a few years however. Thanks to medical progress, the life expectancy is roughly 50-60 years of age, at which point many develop Alzheimers disease.
Another important group to mention is individuals who possess an intelligence quotient (IQ) between 70 and 85 points range (borderline) placing them in what is known today as limitrophe. Until the beginning of the 1980s they were considered to be subjects with mental delay, but since they did not present adaptation problems they were not considered to have a disability.
Nevertheless countries like Mexico, this population faces serious problems, especially in urban areas and mostly when they belong to socioculturally and economically competitive classes; school and work programs are designed for people with normal average IQ, which makes it very difficult to satisfy such expectations. Furthermore, given their functionality level, they can recognize their own limitations and generate a good deal of suffering with notable tendencies toward depression. This groups highest prevalence is found in rural areas with the most important causal factor being family heredity; therefore, the disorder in these cases does not result in serious conflicts because social and family expectations adapt to their abilities.
Clinical diagnosis
In the figure 1, a proposed algorithm for a diagnostic protocol is described.46 The clinical history must put an emphasis on health care during the prenatal, perinatal and postnatal period and include the results of all previous studies, including a genealogical tree for at least three generations and an intentional search for family antecedents of mental delay, psychiatric illnesses and congenital abnormalities.
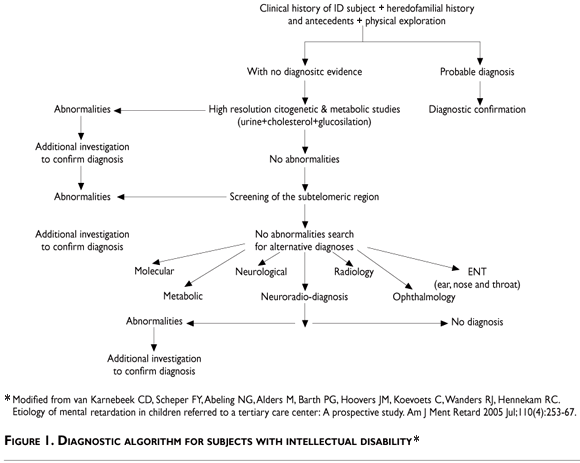
The physical exam should focus on secondary abnormalities and congenital malformations, somatometric measurements and neurological and behavioral phenotype evaluations. If, as a result, signs suggesting a particular etiological diagnosis are recognized, specific analyses are requested; in the case of Rett syndrome, an MeCP2 gene mutation analysis is recommended.
Search for genetic abnormalities
If it is not feasible to establish a clinical diagnosis, it is necessary to conduct high-resolution cytogenetic studies47 in addition to metabolic clinical evaluations.48
For patients with normal results from the previously mentioned analyses, it is possible to request fluorescence in situ hybridization (FISH)49 which is an evaluation of the entire subtelomeric region. In the next step, if no abnormal data are identified, submicroscopic chromosomal disorders are evaluated.
Neuroimages can be useful only if the occipitofrontal circumference of the head is abnormal –below the second or above the 98th percentile– or if the neurological exams reveal abnormalities. In addition, they are recommended if a specific neuroanatomical effect exists (tuberous sclerosis) or a clinical history indicates perinatal hypoxy.
Metabolic analyses can include urinary tests for amino acids, organic acids, oligosaccharides, mucopolysaccarides and uric acid. Plasma levels 7- and 8- dehydrocholesterol for total cholesterol and dienesterol are useful for identifying defects in the distal cholesterol pathways. Other diagnostic tests can be conducted for finding congenital disorders of glycosylation.50
Differential diagnosis
Since mental delay is a developmental disorder that is secondary to many etiological factors, there are few nosological units with which they can be confused; among these are generalized developmental disorders51 (DSM IV 299.00 to 299.80) and, in particular, autism with low-functionality and autistic spectrum disorders.52 Nevertheless, it is important to establish a differential diagnosis since, while some therapeutic interventions are similar with respect to social and work inclusion programs, future expectations are very different.
The clinical profile
Based on the gradual division described above, it is possible to infer that a specific clinical profile does not exist; each one of the levels for each group has its own clinical characteristics.
Symptoms are closely related to the specific sensorimotor, linguistic and cognitive processes, among others. The more moderate the disability, the less evident its symptoms; perhaps alterations in language construction shed more light and, in particular, the comprehension level and behavior of the children themselves compared with that of a chronologically younger age. It is useful to ask the parents if they can establish a comparative age in relation to brothers and sisters or close cousins in the family (if they exist) who could serve as a reference. Parents often say that the patient "speaks and understands everything"; in this case it is important to clarify if they are referring to the use of nouns and verbs or the comprehension of orders and concepts.
It is essential to give credibility to the parents when they insist that a doctor recognize a developmental disorder. It is true that in some cases they tend to be delay or apprehensive or overprotective, but it is more often the case that their perceptions are based on objective, comparative judgments and are therefore correct. Frequently, by the time they get to a doctor who establishes the diagnosis, they painfully express the great frustration that they experienced when they had to repeatedly tell their doctor that "something was wrong," especially if that doctor insisted on not making comparisons and affirming that "no two human beings are alike," that "developing the skills is just a question of time"; such an attitude causes late intervention, among other things. When a diagnosis of slow-learner is established, this creates confusion since it suggests normality rather than disability.
Comorbidities
Individuals who suffer mental delay are more vulnerable for developing a psychiatric abnormality. Statistics exist today that confirm that this population experiences two or three times more mood disorders, anxiety disorders and behavioral problems than persons without intellectual disability.53 Such vulnerability, on occasion, leads to a set of psychotic symptoms that are secondary to the stress experienced when social, family and school demands are excessive.54 On the other hand, other illnesses comorbidly exist that are unrelated to this vulnerability factor; the most common being epilepsy,55 attention deficit disorder and hyperactivity,56 schizophrenia57 and infantile cerebral paralysis.
Treatment
Cognitive disability must, evidently, be understood and diagnosed as a developmental disorder, but fundamental for providing adequate professional care; than to take into account the intellectual level of the patient and his or her ability to adapt to the existing environment and, of utmost importance, the reaction of the parents to this situation.
Since cognitive disability is not curable, the treatment objectives must focus on the normalization of behavior in accordance with the norms and rules determined by society. To this end, intervention as early as possible is fundamental since treatment for developmental disorders can reach its maximum scope only through early intervention. It must be remembered that the process of cerebral plasticity has its greatest potential during to the first five years of life and this is one of the most important supporting factors in attaining the therapeutic goals. Furthermore, since the behavior disorders which are so frequently observed are secondary –due to deficient childrearing in the majority of cases– the parents must be worked with and advised as to adequate childrearing methods for developing adaptation patterns that lead to optimal social integration.
People with mental delay, being limited to a mental age of less than 13 years, cannot aspire to levels of abstract cognitive thought that in normal conditions appear at the beginning of adolescence; for this reason, educational objectives must be focused on the development of skills for achieving a self-sufficient life at an adult age and not on schooling as it happens in many countries. In addition, interaction between peers should be promoted for creating group belonging (relationships with others with approximately the same disability level).
It is evident that the results obtained depend on the age of the subject when the diagnosis is established and when treatment is initiated, the severity of the disability, the affected areas and the methods or techniques used for rehabilitating these areas. Accordingly, treatment is established in the following manner:
During the infancy period (zero to two years), disorders in muscular tone and motor development are treated (motor therapy) and signs of sensory disintegration that almost always accompany motor problems are treated through sensory integration therapy. As for the linguistic developmental disorders themselves, symbolization processes are treated (language therapy) as well as muscular tone alterations that affect respiration, phonation and the bucofacial region (articulation therapy). Likewise, cognitive stimulation should be used for these children at the onset of treatment.
When children are diagnosed after two years of age and before puberty, the ideal is to use instruments that determine the maturity level for each one of the developmental areas and apply the same therapies (motor, sensory, linguistic, etc.), in addition promoting the development of perceptual abilities, with deficits in, and learning abilities (reading, writing, mathematics, etc.), using techniques similar to those used in children with learning disorders (dyslexia, etc.).
It is common to observe behavioral problems in this population, which often motivate parents to seek out professional advice; therefore, behavioral therapy should be included in the health care plan and should be based on humanistic principles (clarification of feelings and positive reinforcement) and not on aversion techniques. Finally, it is essential to work with independent living skills and give the individual the necessary elements for self-sufficiency.
Although it is rare, an adolescent can be seen in the doctors office for poor academic performance or behavioral problems without having been previously diagnosed with ID. This most likely involves a subject with limitrophe and who, upon entering middle school, does not manage to pass the subjects that require abstract thinking (mathematics, physics, chemistry, etc.).
In these cases, as well as for adolescents and adults with intellectual disability, programs oriented toward independent living should be recommended. These programs should cover the areas necessary for achieving a partially or totally self-sufficient life, among which are: the academic-basic skills, community integration programs, developing skills for managing domestic tasks, personal healthcare and sexuality. In addition, a prevocational program should be included for the development of abilities for the workplace and, when possible, for the individual to become integrated into the labor market.
Pharmacological treatment is used for the treatment of comorbidities, and is specific for each one according to the criteria followed for these disorders, both in psychiatry and in neurology. On occasion, when a favorable response is not obtained, a random treatment scheme is established. In the case of attention deficit disorder and hyperactivity, the use of stimulants for the central nervous system (the treatment of choice for this disorder) had been considered not to produce favorable results; nevertheless, recent research shows that elevated doses of methylphenidate (0.60 mg/kg) produce obvious improvements in symptoms related to inattention, impulsivity and hyperactivity.
Because of the above, it is evident that treatment for persons with cognitive disability must be multidisciplinary and include medicine (family, pediatrics, neurology and psychiatry), psychology (educational and clinical), education (regular, and special), rehabilitation (physical, occupational and recreational), nursing, social work, etcetera.
Prognosis
As was already established, intellectual disability is not curable; and yet, the prognosis in general terms is good when using the emotional wellbeing of the individual as a parameter. When the parents of these subjects are asked, after they have accepted the diagnosis, they express than their long-term expectation, that "their children be happy" or that "they be self-sufficient"; that is, to see them content and self-sufficient compensates for the lost hope of having a professional child or one that satisfies the parents unfulfilled dreams. This is a striking contrast with parents who reject the disability and for whom the only acceptable parameter is "normality." Of course, in these cases, the patients not only suffer more but the parents also live in constant agony.
Other conditions exist that, when attained, guarantee the achievement of the objectives and, therefore, the prognosis in terms of obtaining that state of happiness is wholly viable. It is feasible to see an adult with mild or moderate cognitive disability or limitrophe maintain a job, travel to the city, take care of his or her apartment, have a social life or, in other words, manage on ones own. It is therefore necessary to fulfill the following requirements.
The first and most important is the parents acceptance of their childrens limitations and the impossibility of attaining "normality." After this, the age upon beginning the rehabilitation program should be considered as well as obtaining a level of continual productivity that is consistent with the disability, the existence of a group to which to belong and, lastly, the unconditional affection of the parents. It has been stated that the above mentioned factors reduce psychiatric comorbidities (depression, anxiety, behavior) and a prevalence equal to that of the non-disabled population is found; or as one patient said who was asked how it feels to attend an independent living center: "I know I cant go to the university like my brothers and sisters but I can do everything that they can do."
Conclusions
Intellectual disability should be treated in a comprehensive manner. Nevertheless, currently, the fundamental task and perhaps the only one that applies is the detection of the limitation and abilities as a function of subjects age and expectations for the future, with the only goal being to provide the support necessary for each one of the dimensions or areas in which the persons life is expressed and exposed. Nevertheless, this perspective tends to be reductionistic and subjects with disabilities who live in developing countries should have multiple social benefits that today are not present, and there are no signs of them on the near horizon.
Intellectual disability has been absent in the political, social and economic agenda of the countries in the region. In this sense, Mexico is no exception. Subjects with intellectual disability are not considered in the planning strategies for health services, the predominant educational proposals are not based on scientific evidence and virtually no research has been developed in this knowledge area. Substantive but elemental aspects for a dignified life for individuals with intellectual disabilities must be a priority in the legislative arena. Among these are the possibilities for guaranteeing human development, teaching and education, home life, community life, work, health and security, optimal behavioral development, social integration, as well as protection and defense. The organized social response for confronting the social needs of subjects with intellectual disabilities cannot be delayed indefinitely.
References
1. Petterson B, Bourke J, Leonard H, Jacoby P, Bower C. Co-occurrence of birth defects and intellectual disability. Paediatr Perinat Epidemiol 2007;21(1):65-75. [ Links ]
2. Available at: http://www.indesol.gob.mx [Consultado 25 noviembre 2006] [ Links ]
3. Battaglia A, Bianchini E, Carey JC. Diagnostic yield of the comprehensive assessment of developmental delay/mental retardation in an institute of child neuropsychiatry. Am J Med Genet 1999;82(1):60-66. [ Links ]
4. Bundey S, Webb TP, Thake A, Todd J. A community study of severe mental retardation in the West Midlands and the importance of the fragile X chromosome in its aetiology. J Med Genet 1985;22(4):258-266. [ Links ]
5. Skuse DH. Rethinking the nature of genetic vulnerability to autistic spectrum disorders. Trends Genet 2007;23(8):387-395. [ Links ]
6. Schrander-Stumpel CT, Sinnema M, van den Hout L, Maaskant MA, van Schrojenstein Lantman-de Valk HM, Wagemans A, Schrander JJ, Curfs LM. Healthcare transition in persons with intellectual disabilities: general issues, the Maastricht model, and Prader-Willi syndrome. Am J Med Genet C Semin Med Genet 2007;145(3):241-247. [ Links ]
7. Maatta T, Tervo-Maatta T, Taanila A, Kaski M, Iivanainen M. Mental health, behaviour and intellectual abilities of people with Down syndrome. Downs Syndr Res Pract 2006;11(1):37-43. [ Links ]
8. Reiss AL, Hall SS. Fragile X syndrome: assessment and treatment implications. Child Adolesc Psychiatr Clin N Am 2007;16(3):663-675. [ Links ]
9. Jauregi J, Arias C, Vegas O, Alen F, Martinez S, Copet P, Thuilleaux D. A neuropsychological assessment of frontal cognitive functions in Prader-Willi syndrome. J Intellect Disabil Res 2007;51(Pt 5):350-365. [ Links ]
10. Weaving LS, Ellaway CJ, Gecz J, Christodoulou J. Rett syndrome: clinical review and genetic update. J Med Genet 2005;42(1):1-7. [ Links ]
11. Mouridsen SE, Sorensen SA. Psychological aspects of von Recklinghausen neurofibromatosis (NF1). J Med Genet 1995;32(12):921-924. [ Links ]
12. Raznahan A, Higgins NP, Griffiths PD, Humphrey A, Yates JR, Bolton PF. Biological markers of intellectual disability in tuberous sclerosis. Psychol Med 2007;37(9):1293-304. [ Links ]
13. Nyhan WL, Wulfeck BB, Tallal P, Marsden DL. Metabolic correlates of learning disability. Birth Defects Orig Artic Ser 1989;25(6):153-169. [ Links ]
14. Feanny SJ, Chuang SH, Becker LE, Clarke JT. Intracerebral paraventricular hyperdensities: a new CT sign in Krabbe globoid cell leukodystrophy. J Inherit Metab Dis 1987;10(1):24-27. [ Links ]
15. Kalkanoglu HS, Ahring KK, Sertkaya D, Moller LB, Romstad A, Mikkelsen I, Guldberg P, Lou HC, Guttler F. Behavioural effects of phenylalanine-free amino acid tablet supplementation in intellectually disabled adults with untreated phenylketonuria. Acta Paediatr 2005;94(9):1218-1222. [ Links ]
16. Campos AP, Vaz C, Duque F, Leite M, Vilarinho L, Diogo L, Garcia P. Galactosemia: a neurometabolic disease. Rev Neurol 2007;44(11):702-703. [ Links ]
17. Van de Putte T, Francis A, Nelles L, van Grunsven LA, Huylebroeck D. Neural crest-specific removal of Zfhx1b in mouse leads to a wide range of neurocristopathies reminiscent of Mowat-Wilson syndrome. Hum Mol Genet 2007;16(12):1423-1436. [ Links ]
18. Vallance H, Morris TJ, Coulter-Mackie M, Lim-Steele J, Kaback M. Common HEXB polymorphisms reduce serum HexA and HexB enzymatic activities, potentially masking Tay-Sachs disease carrier identification. Mol Genet Metab 2006;87(2):122-127. [ Links ]
19. Buyukgebiz A. Congenital hypothyroidism clinical aspects and late consequences. Pediatr Endocrinol Rev 2003;1(suppl 2):185-190.
20. Téllez-Rojo MM, Bellinger DC, Arroyo-Quiroz C, Lamadrid-Figueroa H, Mercado-García A, Schnaas-Arrieta L, Wright RO, Hernández-Ávila M, Hu H. Longitudinal associations between blood lead concentrations lower than 10 microg/dl and neurobehavioral development in environmentally exposed children in Mexico City. Pediatrics 2006;118(2):e323-e230. [ Links ]
21. Kodituwakku PW. Defining the behavioral phenotype in children with fetal alcohol spectrum disorders: a review. Neurosci Biobehav Rev 2007;31(2):192-201. [ Links ]
22. Morrow CE, Culbertson JL, Accornero VH, Xue L, Anthony JC, Bandstra ES. Learning disabilities and intellectual functioning in school-aged children with prenatal cocaine exposure. Dev Neuropsychol 2006;30(3):905-931. [ Links ]
23. Desmond MM, Montgomery JR, Melnick JL, Cochran GG, Verniaud W. Congenital rubella encephalitis. Effects on growth and early development. Am J Dis Child 1969;118(1):30-31. [ Links ]
24. Odeberg J, Wolmer N, Falci S, Westgren M, Sundtrom E, Seiger A, Soderberg-Naucler C. Late human cytomegalovirus (HCMV) proteins inhibit differentiation of human neural precursor cells into astrocytes. J Neurosci Res 2007;85(3):583-593. [ Links ]
25. Gilad R, Lampl Y, Blumstein G, Dan M. Neurosyphilis: the reemergence of an historical disease. Isr Med Assoc J 2007;9(2):117-118. [ Links ]
26. Sharif M, Ziaei H, Daryani A, Ajami A. Seroepidemiological study of toxoplasmosis in intellectual disability children in rehabilitation centers of northern Iran. Res Dev Disabil 2007;28(3):219-224. [ Links ]
27. Seppanen M, Meri S, Notkola IL, Seppala IJ, Hiltunen-Back E, Sarvas H, Lappalainen M, Valimaa H, Palikhe A, Valtonen VV, Lokki ML. Subtly impaired humoral immunity predisposes to frequently recurring genital herpes simplex virus type 2 infection and herpetic neuralgia. J Infect Dis 2006;194(5):571-578. [ Links ]
28. Juul-Dam N, Townsend J, Courchesne E. Prenatal, perinatal, and neonatal factors in autism, pervasive developmental disorder-not otherwise specified, and the general population. Pediatrics 2001;107(4):E63. [ Links ]
29. Leonard H, de Klerk N, Bourke J, Bower C. Maternal health in pregnancy and intellectual disability in the offspring: a population-based study. Ann Epidemiol 2006;16(6):448-454. [ Links ]
30. Calis EA, Olieman JF, Rieken R, Penning C. Impact of malnutrition on gastrointestinal disorders and gross motor abilities in children with cerebral palsy. Brain Dev 2007;29(8):534. [ Links ]
31. Scheller JM, Nelson KB. Does cesarean delivery prevent cerebral palsy or other neurologic problems of childhood? Obstet Gynecol 1994;83(4):624-630. [ Links ]
32. Naeye RL. Placenta previa. Predisposing factors and effects on the fetus and surviving infants. Obstet Gynecol 1978;52(5):521-525. [ Links ]
33. Niswander KR, Gordon M, Drage JS. The effect of intrauterine hypoxia on the child surviving to 4 years. Am J Obstet Gynecol 1975;121(7): 892-899. [ Links ]
34. Ambalavanan N, Carlo WA, Shankaran S, Bann CM, Emrich SL, Higgins RD, Tyson JE, OShea TM, Laptook AR, Ehrenkranz RA, Donovan EF, Walsh MC, Goldberg RN, Das A; National Institute of Child Health and Human Development Neonatal Research Network. Predicting outcomes of neonates diagnosed with hypoxemic-ischemic encephalopathy. Pediatrics 2006;118(5):2084-2093. [ Links ]
35. Siitonen SL, Kauppinen T, Leino TK, Vanninen E, Kuronen P, Lansimies E. Cerebral blood flow during acceleration in flight measured with SPECT. Aviat Space Environ Med 2003;74(3):201-206. [ Links ]
36. Holota VIa, Sonnyk HT, Odarenko IM. Sequelae for the infants of vacuum extraction operations with the subsequent application of obstetrical forceps. Pediatr Akus Ginekol 1979;(3):57-59. [ Links ]
37. Bouda J, Bouda JJ. Neurological complications during gynecological pelvic surgery. Ceska Gynekol 2005;70(5):388-391. [ Links ]
38. Falcao AS, Silva RF, Fernandes A, Brito MA, Brites D. Influence of hypoxia and ischemia preconditioning on bilirubin damage to astrocytes. Brain Res 2007;1149:191-199. [ Links ]
39. Anderson V, Catroppa C, Morse S, Haritou F, Rosenfeld J. Functional plasticity or vulnerability after early brain injury? Pediatrics. 2005;116(6):1374-1382. [ Links ]
40. Noyola DE, Demmler GJ, Nelson CT, Griesser C, Williamson WD, Atkins JT, Rozelle J, Turcich M, Llorente AM, Sellers-Vinson S, Reynolds A, Bale JF Jr, Gerson P, Yow MD; Houston Congenital CMV Longitudinal Study Group. Early predictors of neurodevelopmental outcome in symptomatic congenital cytomegalovirus infection. J Pediatr 2001;138(3):325-331.
41. Leonard H, Petterson B, De Klerk N, Zubrick SR, Glasson E, Sanders R, Bower C. Association of sociodemographic characteristics of children with intellectual disability in Western Australia. Soc Sci Med 2005;60(7):1499-1513. [ Links ]
42. Emerson E, Hatton C. Contribution of socioeconomic position to health inequalities of British children and adolescents with intellectual disabilities. Am J Ment Retard 2007;112(2):140-150. [ Links ]
43. Matson JL, Dixon DR, Matson ML, Logan JR. Classifying mental retardation and specific strength and deficit areas in severe and profoundly mentally retarded persons with the MESSIER. Res Dev Disabil 2005;26(1):41-45. [ Links ]
44. Widmer ED, Kempf-Constantin N, Robert-Tissot C, Lanzi F, Carminati GG. How central and connected am I in my family? Family-based social capital of individuals with intellectual disability. Res Dev Disabil 2007. [ Links ]
45. Maulik PK, Darmstadt GL. Childhood disability in low- and middle-income countries: overview of screening, prevention, services, legislation, and epidemiology. Pediatrics 2007;120(Suppl 1):S1-S55.
46. van Karnebeek CD, Scheper FY, Abeling NG, Alders M, Barth PG, Hoovers JM, Koevoets C, Wanders RJ, Hennekam RC. Etiology of mental retardation in children referred to a tertiary care center: a prospective study. Am J Ment Retard 2005;110(4):253-267. [ Links ]
47. Borg K, Bocian E, Stankiewicz P, Obersztyn E, Kruczek A, Nowakowska B, Ilnicka A, Mazurczak T. Cytogenetic-molecular analysis of balanced chromosomal rearrangements in nine patients with intellectual disability, dysmorphic features and congenital abnormalities. Med Wieku Rozwoj 2006;10(1 Pt 2):227-246. [ Links ]
48. Poplawski NK, Harrison JR, Norton W, Wiltshire E, Fletcher JM. Urine amino and organic acids analysis in developmental delay or intellectual disability. J Paediatr Child Health 2002;38(5):475-480. [ Links ]
49. Rajcan-Separovic E, Harvard C, Liu X, McGillivray B, Hall JG, Qiao Y, Hurlburt J, Hildebrand J, Mickelson EC, Holden JJ, Lewis ME. Clinical and molecular cytogenetic characterisation of a newly recognised microdeletion syndrome involving 2p15-16.1. J Med Genet 2007;44(4):269-276. [ Links ]
50. Barone R, Sturiale L, Fiumara A, Uziel G, Garozzo D, Jaeken J. Borderline mental development in a congenital disorder of glycosylation (CDG) type Ia patient with multisystemic involvement (intermediate phenotype). J Inherit Metab Dis 2007;30(1):107. [ Links ]
51. Strydom A, Livingston G, King M, Hassiotis A. Prevalence of dementia in intellectual disability using different diagnostic criteria. Br J Psychiatry 2007;191:150-157. [ Links ]
52. Matson JL, Wilkins J, Smith K, Ancona M. PDD-NOS Symptoms in Adults with Intellectual Disability: toward an Empirically Oriented Diagnostic Model. J Autism Dev Disord 2007. [ Links ]
53. Ring H, Zia A, Lindeman S, Himlok K. Interactions between seizure frequency, psychopathology, and severity of intellectual disability in a population with epilepsy and a learning disability. Epilepsy Behav 2007;11(1):92-97. [ Links ]
54. Regnard C, Reynolds J, Watson B, Matthews D, Gibson L, Clarke C. Understanding distress in people with severe communication difficulties: developing and assessing the Disability Distress Assessment Tool (DisDAT). J Intellect Disabil Res 2007;51(Pt 4):277-292. [ Links ]
55. Ring H, Zia A, Lindeman S, Himlok K. Interactions between seizure frequency, psychopathology, and severity of intellectual disability in a population with epilepsy and a learning disability. Epilepsy Behav 2007;11(1):92-97. [ Links ]
56. Voigt RG, Barbaresi WJ, Colligan RC, Weaver AL, Katusic SK. Developmental dissociation, deviance, and delay: Occurrence of attention-deficit-hyperactivity disorder in individuals with and without borderline-to-mild intellectual disability. Dev Med Child Neurol 2006;48(10):831-835. [ Links ]
57. Gottesmann C, Gottesman I. The neurobiological characteristics of rapid eye movement (REM) sleep are candidate endophenotypes of depression, schizophrenia, mental retardation and dementia. Prog Neurobiol 2007;81(4):237-250. [ Links ]
58. Ibrahim AI, Hawamdeh ZM. Evaluation of physical growth in cerebral palsied children and its possible relationship with gross motor development. Int J Rehabil Res 2007;30(1):47-54. [ Links ]
Accepted on: December 5, 2007
Address reprint requests to: Dr. Eduardo Lazcano. Instituto Nacional de Salud Pública. Av. Universidad 655.Santa María Ahuacatitlán, Cuernavaca, Morelos/Gregorio Katz. Hidalgo 7, col. Granjas de Guadalupe, Cuautitlán Izcalli, Estado de Méxco, 54700 México.E-mail: elazcano@insp.mx, gkatzmina@prodigy.net.mx














