Servicios Personalizados
Revista
Articulo
Indicadores
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Salud Pública de México
versión impresa ISSN 0036-3634
Salud pública Méx vol.47 no.4 Cuernavaca jul. 2005
ARTÍCULO BREVE
Informing the TB suspect for sputum sample collection and communicating laboratory results in Nicaragua: a neglected process in tuberculosis case finding
La información al caso sospechoso de TB para la recolección de la muestra de esputo y la comunicación de resultados de laboratorio en Nicaragua: un proceso descuidado en la pesquisa de casos de tuberculosis
Jean Macq, MD, DTM, MPHI; Alejandro Solis, MD, MPHII; Harry Velázquez, MD, MPHII,III; Bruno Dujardin MD, PhD.I
IEcole de Santé Publique, Université Libre de Bruxelles, Belgium
IICentro de Investigaciones y Estudios de la Salud, Universidad Nacional Autónoma de Nicaragua
IIIMinisterio de Salud de Nicaragua-SILAIS
ABSTRACT
OBJECTIVE: To assess the patient information process before sputum sample collection, the quality of sputum sample and transmission of acid-fast bacilli (AFB) examination results to TB suspects, in three local areas of Nicaragua.
METHODS: (a) directed interviews of consecutive series of TB suspects whose sputum had been examined for AFB; (b) directed interview of health personnel; and (c) assessment of the sputum sample quality.
RESULTS: A total of 115 TB suspects and 33 health personnel were interviewed and 625 sputum samples were assessed. Results show multiple weaknesses in the process of information to the patient during sputum collections, as well as in the communication of results.
CONCLUSIONS: This study unveiled an aspect usually overlooked of case finding, that is, the information process during sputum production, sputum sample quality, and the communication of results to the TB suspects. The results illustrate the need for routine assessment of the whole diagnostic process.
Keywords: tuberculosis; diagnostic; patient-provider communication; Nicaragua
RESUMEN
OBJETIVO: valorar el proceso de información del paciente antes de la producción de esputo, la calidad de la muestra de esputo, y la transmisión de los resultados del examen microscópico del esputo a los sospechosos de tuberculosis (TB) en tres áreas de Nicaragua.
MATERIAL Y MÉTODOS: (a) entrevistas dirigidas a sospechosos de TB cuya expectoración ha sido examinada para BK; (b) entrevistas dirigidas al personal de salud de tres áreas de estudio (c) la evaluación de la calidad de la expectoración.
RESULTADOS: Un total de 115 sospechosos de TB y 33 trabajadores de la salud fueron entrevistados; 625 muestras de esputo fueron examinadas. Los resultados muestran varias debilidades en el proceso de información a los sospechosos antes de la producción de esputo.
CONCLUSIÓN: Este estudio revela un aspecto del proceso de diagnóstico de la TB demasiado ignorado. Los resultados ilustran la importancia de evaluar de forma rutinaria el proceso completo de diagnóstico de la TB. Informing the TB suspect for sputum sample collection and communicating laboratory results in Nicaragua: a neglected process in tuberculosis case finding
Palabras claves: tuberculosis; diagnóstico; comunicación prestador-paciente; Nicaragua
Tuberculosis control is a world-wide priority for it kills an estimated 2 million people yearly.1 Reducing the disease's transmission requires reducing the delays in identifying infectious cases and achieving a high cure rate of diagnosed AFB-positive pulmonary tuberculosis. We have assessed in Nicaragua critical steps usually ignored in the process of AFB-positive pulmonary TB cases finding: the information that must be given to TB suspects in order to assist them to produce sputum samples, the quality of the sample produced and the communication of microscopy results back to the patients. That country has a generally well organised TB control programme (TCP). In 2000, the national notification rate was 47/100 000 population for all forms of TB and 29/100 000 population for AFB-positive pulmonary TB. Eighty one percent of the 2000 cohort was declared cured at the end of the treatment and 8% dropped out of treatment.2
In Nicaragua, in compliance with international standards, pulmonary tuberculosis is diagnosed primarily through microscopic examination of the sputum of suspected cases to detect the presence of AFB. The criterion for being catalogued as a suspected case is having a cough of more than 21 days.3,4 In 2000, Nicaragua had an average of one laboratory able to perform AFB sputum smears examination for 30 924 inhabitants.5 The national reference laboratory (CNDR) is responsible for supervision and quality control. In 2000, its staff made 15 supervisory visits focusing on slide preparation techniques (spreading and staining the samples) and checking the microscopes.5
The results of the routine quality control done by the CNDR show since 1998, a stable and very good level of concordance with the peripheral laboratories' results above 99% for AFB-negative and AFB-positive slides.
Material and Methods
This study was conducted in three municipalities or "municipios" (Jinotega, Pantasma and Bocay) in the northern department of Jinotega, Nicaragua, in 2000. These municipalities have a total population of 165 449, 30% of whom live in urban areas. They are covered by 30 health units, i.e., health posts, health centres and hospitals. For the department of Jinotega, the notification rate was of 35/100 000 inhabitants for AFB-positive pulmonary TB in 2000.
We used a "step-by-step" model to assess the process, starting with the explanation given to the patient on how to produce the sputum and finishing when the patient received his AFB examination results.6 This assessment focused on communication and consequent loss of time for suspected cases of TB. The criteria and standard definitions in each of the steps studied were mainly those of the TCP standards.3,4
To perform our assessment, we gathered information from different sources. In March and April 2000 we invited consecutive series of patients who had been suspected of tuberculosis for interviews in May 2000. At the same time, we interviewed health care workers (HCW) who had been involved in the care dispensed to the suspected cases. MPH students as part of their master's research did both the HCW and suspected case interviews.
To assess the quality of sputum specimen production by patients suspected of tuberculosis, laboratory technicians from Jinotega reviewed the sputum samples. We also used information from the patient interviews. The steps assessed, criteria, standards and sources of data are summarised in Table I.

The MPH group of lecturers of Centro de Investigaciones y Estudios de la Salud, in Nicaragua reviewed the study protocol including at ethical aspects and Nicaragua Ministry of Health authorities granted approval for this study.
In line with ethical guidelines, verbal informed consent was sought to all suspected cases of tuberculosis. Confidentiality was stressed throughout the research process.
Results
Of the consecutive 209 patients in Bocay, Pantasma and Jinotega who came with a cough of more than 21 days in March and April 2000, 103 suspected cases responded to the invitation and were interviewed in a health post, health centre or hospital. Twelve TB suspects, accounting for 10% of the non-respondents, were visited at home to decrease selection bias. The patterns of their answers were similar to those of the 103 suspected cases. Eighty percent of the respondents were between 15 and 49 years old and 11/115 (10%) were AFB-positive. Fifty percent of the suspects were illiterate.
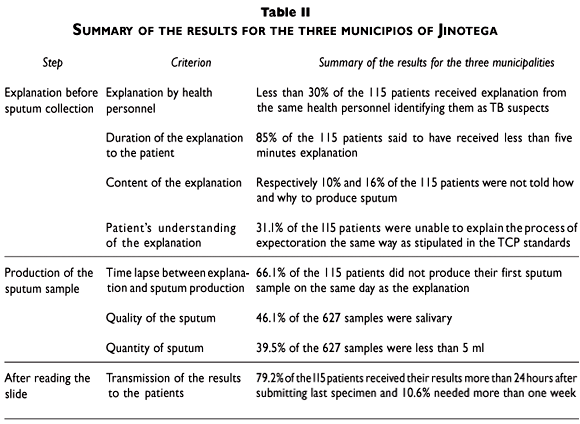
For the first step in our model, a minority of the patients was given, by the same health care provider who identified them as suspects, explanations on "how" (29%) to produce sputum and "why" (28%) the sputum sample was needed. Others were given explanations by the TCP nurse or laboratory technician. However, 10 and 16% of the patients, respectively, were not told how and why to produce sputum. For those who were given explanations on how to produce sputum, 98/104 (94%) said that the explanations took less than 5 minutes. Forty-one patients (31.1%) were not able to explain correctly the various steps to produce sputum for examination and 76/115 (66.1%) did not produce their first sputum samples on the same day that they received the explanation on how to do it. At the time of the interview, 29/115 (25.2%) had had more than three sputum examinations. Finally, 91/115 (79.2%) received their results more than 24 hours after submitting the last specimen, but 12/115 (10.6%) needed more than one week to receive their results. Concerning the quality and quantity of sputum, the laboratory technician reported that 46.1% (289/627) of the samples were salivary and 39.5% (248/627) were less than 5 ml. The overall results are summarised in Table II.
Discussion
Our results' validity may be criticised for two main reasons that we think are not sufficient to reject them. First, there might be a selection bias in our sample, for the response rate in our sample is low and the number of non-respondents who were visited at home was not great. The non-respondents probably had more accessibility problems than the respondents, a situation that in itself is unlikely to have influenced the explanation process and specimen production. It might have had a consequence on the transmission of results to the patients (i.e., there might be a higher proportion of non-respondents coming later to receive their results). Second, sputum quality and quantity are presented together, even though these characteristics will be significantly affected by the disease's severity and whether specimens have been collected on the spot or in the morning at home, in addition to the knowledge how to produce sputum. However, a result of more than 40% of salivary sputum is a problem from both the patients' and the health services' perspectives, regardless of the patients' characteristics.
Having said that, our findings raise important questions. In the Nicaraguan context, where there is a seemingly excellent concordance levels for reading the sputum smears for AFB, our study revealed multiple weaknesses in the process of sputum production. First, our results showed that more than two-thirds of the patients were given explanations on how and why to produce sputum by another health personnel than the one identifying them. This may be acceptable if the medical doctor who usually identifies the suspected case personally takes the patient directly to the nurse or laboratory technician who gives the explanation. However in practice, it meant that the TB suspect often had to join additional queues and had longer waits in the health facility because of poor coordination between the doctor from the curative consultation and the TCP nurse or laboratory technician. Second, two-thirds of the TB suspects from our sample lost at least one day and possibly transport costs to come back another day to produce their first sputum sample. This was often related to health unit organisation problems. For example, when a suspected case came from far away and reached the health unit late in the day, s/he would find the laboratory closed because the laboratory technician stopped working at the end of official working hours. Third, one-fourth of the patients lost time and possibly travel expenses because they were sent for sputum examinations more than three times because of the poor quality of their sputum. Indeed, producing sputum is not an easy process for people suspected of having TB. Indeed, it may be considered impolite behaviour, particularly for women. This has been documented in Asia.7 This difficulty is probably exacerbated by the health personnel's behaviour, as the HCWs often show disgust and fear to the patients who need to produce it. This issue is strongly related to the whole theme of tuberculosis-related social stigma and needs particular attention from TB programme supervisors. Finally, patients lost time because only one-fifth of them received their laboratory results less than one day after producing their last sputum and one tenth had to wait more than a week. In addition to these multiple potential causes of wasted time and money for the patient, the number of false negatives might be under-estimated by the routine procedure of supervision and quality control, as reflected by the high proportions of salivary sputum samples and specimens that were too small.
Conclusion
This study shed light on a usually overlooked aspect of case finding, that is, the information process to the TB suspect that starts with the explanation given to the patient on how to produce the sputum and finishes when the patient receives her/his AFB examination results. Our study revealed various causes of wasted time and money and loss of AFB-positive patients. It is unlikely that they are peculiar to Nicaragua. This is important enough to be considered much more carefully in supervising and monitoring TB control programmes.
Acknowledgements
We thank specially Lic. Neria Lopez and Dr. Moise Huete for having collected the data and participating in their analysis and Dr. Fabiola Prades, the former national TB program coordinator for having facilitated this study.
This study was financed by the European Union (project IC-18 CT 98-0350 of DGXII) and the "Commission Universitaire pour le Développement" (CUD) of the CIUF.
References
1. Dye C, Scheele S, Dolin P, Pathania V, Raviglione M. Consensus statement. Global burden of tuberculosis: estimated incidence, prevalence and mortality by country. WHO global surveilance and Monitoring Project. JAMA 1999;(282):677-86. [ Links ]
2. Tardencilla A. Informe anual del programa de control de la tuberculosis. Managua - Nicaragua; 2002. [ Links ]
3. Cruz JR. Manual del programa de control de tuberculosis. Ministerio de Salud de Nicaragua. Managua, Nicaragua: El Amanecer; 1993. [ Links ]
4. Cruz JR. Manual del programa de control de tuberculosis. Ministerio de Salud de Nicaragua. Managua: Imprimatur; 2001. [ Links ]
5. Prado Malespin MF. Informe anual del programa de control de tuberculosis - edición 2000. Managua, Nicaragua; 2001. [ Links ]
6. Dujardin B, Kegels G, Buve A, Mercenier P. Editorial: Tuberculosis control: Did the programme fail or did we fail the programme? Trop Med Int Health 1997;2(8):715-8. [ Links ]
7. Begum V, de Colombani P, Das Gupta S, Salim MAH, Hussain H, Pietroni M, et al. Tuberculosis and patient gender in Bangladesh: sex differences in diagnosis and treatment outcome. Int J Tuberc Lung Dis 2001;5(7):604-10. [ Links ]
Received on: December 7, 2004
Accepted on: July 25, 2005
Address reprint requests to: Jean Macq; Ecole de Santé Publique, Département Politiques et Systèmes de Santé; Université Libre de Bruxelles; Campus Erasme, CP 597; Route de Lennik, 808; B-1070 Brussels; Belgium. Email: jmacq@ulb.ac.be














