Servicios Personalizados
Revista
Articulo
Indicadores
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Salud Pública de México
versión impresa ISSN 0036-3634
Salud pública Méx vol.44 no.4 Cuernavaca jul. 2002
Design and methods of the evaluation of an HPV-based cervical cancer screening strategy in Mexico: The Morelos HPV Study
Yvonne Flores, MPH,(1,2) Keerti Shah, MD, Dr PH,(2) Eduardo Lazcano, MD, DrSc,(3) Mauricio Hernández, MD, DrSc,(3) David Bishai, MD, Ph D,(2) Daron G Ferris, MD,(4) Attila Lörincz, Ph D,(5) Pilar Hernández, BA,(3) Jorge Salmerón, MD, DrSc,(1) The Morelos HPV Study Collaborators*,(1,3,6,7)
Flores Y, Shah K, Lazcano E, Hernández M, Bishai D, Ferris DG, Lörincz A, Hernández P, Salmerón J, The Morelos HPV Study Collaborators.
Design and methods of the evaluation of an HPV-based cervical cancer screening strategy in Mexico: The Morelos HPV Study.
Salud Publica Mex 2002;44:335-344.
The English version of this paper is available too at: http://www.insp.mx/salud/index.html
Abstract
Objective. The purpose of this paper is to describe the design and methodology of the Morelos HPV Study. The main objective of this study is to examine the use of two different methods for obtaining HPV DNA specimens, self-collected vaginal and clinician-collected cervical, to detect pre-invasive cervical lesions and cancer. Material and Methods. This study was conducted within the regular population-based framework of the Mexican Institute of Social Security (IMSS) cervical cancer screening program in Morelos. A total of 7,868 women were recruited between May and October 1999 and are representative of the population of women attending cervical cancer screening services at the 23 IMSS clinics in the state of Morelos in 1999. Women were provided with a detailed description of the study before signing an informed consent form. Basic data were obtained from all participants using a standard IMSS registration form. During the initial recruitment visit, a randomly selected subsample of 1 069 participants were interviewed to collect additional information about cervical cancer risk factors, acceptability of the HPV and Pap tests, as well as patient costs. Before the pelvic exam, participants were asked to provide a self-collected vaginal specimen for HPV testing. All participants underwent a pelvic examination that involved collecting a cervical sample for the Pap smear and a clinician-collected HPV specimen. Data were evaluated from 7 732 women with complete information for the three tests. The 1 147 women who received at least one positive result (Pap, self- and/or clinician-HPV tests) were invited to return for a colposcopic examination. During colposcopy, biopsies were taken as appropriate, to histologically confirm a diagnosis of cervical intraepithelial neoplasia (CIN) 2/3 or invasive cancer. A total of 1,015 women attended colposcopy, and 101 women received a histologically-confirmed CIN 2/3 or cervical cancer diagnosis. Conclusions. The initial enrollment activities of the Morelos HPV study are the basis for a prevalent case-control study and a prospective cohort study that will investigate the natural history of HPV infections and determine if an HPV-based screening strategy is a safe and cost-effective alternative to Pap screening. The English version of this paper is available too at: http://www.insp.mx/salud/index.html
Key words: HPV; cervical cancer; screening; Papanicolaou; México
Flores Y, Shah K, Lazcano E, Hernández M, Bishai D, Ferris DG, Lörincz A, Hernández P, Salmerón J, The Morelos HPV Study Collaborators.
Diseño y métodos de la evaluación del uso de la prueba de virus de papiloma humano para tamizaje de cáncer cervical en México: el estudio de VPH en Morelos.
Salud Publica Mex 2002;44:335-344.
El texto completo en inglés de este artículo también está disponible en: http://www.insp.mx/salud/index.html
Resumen
Objetivo. Describir los métodos y el diseño del Estudio de VPH en Morelos. El objetivo principal de este estudio es examinar el uso de dos diferentes técnicas para obtener muestras de ADN de VPH, autotoma vaginal y toma clínica cervical, para detectar lesiones cervicales preinvasoras y cáncer. Material y métodos. Este estudio se realizó en el marco del Programa de Detección Oportuna de Cáncer Cervical (DOC) del Instituto Mexicano del Seguro Social (IMSS) en Morelos. Un total de 7 868 mujeres aceptaron participar en el estudio durante los meses de mayo a octubre de 1999. Esta muestra es representativa de la población de mujeres que acudieron a los programas de DOC en las 23 clínicas del IMSS en Morelos durante ese año. Se les proporcionó una explicación detallada del estudio a las participantes antes de que firmaran una carta de consentimiento informado. Se obtuvo información básica de todas las participantes y se usó el formato oficial de registro de datos del programa institucional de DOC del IMSS. Además se seleccionó una submuestra aleatoria de 1 069 participantes que fueron entrevistadas durante su visita inicial para obtener información adicional sobre los factores de riesgo de cáncer cervical, aceptabilidad de las pruebas de Papanicolaou (Pap) y VPH-autotoma, y los costos de las pacientes. Todas las participantes se tomaron una muestra de exudado vaginal para la prueba de VPH-autotoma. Posteriormente, se les realizó una exploración pélvica para obtener muestras cervicales para las pruebas de VPH-clínica y Pap. Se evaluó la información de 7 732 mujeres con resultados completos de las tres pruebas. A las 1 147 mujeres que recibieron un diagnóstico positivo de Pap, VPH-autotoma o VPH-cervical se les invitó a acudir a colposcopía para tomar una biopsia de las lesiones cervicales y confirmar el diagnóstico de neoplasia intraepitelial cervical (NIC) 2/3 o cáncer invasor. Un total de 1 015 mujeres acudieron a colposcopía, y 101 mujeres recibieron un diagnóstico histopatológico de NIC 2/3 o cáncer cervical. Conclusiones. Las actividades iniciales de reclutamiento del estudio de VPH en Morelos son la base para un estudio de casos y controles y un estudio de cohorte, que investigarán la historia natural de la infección con VPH y determinarán si el tamizaje por VPH es alternativa segura y costo-efectiva en relación con el tamizaje por Papanicolaou. El texto completo en inglés de este artículo también está disponible en: http://www.insp.mx/salud/index.html
Palabras clave: VPH; cáncer cervical; tamizaje; Papanicolaou; México
Cervical cancer (CC) is a major public health problem around the world. In many developing countries it is the most frequent female cancer, as well as the main cause of cancer-related death among women. There is a large discrepancy between the incidence and mortality of CC in developed and developing countries. Approximately 80% of the cases of CC occur in developing countries, mostly because industrialized countries have a greater availability of screening and treatment facilities.1
In Mexico, CC continues to be a serious public health problem. Over the past 25 years, CC mortality rates have remained stable, fluctuating little from 16.9 per 100 000 women in 1980, to 17.1 per 100 000 in 1997.2 Although there has been a national screening program in effect since 1974, CC remains one of the leading causes of death for women in Mexico. Each year, more than 4 000 Mexican women die from this disease.3,4 Epidemiological reports from the Mexican Institute of Social Security (IMSS) indicate that in 1995, CC was the leading cause of death due to cancer among women.5 In 1985, incidence of invasive CC was estimated to be 40 new cases per 100 000 women, and by 1997 this estimate had increased to 50 new cases per 100 000.3,4 The mortality and high incidence rate of late stage CC are indirect evidence of the low impact of the Mexican National Cervical Cancer Screening Program (CCSP); especially in light of the fact that 90% of CC cases can and should be detected using the Papanicolau (Pap) test.6
In Mexico, it has been difficult to establish and maintain an effective Pap test screening program, in comparison to those that are credited with reducing CC rates in the developed world.7 It is estimated that the current CCSP prevents less than 13 percent of the potentially preventable cases of CC in Mexico.8 Unfortunately, in Mexico the Pap test has a greater sensitivity to detect invasive cancer than pre-invasive disease. In Mexico, it has been reported that 60 percent of the cases detected using the Pap test are in fact cases of invasive CC.9
The decline in number of advanced cases and mortality rates for patients with CC that has occurred worldwide over the last 40 years, has mainly been attributed to screening programs.10 However, in the last two decades this decreasing trend is no longer occurring in some developed areas, which have reported a significant increase in incidence and mortality among women under the age of 50. This is probably related to an increase in the incidence of infection with human papillomavirus (HPV), in more recent decades.11 It is also important to note that in some developed countries with well screened populations, CC mortality rates have stabilized and further reductions in mortality are not expected. In a recent audit of the UK national CCSP, 50 percent of invasive cancers were detected in women who had been adequately screened.12 Until now, the Pap test has been the most widely used technology to detect CC. However, the high false negative rates of the test, especially in developing countries, typically result in a misdiagnosis or delayed diagnosis, and in additional costs.
Recent attention has started to focus on developing more sensitive and effective procedures to detect CC, such as the use of HPV testing as a screening alternative. Genital HPV infection is the most common sexually transmitted viral infection.13The recognition of HPV infection as a necessary cause of cervical dysplasia and CC has produced an interest in the use of HPV diagnostic tests for CC screening activities. Although HPV testing is not currently used in most CCSPs, some research indicates that it might be widely used in the near future.14
Our group is currently undertaking a major effort in Mexico, to examine the usefulness of HPV testing for CC screening. The main objective of the Morelos HPV Study is to evaluate the effectiveness of two different methods for obtaining HPV DNA specimens (self-collected vaginal and clinician-collected cervical), to detect pre-invasive cervical lesions and CC, as compared to the Pap test. A secondary objective is to investigate the role of HPV infection and variables of HPV infections, such as viral load and presence of specific HPV types, for the risk of CC and its precursors.
This article describes the enrollment activities, design and methodology, Pap and HPV testing procedures, colposcopy and histopathology evaluations, diagnostic criteria, and the quality control processes of the Morelos HPV Study.
Material and Methods
Study Site
Morelos state is located in central Mexico, bordering with Mexico, D.F., Puebla, Guerrero, and the State of Mexico. The population of the state was estimated to be 1 555 296 in 2000 (1.6% of the country's population).15 The area of the state is only 0.20% of the area of Mexico (3 927 km2),16 and it has a population density of 396 inhabitants per km2. The main economic activities in Morelos include agriculture, industry and tourism. Approximately 25% of the state population consists of women of reproductive age.17 In 1999, the general mortality rate throughout the state was 4.2 deaths per 1 000, the infant mortality rate was 12.8 per 1 000 children born alive, in 1997 the maternal mortality rate was 1.8 per 1 000 births,18 and in 1998, life expectancy for women was 77.6 years.19 Morelos was chosen as the study site because it consistently reports high mortality due to CC. In 1997, the CC mortality rate was 23.4 per 100 000 women over the age of 20, the third highest in the country.20 The state of Morelos also has a well-established health infrastructure, with 106 physicians per 100 000 inhabitants, 53.5 hospital beds and 43.7 clinics per 100 000 persons.21
Reorganization and Improvement of the Morelos Cervical Cancer Screening Program
In Mexico, CC screening services are available to all women free of charge, under the national CCSP. Until recently, the coverage of the program in Morelos was low and ineffective. However, during the past three years the program has been improved, coverage has increased, and quality standards have been enforced. Beginning in 1997, a number of important activities were implemented to reorganize and improve the IMSS CCSP of Morelos.22 A program was set up to improve the quality of the Pap samples obtained, which included: a) standardizing the procedures followed at clinics that offer the Pap test; b) a guarantee that all necessary supplies would be made available; c) the use of new intake and medical history forms; d) a more efficient system for sending the Pap slides to the lab; and e) the implementation of effective quality control mechanisms. In 1996, approximately 28% of the Pap samples taken were of poor quality, and now fewer than 5% of them are of poor quality. The quality of the diagnosis was improved by creating a specialized laboratory facility that was specifically set up to meet the new diagnostic quality requirements. This lab is serviced by four highly qualified cytotechnicians who received specialized training, new microscopes, all the necessary resources, and new reporting forms. Ongoing supervision of the cytotechnologists helps ensure the quality of diagnosis, as well as the prompt reporting of results.
A program was also set up to improve the diagnosis, treatment, and follow-up of patients. Before the reorganization and improvement of the CCSP there was no colposcopy center at the IMSS facilities in Morelos. If a woman received an abnormal Pap test she was referred to a gynecologist who was expected to perform a pelvic exam and take a biopsy, without the use of a colposcope. As part of the reorganization and improvement of the institutional CCSP, a colposcopy center was set up at the main IMSS hospital in Cuernavaca. This center is now equipped with three qualified physicians who received specialized training, three new colposcopes, all the necessary resources, and new reporting forms.
A number of activities have also been implemented to increase demand for CC screening. Family physicians were informed about the importance of referring women to the Pap clinics. Special stickers were placed in selected medical charts, as a reminder for physicians to invite the women to come in for a Pap test. This strategy resulted in a 150% increase in the utilization of Pap screening services. Some women were also reminded by personal letter to come in for a Pap, and approximately 40% of these women came in for a test.23 In 1996, the coverage of the Morelos CCSP was 22%, but after the reorganization and improvement activities this coverage has increased to 72%. Well-defined guidelines for triage, diagnosis and management of cervical abnormalities and case surveillance have also been established.24 Finally, a computerized surveillance system has been created to monitor the IMSS CCSP in Morelos.
Organization of the Study
This study is an interinstitutional collaboration between the Mexican Institute for Social Security (IMSS), the National Institute of Public Health of Mexico (INSP), the Johns Hopkins Medical Institutions, and Digene Corporation. The institutional review boards of the participating institutions have approved this study. Assistance was also received from outside collaborators who provided technical support and expertise at various stages of the study.
Study Population
This study is being carried out within the regular population-based framework of the IMSS CCSP in Morelos. IMSS, a federal agency, is the main social security institution in Mexico providing health insurance coverage to approximately 50-60% of the population. People who are, or have been, employed in the formal sector (as well as their spouses and dependants) are eligible for IMSS services. In Morelos, an estimated 95 000 women, between the ages of 25 and 65, make up the target population of the IMSS CCSP. Currently, the coverage of the IMSS CCSP in Morelos is estimated at 72%, and is expected to increase to 80% by the end of 2002. The study participants were obtained as a sample of all consecutive women attending CC screening services at any one of the 23 health units that make up the IMSS CCSP in Morelos.
Study Design
Women attending any of the IMSS CC screening clinics in Morelos were invited to join the enrollment phase of the study between May and October 1999. A total of 7 872 women between the ages of 15 and 85, without a prior diagnosis of cervical intraepithelial neoplasia (CIN) 2/3 or CC, hysterectomy or other treatment, enrolled in the study. At the recruitment visit, all participants provided informed consent, after a written and oral explanation of the study was provided.
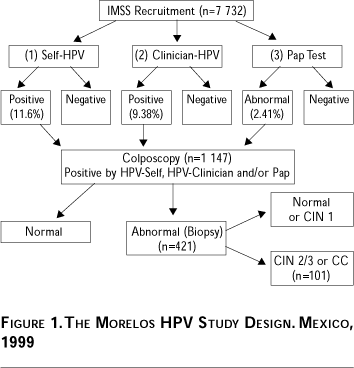
Participants were asked to provide a self-collected (SS) vaginal specimen for HPV testing. All participants also underwent a pelvic examination that involved collecting a cervical sample for the Pap smear, and a clinician-collected cervical HPV specimen (CS). Data were evaluated from 7 732 women with complete information for the three tests (median age=41). The 1 147 women who received at least one positive result (Pap, SS and/or CS) were invited to come back for a colposcopic evaluation. During colposcopy, biopsies were taken as appropriate, to histologically confirm a diagnosis of cervical intraepithelial neoplasia (CIN) 2/3 or invasive cancer. A total of 1 015 women returned for colposcopy, and 101 women have received a histologically confirmed CIN 2/3 (n=89) or CC (n=12) diagnosis (Figure 1). All women identified with CIN 2/3 or CC received appropriate treatment, following standard IMSS procedures.
Enrollment Procedures
All of the nurses involved with recruiting participants and collecting samples were trained at the 23 IMSS health centers that offer CC screening services. To encourage participation and to make the women feel as comfortable as possible, only female nurses and interviewers were employed. The training process involved explaining the study, describing the informed consent process, demonstrating how to take a proper sample (Pap and HPV), labeling and managing the samples, as well as reporting the results. A supervision process was established at the beginning of the study, to ensure the quality control of the HPV and Pap collection procedures. During the enrollment phase, brochures (available on request) that contained a brief explanation about HPV infection, its association with CC and the potential benefits of detection, were distributed to all women attending the CCSP.
During the enrollment period, all women attending CC screening services at any of the 23 IMSS clinics were informed about the study and invited to participate. These women were also read (or asked to read) a detailed description of the study. Before signing the informed consent form, the study participants received an explanation of the benefits and risks involved with participating in the study. They were also told that they might have to return to the clinic for follow-up activities. Women with a history of CIN 2/3 or CC, with a previous hysterectomy, or who were pregnant at the time, were not enrolled in the study. Overall, the response rate to participate in the study was greater than 95 percent. The study sample is representative of the women attending cervical cancer screening services at the 23 IMSS clinics in Morelos in 1999. The age distribution and the Pap test results of the study women were similar to those of all women attending the clinics in 1999 (See Tables I and II).
During the recruitment visit, all participants were interviewed by female staff using a standard IMSS registration form. In addition, during the initial recruitment visit a randomly selected subsample of 1 069 participants were interviewed to collect additional information about their demographic data (education level, income, number of dependants, etc.); obstetric, family planning and sexual history; risk factors for HPV and CC; knowledge and use of the CCSP; experience and acceptance of the Pap and HPV tests; patient costs of screening; and willingness to pay to reduce risk of CC. All interviews were reviewed and edited by the field supervisor; they were then coded and entered into a database (FoxPro) by a team of data entry clerks at the central offices in Cuernavaca. At the end of each day, a supervisor examined all entries for accuracy by comparing the database information to the questionnaires and forms, and by running visual checks for quality control purposes.
Self-collected HPV Test
Participants were asked to provide a self-collected vaginal specimen for HPV testing, before undergoing a pelvic exam. To help facilitate the understanding of how to obtain the vaginal self-collected specimen, a series of posters that explained the procedure were strategically placed in the participating clinics. Posters were hung in the waiting rooms, exam rooms, and bathrooms of the clinics so women could read them and prepare themselves to provide a sample. (Posters are available on request). The nurses also explained the self-collection procedures to all the participants. The women were instructed to remove their undergarments, squat, insert a 15 cm cotton-tipped, sterile Dacron swab into their vagina until their fingers reached their labia, and then rotate the swab once to the left and once to the right. After removing the swab from their vagina the women were asked to place the specimen in a transport medium test-tube (Digene Corporation, MD), and hand the specimen to the nurse. The samples were kept at room temperature and delivered to the INSP HPV laboratory facilities once a week, where they were stored at ¾20 °C until analyzed.
Pelvic Examination to Obtain Pap and Cervix-HPV Samples
Specialized female nurses with previous experience on the proper collection of Pap and cervical-HPV specimens performed the pelvic examinations. Following the standard IMSS protocol, the patients were asked to recline in the dorsal lithotomy position on an examination table. The nurses then followed international recommendations for cervical sampling procedures. A sterile, non-lubricated speculum was inserted, a sample of endocervix cells was obtained using a Dentilab Cytobrush, and ectocervix cells were collected using a spatula. After collecting the samples, the endocervical cells were spread on one half of a glass slide, the ectocervical cells were spread on the other half, and the slide was immediately fixed. Each labeled sample was then sent to the regional reading center for cytological interpretation.
Once the Pap smear sample was collected, the nurse then proceeded to obtain a sample of cervical cells (that would be analyzed to determine the presence of HPV DNA) by inserting a 15 cm cervical sampler brush (Digene Corporation, MD) into the vagina, making sure that between 1 and 1.5 cm of the brush was inside the os, and that the largest outer bristles of the brush touched the ectocervix. The brush was rotated in the endocervical canal three complete turns, in a counter-clockwise direction, and was then removed. The brush was then placed in a specimen transport medium test-tube (Digene Corporation, MD). The clinician-collected specimens were also kept at room temperature and delivered to the INSP HPV laboratory facilities once a week, where they were stored at ¾20 °C until analyzed.
Cytology Interpretation
For quality control purposes, the cytotechnicians were blinded when they re-read 2% of each other's slides, and if there was a discrepancy in the diagnoses the slide in question was then read by a pathologist (EC). Approximately 1% of the negative slides and all the positive slides were also re-read by a pathologist (EC), following international recommendations for diagnostic categories for cytological interpretation.6
Of the 7 868 Pap smears that were collected, 136 (1.8%) slides were considered of unsatisfactory quality for cytologic evaluation. Since these women did not return for a second Pap test they have been excluded from the analyses. Among these 136 inadequate Pap smears 11 were HPV positive (1 CS; 3 SS; 7 CS and SS) and 125 were HPV negative. A total of 7 732 participants had complete Pap, self- and clinician-collected HPV test results. Among the 7 732 Pap smears that were evaluated, 187 (2.42%) were abnormal. The abnormal results are the following: atypical squamous cells of undetermined significance (ASCUS) (n=55); CIN 1 (n=68); CIN 2/3 (n=42); atypical glandular cells of undetermined clinical significance (AGUS) (n=6); adenocarcinoma in situ (AIS) (n=4); adenocarcinoma (n=2); and squamous cell carcinoma (n=10). The abnormality rate and age distribution is similar to that observed in the reference population (Tables I and II).
HPV Testing
A total of 7 732 paired self-collected vaginal and clinician-collected cervical specimens were tested for HPV DNA at the INSP laboratory, using the Digene Hybrid Capture 2 Probe B, microtiter assay. A specialized HPV lab was set up and validated at INSP with the help of Digene technicians, and the samples were tested according to the manufacturer's instructions.25 First, the specimens were denatured and 75 µL of each sample was hybridized with 25 µL of probe B, which is a pool of full-length RNA probes for HPV types 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, and 68. During the hybridization reaction, the RNA probes bind to the HPV DNA that may be present in the specimens, forming RNA-DNA hybrids. The resulting hybrids are captured on the surface of microplate wells by an immobilized antibody that specifically recognizes RNA-DNA hybrids. The captured RNA-DNA hybrids are then reacted with a second antibody conjugated to alkaline phosphatase, and detected by adding a chemiluminescent dioxetane-based substrate. Light is emitted while the substrate is cleaved by the bound alkaline phosphate conjugate, and this long-lived glow reaction is measured in relative light units (RLUs) using a microplate luminometer. The intensity of the light that is emitted is proportional to the amount of target DNA in the specimen, and it is usually expressed as a ratio of the signal to the positive control (RLU/PC). A specimen is classified as positive if the RLU/PC ratio is ž1. The RLU/PC ratio also provides a semi-quantitative measure of viral burden, which can be used as an estimate of the intensity of infection. Approximately five percent of the HPV samples were found to have a "borderline" result with an RLU/PC ratio of between 0.8 and 2.0; these were re-tested for quality control purposes, and the second result was used as the final diagnosis.
Colposcopy Procedures
A total of 1 147 women who had at least one positive Pap, self- or clinician-collected test result were invited to come back for a colposcopy evaluation. Women with a Pap result of ASCUS or worse were referred to colposcopy. We implemented special follow-up strategies to improve patient compliance. In addition to the standard protocol that is used to report Pap test results and colposcopy attendance, each participant was to called remind them to come in for their colposcopy appointments. We also conducted special home visits for women without a phone to invite them to return for colposcopy at least once, and up to five times.
However, despite these additional efforts some women who were scheduled to come in for colposcopy did not return. We were able to evaluate a total of 1 015 women, resulting in a return compliance rate of 88.5%. There were 132 women who did not attend colposcopy services for the following reasons: (1) 17 women refused to come in because they had a positive HPV test but a normal Pap, so they decided not to continue with the study; (2) 22 women moved away; (3) 38 women gave an incorrect address at the enrollment visit; (4) two women became pregnant after enrolling in the study, and will return to colposcopy after giving birth; and (5) 39 women decided to use private or other colposcopy services instead of IMSS. There are 14 additional women who did not return for reasons unknown. Women with all negative results on their Pap, self- and clinician-collected HPV tests were not referred to colposcopy.
Certain measures were taken to ensure the quality control of the colposcopic diagnosis. The IMSS colposcopists received extensive specialized training in the U.S. and Mexico. A senior colposcopist (DF), visited the IMSS colposcopy center on two occasions at the beginning of the study to ensure all colposcopic procedures were performed correctly and the equipment was properly standardized. Many colposcopy procedures were videotaped so that an external expert could evaluate them. A total of 510 colposcopy video-films will be reviewed by an expert who will be blinded to the initial colposcopy diagnosis, Pap, and HPV test results. Also, colposcopic-images were taken for all the women using a digital imaging system for the quality control of colposcopy diagnosis and biopsy-sampling sites (DIMS, Denvu, AZ). A series of between 3-12 cervical images was obtained (as needed) for each woman. These images document the lesions that were observed and indicate the biopsy site with an arrow. For quality control purposes, the images obtained using the digital imaging system cannot be altered or updated. These colposcopic-images will also be evaluated as a balanced random sample of 300 images from clinically positive women (positive colposcopy= clinical evidence of lesions) and 300 women with negative colposcopy results.
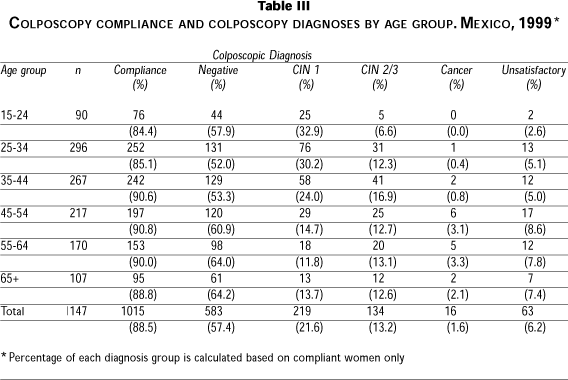
The colposcopists were aware of the cytology and HPV results of the women they were evaluating. The colposcopic diagnoses of the 1,015 compliant women were the following: normal (n=583); CIN 1 (n=219); CIN 2/3 (n=134); cancer (n=16); and unsatisfactory colposcopy (n=63) (See Table III) A biopsy was taken of all suspicious lesions. The women with unsatisfactory colposcopy had an endocervical curettage for histologic diagnosis. A second cervical sample was collected for HPV testing immediately prior to initiating the colposcopic exam, following the same procedures that were used during the enrollment visit. All cases received the appropriate treatment and are under surveillance according to the IMSS CCSP guidelines.
Final Histopathological Diagnosis
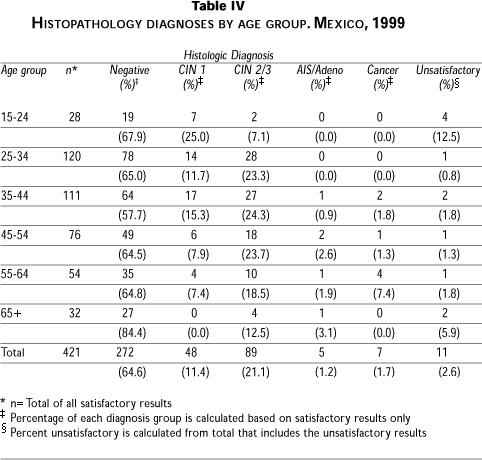
A total of 421 women underwent histological evaluation. The biopsy and ECC specimens were reviewed and diagnosed independently by two pathologists (EC and BR) without knowledge of the cytologic diagnoses, colposcopy data, or HPV testing results. In order to achieve improved consensus for the histologic diagnoses rendered on the cervical biopsy specimens in this study, the two pathologists reviewed routine cervical biopsy specimens from the IMSS Regional Hospital in Cuernavaca, Morelos. A multiheaded microscope was used to establish diagnostic categories and criteria for the evaluation of the biopsy specimens. A first evaluation was made by EC at the main IMSS hospital in Cuernavaca, and a second evaluation was performed by BR at the Johns Hopkins School of Medicine. All specimens for which the diagnosis of the first reviewer (EC) matched the diagnosis of the second reviewer (BR) were assigned that final histologic consensus diagnosis. The diagnostic concordance of the histopathology results between EC and BR was quite high, with a kappa value of 0.92. The 38 discordant cases were reviewed by a third pathologist (MS), and the final diagnosis was rendered by majority. The final histopathological diagnoses of these women were: normal (n=272); CIN 1 (n=48); CIN 2/3 (n=89); AIS and adenocarcinomas (n=5); cancer (n=7); and unsatisfactory for histological interpretation (n=11) (See Table IV).
Discussion
The initial enrollment activities of the Morelos HPV Study have been quite satisfactory. Approximately 95% of the women who were invited to join the study did so, which resulted in a baseline enrollment of 7 732 participants. These women represent 5.1% of female IMSS enrollees between the ages of 15 and 85 with access to the CCSP,* in Morelos during 1999, and they represent 1.4% of the women in that state in this age range.17 Also, almost 90% of the women who were asked to return for a follow-up colposcopy visit complied. This is a very high follow-up rate, especially for a large study.
It is important to note that prior to this study, a great deal of work was dedicated to the reorganization and improvement of the IMSS CCSP in Morelos. Much of the success of the initial enrollment of the Morelos HPV Study can be attributed to these activities. For example, the high concordance between the histopathologists in Mexico (EC) and in the U.S. (BR) is in part a reflection of the aforementioned capacity building and quality improvement activities. Additionally, there are other reasons for the successful enrollment phase of this study, these include guidance and support from all of the researchers involved, a significant amount of interinstitutional funding and collaboration, and a total quality management approach.
This description of the enrollment activities, design and methodology of the Morelos HPV Study may be of interest to other researchers in the field. The enrollment phase of this study has generated important information about the prevalence of HPV infection, and the prevalence of the various stages of cervical disease and cancer. The sensitivity and specificity results of both the self-collected and clinician-collected HPV tests, in relation to the Pap will be reported in future publications. Other findings, such as the acceptability of the self-collected HPV test as compared to the Pap, and the cost-effectiveness of HPV testing vs. the Pap, will also be described in separate publications.
Acknowledgements
We would like to thank Dr. Mario Balbuena and Dr. Sergio Juarez for their logistic support during the beginning stages of this study. Also, we would like to acknowledge the women who participated in this study, as well as the help and support of many individuals from the participating institutions.
References
1. National History of Cervical Cancer: Even Infrequent Screening of Older Women Saves Lives. Cervical Cancer Prevention Fact Sheet. Program for Appropriate Technology in Health (PATH). November, 2000. Available from: http://www.path.org. [ Links ]
2. Estadísticas de mortalidad relacionada con la salud reproductiva. México, 1997 (Indicadores). Salud Publica Mex 1999;41:138-146. [ Links ]
3. Hernández-Avila M, Lazcano-Ponce EC, Alonso-de Ruiz P, Romieu I. Evaluation of the cervical cancer screening program in Mexico: A population-based case-control study. Int J Epidemiol 1998;27:1-7. [ Links ]
4. Lazcano-Ponce EC, Rascón-Pacheco RA, Lozano-Ascencio R, Velasco-Mondragón HE. Mortality from cervical carcinoma in Mexico: Impact of screening, 1980-1990. Acta Cytol 1996;40:506-512. [ Links ]
5. Salmerón-Castro J, Franco-Marina F, Salazar-Martínez E, Lazcano-Ponce EC. Panorama epidemiológico de la mortalidad por cáncer en el IMSS: 1990-1995. Salud Publica Mex 1997;39:266-273. [ Links ]
6. National Cancer Institute Workshop: The 1988 Bethesda System for reporting cervical/vaginal cytological diagnoses. JAMA 1989;262:931-934. [ Links ]
7. Lazcano-Ponce EC, Alonso de Ruiz P, Salmerón Castro J, Hernández Avila M. Cervical cancer screening in developing countries: Why is it ineffective? The case of Mexico. Archives of Medical Research; 30: 240-250. [ Links ]
8. Lazcano-Ponce EC, Nájera-Aguilar P, Alonso-de Ruiz P, Buiatti E, Hernández Avila M. Programa de detección oportuna de cáncer cervical en México: Diagnóstico situacional. Cancerologia 1996;42:123-40. [ Links ]
9. Lazcano-Ponce EC, Castro R, Allen B, Nájera-Aguilar P, Alonso-de Ruiz P, Hernández Avila M. Barriers to early detection of cervical-uterine cancer in Mexico. J Women's Health 1999;399-408. [ Links ]
10. Mitchell MF, Tortolero-Luna G, Wright T, Sarkar A, Richards-Kortum R, Hong WK et al. Cervical human papillomavirus infection and intraepithelial neoplasia: A review. Monogr Natl Cancer Inst 1996;21:17-25. [ Links ]
11. Herrero R. Epidemiology of cervical cancer. Monogr Natl Cancer Inst 1996;21:1-6. [ Links ]
12. Cuzick J, Meijer CJ, Walboomers JM. Screening for cervical cancer. Lancet 1998;351:1439-1440. [ Links ]
13. Division of STD Prevention. Prevention of Genital HPV Infection and Sequelae: Report of an External Consultants' Meeting. Department of Health and Human Services, Atlanta (GA): Centers for Disease Control and Prevention (CDC), December 1999. [ Links ]
14. HPV Testing: Promises and Challenges. Cervical Cancer Prevention Fact Sheet. Program for Appropriate Technology in Health (PATH). November, 2000. http://www.path.org [ Links ]
15. Instituto Nacional de Estadística, Geografía e Informática. Censo General de Población y Vivienda, 2000. Tabulados Básicos y por Entidad Federativa. Bases de Datos y Tabuladores de la Muestra Censal. México, D.F.: INEGI, 2001. [ Links ]
16. Instituto Nacional de Estadística, Geografía e Informática—DGG. Superficie de la República Mexicana por Estados. 1999. [ Links ]
17. Instituto Nacional de Estadística, Geografía e Informática. Estados Unidos Mexicanos. XII Censo General de Población y Vivienda, 2000. Tabulados de la Muestra Censal. Cuestionario Ampliado. México, D.F.: INEGI, 2000. [ Links ]
18. Principales resultados de la estadística sobre mortalidad en México. Salud Publica Mex 1998;40:517-523. [ Links ]
19. Secretaría de Salud, Mortalidad 1998. México, D.F.: SSA, Febrero 2000. [ Links ]
20. Estadísticas de mortalidad relacionada con la salud reproductiva. Salud Publica Mex 1999;41:138-146. [ Links ]
21. Secretaría de Salud. Boletín de Información Estadística No. 19, 1999. vol. 1, Recursos y Servicios. México, D.F.: SSA, 2000. [ Links ]
22. Salmerón J, Juárez S, Lazcano EC, Hernández M. Evaluación de una intervención comunitaria para el control de cáncer cervical en la delegación Morelos del Instituto Mexicano del Seguro Social. En: García MC, Reyes H, Viniegra L, ed. Las múltiples facetas de la investigación en salud: Proyectos estratégicos del Instituto Mexicano del Seguro Social. México, D.F.: Instituto Mexicano del Seguro Social, 2001. [ Links ]
23. Torres G, Salmerón J, Téllez M, Lazcano EC, Juárez S, Gil L et al. Call and recall for cervical cancer screening: A randomized field trial. Int J Cancer 2000;87(6):869-873. [ Links ]
24. Salmerón-Castro J, Lazcano-Ponce EC, Pérez-Cuevas R, Del Río-Gómez I, Torres-Torija I, Hernández-Avila M. Proposal to institutionalize criteria and quality standards for cervical cancer screening within a health care system. Cad Saude Publica 1998;14:67-75. [ Links ]
25. Lörincz A. Hybrid Capture‰ method for detection of human papillomavirus DNA in clinical specimens. Papillomavirus Report. 1996;7: 1-5. [ Links ]
* Mark E. Sherman, MD,(6) Brigitte M Ronnett, MD,(6) Enrique Carmona, MD,(1) Alfredo Antúnez, MD,(1) Horacio Manzanares, MD,(1) Mario Uribe, MD,(1) Ricardo Pérez-Cuevas, MD, MPH,(7) Ahidee Leyva, MSc,(3) Elsa Yunes, MD, MSc.(3)
This study was supported by: Instituto Mexicano del Seguro Social (IMSS), Consejo Nacional de Ciencia y Tecnología (CONACyT grant #26267M), Instituto Nacional de Salud Pública (INSP), National Institutes of Health (NIH grant #U19 AI38533), and Digene Corporation.
(1) Instituto Mexicano del Seguro Social, Cuernavaca, Morelos, México.
(2) The Johns Hopkins University Bloomberg School of Public Health, Baltimore, MD, USA.
(3) Instituto Nacional de Salud Pública, Cuernavaca, Morelos, México.
(4) Departments of Family Medicine and Obstetrics and Gynecology, Medical College of Georgia, Augusta, GA, USA.
(5) Digene Corporation, Gaithersburg, MD, USA.
(6) Department of Pathology and Obstetrics and Gynecology, The Johns Hopkins University School of Medicine and Hospital, Baltimore, MD, USA.
(7) Instituto Mexicano del Seguro Social, México, D.F., México.
Received on: October 11, 2000 • Accepted on: November 17, 2001
Address reprint requests to: Yvonne Flores. Unidad de Investigación Epidemiológica y en Servicios de Salud. Hospital General Regional con Medicina Familiar No. 1. Avenida Plan de Ayala Esq. Central S/N, colonia Chapultepec, 62450 Cuernavaca, Morelos, México.
E-mail: yflores@jhsph.edu














